How a large healthcare system standardized its nurse residency programs.
- Research indicates that newly licensed nurses who receive support through a residency program will more likely remain in their job for longer periods and demonstrate more confidence than those who don’t participate.
- A newly integrated large healthcare organization identified the need to align nursing professional development programs from five legacy organizations, providing a standardized approach to role transition, education, and career advancement.
- The creation of an enterprise level nurse residency program ensured alignment with national standards and accreditation criteria while identifying and preserving best practices from the legacy organizations.
Learning Objectives
- Understand how standardizing a nurse residency program impacts nursing transition, professional growth, and retention.
- Identify the benefits and challenges of unifying nurse residency programs to improve nurse retention.
Reflective Learning Question 1:
How could standardizing a nurse residency program impact professional growth and retention within my organization?
Reflective Learning Question 2:
What key benefits of unifying nurse residency programs are relevant to my organization?
No relevant financial relationships were identified for any individuals with the ability to control content of the activity.
Expiration: 4/1/29
1.5 ANCC contact hours
In 2022, The merger of two regional health systems gave rise to a healthcare enterprise covering six states and employing nearly 3,000 prospective newly licensed nurses (NLNs) who graduated from an accredited program and had less than 6 months of nursing experience. To ensure alignment with national standards and accreditation criteria, the enterprise worked to standardize the nursing programs, which included creating a single nurse residency program (NRP).
Within the newly formed enterprise, several NRPs existed, each originating from four legacy approaches; one site lacked a formal NRP. The programs varied by length (from 6 to 12 months), specialty, and accreditation status. Delivery methods ranged from hybrid and online formats to in-person immersion, each tailored to localized needs. Site volumes, cohort sizes, retention rates, and accreditation status also differed.
The new enterprise’s NRP standardization efforts focused on creating an optimal NLN transition-to-practice experience. The restructuring reflects the new system’s nursing vision and desire to cultivate abundant opportunities for educational and career advancement. This standardized approach also aimed to serve as a catalyst for nursing excellence, including bolstered nurse recruitment and retention, heightened NLN competence in clinical skills and critical thinking, and smoother assimilation into the profession and the health system. In an era marked by healthcare consolidation, with mergers and acquisitions becoming commonplace, nurse leaders must understand the intricacies of transition, leverage the strengths and innovations of legacy programs, and transform nursing education to accelerate care at the bedside.
According to Nursing Solutions, Inc., the average retention rate for NLNs from 2022 to 2025 was 70.6%. These figures contrast with the projections provided by the Bureau of Labor Statistics, which estimates that approximately 203,200 annual job openings for RNs through 2031. In their 2024 study, Riches and colleagues discuss how NLNs who receive support during the transition from student to professional nurse through a residency program will more likely remain in their job for longer periods and demonstrate more confidence than nurses who don’t participate.
Program development
The nursing professional development leaders identified the need for a standardized enterprise-wide NRP to aid nursing integration efforts. In early 2023, nursing professional development leaders from all regions, with the primary responsibility of creating a standardized NRP, met to form a transition-to-practice (TTP) committee. Overarching goals of the committee included creating an enterprise approach for the program using a 6-month model and preparing for implementation with considerations of practice transition accreditation program timelines.
In initial meetings, the committee provided an overview of current regional NRP practices, set forth a system-wide vision statement, and identified what decisions would fall within the scope of the standardization project. TTP committee chairs defined principles to guide each working meeting, including team decision-making through consensus, guided discussions, and questions to define the what, who, when, where, why, which, and how of the program.
Key priorities at monthly meetings included incorporating the system-wide vision statement, maintaining regional accreditation, and developing a curriculum for use across the system. Assignment of pre-work and post-work helped to use team’s time efficiently.
Legacy program analysis
Nursing leaders for each legacy residency program assessed recent literature and existing NRP programming. The TTP committee developed a comprehensive NRP integration assessment table to compare topics, duration, and teaching and delivery modalities of legacy NRPs. The integration assessment offered an overview of the American Nurses Credentialing Center (ANCC) Practice Transition Accreditation Program standards, which had been integrated into each legacy program’s curriculum using the ANCC Practice Accreditation Gap Analysis Tool. The analysis identified the following topics as consistent across the five regions: communication, delegation/prioritization/time management, professionalism, and well-being. (See Legacy nurse residency comparison.)
