Job Search
Whether you’re looking for your first nursing job or deciding to make a move after years in the same place, tips about job searches, resume writing, and interviewing techniques will only help. Take the time read more and find out how to use current technology to improve your prospects
PART 4 – OSTEOPOROSIS, THE SILENT EPIDEMIC
The
direct relationship between failing ovarian function and an increase in bone
loss and fractures was one of the earliest observations in the history of the
science of endocrinology.SKELETON (BONE): Here is
one part of the body that is dramatically impacted by hormones. I always quote
a question I once heard a friend of mine’s 12-year-old son ask him: “Dad, why
are grandmas always so short?” Let me explain why.If you
have ever seen or felt a real skeleton, the thought must cross your mind that
bone is a pretty permanent substance; once developed, never changing. This is
just so far from the truth. Like every other part of the body, bone is dynamic.
It is constantly renewing itself in a process called bone remodeling.Bone
remodeling is a delicate balancing act. As bone ages, it becomes brittle, and
brittle bones break more easily. The body needs to get rid of the brittle bone
and replace it with new strong and flexible bone. This balance is maintained by
a process that has to take out the old bone (bone resorption) and replace it with new bone (bone deposition).As a
child grows, there is a heavy emphasis on building new bone. Under normal
circumstances, this positive balance of more bone deposition than resorption
will go on into the late 20s and early 30s when the individual reaches peak bone mass. This is a time when we
have the most bone in the bank that we will ever have. The amount of bone will
be determined by many factors including genes, sex (men have more bone than
women), diet (good protein, calcium, mineral and vitamin intake), vitamin D,
exercise and activity, and so forth.After a
plateau in middle age, the balance begins to go the other way, and aging is
associated with losing more bone than making it. If this negative balance goes
too far, so much bone is lost that it now has the risk of breaking (fractures), and we call this condition
of abnormal low bone mass or bone thinning osteoporosis.
Both men
and women lose bone as they age. Risk factors that increase the likelihood of
developing osteoporosis include family history, sex, race, age of menopause,
diet and nutrition, smoking and alcohol abuse, taking corticosteroid drugs such
as for asthma, and chronic diseases, for example of the kidney or thyroid.Women are
unfortunately at greater risk of developing osteoporosis for a number of
reasons:1. They
start with less bone in the bank than men.2. They are
the stronger sex and live longer, giving more time for the gradual loss with
aging to accumulate.3. Estrogen
plays a key role in preventing bone loss. The reduction of estrogen at
menopause results in a few years of rapid
bone loss – in 5 to 7 years, up to 10% of the skeletal bone mass can
disappear.Brittle
osteoporotic bone is more likely to break. This can result from a fall, or from
something as simple as a bump in the road. More than half of American women
over 50 demonstrate bone loss – over one-third will eventually have problems.
Postmenopausal osteoporosis is associated with over a quarter million hip
fractures a year, costing our health system over 15 billion dollars every year.
But the real cost is in human terms – one in two women will lose independent
living after a hip fracture and a quarter of those will never leave nursing
institutions; 10% die within 12 months.The
spinal bones (vertebra) can break
silently. What happens is that any extra pressure on the weakened bones results
in them compressing or crushing. Simply stepping off a sidewalk could do this.
As the vertebrae crush, the spine curves forward and the result may be the
so-called “dowagers hump.” Not only does this drop the bottom of the rib cage
in front lower toward the top of the pelvic bone, giving a bulge of the
stomach, but it also results in loss of height – thereby giving the answer to
the question posed by my friend’s son.Unfortunately,
crush fractures of the vertebrae can also be associated with terrible back
pain. This can be so severe as to literally immobilize a woman, and in many
instances is the difference between independent living and moving into an
institution.This
human tragedy following fractures of the hip and spine is largely preventable.
There have been huge strides in our knowledge about the problem, and several
families of new drugs have been developed to prevent or treat established
osteoporosis. All about this later…TEETH: The jaws are bone, and
teeth are really a kind of specialized bone. Tooth loss after menopause results
from atrophy (shrinkage) of the bony tooth sockets. This in turn leads to
retraction of the gums, the non-enamel part of the teeth getting exposed, and
bacterial invasion of little pockets that open up around the teeth. Indeed,
women with severe osteoporosis are three times more likely to have no teeth
than unaffected women.Prevention
of bone loss after menopause is truly necessary for good dental health.Coming
soon I will discuss treatments and the growing debate about bisphosphonates,
hormones, and other medications.Next week
will mark the tenth anniversary of the termination of the estrogen/progestin
arm of the WHI. I will have a lot to say about that!Have a
great week.Wulf Utian MD PhD DSc
Author; CHANGE YOUR MENOPAUSE – Why one size
does not fit all. http://www.amazon.com/Change-Your-Menopause-size-does/dp/0982845723/Click here for a limited offer for a free newsletter
FTC supports APRN practice in new report
The Federal Trade Commission (FTC) has released “Policy Perspectives: Competition and the Regulation of Advanced Practice Nurses (APRNs),” which cautions against legislators and policymakers taking actions that limit access to care provided by APRNs, including areas related to physician supervision. The report states, “expanded APRN scope of practice is good for competition and American consumers.” Read the report.
Releasing our attachments to the past
Jake, a critical care nursing director, works for a large healthcare system that has invested heavily in testing the use of robots to support operational tasks and provide new ways for physicians to interact with patients. During his monthly staff meeting, Jake presents an overview of the robotic products and what they’re designed to do. He’s surprised at how some of the senior nurses react; they immediately criticize the initiative as just another attempt to reduce staffing costs and dehumanize health care.
The meeting quickly lapses into a discussion of the “good old days” in nursing. Jake explains that the robotics venture is exploratory and the jury is still out on this cutting-edge technology. Although he supports his organization’s willingness to be an early adopter, some of his staff clearly feel otherwise. He realizes part of his role as a leader is to help them release their attachments to the past and embrace innovative changes.
Over the past decade, the pace of change in healthcare delivery has been relentless. Leaders like Jake have been challenged to help staff adapt to these changes. Tim Porter-O’Grady, an expert on organizational innovation, conflict, and change, observed that part of nurse leaders’ work is to “close the door on old models of health delivery and clinical work…and face the future viewing the entire landscape to develop a workable vision.”
Helping staff release their attachments to the past and embrace new innovations can be hard work, as Jake will learn. When we’re attached to something—be it a person, situation, or practice—we want circumstances to be a certain way and tend to resist changes in our expectations. Change can be quite emotional for some people. Often, it means letting go of something you’ve valued in the past.
