In nursing education, we often talk about trauma-informed care, emotional awareness, and professional behavior. Yet in classrooms and clinical settings, many students continue to struggle with disengagement, shutdown, or reactivity. These patterns are frequently interpreted as motivation issues, attitude problems, or gaps in professionalism.
However, what I have observed, both as a nurse and an educator, is something different. Many of these struggles are not failures of insight or effort. In fact, they are signs of dysregulation. When the nervous system is overwhelmed, learning, reflection, and behavior change become difficult. Sometimes they are impossible, regardless of intention.
This raises an uncomfortable but necessary question for nursing education: Are we asking for behavior before we have established regulation?
Regulation Is Not the Same as Awareness
In nursing education, we often assume that once students understand expectations, they will be able to meet them. We emphasize insight, reflection, and accountability, believing these are the primary drivers of behavior change. When students struggle, we may increase feedback, reinforce policies, or revisit professionalism standards.
What this approach overlooks is the role of the nervous system.
In other words, awareness does not equal regulation. A student can fully understand expectations and still be unable to access the cognitive and emotional capacity required to meet them. When stress, sensory overload, fear of failure, or prior trauma are present, the nervous system may shift into survival modes that limit learning, flexibility, and engagement (Herrera Torres et al., 2021). In these moments, behavior is not a choice in the way we often assume. It is a physiological response.
Why Behavior Comes Last, Not First
Regulation precedes learning, reflection, and behavior. This is not a theoretical concept; it is observable in everyday nursing education environments. For example, when learners feel safe, supported, and regulated, they are more likely to:
- Engage in discussion
- Ask questions
- Tolerate feedback
- Integrate new information
- Recover from mistakes
When regulation is absent, the opposite occurs. Students may appear withdrawn, defensive, irritable, or disengaged. However, these behaviors are frequently labeled as lack of motivation or unprofessionalism, when they may instead reflect nervous system overload.
“Regulation Before Learning” visual framework
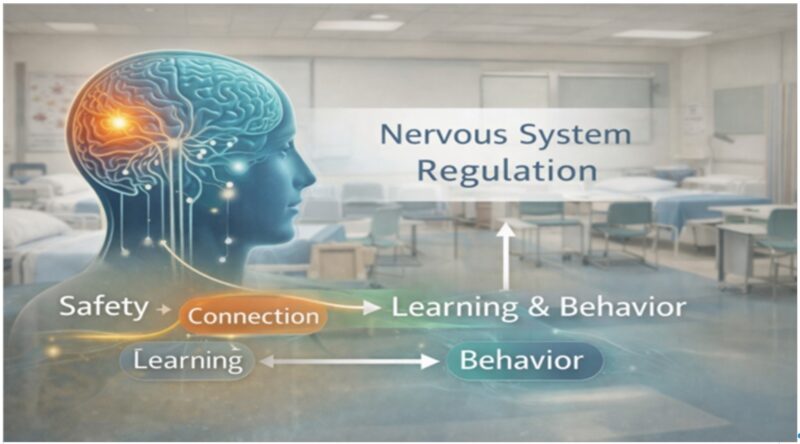

This distinction matters because it changes how educators respond.
Research supports this relationship between regulation and learning capacity in higher education. Students who experience external and internal regulation support demonstrate higher engagement and improved learning outcomes (Herrera Torres et al., 2021). Similarly, faculty report that emotionally attuned support and relational presence significantly influence students’ ability to persist and succeed in nursing programs (Brower & Henry, 2025).
A Brief Classroom Example
During a recent class session, one of my students sat in the middle row, in the last seat against the wall. An older peer, who had helped mentor him earlier in the term, sat directly behind him. Over the first part of class, I noticed the student was beginning to drift off. He shifted restlessly in his seat, his attention fading. Eventually, he lowered his head onto the table and began scrolling on his phone.
Importantly, I was not the only one who noticed. Another student quietly suggested that we shut the door to reduce hallway noise. I dimmed the lights slightly, slowed the pacing of the lesson, and softened my tone.
Within minutes, his posture changed. He lifted his head, put his phone away, and began tracking the discussion again. Later in the session, he leaned forward and contributed a thoughtful comment related to the topic. Nothing about his intelligence, values, or professionalism changed that day. What changed was his level of regulation.
This is what regulation before behavior looks like in practice.
Reframing the Educator’s Role
A regulation-centered approach does not lower standards or excuse harmful behavior. Instead, it reframes the educator’s role from enforcing compliance to supporting capacity.
This includes intentional attention to:
- Environmental regulation (lighting, noise, pacing, predictability)
- Relational regulation (tone, presence, clarity, psychological safety)
- Co-regulation before self-regulation.
Only after regulation is established can reflective practice, accountability, and professional growth truly occur.
This perspective aligns with emerging evidence that self-regulation is a learned, supported skill rather than an assumed trait. For example, students’ ability to manage stress, attention, and emotional demands develops over time and improves when learning environments provide consistent external regulation support (Kim et al., 2020).
Why This Matters for Kansas Nursing Education
Kansas nursing programs, like many across the country, are facing increased student stress, higher attrition, and growing concerns about burnout and mental health. Many students balance coursework with employment, caregiving, and financial strain while navigating emotionally demanding clinical environments.
When we interpret dysregulated behavior as a character flaw or professionalism deficit, we risk misidentifying the problem and responding in ways that increase distress rather than capacity.
By embedding regulation into our educational practices, we strengthen:
- Clinical judgment and patient safety
- Retention and remediation outcomes
- Professional identity formation
- Ethical, trauma-informed teaching practices
This is not about making nursing education easier. It is about making it more effective.
Where Nursing Education Can Shift
If nursing education is serious about trauma-informed care, then regulation must move from the margins to the center of practice. This means asking different questions when students struggle:
- What might be overwhelming the nervous system here?
- What support would increase capacity before addressing behavior?
- How can safety be established before correction?
These questions do not weaken education. They strengthen it. They move us toward a model of teaching that recognizes regulation as a prerequisite for learning rather than a reward for good behavior.
Conclusion
Nursing education is grounded in compassion, safety, and evidence-based practice. Yet we often overlook the most basic prerequisite for learning: a regulated nervous system. When we shift from asking, “Why won’t this student behave differently?” to “What support would help this student access regulation?” we do more than improve outcomes. We align our educational practices with what neuroscience and lived experience already tell us.
Regulation before behavior is not a soft approach. It is a precise, ethical, and evidence-informed framework for educating the next generation of nurses.
References
Brower, E., & Henry, M. (2025). Faculty’s experience providing nursing student support. Nurse Education Today, 150, 106718. https://doi.org/10.1016/j.nedt.2025.106718
Herrera Torres, L., Souza-Soares de Quadros, M. R., Sánchez-Sánchez, L. C., & Ramiro-Sánchez, T. (2021). Satisfaction with self and external regulation of learning in higher education students in Brazil. International Journal of Environmental Research and Public Health, 18(11), 5914. https://doi.org/10.3390/ijerph18115914
Kim, K., Lee, J., & Kim, B. (2020). Self-regulation, academic engagement, and learning outcomes in higher education. Journal of Educational Psychology, 112(3), 495–508.
When stress, sensory overload, fear of failure, or prior trauma are present, the nervous system may shift into survival modes that limit learning, flexibility, and engagement.