Legacy nurse residency comparison
The following table provides an overview of the legacy nurse residency program structure and content delivery.
(no formal residency program prior to 2022)
Self-paced (3x)
- Critical care
- Emergency
- Maternal/newborn
- Medical–surgical
- Pediatrics
- Ambulatory
- Behavioral health
- Critical care
- Emergency
- Maternal/newborn
- Medical–surgical
- NICU
- Oncology
- Pediatrics
- Surgical services
- Critical care
- Emergency
- Maternal/newborn
- Medical–surgical
- NICU
- Oncology
- Pediatrics
- PICU
- Surgical services
- Critical care
- Emergency
- Maternal/newborn
- Medical–surgical
- Pediatrics
- Surgical services
- Critical care
- Emergency
- Medical–surgical
- NICU
- Oncology
- Pediatrics
- PICU
- Surgical services
*Nursing Solutions, Inc., retention rate for newly licensed nurses in 2022 was 77.5%.
NICU = neonatal intensive care, PICU = pediatric intensive care, TTP = Transition to practice
TTP committee leaders found curriculum objectives consistent with critical thinking, foundational knowledge, and practical application. Legacy NRP delivery models differed with a combination of in-person, instructor-led, virtual instructor-led, self-paced modules, and simulation. During analysis of the integration assessment data, the committee identified best practices and top-performing topics from each program.
At the same time as this analysis, the ANCC updated the Practice Transition Accreditation Program® Application Manual. In late 2023, the ANCC granted early access to the restructured manual to established programs. The new version of the manual provided the basis for the health system’s redesign process.
In April 2023, the TTP committee’s review of enrollment practices revealed regional variations. For example, legacy programs enrolled NLNs with 6 months to a year of practice. After reviewing best practices, including definitions and criteria from each legacy program and the ANCC Practice Transition Accreditation Program requirements, the committee agreed to define an NLN as an RN with less than 6 months of experience who graduated from an accredited school of nursing. To guide NRP topic selection, the committee assessed the current literature, results from the legacy program content inventory, topics required for practice transition accreditation, the nursing strategic plan, concerning data trends, and best practices.
In a pre-work email poll, TTP committee members ranked the order of the didactic program topics from the first session to the last. A review of the literature, as well as the ANCC Practice Transition Accreditation Program requirements, group consensus, and special regional needs, guided topic cadence. Committee chairs met separately to provide the larger committee with program model options, including best practices integrated from legacy programs and the literature.
The TTP committee selected monthly sessions for 6 months as the program model. This model aligns with ANCC Practice Transition Accreditation Program requirements and has been successfully implemented in a legacy region where the condensed format improved program completion rates without negatively impacting overall retention.
Committee chairs met offline to develop an overarching implementation timeline and presented the recommendations to the two health enterprise vice presidents of nursing education and the nursing professional development council. Everyone supported and embraced the proposal for a 6-month residency model, planned curriculum, and proposed implementation timeline.
Stakeholder assessment
In July 2023, the TTP committee received permission from Failla and colleagues to use the valid and reliable NRP Stakeholder Evaluation Survey as a program evaluation tool. This survey gathered feedback to help the committee design and implement a standardized NRP and provide an opportunity for self-assessment of current and former NLNs.
The survey collected demographic, qualitative, and quantitative data. Over 3,000 NRP stakeholders (including hiring leaders, preceptors, and nursing professional development specialists) received the survey; 1,265 completed it. The collected qualitative and quantitative data shed light on stakeholders’ perceptions of topic significance. (See Survey: Topic results)
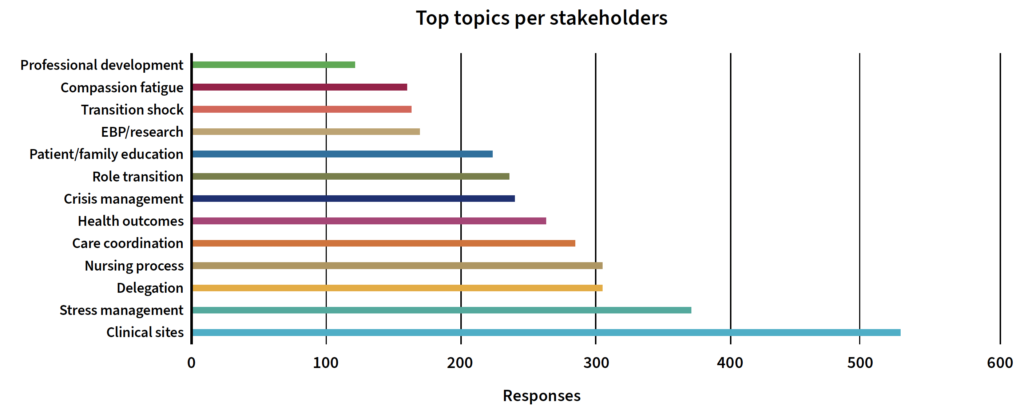
Survey: Topic results
The Nurse Residency Program (NRP) Stakeholder Evaluation Survey asked 3,000 NRP stakeholders to rate session topics; 1,265 completed the survey. Clinical skills received the highest rating, followed by stress management and delegation. The following graph provides an overview of top-performing topics.