Why we attach to the past
Life can be a delicate balance of holding on and letting go. Changing our viewpoints on issues or abandoning old behaviors involves both a loss of what was and a leap into the unknown. This can make us feel insecure about our work—and it can be exhausting. There’s safety in what we know and risk in what we don’t know.
For some people, it’s a challenge to think positively about the creative possibilities that accompany innovation. That’s why the reaction to any change can be so emotional. Nursing staff may worry that introducing robots into health care could mean fewer jobs. Older nurses may feel insecure about their technological skills and lack confidence in their ability to master new products or processes. In contrast, younger nurses who grew up in the digital age view technology as an integral part of their work and may react differently.
Five strategies to help staff let go
Jake needs to understand that as a leader, he plays a key role in framing the context of change for his staff. His support of his organization’s new initiative is important in gaining staff buy-in and can help his staff release their attachments to old ways of delivering care. Introducing robotic products into the workplace involves what management educator Barbara Mackoff describes as an adaptive change. This type of change requires us to let go of old ideas and experience some uncertainty and loss in what’s comfortable. To help staff let go, use these five leadership strategies.
1 Meet staff where they are in the acceptance and transition process.
Not everyone accepts change in the same way or on the same timeline. Leadership expert Kerry Bunker suggests that to avoid frustration, we must meet people wherever they are in the change process. Accept that some people won’t be as far along as you might want them to be. Where they are depends on their comfort with change (ability to take on new learning) and capacity for change (ability to learn what’s required). As a leader, you need to accept where people are in the acceptance process.2 Frame the issues in easily understood language.
With the changes stemming from healthcare reform and declining reimbursements, organizations have good reason to look for new and different ways to innovate their care delivery. Jake should frame the robotics initiative as an innovative way to help his staff see the need for new technologies. Staff depend on their leaders to help them understand the meaning of innovations. How leaders use language to frame people, situations, and events has important consequences for how staff make sense of the world and their actions.3 Recognize people have different responses to change.
Bunker proposes that a person’s response to change can occur in four distinct patterns—entrenched, overwhelmed, poser, and learner. (See Four responses to change.)4 Help people identify where and how they can fit into the change.
In most situations where we’re asked to change, we’re replacing the old with the new and unfamiliar. But change can lead to a new, brighter future—and leaders need to convey this. For instance, Jake can cite recent changes in the hospital environment, such as introduction of electronic health records and medication barcoding, to demonstrate to staff how they’ve been able to incorporate these innovations into their current practice successfully. Leaders who stay calm, truthful, and optimistic in their communications help prevent the spread of misinformation and reduce staff anxiety.5 Give people hope.
Every situation has a silver lining, and leaders need to be the first to help everyone see what it is. An optimistic attitude can be energizing and contagious, motivating your staff to do their best. To achieve success, you need to expect success.Focusing on the future
For many nurses with long careers, the chaos and complexity of today’s environment challenges the sense of order. When we feel fearful, clinging to what worked in the past can be comforting.
Leaders should be skilled in working in the present with an eye toward the future. When you think about the past, it’s good to reminisce but important to keep in mind the phrase, “That was then. This is now.” Here are three key ways to stay future focused.• Track trends. Major trends in our environment—work, home, or the world—almost always are preceded by many signs, large and small. If you’ve been paying attention to healthcare trends, such as use of robotic technology in manufacturing and operating rooms, applying this technology to other areas of health care shouldn’t be a surprise.
• Look for opportunities to reinvent. Management guru Peter Drucker said, “The best way to predict the future is to create it.” This is great advice. If things clearly are changing and innovation is needed, why not embrace the change and develop an innovator’s mindset? Just because you’ve been doing things a certain way doesn’t mean that’s the best way to do it now. When you’re passive about change, it’s easy to feel like a victim of what’s happening. You’ll be much more willing to embrace something you take an active role in implementing.
• Talk to younger nurses. Investing in relationships with younger team members helps you understand today’s environment. The pace of change in health care doesn’t seem to frustrate younger nurses. In their short careers, they’ve learned to adapt quickly to a rapidly changing environment. They’re full of optimism and can give you great hope for the future.The future belongs to those who create it
When talking to his staff about their attachment to the past, Jake could use the metaphor of a ship: When the ship has left the dock, you’re either on board or not. The ship won’t head back to port to pick you up.
Sometimes, life and work events match our desires; other times, they don’t. Surrendering our attachments to the past is a choice, but an important—and potentially liberating—one. Whenever you find yourself talking about the good old days of nursing, reflect on what’s to be gained by doing that and whether anyone’s listening. The future belongs to those who create it.
Rose O. Sherman is a professor of nursing and director of the Nursing Leadership Institute at the Christine E. Lynn College of Nursing at Florida Atlantic University in Boca Raton. You can read her blog at www.emergingrnleader.com. Portions of this article were published previously on the author’s blog. Note: Names in scenarios are fictitious.
Selected references
Bunker KA. Introduction. In: Rush S, ed. On Leading in Times of Change. Greensboro, NC: Center for Creative Leadership; 2012.
Kotter JP. Leading Change, With a New Preface by the Author. Boston: Harvard Business Review Press; 2012.
Mackoff BL. AONE leadership laboratory insights: the practice of change leadership. Nurs Lead. 2014;12(6):23-6.
Porter-O’Grady T, Malloch K. Quantum Leadership: Building Better Partnerships for Sustainable Health. 4th ed. Burlington, MA: Jones & Bartlett Learning; 2015.
Does evidence-based nursing increase ROI?
Catholic Health Initiatives (CHI) is committed to improving the patient and family experience through evidence-based practices (EBP) and other effective improvement strategies. Based in Englewood, Colorado, CHI is the third largest not-for-profit healthcare system in the United States, with more than 70 hospitals and 30,000 nurses.
Our EBP program aims to bring evidence-based care to the patient using systemwide standards of care, toolkits, education, organizational-level engagement, and metrics for determining clinical and fiscal impact. The program includes four clinical metrics and one financial metric for cost-of-care avoidance related to reducing preventable adverse events for which the Centers for Medicare & Medicaid Services no longer reimburses healthcare costs.
