





After the COVID-19 pandemic pushed nurses to their limits, it became impossible to ignore the vulnerability of the healthcare workforce. From a leadership standpoint, traditional, top-down approaches weren’t helping to ease the moral distress, nonstop pressure, or burnout nurses faced. Clearly, something needed to change. Nurses required a model that valued both results and humanity—and they were ready to forge that shift themselves.
One group of determined nurse executives believed they had the power to spark the change. That belief led to Human-Centered Leadership in Healthcare: The Revolution Continues, by Lucy Leclerc, PhD, RN, NPD-BC, Kay Kennedy, DNP, RN, NEA-BC, CPHQ, and Susan Campis, MSN, RN, NE-BC, NBC-HWC, published by the American Nurses Association in January. What started as a conversation has grown into a validated framework—and, as the authors describe, a movement—designed to help nurses lead with authenticity, courage, inclusiveness, and respect while co-creating a healthier work environment.


Why human-centered leadership matters now
The authors identified a core issue—patient care suffers when providers themselves aren’t thriving. To create a healthy work environment where nurses can be at their best, leaders must look within.
“Human-centered leadership in healthcare® (HCL-HC) starts with self,” explained Kennedy. “We like to say, ‘It starts with you, but it’s not about you.’ In complex organizations like healthcare, the most effective way to achieve outcomes is through relationships.”
The foundation of HCL-HC is the leader’s focus on their own well-being and sense of purpose, Campis added. “When you cultivate emotional awareness and extend compassion to yourself, you expand your capacity to recognize and honor those qualities in others.”
HCL-HC is a way of being, not a checklist. It’s evidence-based, practical, and predictive of outcomes. “It’s a framework,” Kennedy said, “that helps you connect the dots between who you are, how you show up, how your team responds, and the culture you co-create.”
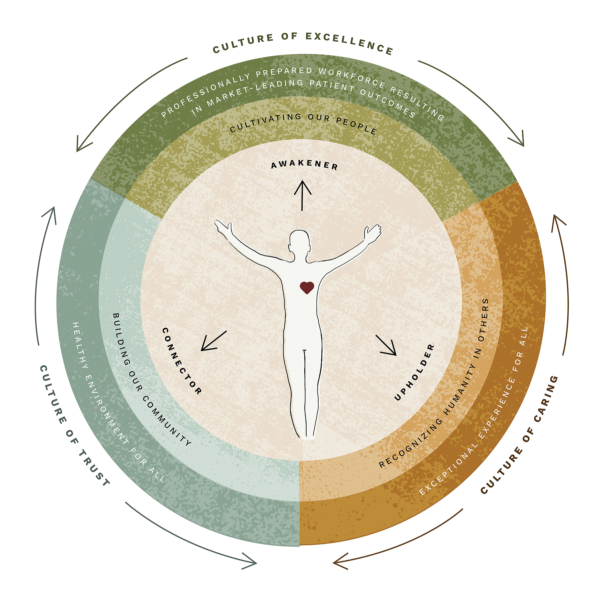
The Framework: Self, Awakener, Connector, Upholder
At the heart of the HCL-HC model is a four-part framework that guides leaders in building cultures of excellence, trust, and caring.
Self – “I matter.”
Leadership begins with self-awareness, mindfulness, and self-compassion. Nurse leaders can’t pour from an empty cup; they must nurture themselves emotionally, mentally, and spiritually. This dimension emphasizes the importance of prioritizing one’s own well-being.
Awakener – “I believe in you.”
The awakener seeks excellence in others, creating opportunities for growth through coaching, mentoring, and advocacy. By awakening potential, leaders foster professional development and inspire confidence.
Connector – “I trust you.”
Trust is the foundation of any team. The connector builds psychologically safe environments where staff members feel empowered to speak up, share ideas, and be their authentic selves.
Upholder – “I see you.”
The upholder dimension is about belonging and inclusiveness. Leaders recognize the humanity in others, lead with emotional intelligence, and create cultures of caring.
Although leaders may naturally identify with one dimension, they’ll be most successful when they integrate all four. “The outward-facing dimensions—awakener, connector, upholder—come together with self in the center,” Campis said. “When you start with self-compassion and well-being, you’re better able to lead others.”

