Introduction
In the United States, approximately one in four adults has a disability, making this population one of the largest minority groups in the country (Centers for Disease Control and Prevention [CDC], 2020; Smeltzer et al., 2017). Globally, over one billion people, or 15% of the world’s population, experience disability (World Health Organization [WHO], 2020). Disability and health are separate concepts; having a disability does not inherently equate poor health, and promoting health is essential for everyone (Mitra et al., 2022). Nearly everyone will experience disability during their lifespan, underscoring the necessity for healthcare professionals to receive disability-specific training (Smeltz et al., 2024).
Adults with disabilities are more likely to report their health as “fair” or “poor” compared to those without disabilities, and they also face increased risks for secondary conditions like depression, diabetes, stroke, obesity, and poor oral health (WHO, 2020). Additionally, people with disabilities (PWD) commonly experience poor healthcare quality, unmet medical needs, higher comorbidities, increased vulnerability to abuse, and shorter life expectancy (Gréaux et al., 2023). Despite these known disparities, healthcare curricula continue to lack structured, disability-specific training, resulting in nurses who are inadequately prepared to meet the needs of PWD (Smeltz et al., 2024).
Several nursing-specific calls to action have emphasized the importance of integrating disability education to improve healthcare outcomes for PWD (Miner et al., 2024). Most major nursing organizations acknowledge that addressing disability in nursing education curricula is critical to developing nurses capable of providing appropriate, ethical care across the lifespan. The purpose of this study was to develop and implement an undergraduate nursing elective, Exploring Disability in Healthcare, and examine its impact on students’ self-perceptions of comfort, skill, and clinical approach when caring for PWD. Findings from this study also support the position that disability education should be integrated as a core, required component of undergraduate nursing curricula rather than offered solely as an elective.
Design
This quasi-experimental quantitative study used a pre- and post-survey comparison design to evaluate the effects of the Exploring Disability in Healthcare elective course on undergraduate nursing students’ self-perceptions of caring for people with disabilities (PWD). The study was reviewed and approved by the Institutional Review Board (IRB) at the institution where it was implemented.
Setting and Participants
The study took place at a large public university in Maryland with a well-established nursing program. Eligible participants were undergraduate nursing students enrolled in the elective course Exploring Disability in Healthcare.
Intervention
Faculty developed a three-credit elective course specifically aligned with the Core Competencies on Disability for Health Care Education (ADHCE, 2024). The course was primarily asynchronous, except for one synchronous Zoom debriefing session at semester’s end. The course content included disability-specific learning modules, reflective assignments, discussion boards, guided debriefings, and exams.
Measures
Students’ self-perceptions were assessed with a modified Healthcare Provider Questionnaire (Robey et al., 2001), featuring scenario-based prompts across four clinical situations: (1) a person without apparent disabilities, (2) a verbal person using a power-assisted wheelchair, (3) a person with an intellectual disability, and (4) a person using both a power-assisted wheelchair and an assistive communication device. Participants rated themselves on 12 self-perception items measuring perceived skill, comfort, and clinical approach using a 7-point semantic differential scale. For each item, a score of 7 corresponded to the positive anchor (e.g., skilled, comfortable, rational), while a score of 1 corresponded to the opposing anchor (e.g., unskilled, uncomfortable, intuitive), with higher scores indicating more favorable self-perceptions.
Data Collection
Data was collected anonymously at two points: before exposure to course content (pre-course survey) and after course completion (post-course survey). Students accessed the pre-course survey electronically via their Learning Management System (LMS) and email prior to starting the course. The post-course survey was administered at semester’s end during a synchronous Zoom debriefing, with a survey link shared in the chat. Because the surveys were anonymous, individual responses could not be matched between the two time points, necessitating analysis as independent samples. Data was collected over two semesters (Fall 2023 and Spring 2024) and analyzed in aggregate.