The TTP committee finalized the curriculum based on the stakeholder survey results and initial committee topic selections. To determine the amount of time for each topic, the committee reviewed the NRP integration assessment and learning objectives. The committee compiled the information using Microsoft’s Power Business Intelligence dashboard, allowing the team to visualize commonalities and differences across regions.
After reviewing the findings, the committee recommended times that ranged from 15 to 45 minutes per topic. A sub-team developed overarching program goals and outcomes based on ANCC Practice Transition Accreditation Program requirements, including nursing professional development, learner competency, self-report, stakeholder evaluation, and financial goals. (See the Final Curriculum)
Final curriculum
The final nurse residency program curriculum includes the following sessions.
- Introduction and role transition
- Peer support
- Professionalism
- Well-being
- Communication
- Interprofessional teamwork
- Nursing scope and standards
- Critical thinking
- Time management and delegation
- Care coordination
- Diversity, equity, and inclusion
- Patient and family education
- Social drivers/determinants of health
- Ethics
- Health outcomes
- Peer support
- Workplace violence
- Peer support
- Professional development
- Mentorship
- Well-being
Measurement
The TTP committee assessed the literature for current NLN progression surveys and chose the Casey-Fink Graduate Nurse Experience Survey to guide participant progress throughout the program. The survey consists of two main sections. The first section evaluates role confidence, role satisfaction, stress/burnout, resiliency, organization commitment, and preceptorship. The second, evaluates confidence and nursing skills.
The survey developers recommend administering the tool within the first weeks of joining the program, at the midway point, and at program conclusion or at the end of the first year of practice. After discussion with one of the developers and consideration of the truncated 6-month NRP experience, the committee elected to administer the survey 2 months into the program and at the conclusion.
Content development
The TTP committee completed a reference survey to identify top areas of interest and expertise for content development. Next, the committee selected content development teams, which coordinated meetings; reviewed content, policies, and practice standards; consulted with subject matter experts; identified learning objectives; and created final content.
The content development teams used the ADDIE (Analysis, Design, Develop, Implement, Evaluate) model and Benner’s Novice to Expert theory as frameworks to guide the creation of session content, data collection, and analysis. The ADDIE model, developed by McGriff, aims for a learner-centered rather than a traditional teacher-centered approach to instruction. Benner’s Novice to Expert theory provides the overarching ideological structure; whereas the ADDIE model correlates with feedback from the stakeholder survey, which identified the need for more personalization throughout the NRP.
Content development teams provided updates and reports to the TTP committee and facilitated a peer review process for each session. During this process, development teams proposed ideas to the committee, subject matter experts, and nursing professional development peers, who incorporated it into session content.
Implementation
Content implementation throughout the enterprise required a multifactorial analysis of each site. Facility size, location, and available resources served as compelling factors when determining the number of NRP cohorts needed per month and year and the content facilitation methods best-suited to accommodate their needs and resources. (See Region cohort comparison)
Region cohort comparison
The following table provides an average annual comparison of the legacy nurse residency programs by region.
NLN = newly licensed nurse
Each region uses the same master slide deck, structured approach, and facilitator guide to deliver content for each session. The ANCC Practice Transition Accreditation Program requires program and curriculum standardization to ensure program consistency and quality.
Facilitators teach each 2-hour session in consecutive order. Participant polls, audience response systems, and live interaction encourage engagement. Participants receive 12 hours of didactic learning and an average of 14 weeks of precepted clinical time under the revised model. Routine NRP quality assurance audits conducted by program directors and bi-annual reviews validate uniformity of material and ensure integrity maintenance.