This article describes CHI’s cost-of-care metric for five healthcare-acquired conditions (HACs)—catheter-associated urinary tract infections, methicillin-resistant Staphylococcus aureus infections, Clostridium difficile infections, surgical "never" events, and patient falls. Our metric calculates cost savings when an HAC is avoided. Developed and successfully implemented within 18 months, this initiative serves as an organizational- and system-level vehicle for evaluating costs avoided by implementing specific care bundles for HAC prevention.
To help prevent surgical "never" events, CHI implemented the World Health Organization’s surgical checklist and recommended practices of the Association of periOperative Registered Nurses to reduce complications and death rates in patients undergoing surgery across a diverse group of hospitals. CHI also implemented a care bundle to prevent healthcare-associated infections, based on established guidelines from national sources, such as the National Healthcare Safety Network of the Centers for Disease Control and Prevention.
Cost avoidance plus cost savings
The Institute for Healthcare Improvement uses the term "dark green dollars" when quality-improvement initiatives yield cost savings that can be tracked to the bottom line through both cost avoidance and cost savings. At CHI, the average cost of each incident type was established during the planning phase of our initiative through an extensive review of empirical literature on cost averages associated with each HAC. This allowed us to establish a benchmark cost to gauge the return on investment (ROI) realized through cost avoidance. (See Costs for each healthcare-acquired condition by clicking the PDF icon above.)
Advancing understanding of data
Our cost-of-care calculator tool allows local and system-level users to understand the contributions of nurses and other caregivers to EBP, specific to care bundles and estimated cost avoidance when these bundles are used. Data transparency advances clinicians’ understanding of nurse-sensitive measures linked to ROI methodology and accountability.
Created with Excel Workbook, our cost-of-care metric was designed to measure organizational- and system-level estimated cost-avoidance costs by volume-of-event occurrences during baseline and measurement periods. In the metric, the volume of baseline-period event occurrences is multiplied by the estimated cost associated with one event occurrence, followed by subtraction of data for the measurement period.
HAC occurrences are reported quarterly using agreed-on formulas. The general formula for calculating cost-avoidance costs incorporates the numerator divided by the denominator, along with rate definitions and calculations for specific outcome metrics. (For detailed formulas used with each care bundle, see Formulas for calculating event occurrences.) At CHI, total system findings between the baseline and measurement periods for each of five care bundles implemented showed a 30% decrease in HACs, yielding an overall estimated cost avoidance of more than $8 million aggregated for fiscal year 2010.
CHI’s cost-of-care metric supports a culture of safety and nursing’s contribution to creating healthcare value. It focuses on the role of event prevention in improving patient outcomes during hospitalization, and links prevention with fiscal metrics in determining estimated cost avoidance. A synopsis of clinical outcome improvement and estimated cost avoidance provides compelling evidence that connects EBP to financial metrics.
Selected references
Aleccia J. Who foots the bill for medical mistakes? MSNBC; February 28, 2008. www.msnbc.msn.com/id/23341360/ns/health-health_care/t/patients-still-stuck-bill-medical-errors. Accessed November 14, 2011.
Allman RM, Goode PS, Burst N, Bartolucci AA, Thomas DR. Pressure ulcers, hospital complications, and disease severity: impact on hospital costs and length of stay. Adv Wound Care. 1999 Jan-Feb;12(1):22-30.
Anderson DJ, Kirkland KB, Kaye KS, et al. Underresourced hospital infection control and prevention programs: penny wise, pound foolish? Infect Control Hosp Epidemiol. 2007 Jul;28:767-73.
Association of PeriOperative Registered Nurses. Perioperative Standards, Recommended Practices and Guidelines 2010. Denver, CO: Author; 2010.
Bates DW, Pruess K, Souney P, Platt R. Serious falls in hospitalized patients: correlates and resource utilization. Am J Med. 1995 Aug; 99(2):137-43.
Centers for Disease Control and Prevention. Central line insertion practices (CLIP) adherence monitoring. June 2011. http://www.cdc.gov/nhsn/PDFs/pscManual/5psc_CLIPcurrent.pdf. Accessed November 22, 2011.
Dubberke ER, Reske KA, Olsen MA, et al. Short- and long-term attributable costs of Clostridium difficile–associated disease in nonsurgical patients. Clin Infect Dis. 2008 Feb 15;46:497-504.
Elixhauser A, Steiner C. Infections with methicillin-resistant Staphylococcus aureus (MRSA) in U.S. hospitals, 1993-2005. HCUP Statistical Brief #35. July 2007. Agency for Healthcare Research and Quality.
5 Million Lives Campaign. Getting started kit: Prevent central line infections; How-to guide. Institute for Healthcare Improvement. Last updated October 1, 2008. www.ihi.org/knowledge/Pages/Tools/howtoGuidePreventCentralLineAssociatedBloodstreamInfection.aspx. Accessed November 22, 2011.
5 Million Lives Campaign. Getting started kit: Reduce methicillin-resistant Staphylococcus aureus (MRSA) infection; How-to guide. Institute for Healthcare Improvement. Last updated December 17, 2008. www.ihi.org/knowledge/Pages/Tools/HowtoGuideReduceMRSAInfection.aspx. Accessed November 22, 2011.
Haynes AB, Weiser TG, Lipsitz S, et al; Safe Surgery Saves Lives Study Group. A surgical safety checklist to reduce morbidity and mortality in a global population. N Eng J Med. 2009;Jan 20:491-9. doi:10.1056/NEJMsa0810119.
National Quality Forum (NQF). Safe Practices for Better Healthcare–2009 Update: A Consensus Report. Washington, DC: NQF; 2009:279-83.
Schifalacqua MM, Mamula J, Mason AR. Return on investment imperative: the cost of care calculator for an evidence-based practice program. Nurs Adm Q. 2011 Jan-Mar;35(1):15-20. doi:10.1097/NAQ.0b013e318203227a.
Scott RD. The direct medical costs of healthcare-associated infections in U.S. hospitals and the benefits of prevention. Publication No. CS200891-A; March 2009. Centers for Disease Control and Prevention.
Marita MacKinnon Schifalacqua is a principal with M. Schifalacqua Consulting in Henderson, Nevada and a former vice president of evidence-based practice and clinical technology at Catholic Health Initiatives (CHI) in Englewood, Colorado. Sr. Maurita Soukup is a Health Trustee for Mercy Hospital in Sioux City, Iowa and Mercy Medical Center in Cedar Rapids, Iowa; she is also a nurse consultant/researcher in the areas of critical care and evidence-based practice. Wanda Kelley and Alison Rich Mason are clinical process specialists in evidence-based practice at CHI.