Psychological safety: The bedrock of trust
A crucial part of human-centered leadership is psychological safety. Without it, nurses may hesitate to speak up, which can erode team morale and risk patient safety.
Kennedy, a former CNO and vice president at a number of healthcare organizations, explained: “The concern is that if nurses speak up and it’s not a popular thought, there will be retribution or disrespect. That lack of psychological safety can mean patients are in jeopardy—or staff stop caring altogether.”
Building psychological safety requires intentional effort:
- Leaders admit they don’t have all the answers.
- They encourage perspectives and frame mistakes as learning opportunities.
- They distinguish between unsafe errors and “smart mistakes” born of innovation.
Leclerc, a nurse scientist at Emory Healthcare in Atlanta, emphasized the importance of creating a learning environment. “We know to err is human. When mistakes happen, we need to learn from them, not punish people.”
Campis, an executive director and nurse manager with 25 years of experience, emphasized that vulnerability is essential for leaders who want to build trust and help their teams grow. “When I first became a leader, I thought I had to solve every problem and always have the right answer,” she said. “But once I let my guard down and truly listened, I realized my team already had the insight we needed. My job was to guide, listen, and trust. Vulnerability is what creates an atmosphere of excellence, trust, and caring.”
Psychological safety, then, isn’t a buzzword, it’s the foundation of effective, compassionate leadership.
The authors’ journey
The collaboration among Kennedy, Leclerc, and Campis, all Georgia Nurses Association members, is a testament to relational leadership. Kennedy and Campis first worked together in hospitals, where Kennedy admired Campis’s transformational leadership style. Later, Kennedy met Leclerc at another organization, where their one-on-one meetings frequently turned into brainstorming sessions about leadership.
“I wanted all of us to come together and see what could happen,” Kennedy recalled. “Together, we had something powerful.”
The trio began meeting in 2019 to discuss their feelings of burnout and disillusionment. At the time, all three nurses practiced various forms of servant leadership. However, the limitations of that model, which encourages leaders to put others first, were weighing on them. They all found themselves last when it came to self-care. This sparked the realization that leaders must prioritize self as well as service. That insight became the seed of HCL-HC.
They decided to embark on a research project, starting with interviewing leaders in their own network. When the pandemic hit, the authors thought they’d missed the window to develop their idea, only to quickly realize it was more relevant—and necessary—than ever.
The authors now head their own consultancy, uLeadership, to teach and speak on HCL-HC.
Learning from challenges
The authors acknowledge that even the most seasoned human-centered leaders face struggles. Every healthcare environment has what they call “joy interrupters,” people who, intentionally or not, disrupt positivity. “People ask, ‘What do I do if I’m not surrounded by likeminded leaders?’” Leclerc recalled. “Joy interrupters happen. Sometimes it’s just someone having a bad day; sometimes it’s pushback from a more traditional, top-down leader. The best we can do is stay true to our values, ground conversations in facts, and lead with kindness.”
Kennedy admits she’s been a joy interrupter herself during periods of intense stress. For her, the antidote is mindfulness: being present enough to respond with empathy rather than adding to the disruption. Campis agreed, framing these moments as chances to practice mindfulness and train the brain to respond rather than react. “When you can name your emotions and reflect on what’s happening, you build self-awareness and compassion,” she explained. “It’s about caring for yourself so you can show up as your best self.”
By naming the reality of joy interrupters, the authors keep their framework grounded. Leaders don’t have to be perfect—they just need awareness and resilience to reduce the impact of those inevitable disruptions.
From theory to practice: Stories of transformation
The promise of HCL-HC has now been validated through research and practice. After the first book was published, the authors worked with an independent psychometrician to assess the validity of their HCL-HC self-assessment survey. The results showed predictive validity: leaders who scored well in the “self” dimension also performed better in leading others.
Kennedy recalled the excitement of this discovery: “What we knew at our core was proven with science!”
The new edition of the book includes stories from nurses and organizations that have implemented the framework. These narratives illustrate how theory translates into practice, offering real-world evidence of improved outcomes. The stories “bring the theory to life,” said Leclerc, who has been an executive director and assistant professor of nursing. “Nurses see that human-centered leadership in healthcare isn’t just a hypothesis; it’s actionable. They can operationalize the model in practice and see results.”
The use of HCL-HC principles in academic settings has had notable impacts. Doctor of nursing practice students have used the framework in capstone projects, testing for statistical significance and contributing their stories to the book.
Leclerc recalled nurses approaching herself, Kennedy, and Campis after presentations: “They said, ‘You gave me hope that there is a different way to be.’ That’s validating. It shows the difference this framework can make in one nurse’s life.”
Embracing the future
Every nurse has the power to shape the future of the profession, the authors believe. When nurses lead with authenticity, courage, inclusiveness, and respect, they not only build trust and unlock the potential of their teams but also protect the humanity at the heart of care.
As healthcare becomes increasingly driven by digital tools and efficiency demands, the HCL-HC model serves as a grounding force. By prioritizing relationships, empathy, and trust, it can help ensure that technology enhances nursing, rather than eroding the human connection that defines it.
Leclerc noted that this approach is even more critical as artificial intelligence (AI) and virtual nursing continue to expand. “Human-centered leadership in healthcare is about prioritizing human connection in an age of lightning speed technology,” she explained. With courage and empathy, leaders can help nurses navigate uncertainty about AI and guide these innovations in ways that strengthen the profession.
Empowerment and hope for nurses
Beyond frameworks and validation, the book offers something equally vital: hope.
“Our bold statement,” Kennedy said, “is that what started as a theory is now a movement.”
“We say every nurse is a leader,” she explained. “We want all nurses to feel empowered. Especially those close to the bedside—they have the ability to create culture and outcomes for staff and patients.”
Campis added: “I want nurses to feel hope when they read the book. Nursing is complex and chaotic, but it is also exceptionally rewarding. Human-centered leadership in healthcare reassures us that we can do this with compassion, empathy, caring, excellence, and trust.”
—Elizabeth Moore is a content creator at ANA.
Resources
Discover Human-Centered Leadership in Healthcare: The Revolution Continues and other leadership tools and resources at nursingworld.org/nurses-books.




