Revision process
The bi-annual review process ensures that content within the NRP is based on the most recent evidence available, consistently delivered across the enterprise, and aligned with the ANCC Practice Transition Accreditation Domains: Program Leadership, Program Goals and Measures, Organizational Enculturation, Development and Design, and Practice-Based Learning. The first bi-annual review occurred in fall 2024 and resulted in minor enhancements, including course material handouts, updated screenshots or links included in the slides, and slide formatting. Subsequent reviews will occur biannually in May and October along with additional reviews as necessary to align with relevant policy updates and enterprise priorities.
Outcomes
As each region facilitates NRP sessions, coordinators collaborate to identify content strengths and opportunities. Sharing facilitation experiences allows for efficacy and improvements in real-time and promotes success for upcoming sessions. Evaluations administered at the end of each session and tracked through a standardized tool provide participant data. Using a five-point Likert scale, participants rate their satisfaction and engagement with the content as well as their overall satisfaction with each session. Free text comments inform prospective changes to future sessions. (See Participant feedback.)
Participant feedback
Newly licensed nurses complete evaluations at the conclusion of the nurse residency program. The following table provides an overview of the integrated/standardized NRP outcomes to date (Jan 2024–March 2025).
- Appreciate peer support opportunities and well-being moments
- Interest in clinical skills
- Importance of conflict resolution, setting boundaries, personal growth, and awareness
- Appreciate peer support focus
- Understanding the importance of critical thinking and the nursing process
- SDOH awareness
- Highlighted need for patient-centered care based on cultural background and differences
- Advocating for patient autonomy and safety
- Supporting colleagues facing challenges
- Self-care focus
Top topics
- Care coordination
- Communication
- Critical thinking
- Ethics
- Peer support
Learning experience = percentage of respondents who felt the learning experience related directly to the course objectives; Overall rating: 1=Completely unsatisfactory, 2=Less than satisfactory, 3=Satisfactory, 4=More than satisfactory, 5=Outstanding; NRP = nurse residency program, SDOH = social determinants of health
Monitored outcomes align with the domains of ANCC Practice Transition Accreditation. Upon completion of a development pathway, NLNs reflect on their professional goals, identify career aspirations, and outline a plan for achievement. Data analysis demonstrates that NLNs who completed the development pathway reported clearer career goals and made measurable progress toward achieving them, demonstrating the pathway’s effectiveness in supporting professional growth.
Stress and burnout levels for NLN participants were assessed at the beginning and end of the program using the Casey-Fink survey. Results from the Stress and Burnout subscale showed that mean scores at both time points remained below the program benchmark of 3.0, indicating overall low levels. Although the mean score increased slightly from program onset to completion, it didn’t exceed the benchmark. According to the survey guidelines, lower mean scores reflect lower stress and burnout. This subscale allows participants to report the impact of program demands and personal factors.
Program success requires stakeholder support and feedback. For example, feedback related to collaboration and interprofessional teamwork provides valuable information related to the NLN’s clinical performance, confidence, and competence. Stakeholder survey results demonstrated that increased support and collaboration, particularly in interprofessional teamwork, correlated with gains in clinical performance, confidence, and competence among NLNs.
The enterprise NRP has demonstrated strong retention outcomes, achieving 96.4% program completion since inception. The literature supports this program model. For example, Riches and colleagues noted that condensed, time-limited nurse residency programs can promote increased completion rates and retention without compromising role-transition quality. The 2024 program completion 96.4% rate surpasses the NSI National Health Care Retention & RN Staffing Report of 83.6% for the same period.
Before integration of the new NRP, content delivery took an average of 24 hours. The revised approach enhanced efficiency of the enterprise-wide process and achieved savings of 12 hours per resident and facilitator, ensuring a consistent delivery time of 12 hours across all regions. Initial calculations of the legacy programs for 2,747 NLNs and facilitators for 24 hours of class time netted a cost of $2,742,399 annually. Return-on-investment estimates for this modification resulted in annual savings of $1,337,200 or $500 per participant. This cost savings reflects the difference in salaries for the NLN and facilitators after the standardization process. This figure accounts for the time and salary savings for 10 facilitators for five sessions and the salaries for 2,747 NLNs per year.
Future considerations
TTP committee members remain steadfast in their commitment to continuous NRP improvement. As the program evolves, the system must align with ANCC Practice Transition Accreditation Program standards, survey results, and specialty curriculums.