Analysis: Good communication enhances patient safety, satisfaction
A new report from HealthGrades finds that hospitals with the highest patient ratings in physician and nursing communications on average have fewer patient safety events. The report notes that 27% more overall patient safety events occurred in hospitals performing in the bottom 10% for nursing communication, compared to the top 10%. Read more.
On March 11, the U.S. Food and Drug Administration issued a warning about counterfeit surgical mesh being distributed under C. R. Bard/Davol brand name. Affected lot numbers are at: http://www.fda.gov/NewsEvents/Newsroom/PressAnnouncements/ucm204199.htm.
Role of the staff nurse in undergraduate nursing education
The staff nurse plays an integral role in clinical nursing education, helping to prepare undergraduate nursing students for professional practice. A positive and enriched learning environment can influence a student’s perception of the healthcare facility as a possible future employment site. As healthcare reform continues to alter the healthcare workforce, providing positive clinical learning experiences can aid recruitment of future nursing staff.
But while many staff nurses find the teaching role satisfying, others don’t see it as their responsibility. Greater patient acuity, high nurse-to-patient ratios, and increased workloads stop some nurses from participating in students’ education.
The student-staff nurse relationship profoundly affects learning. Not all staff nurses have formal preparation for the role of mentor or are responsible for evaluating a student’s clinical performance. Staff nurses are meant to be resources for students when faculty members are unavailable. They also serve as nursing role models and educational facilitators of practical nursing skills. This socialization into the profession is a crucial component of the student’s education.
Practice makes perfect
Applying classroom concepts to actual practice is an exciting and anticipated part of the curriculum for young, eager nursing students. They arrive with theory, knowledge, and simulated laboratory experience, ready to practice nursing skills on real patients.
Partnerships between staff nurses and students
Nursing students are partnered with staff nurses as an extension of the learning model and are supervised by a faculty member. A positive experience in the clinical site with a dedicated, kind, nurturing role model can promote learning. A negative experience with an overburdened, unpleasant, uninterested mentor can impede learning.
Clinical preparation is crucial. Hospital surveys have shown new nurses have high expectations. Many staff nurses, on the other hand, believe nursing education programs don’t adequately prepare new staff for increased patient acuity and blame a lack of clinical-skills preparation. Yet some of these same nurses dislike teaching nursing students.
Students’ attitudes and expectations also affect clinical learning. How strong is the student’s desire to learn? Is the student self-directed? New learners lack experience, which contributes to increased stress. They’re also less self-directed and need more nurturing and structure in their learning environment. Undergraduates tend to focus narrowly on basic tasks and skills; experienced nurses see the broader picture.
Clinical settings place a high priority on clinical competency. Yet new learners may be awkward and slow, which can frustrate a hurried clinician. Effective mentors have such characteristic behaviors as guiding, cooperating, supporting, and listening actively. (See Effective mentoring behaviors by clicking the PDF icon above.) When staff nurses lack these characteristics, nursing students may be afraid to ask questions and may lose their confidence. If these mentoring deficiencies persist throughout the student’s clinical experience, it creates a poor learning environment for everyone. On the other hand, if a mentor interjects simple praise or suggestions, such as “Take your time, you’re doing fine” or “Try positioning the lead farther over here,” this may calm the student-and reassure the patient that the clinical situation is under professional supervision.
Clinical teaching challenges
Many challenges exist in clinical teaching. Some challenges, such as lack of clinical sites and poor attitudes from patients, are outside educators’ control. Students and faculty also face obstacles from within. Although staff nurses work closely with students, few are adequately prepared or formally recognized for their role as clinical facilitators.
Responsibilities of educational and clinical institutions
The learning experience is richer when administrators believe the staff nurse plays a critical role in improving the quality of nursing education. Hospitals and other healthcare employers must be held accountable for providing these educational experiences.
Partnerships between staff nurses and clinical faculty should be cultivated so both groups can foster a culture of learning and support. To bridge the gap between education and practice, educational institutions should implement some form of educational preparation for staff nurses who are acting as preceptors for students.
Student responsibilities
Students need to be respectful and courteous to teachers. Sometimes, a hospital unit has as many nursing students as clinicians. Even small niceties, such as students offering staff their seats in crowded places or recognizing the need for quiet conversations in areas reserved for charting, show a respectful attitude toward their nurse-teachers.
Also, students should refrain from challenging mentors by saying, for example, “My teacher says it should be done this way.” The student’s role is that of learner, not critic. Students should appreciate that they’re guests of the facility and make sure their behavior shows they understand this concept.Recognizing staff nurses’ contribution
Observing all aspects of professional nursing is educational for students. This includes observing interactions among staff nurses and colleagues, physicians and other healthcare providers, support staff, patients, and visitors. Discussing these observations in postconference debriefings held with faculty and students immediately after clinical experiences provides important learning opportunities, whether perceived as positive or negative.
Students and faculty should recognize all clinical experiences by acknowledging the staff nurses’ efforts to mentor students. Whether it’s a small gesture (such as a written thank-you note or a home-baked or store-bought treat from students) or something more formal (such as a staff nurse-appreciation luncheon hosted by the educational institution), all thoughtful actions go a long way toward recognizing staff nurses’ contributions to clinical nursing education.
Educating future caregivers
Staff nurses are educators by definition. They educate patients, families, the community, and each other. We need to help them realize they have a vested interest in their vital teaching role, because today’s nursing students are tomorrow’s caregivers.
Transitioning from nursing as a collection of skills learned from a textbook to nursing as a profession in a peopled work setting is difficult, at best. How can we foster professional growth in nursing students? Staff nurses and clinical faculty strive to balance academic and clinical knowledge in daily nursing practice. Giving students learning opportunities to find this balance is a key component of clinical education—and the staff nurse plays a critical role.
Staff nurses should value and recognize their role in ongoing development of future nurses. Of course, staff nurses vary in terms of educational personalities. Some are more productive educationally to students than others; those who’ve received little or no formal training in teaching and mentoring students may be ill prepared for this role. With even minor improvements in the educational atmosphere-including positive attitudes from staff, students, and administrators-staff nurses will be able to more fully appreciate and enjoy their important contribution.
Click here for a complete list of references.
Kathleen A. Ahonen is an assistant professor at the University of Toledo College of Nursing in Toledo, Ohio, and maintains a part-time practice as a women’s health nurse practitioner (NP). Colleen M. Quinlan is an assistant professor at the University of Toledo College of Nursing and a certified women’s health care NP.