Data Analysis
Survey responses from Qualtrics were imported into IBM SPSS Statistics (version 29). Mean and standard deviation scores for each of the 12 self-perception items were calculated for both pre- and post-course surveys across each clinical scenario. Independent-samples t-tests compared mean self-perception scores between pre- and post-course groups, and one-way ANOVA assessed overall variance between groups. Data visualization (e.g., line charts) was utilized to illustrate changes in students’ self-attributions from pre-course to post-course across scenarios.
Results
A total of 15 nursing students completed the pre-course survey prior to exposure to disability-related course content. Surveys were distributed electronically via the Learning Management System and email, which may have contributed to the lower response rate. Following completion of the disability course content, 39 nursing students completed the post-course survey at the end of the semester. The post-course survey was administered after a 45-minute synchronous small-group debriefing conducted via Zoom, with distribution occurring during the live session.
Figure 1 displays the average ratings for each of the 12 self-perception items across four clinical scenarios for both the pre- and post-course surveys. Pre-course scores ranged from 4.13 to 5.40, while post-course scores ranged from 5.18 to 5.97.
Comparing Self-Perception Between the Pre- and Post-Course Surveys
The mean scores for all 12 self-perception items were consistently higher in the post-course survey across all four scenarios, reflecting improvements in participants’ confidence, comfort, and clinical approach after completing the disability course. The mean differences between pre- and post-course survey scores ranged from 0.32 to 1.37, with an average increase of 0.64 to 0.77 points per scenario (Figure 1).
Mean scores for all four scenarios were higher in the post-course survey compared to the pre-course survey (Figure 1). Independent-sample t-tests revealed a statistically significant increase in self-perception scores for Scenario 1 (p = 0.047).
Figure 1. Mean Self-Attribution Scores in Each of the Four Scenarios in the Entry and Exit Course Surveys |
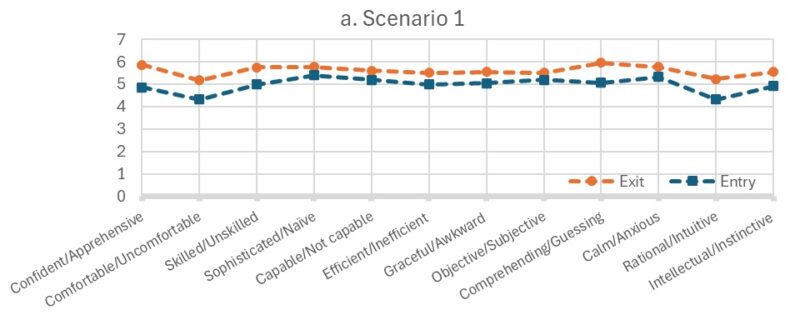

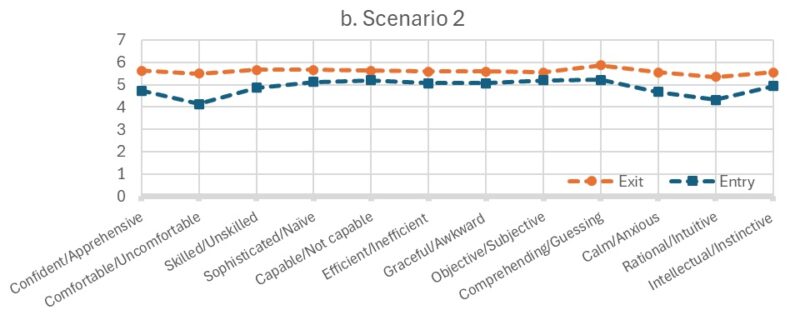

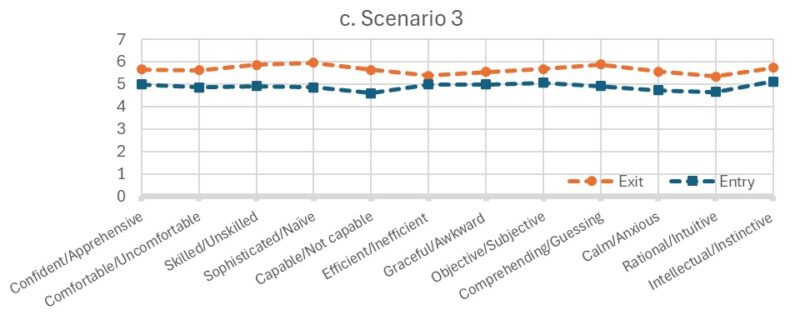

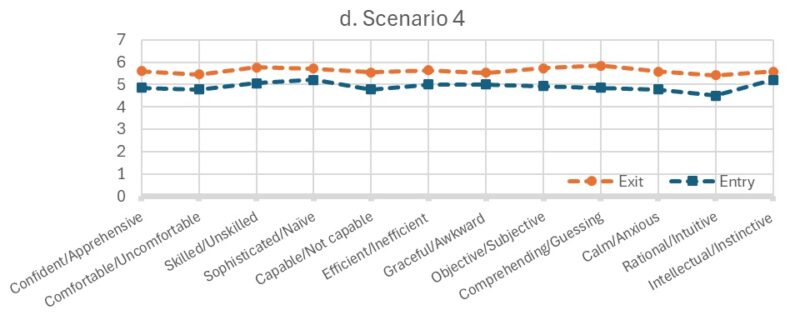
Scores range 1-7, with higher scores indicating more positive self-attributes. The questionnaire used scenario-based prompts where nursing students were asked to imagine themselves in four different clinical scenarios involving; (1) a person who has no apparent disabilities; (2) a person who uses a power-assisted wheelchair and is verbal; (3) a person who has an intellectual disability; and 4) a person who uses a power-assisted wheelchair and uses an assistive communication device.
Discussion