All nonaccredited sites should consider practice transition standards. At the onset of integration efforts, not all sites had received accreditation; however, they’ll all be included in the 2026 ANCC Practice Transition Accreditation Program self-study document. The ANCC states that NRPs using the Practice Transition Accreditation Program standards must be robust and comprehensive to aid NLN transition into and within the profession. According to Cosme, NRP directors use these standards as benchmarks to model program excellence and rigor.
Casey-Fink participant survey results indicate that program facilitators demonstrate their commitment and dedication to ensuring program and NLN success. The program will give future consideration to NLN assessment using the Casey-Fink 1 year from date of hire for continued transition monitoring.
The TTP committee aims to equip NLNs with tools and resources for career success through the addition of specialized curriculums within the program. Evaluating legacy offerings will help the committee create a standardized specialty curriculum to enhance the generalized NRP. Identifying common practice settings and establishing consistent operational methods also will take precedence in the development process.
Other potential challenges include inconsistent resources for program delivery among the regions. TTP Committee members must remember that each region within the NRP maintains varying levels of support. To avoid concerns with adequate internal assets, each region has flexibility in delivery methods to best support their unique situation.
Equipping nurses for the future
The enterprise-wide NRP analyzed legacy programs, evaluated stakeholder surveys, reviewed literature, adhered to ANCC Practice Transition Accreditation Program Standards, and applied adult learning principles. Its primary objective remains to enhance operations across all regions by faciliating the transition of NLNs to new practice settings.
This new NRP presents opportunities for the enterprise and NLNs. Equipping NLNs with necessary expertise and acumen will shape the future of nursing and healthcare.
Julie Padilla and Veronica Bigott are nursing professional development program managers at Advocate Health in Charlotte, North Carolina. Molly Eady is a nurse educator specialist at Atrium Health Navicent in Macon, Georgia. Stephanie Jenkins is a nursing professional development manager at Atrium Health Floyd in Rome, Georgia. Anika Lyerly is a nurse manager at Atrium Health Wake Forest Baptist in Winston-Salem, North Carolina. Tamika Moore is program coordinator of the new graduate nurse residency program, nurse extern program, student nurse pathway, and recruitment at Atrium Health Wake Forest Baptist. Stephanie Zidek is the executive leader for nursing professional development executive leader program at Advocate Health.
American Nurse Journal. 2026; 21(4). Doi: 10.51256/ANJ042606
References
American Nurses Credentialing Center. 2024 Practice Transition Accreditation Program® Application Manual. nursingworld.org/organizational-programs/accreditation/ptap/download-ptap-manual
Benner P. From Novice to Expert: Excellence and Power in Clinical Nursing Practice. Boston, MA: Addison-Wesley Publishing; 1984.
Casey K, Fink RM. Casey-Fink Graduate Nurse Experience Survey. 2023. caseyfinksurveys.com/surveys
Casey K, Fink RM. Revisions to the Casey Fink Graduate Nurse Experience Survey reflect current healthcare trends. J Nurs Adm. 2021;51(5):233-4. doi:10.1097/NNA.0000000000001004
Cosme S. Transition to practice accreditation: Raising the bar in nursing excellence. J Contin Educ Nurs. 2023;54(3):101-3. doi:10.3928/00220124-20230214-02
Failla KR, Ecoff L, Stichler JF, Kendal C. Psychometric testing of a nurse residency program stakeholder evaluation survey. J Nurses Prof Dev. 2021;37(6):353-7. doi:10.1097/NND.0000000000000797
McGriff SJ. Instructional System Design (ISD): Using the ADDIE Model. College of Education, Penn State University. 2000. snazlan.wordpress.com/wp-content/uploads/2017/03/instructional-system-design-isd-using-the-addie-model.pdf
Nursing Solutions Inc. 2025 NSI National Health Care Retention & RN Staffing Report. nsinursingsolutions.com/documents/library/nsi_national_health_care_retention_report.pdf
Riches C, Pitt R, Tyler S, Wise M, Watman P, Henderson A. Comparative analysis of newly graduated nurse support through periods of turmoil: Lessons learnt for building a future workforce for uncertain times. BMC Nurs. 2024;23(1):796. doi:10.1186/s12912-024-02460-4
Key words: transition to practice, newly licensed nurse, nurse residency program