Letters to the Editor – March 2009
Avoiding the dangers of I.V. phenytoin
As an infusion nurse specialist, I’d like to add some information to and clarify some points in “Phenytoin: Keep patients in the range and out of danger” in the January 2009 issue. The author recommends giving phenytoin through a central venous catheter, a good practice, but she didn’t mention the importance of assessing for a brisk blood return before administration. Certain factors can alter the fluid pathway, causing a retrograde flow and leakage of this vesicant drug into the subcutaneous tissue. Because of this danger, a nurse should also frequently check for blood return during the infusion—even when using an infusion pump. Remember, a pump can keep pumping an extravasated drug without sounding an alarm.
For peripheral administration, many sources recommend a large catheter, such as an 18-gauge catheter. But an infusion nursing standard of practice is to always use the smallest gauge catheter capable of delivering therapy. A large catheter can alter blood flow through the vein, reducing the amount of blood available to dilute the drug. It can also cause mechanical and chemical vein irritation and increase the risk of thrombosis distal to the venipuncture site. All these factors increase the risk of extravasation injury. To avoid this complication, I would use a 22-gauge or 24-gauge catheter, frequently assess for a brisk blood return, and flush the catheter with 10 mL of normal saline solution before and after administration. As the author points out, I.V. administration of phenytoin always requires a 0.22 micron in-line filter. I would add that filters may easily clog with drug precipitate and should be replaced if occlusion occurs.
Lynn Hadaway, MEd, RN, BC, CRNI
Milner, GAEditor’s comment: Now that generic fosphenytoin is available, the Institute for Safe Medication Practices recommends using it instead of I.V. phenytoin to avoid these complications.
Foreign nurses: A question of education
I read “Short-term solution to our shortage” in the November 2008 issue’s Letters to the Editor, and I agree that nursing education is a vital solution to the shortage. But I don’t agree with the suggestion that hiring nurses from other countries puts patients at risk.
Nurses educated outside the United States are subject to the same standards of practice as nurses educated in this country. Plus, many of these nurses undergo difficult training, earn bachelor’s degrees, and pass numerous board and proficiency exams. All nurses are worthy of the respect of the public and other nurses.
Johanna Divinagracia, BSN, RN
New York, NYDocumenting our stories
I enjoyed the thought-provoking Editorial, “Telling our story” in the January issue and would like to share some suggestions. To make our accomplishments known, we must collect and publish value-added outcome data. Our traditional missions include providing patients and family members comfort, realistic hope, and appropriate alternatives. We accomplish these missions daily, but we don’t document an increase in our patients’ comfort or hope. Nor do we document our suggestions for alternative therapies when a patient faces a difficult regimen. And we don’t document whether a patient adopted our suggestion and whether or not it worked.
Nurse administrators should track data about strategies they use to effectively orient, reward, and retain good nurses. These strategies include making staffing decisions based on patient and family needs and creating work schedules based on needs of nurses. Outcome data about such decisions, including attendance, overtime, and retention, must be published to share what works.
Data on patient and management outcomes are more likely to show positive changes if they are based on a shared theory of nursing, in which all healthcare team members are invested. To collect value-added patient data, we need to devise mechanisms for charting. When medical records show positive outcomes and they are publicized, nurses will be telling their stories effectively and credibly.
Dr. Kathy Kolcaba PhD, RN
Chagrin Falls, OHCorrection: In the January 2009 issue, the table on page 20 called “Interpreting arterial blood gas values” has two incorrect values. The compensation value for metabolic acidosis should be Paco2 < 35 mm Hg, and the compensation value for metabolic alkalosis should be Paco2 > 45 mm Hg. Visit www.AmericanNurseToday.com/journal for a corrected PDF.
We welcome your comments. You may submit letters to the editor electronically at www.AmericanNurseToday.com/letters. Or you may send them by regular mail to: Letters to the Editor, American Nurse Today, c/o HeatlhCom Media, 259 Veterans Lane, 3rd Floor, Doylestown, PA 18901. Please include your full name, credentials, city, state, and daytime phone number or e-mail address. Letters should contain no more than 250 words and will be edited for grammar, length, content, and clarity. All letters are considered American Nurse Today property and therefore unconditionally assigned to American Nurse Today.
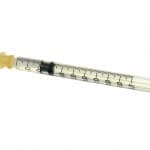
Safe sharps disposal in the home
More than 7.8 billion needles are used each year by the 13.5 million people who self-inject medications outside of a healthcare setting. That 7.8 billion number doesn’t take into account the lancets that are used by those with diabetes who test their blood sugar. Self-inject medications are used for treating a wide range of conditions, including osteoporosis, multiple sclerosis, HIV, AIDS, hepatitis C, migraines, cancer, kidney disease, and psoriasis. In addition, patients administer blood thinners, growth hormones, infertility drugs, vitamin B-12, and allergy shots. As the number of drugs injected at home continues to grow, the use of sharps in the home will dramatically increase as well. Where will all these needles go? Too many times, patients throw them in the trash, creating significant health concerns.
Scope of the problem
Upon discharge from a hospital, long-term facility, or a homecare agency, patients may be given a needle disposal container, but facilities for needle disposal are often not available, as only few states have needle disposal programs or options for disposal other than household trash. Previously, hospitals and doctors’ offices were willing to accept this as medical waste, but due to the high cost of medical waste disposal this courtesy is usually no longer available.
As a diabetes educator, I find it amazing that patient’s may dispose of the needles, syringes, and lancets in the household trash or into the sewage system. Typically needles, syringes, and lancets are placed in soda bottles, coffee cans, and detergent bottles and then disposed of in household trash. This trash is then compacted, crushing the container and spilling needles into the landfill or clogging conveyor belts, requiring sanitary workers to hand pick syringes with exposed needles out of the system.
This is serious health concern for many individuals who are untrained regarding the health risk to which they are exposed on a daily basis. A surprise encounter with a used syringe, needle, or other sharp in a playground, park, or at work can provoke intense fears of injury and life-threatening infections. If a needle stick injury occurs, the costs of providing post-injury counseling and prevention measures are significant. While there are limited data on these occupational and nonoccupational risks, problems that can arise from unsafely discarded used sharps include needle stick injuries and potentially fatal blood-borne infections.
Coalition for Safe Needle Disposal
As nurses, we have lobbied long and hard for safe needle and sharp safety in hospitals. We now need to raise awareness in communities, local governments, and state governments about the need to provide a safe needle disposal option in communities, and we need to educate the public on the problem and possible solutions.
