The ethical landscape of nursing is rapidly evolving. For nurses practicing in Oklahoma, these changes are especially salient given the state’s unique healthcare environment, marked by rural health inequities, a strong presence of Indigenous populations, and persistent workforce shortages. These realities heighten the need for clear ethical guidance in clinical decision-making, patient advocacy, and health system leadership. This article examines key ethical challenges faced by nurses in Oklahoma, including moral distress, health equity, patient autonomy, confidentiality, and staffing ethics, and illustrates how the American Nurses Association (ANA) Code of Ethics can serve as a practical framework to navigate them.
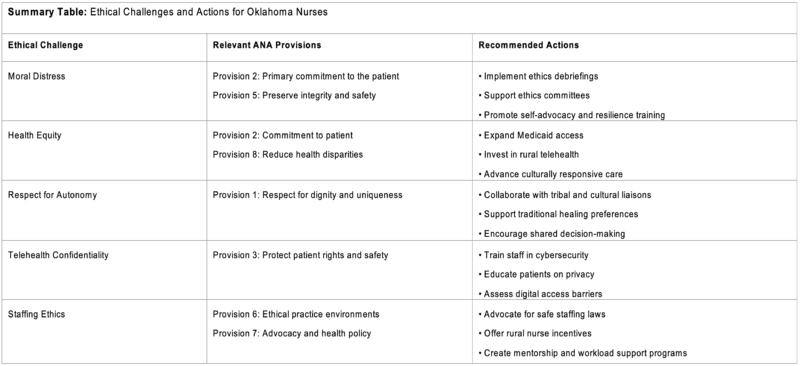
Nurses often encounter situations where they are unable to act according to their ethical convictions due to institutional constraints, policy mandates, or inadequate staffing. This experience, known as moral distress, can undermine both nurses’ well-being and patient care quality (Aljabery et al., 2024). These emotionally taxing situations also threaten the ethical integrity of care environments. Provision 2 of the ANA Code of Ethics affirms that the nurse’s primary commitment is to the recipient of care, whether an individual, family, or community. Additionally, Provision 5 highlights the nurse’s responsibility to safeguard their dignity, integrity, and professional competence (ANA, 2025). To mitigate moral distress, healthcare organizations must cultivate ethical practice environments. This includes facilitating ethics debriefings to process complex cases, supporting institutional ethics committees and moral resilience programs, and promoting professional development in self-advocacy and emotional well-being.
Oklahoma nurses serve on the frontlines of a state marked by stark disparities in healthcare access and outcomes. Oklahoma is worse than the U.S. average for healthcare metrics such as cardiovascular disease death, colorectal cancer deaths, firearm suicides, and premature death (NYU Grossman School of Medicine & Robert Wood Johnson Foundation, n.d.). These disparities, driven by geography, income, race, and historical inequities, are particularly pronounced in rural counties, tribal communities, and underserved urban areas. Nurses in these settings witness firsthand the impact of unreliable transportation, underfunded facilities, and limited broadband infrastructure, all of which contribute to inequitable care (Centers for Medicaid and Medicare, 2024; U.S. Census Bureau, n.d.). Provision 8 of the ANA Code of Ethics calls nurses to collaborate to protect human rights and reduce health disparities. Provision 2 reiterates the imperative of prioritizing patient-centered care for all populations (ANA, 2025). To address these ethical responsibilities, nurses and policymakers in Oklahoma should work to expand Medicaid to close coverage gaps, invest in telehealth infrastructure, especially in rural and tribal communities, and advance culturally responsive care models that recognize social determinants of health.
Respect for patient autonomy is a fundamental nursing value and one that carries particular ethical weight in Oklahoma’s richly diverse cultural landscape. With 39 federally recognized tribal nations and a growing array of cultural traditions across the state, nurses must often navigate nuanced care preferences rooted in spiritual beliefs, community norms, and traditional healing practices. Provision 1 of the ANA Code affirms that “the nurse practices with compassion and respect for the inherent dignity, worth, and unique attributes of every person” (ANA, 2025). Oklahoma nurses may encounter patients who integrate traditional healing with biomedical treatments, family- and community-led decision-making in end-of-life care, and culturally influenced expressions of pain or preferences around pharmacologic interventions. To uphold autonomy in culturally diverse care, nurses should: collaborate with tribal boards, liaisons, and cultural advisors; and provide safe, respectful environments where patients and their support systems can discuss their values and preferences.