The purpose of this study was to develop and implement an undergraduate nursing elective and measure its effect on nursing students’ self-perceptions of their skill level, comfort, and interpersonal approach when caring for PWD. Although improvements were observed across all domains, several patterns were notable. Gains in perceived skill were most evident in items related to capability, efficiency, and comprehension, suggesting less uncertainty and more intentional clinical reasoning. Improvements in comfort, including confidence and calmness, appeared to occur alongside skill development rather than in isolation, indicating that comfort may be grounded in preparedness rather than familiarity alone. Changes in clinical approach reflected a shift toward more rational and objective decision-making, suggesting movement away from instinctive or assumption-based care.
Improvement in Self-Perceptions Across Scenarios – The study results indicated consistent improvements in students’ self-perceptions across all four clinical scenarios, with mean scores increasing for each of the 12 measured items. These improvements were observed in scenarios involving patients without apparent disabilities, as well as those using assistive devices or diagnosed with intellectual disabilities. The uniformity of these positive changes suggests that the course effectively addressed common barriers to providing care for PWD, such as discomfort, uncertainty about appropriate clinical approaches, and perceived lack of skill. The increase in mean scores ranged from 0.32 to 1.37 points, with average improvements of 0.64-0.77 points across scenarios, emphasizing the course’s impact on students’ confidence and competence.
These findings align with previous studies that demonstrate that structured disability education enhances healthcare providers’ confidence and competence in caring for PWD (Ailey et al., 2024; Edwards et al., 2022). The consistency of improvements across all clinical scenarios suggests that this elective course provided a strong foundation for nursing students to build more inclusive, empathetic, and effective care practices.
Participation – Participation differed between the pre-course and post-course surveys, offering faculty important insights for future course design. The higher response rate following the synchronous guided debrief suggests that real-time, reflective engagement may foster greater student investment, a finding consistent with literature indicating that synchronous learning environments can enhance connection and accountability. Scenario-specific findings such as particularly stronger self-perception changes in Scenario 1 compared to later scenarios, may reflect students’ initial changes in their foundational assumptions about disability, with subsequent scenarios requiring more complex communication and systems-level considerations. Together, these observations highlight opportunities to refine course timing, reinforce scenario progression, and intentionally integrate synchronous reflection to further support student engagement and learning in future iterations of the course.