The Coalition for Safe Needle Disposal encourages grass-roots efforts to be organized by stakeholders throughout the United States. The Coalition hopes to raise awareness of the need for proper needle disposal programs to be established in all communities. It is vital that all healthcare providers become involved as they play an important role in awareness campaigns, in forging of partnerships, and in changing regulations, policies, and laws to guarantee access to safe disposal programs.
In 2004, the Environmental Protection Agency (EPA), in collaboration with the Coalition for Safe Needle Disposal, published new guidelines for safe needle disposal outside traditional healthcare settings. The guidelines request that individuals using sharps participate in a safe needle disposal program and not throw needles, syringes, or lancets into household trash.
These new recommendations are found in the publication “Protect Yourself, Protect Others: Safe Options for Needle Disposal” (http://www.epa.gov/osw/nonhaz/industrial/medical/med-home.pdf) and a second publication “Community Options for Safe Needle Disposal,” (http://www.epa.gov/osw/nonhaz/industrial/medical/med-govt.pdf) which provides information for local governments on the establishment of needle disposal programs in their community.
Unfortunately the EPA, a regulatory agency, has no power to enforce laws or write regulations although it may make recommendations. Therefore, it is the responsibility of local governments, communities, and waste management programs to establish programs. Few states have passed any legislation or instituted any regulations regarding needle disposal programs outside of healthcare settings. As awareness of this problem has increased, some hotels and public facilities have opted to provide needle disposal systems in restrooms in an effort to protect their employees. These facilities contract with a medical waste disposal company to monitor these systems. Some hotel chains offer needle disposal containers to those who request the service.
Unfortunately, laws and regulations governing medical waste (including needles and other sharps) were primarily designed for healthcare facilities and medical waste operations. These laws and regulations can hinder community efforts to gather and consolidate household sharps for safe disposal as medical waste, for example, at fire stations or pharmacies.
Most people who give themselves injections have received limited and at times contradictory guidance about safe disposal of used sharps. Physicians, pharmacists, and diabetes educators, to whom they would most likely turn for help, are often uncertain of what to advise. For illegal drug users, the criminal penalties for syringe possession are strong disincentives to safe disposal of their potentially infectious used syringes and needles. Many are unwilling to participate in safe disposal because of the real risk of arrest for possession of drug paraphernalia.
A complete listing of all state laws and regulations can be found on the Coalition for Safe Community Needle Disposal website.
Needle disposal options and programs
Several options for disposing of needles outside of a health-care setting exist.
Community-based programs
Community-based programs offer drop-off locations for used needles. Drop-off programs may exist at police stations, fire stations, physicians’ offices, hospitals, clinics, health departments, or medical waste facilities. An example of a community-based effort is found in New York State, which uses a program available through Chrysalis Environmental Services. This company, which produces products, services, and educational programs to ensure the safe and environmentally friendly disposal of residential medical waste, has established a kiosk program, a joint effort between participating pharmacies or other organizations, and a medical waste hauling company. As part of the program, electronic kiosks, called “Zeedles,” are placed in facilities to accept residential medical waste. Individuals may dispose of their used needles and syringes in a needle disposal container or into a container a home that they drop it into the kiosk. Additional information about the program is available at http://www.aboutneedledisposal.com
Residential pickup
Residential special waste pick up works well in small communities. Special recycling containers are placed outside the home to be picked up by trained waste workers. This may be done on a regular schedule or as a requested service.
Syringe exchange
Syringe exchange programs allow illegal drug users to exchange used syringes and needles for new ones. The used needles are then properly discarded at a medical waste collection site. These types of programs are usually run by nonprofit groups and are frequently not publicized. They offer educational programs and services for people with HIV and AIDS. For more information on the availability of a needle-exchange program in your area, contact the North American Syringe Exchange Network at 253-272-4857 or online at www.nasen.org.
Hazardous waste collection
Household hazardous-waste collection sites are similar to a recycling center, in which needle disposal containers are placed in a designated medical waste collection container. Many of these programs provide a new sharps container when a person disposes of his or her used container. Sharps containers may be purchased at a local drug store or durable medical equipment company.
Needle destruction devices
Needle destruction devices are available for use in the home. These devices bend, break, or shear the needle. However, the problem still exists as to what to do with the needles, and this solution does not work well for lancets.
Mail-back programs
Some companies offer a sharps container mail-back program in which a sharps disposal container is purchased at a pharmacy or a durable medical equipment company. An additional charge is added to the price of the container to cover the cost of a mailing envelope provided to ship the container to a medical waste facility. Unfortunately, this program is not covered by insurance and the patient is required to pay for the needle disposal container and the mailer, further increasing their financial burden. Patients taking Humira (Abbott Labs) are eligible for a free mail-back program by calling 1-800-448-6472 or signing up on line at http://www.myhumira.com/Disposal/Default.aspx. Patients taking Simponi (Johnson and Johnson) are eligible for a free mail-back program by calling 1-877-697-4676 or signing up online at
http://www.simponi.com/rheumatoid-arthritis/get-support/treatment-support/safe-returns.What should you tell your patients?
Learn what needle disposal options are available in your community so you can provide your patients with accurate information. It’s also important to assess the needs of your patients when advising them on how to dispose of their sharps. For instance, if your patient will only be administering injections for a short period of time, a mail-back option is probably the best solution. Patients who will require long-term treatment for diabetes, HIV, or other chronic conditions should be counseled in the use of a home needle destruction device as this will be the most economical solution. For those patients using therapies for infectious diseases such as HIV or Hepatitis C, it is imperative that they receive instruction regarding the importance of proper needle disposal in order to protect the community.
If you do not have needle-disposal programs in your area, instruct your patients to:
- Put needles into a container that has a lid and is strong enough to keep the needles from sticking through the sides, such as a liquid detergent bottle or metal can.
- Throw the container away before it is full all the way to the top.
- Put the container lid on tight and use heavy tape to keep it on.
- Put the container in the center of your garbage.
For more information and an instructional brochure, What Do I Tell My Patients, contact the Coalition for Safe Needle Disposal at 800-643-1643 or print it from their web site: http://www.safeneedledisposal.org/.
Other resources for you and your patients include:
- United States Environmental Protection Agency. Protect yourself, protect others: safe options for needle disposal. Washington, DC: EPA; June 2006. Pub. no.: EPA530-F-06-014. May be ordered from EPA at 800-490-9198; also available at http://www.epa.gov/epaoswer/other/medical/med-home.pdf.