Telehealth has emerged as a critical care delivery tool, particularly in Oklahoma’s rural and underserved areas. However, the rapid shift to virtual care brings new ethical challenges, especially related to confidentiality and informed consent (Houser et al., 2023). Patients may participate in telehealth visits from crowded homes, on shared devices, or without a full understanding of privacy risks. These factors complicate nurses’ efforts to safeguard sensitive health information. Provision 3 obligates nurses to “promote, advocate for, and protect the rights, health, and safety of the patient” (ANA, 2025). To maintain ethical standards, nurses and institutions should provide cybersecurity and privacy training for staff, educate patients on protecting their privacy during virtual visits, and screen for digital access barriers and tailor communication accordingly. As the telehealth infrastructure continues to grow in Oklahoma, nurses must advocate for equitable and secure systems that protect patient dignity.
Although staffing shortages are a national issue, they are especially acute in Oklahoma’s rural and frontier communities, where geographic isolation and strained hospital resources exacerbate the challenge (Oklahoma Hospital Association, n.d.). In these settings, nurses may face difficult decisions about delaying non-urgent care, prioritizing acute needs, or forgoing patient education due to time constraints. These ethical dilemmas are addressed in Provision 6, which underscores the need for ethical practice environments that support safe, high-quality care, and Provision 7, which charges nurses with advancing the profession through advocacy and health policy (ANA, 2025). Oklahoma nurses can advocate for safe staffing legislation to ensure safe nurse-patient ratios, rural recruitment and retention incentives, including loan forgiveness and housing stipends, and organizational mentorship and workload management programs. Creating ethical work environments is not aspirational, it is essential for protecting nurses and the communities they serve.
The moral complexity of modern nursing cannot be overstated. Whether rooted in systemic inequities, workforce constraints, or cultural differences, ethical challenges affect both nursing decision-making and patient outcomes. For nurses in Oklahoma, navigating these realities requires not only clinical skill but also ethical clarity and courage. By aligning daily practice with the ANA Code of Ethics, Oklahoma nurses can respond to adversity with integrity, cultural humility, and compassion. Participation in professional organizations like the Oklahoma Nurses Association, collaboration with tribal health boards, and service on hospital ethics committees are all meaningful avenues for ethical leadership. The ANA Code is not just a guide; it is a call to action. By championing ethics at the bedside, in leadership, and beyond, Oklahoma nurses can help shape a more just and equitable healthcare system, one decision, one patient, and one voice at a time.
References
Aljabery, M., Coetzee-Prinsloo, I., van der Wath, A., & Al-Hmaimat, N. (2024). Characteristics of moral distress from nurses’ perspectives: An integrative review. International Journal of Nursing Sciences, 11(5), 578–585. https://doi.org/10.1016/j.ijnss.2024.10.005
American Nurses Association. (2025). Code of ethics for nurses with interpretive statements. American Nurses Association.
Centers for Medicare & Medicaid Services. (2024, November). Advancing health care in rural, tribal, and geographically isolated communities: FY 2024 year in review. U.S. Department of Health & Human Services. https://www.cms.gov/files/document/fy-2024-advancing-rural-health-508.pdf
Houser, S. H., Flite, C. A., & Foster, S. L. (2023). Privacy and security risk factors related to telehealth services–a systematic review. Perspectives in Health Information Management, 20(1), 1f.
NYU Grossman School of Medicine, Department of Population Health, & Robert Wood Johnson Foundation. (n.d.). Congressional District Health Dashboard. Retrieved May 15, 2025, from https://www.congressionaldistricthealthdashboard.org/
Oklahoma Hospital Association. (n.d.). Workforce. https://www.okoha.com/OHA/OHA/Health_Care_Issues/Workforce_/Workforce.aspx
U.S. Census Bureau. (n.d.). Digital Equity Act Population Viewer [Data visualization]. Retrieved May 15, 2025, from https://mtgis-portal.geo.census.gov/arcgis/apps/webappviewer/index.html?id=c5e6cf675865464a90ff1573c5072b42