Implications for Nursing Education – The consistent positive changes in self-perception across all measured dimensions suggest that integrating structured, disability-specific education into nursing curricula can effectively enhance nursing students’ comfort, skills, and clinical approaches when caring for PWD. These results support other calls for more comprehensive disability education within all healthcare training programs, aligning with broader healthcare goals of promoting equity and inclusion. By addressing potential biases and fostering empathy, courses like “Exploring Disability in Healthcare” can prepare future nurses to deliver higher-quality care to a diverse patient population.
Limitations – Several limitations should be considered when interpreting these findings. The difference in sample sizes between the pre-course and post-course surveys presents a challenge for direct comparison, potentially affecting the generalizability of the results. The method of survey administration, particularly the reliance on self-reported data, introduces the possibility of social desirability bias, where students may have rated themselves more favorably post-course. Future research should explore the long-term impact of disability-specific education on clinical practice through follow-up assessments and qualitative student reflections. Another limitation of this study is the inability to match individual pre-course and post-course survey responses, as all data were collected anonymously. This prevented the use of paired statistical comparisons and required treating the pre-course and post-course groups as independent samples. Future studies should consider implementing confidential participant tracking methods to allow for more precise within-subject comparisons.
Conclusion
This study contributes to the growing body of evidence on the importance of integrating disability education into healthcare curricula. The “Exploring Disability in Healthcare” course successfully enhanced Maryland nursing students’ self-perceptions of their skill, comfort, and clinical approaches when caring for PWD. These findings highlight the potential benefits of such educational initiatives in promoting more inclusive and empathetic care. Future research should continue to explore the most effective methods of delivering disability education and examine its impact on clinical outcomes.
*Author Affiliation: University of Maryland School of Nursing. Correspondent author’s email rweston@umaryland.edu
References
Ailey, S. H., Bathje, M., Tichá, R., Abery, B., Khuu, B. K., & Angel, L. (2024). Health professionals’ education related to people with intellectual and developmental disabilities: A scoping review. Journal of Applied Research in Intellectual Disabilities, 37(3), e13208.
Alliance for Disability in Healthcare Education. (2019). Core competencies on disability for health care education. https://nisonger.osu.edu/wp-content/uploads/2019/08/post-consensus-Core-Competencies-on-Disability_8.5.19.pdf
Centers for Disease Control and Prevention. (2020). Disability impacts all of us. https://www.cdc.gov/disability-and-health/articles-documents/disability-impacts-all-of-us-infographic.html
Gréaux, M., Moro, M. F., Kamenov, K., Russell, A. M., Barrett, D., & Cieza, A. (2023). Health equity for persons with disabilities: A global scoping review on barriers and interventions in healthcare services. International Journal for Equity in Health, 22(1), 236. https://doi.org/10.1186/s12939-023-02035-w
Miner, D. C., Ailey, S. H., Thompson, R. A., Squires, A., Adarlo, A., & Brown, H. (2024). “We have met the enemy and it is us”: Healthcare professionals as the barrier to health equity for people with intellectual and developmental disability. Research in Nursing & Health, 47, 269–273. https://doi.org/10.1002/nur.22376
Mitra, M., Long-Bellil, L., Moura, I., Miles, A., & Kaye, H. S. (2022). Advancing health equity and reducing health disparities for people with disabilities in the United States. Health Affairs, 41(10), 1379–1386.
Robey, K. L., Gwiazda, J., & Morse, J. (2001). Nursing students’ self-attributions of skill, comfort, and approach when imagining themselves caring for persons with physical impairments due to developmental disability. Journal of Developmental and Physical Disabilities, 13(4), 361–371.
Smeltz, L., Havercamp, S. M., & Meeks, L. (2024). Disability education in nursing: A call to action. AMA Journal of Ethics, 26(1), E54–E61. https://doi.org/10.1001/amajethics.2024.54
Smeltzer, S. C., Mariani, B., & Meakim, C. (2017). Advancing care excellence for persons with disabilities. Villanova University College of Nursing. https://www.nln.org/education/teaching-resources/professional-development-programsteaching-resourcesace-all/ace-d/additional-resources/overview-and-introduction-to-disability-3830c45c-7836-6c70-9642-ff00005f0421