- United States Environmental Protection Agency. Community options for safe needle disposal. Washington, DC: EPA; October 2004. Pub. no.: EPA530-K-04-001. May be ordered from EPA at 800-490-9198; also available at http://www.epa.gov/epaoswer/other/medical/med-govt.pdf.
- Journal of the American Pharmaceutical Association. Supplement to the Journal of the American Pharmaceutical Association. 2002;42(6)suppl 2:S1- S119 at http://www.aphanet.org/JAPhA/suppl2_cdc.pdf
A call to action
Nurses can help address a critical public health problem: limited options available for the safe disposal of used needles and other sharps in the community at large. Safe disposal will protect workers and the public from injury and possible infectious disease transmission. Join the Coalition for Safe Needle Disposal to help educate the American public about this issue and effective alternative solutions to discarding used sharps into the solid waste system that best suit your community. If you are interested in obtaining more information or starting a sharps-disposal program in your community, contact Jenny Schumann of the Coalition for Safe Community Needle Disposal at 800-643-1643 or at jschumann@safeneedledisposal.org.
Kathy Gold is director of outreach and education for the Diabetes Research and Wellness Foundation in Washington, D.C.
FDA approves new type of drug for insomnia
On August 13, the U.S. Food and Drug Administration (FDA) approved Belsomra (suvorexant) tablets for treating insomnia. Belsomra is the first approved orexin receptor antagonist. Read more
When patient privacy endangers staff
A few weeks ago, the conversation in my ethics class turned to patient privacy. In general, the students were all for it. But when they began swapping stories about everything from HIV-positive patients to violent psychiatric patients, their opinions changed: They were all against it.
At my request, the students put their stories in writing, and we analyzed them in class. Here’s one of the stories.Around midnight, a 29-year-old man with diagnoses of bipolar disorder, substance use disorder, and antisocial personality disorder arrived at our emergency department (ED) for a 72-hour involuntary placement for psychiatric assessment under the Baker Act. Our ED personnel shuttled the patient to the Psychiatric Assessment—Referral office with these comments: “Get rid of this guy fast. He’s trouble.” “This guy abuses the system.” “He has assaulted several healthcare workers.” “He needs constant intervention to maintain the safety of staff and other patients.”
In the Psychiatric Assessment-Referral office of our Baker Act-receiving facility, a registered nurse specializing in mental health assesses patients and discusses them with the on-call psychiatrist, who determines the level of care needed and the patient’s placement. I am that intake nurse. Our office also keeps a “do not admit” list, and this patient was on it. Some of the nurses on our own adult psych unit told me that during a previous admission, he assaulted a nurse. He was jailed and convicted of the assault. The nurse suffered knee damage and still has a restraining order against him.
Nurse’s assessment
When I assessed him, he was generally calm and cooperative, aside from his persistent, aggressive requests to smoke and several attempts to leave the office without an escort to do so. Both the psychiatrist on call and I were new to the facility, so we didn’t have any firsthand knowledge of the patient’s history and treatment. Before calling the psychiatrist, I called some other psych units in the area and found that this patient had been discharged the day before from a facility 70 miles away—and that he was not welcome back because of his aggressive behavior.I also learned that our local community mental health facility would not accept a referral because this patient had assaulted personnel there. A colleague at the community center told me that the patient “burned all his bridges in a 100-mile radius.”Making a decision
Based on this information, should I call the psychiatrist and say, “This guy is bad news, and the unit will have your head and mine if we admit him”? Or should I say, “This patient is suicidal, and he has a plan to kill himself. We have the closest bed”? And what are the ethical implications of a “do not admit” list, particularly when hospital personnel know a patient’s situation and have not implemented options that might break his cycle of use and abuse of acute services?Author’s commentary
To help highlight the ethical problems, we decided to start with the most obvious legal problem: It is illegal, and unethical, for a hospital to have a “do not admit” list. At a minimum, the risk manager should be told about the list as soon as possible. Moreover, a Baker Act facility voluntarily assumes a duty to admit patients who meet Baker Act criteria. If state authorities knew that the hospital maintained such a list, the hospital would lose its status as a Baker Act facility. Moreover, the nurse is asking about how she should present information to the physician. Certainly, how things are phrased can have an impact on another’s judgment, but the alternatives the nurse expresses are designed to influence. The nurse should present the physician with her assessment and the patient’s past history at that facility, including the existence of the restraining order. In so far as humanly possible, the relevant information should be provided objectively.Asking the right questions
The nurse’s first duty is to determine if the patient meets the criteria for a Baker Act admission. If the patient does meet the criteria, the only suitable questions have to do with how, when, and where the patient will be cared for; whether or not he will be admitted has already been determined.Conclusion first, assessment second?
The ED staff’s comments about the patient before her assessment tainted the nurse’s conclusions. Certainly, a patient who knows the provisions of the Baker Act could “game” the system by pretending to be suicidal. But is it more likely that this nurse based her conclusion on an initial assessment or on the ED staff’s comments? A few taps on the computer provided the nurse with information about his past admissions. But she also called the inpatient adult psych unit. Would she have made that call—and been told of an attack on a nurse and a nurse’s restraining order—if she hadn’t heard the ED staff’s comments? Is the patient scamming the system, or is the system running roughshod over the patient?If a restraining order actually exists, the patient presents the hospital with logistical problems, yet the nurse doesn’t call the administrator on call to alert him or to verify the information she has uncovered.
Instead, she undertakes a “fact-finding” mission, and uncovers the opinion that the patient is not welcome anywhere and has burned all his bridges. Still, she doesn’t call either the psychiatrist on call or the administrator on call—the two people she should be calling to discuss preparations for holding this man for even a short time.
Violating HIPAA
The nurse’s calls to area psych units, the mental health facility, and the facility that discharged the patient the day before all violate the provisions of the Health Information Portability and Accountability Act (HIPAA). Why? Although the patient’s history of violence is pertinent to his admission, the nurse already knows, or should know if she read the discharge summary, that the patient has a history of violence. She already knows that precautions need to be taken to protect the patient and personnel. Plus, she has a boatload of unsolicited (and unsubstantiated) comments from ED and inpatient psych unit personnel to alert her to the risk of violence.If discovered, these violations of patient confidentiality could result in a series of HIPAA-generated fines for the facility. The nurse could lose her nursing license. The nurse’s disregard for patient confidentiality is also a violation of the American Nurses Association’s (ANA) “Code for Nurses,” and, depending on the state, it could be a violation of the Nurse Practice Act.
One ethical precept that serves professionals well is: Never do privately what you would not want known publicly.Ethical perspective
Whether or not this patient gamed his way into the ED by lying to police officers, the Baker Act requires an assessment within 72 hours. The law also demands that treatment be contingent upon the patient’s consent, unless the patient is a clear and present danger to self or others. While staff question the validity of his danger to himself, there are documented instancesstances of his danger to others, notably hospital staff. Thus, a well-trained psychiatric aide should be readily available in case the “persistent, aggressive requests to smoke and several attempts to leave the office” turn into more physically aggressive behavior.Because we can’t know for sure that the patient is gaming the system, we must assume that he is suicidal. Ethically, this is a key point. Treating such a person involuntarily is a de facto violation of the right to bodily integrity, a right generally upheld by the law. Only when the danger is clear and present is it permissible to ignore this right. From an ethical perspective, the law permitting involuntary treatment of suicidal patients is murky: The legal assumption is that anyone who wants to commit suicide is at least temporarily incompetent. The ethical standard is higher: An assumption of incompetence would have to be supported by much more data. And, an assumption that a patient is gaming the system is, simply put, unethical.
Understanding human rights
A legal right is a permission granted and secured by law. It may or may not protect a human right. A human right is derived from fundamental, universal human needs, and its exercise is an option that may not be obstructed by others.A human right is generally considered to be above the law because it’s based on what humans need to be human. As with all rights, human rights are limited by the rights of others (which is why the patient could be forcefully medicated or restrained if he presented a danger to others). Patients do have rights, but so do nurses and other clinical personnel. They have a right to bodily integrity and to a safe working environment.
Clinically, if not legally, a patient’s history of violence is the best predictor of future violence. With this patient, certain steps must be taken before providing care:
• Precautions must be taken to protect personnel from harm.
• Hospital administration must be notified, so the administrator on call can notify the nurse who has the restraining order.
• The psychiatrist on call must be notified immediately and consulted on the proper assessment and treatment of this patient.Knowing your role
On the surface, this case seems to present a conflict of rights. Workers have a right to a safe work environment. Patients have a right to treatment, to privacy, and to humane and respectful care. But another ethical and legal issue simmering under the surface involves common, prejudicial, and perhaps illegal communications among healthcare personnel. The decision on whether this patient abuses the system should not be made by the clinicians caring for the patient. Their role is to care for the patient and be an advocate for him. There are plenty of people—case managers, insurance executives, legislators, financial experts, and even voters—who are charged with protecting the system. Healthcare professionals are responsible for the efficient, appropriate use of resources, not for rationing resources based on their own opinions.Need for education
The scope of the problem suggests a widespread need for education. Neither nurses nor physicians can make decisions in a vacuum. Communication and collaboration are essential. In this case, there was communication, but it wasn’t informed. The intake nurse, the ED personnel, the nurses in the inpatient adult psych unit, and those in the institutions contacted by the intake nurse all communicated with a total disregard for HIPAA requirements and ethical standards.Selected references
American Nurses Association. Code for Nurses with Interpretive Statements (Code for Nurses). Available at: http://nursingworld.org/MainMenuCategories/EthicsStandards/CodeofEthicsforNurses/Code-of-Ethics-For-Nurses.html. Accessed November 14, 2006.Baker Act reform. Available at: www.bakeractreform.com. Accessed November 14, 2006.
Curtin LL, Flaherty MJ. Nursing Ethics: Theories and Pragmatics. Upper Saddle River, N.J: Prentice Hall; 1982:104.Frequently asked questions about reform of Florida’s Baker Act. Available at: www.psychlaws.org/PressRoom/faqonbakeract.htm. Accessed November 14, 2006.
The Health Information Portability and Accountability Act. Available at: http://www.hhs.gov/ocr/hipaa/privacy.html. Accessed November 14, 2006.
Molbert B, Beck JC. Assessing violence in patients: legal implications. Available at: http://www.psychiatrictimes.com/article/showArticle.jhtml?articleId=175802294. Accessed November 14, 2006.
U.S.: Number of mentally ill in prisons quadrupled. Human Rights News. September 6, 2006. Available at: http://hrw.org/english/docs/2006/09/06/usdom14137.htm. Accessed November 14, 2006.
Leah Curtin, DSc(h), RN, FAAN, a Clinical Professor of Nursing at the University of Cincinnati College of Nursing in Ohio, was the Editor-in-Chief of Nursing Management for 20 years. She also is Managing Partner of Metier Consultants, and the Director of Cross Country Education’s Nurse Manager Boot Camp.
Editorial Staff Lillee Smith Gelinas, MSN, RN, FAAN
Editor-in-Chief
lgelinas@healthcommedia.comCynthia Saver, MS, RN
Editorial Director, Author Contact
csaver@healthcommedia.comJulie Cullen
Managing Editor
jcullen@healthcommedia.comJane Benner
Copy EditorSubscription Questions?
Christian Evans Gartley
Production Director
215.489.7004
cevansgartley@healthcommedia.comChange in Mailing Information?
To change your subscription information online, send request to:
cevansgartley@healthcommedia.comPublishing Staff Gregory Osborne
Group Publisher
215.489.7000 x101
gosborne@healthcommedia.comSofia Goller
Vice President of Publishing & Sales
215.489.7000 x120
sgoller@healthcommedia.comTyra London
Director, Marketing & Program Mgmt.
215.489.7000 x115
tlondon@healthcommedia.comSales Staff
John Travaline
Sr. Account Manager
215-558-3900
jtravaline@healthcommedia.comMeg Celmayster
National Account Director
215-489-7000 x117
mcelmayster@healthcommedia.comStanley Anton
Account Manager
215-489-7000 x107
santon@healthcommedia.comClassified Ad Sales
Sofia Goller
Vice President of Publishing & Sales
215.489.7000 x120
sgoller@healthcommedia.comProduction Staff
Chris Evans Gartley
Production Director
215.489.7004
cevansgartley@healthcommedia.comDave Beverage
Art DirectorJoint Commission proposes alarm management as 2014 National Patient Safety Goal
The Joint Commission is inviting comments on its proposed 2014 National Patient Safety Goal on management of alarms. The 15-question survey should take about 10 to 15 minutes to complete. Read more.