An indwelling urethral catheter increases the risk of urinary tract infection (UTI) by compromising urinary tract defenses, irritating the urethral and bladder mucosa, and promoting growth of a bacterial biofilm. Roughly 25% of patients in acute-care hospitals have indwelling catheters at some point. Of the more than 1 million hospital-acquired UTIs occurring in the United States each year, 80% are linked to indwelling catheters.
Catheter-associated UTIs increase morbidity and mortality, lengthen hospital stays by 1 to 3 days, and add approximately $675 per patient to overall costs, with an additional $3,800 if bacteremia occurs. Research confirms that most of these UTIs result from pathogens that ascend the urethra and that the urethral meatus, drainage bag, and connections are potential bacterial reservoirs in catheterized patients.
In October 2008, the Centers for Medicare & Medicaid Services (CMS) stopped reimbursing hospitals for costs associated with hospital-acquired conditions (HACs) that were absent at admission and could have been reasonably prevented had appropriate guidelines been followed. UTI is one of these HACs. The Joint Commission’s 2012 National Patient Safety Goals include a new goal for preventing catheter-urinary tract infections caused by catheters.
Caregivers have been using traditional catheter practices for years, although some of these practices have been proven to be ineffective or even potentially harmful. Studies suggest that one of them—prophylactic systemic antibiotic therapy—may merely delay a catheter-related UTI and might even contribute to emergence of antibiotic-resistant bacteria. Generally, organisms deep within the matrix of the urinary tract’s bacterial biofilm are unaffected by antibiotics.
Best practices for UTI prevention
The Centers for Disease Control and Prevention and the Joanna Briggs Institute offer research-based best practices for the care of catheterized patients. Sufficient evidence exists to recommend the following strategies for preventing catheter-acquired UTIs:
- Insert a urethral catheter only when indicated, and remove it at the earliest possible time.
- Maintain good hand hygiene and use gloves before manipulating the catheter. Dispose of gloves and promptly wash hands after contact with the patient and catheter.
- Maintain a closed drainage system; any opening creates an entry route for bacteria, which can lead to infection. Don’t violate the closed system to collect sterile urine specimens. Instead, collect specimens by aspirating with a sterile needle from the bag sample port only after cleaning the port with 70% isopropyl alcohol and letting it dry thoroughly.
- Perform meatal care twice daily using soap and water and working from the front to the back of the perineal area. Evidence shows no advantage to antiseptic use. Though some research suggests cleaning the catheter with povidone-iodine and applying antibiotic ointment at the insertion site may decrease bacteria, most studies show this practice has no benefit and may even lead to infection.
- Avoid unnecessary irrigation, which hasn’t been proven to decrease bacteriuria.
- Secure the catheter. Although little evidence exists to support any particular method, securing the catheter may prevent meatal and urethral irritation, tension on the catheter, bladder-neck trauma, and urethral tearing. It also improves patient comfort and decreases the risk of inadvertent dislodgement.
- Check the tubing for kinks to ensure that urine flows unobstructed into the drainage bag.
- Empty the urine collection bag regularly, using a separate container for each patient. Never let the spigot and nonsterile collecting container come into contact, as this can introduce bacteria.
- Keep the collection bag below bladder level to prevent backflow of contaminated urine.
- Increase the patient’s fluid intake. This has been shown to decrease UTI incidence, possibly by diluting the urine and flushing out bacteria.
- Personnel should be taught how to insert a urinary catheter correctly, with opportunities for re-education as needed.
Also, be aware that several authors caution against housing two patients with indwelling catheters in the same room, because caregivers might be tempted to provide care for both patients without washing hands or changing collection equipment.
UTIs: No longer inevitable
UTIs are a serious problem, with lethal potential. The spotlight cast on UTIs by the CMS nonreimbursement policy is a crucial reminder. Nursing documentation of admission assessments can help determine whether a patient had an HAC before admission.
In the past, catheter-associated UTIs were seen as an inevitable consequence of hospitalization. Now they’re considered unacceptable results of poor care. With the risk of lost revenue, hospitals have a powerful incentive to address this often-neglected aspect of care. By implementing best practices, we can help ensure that hospitals receive full reimbursement for the care patients receive.
Linda M. Redd works in the emergency department at Massachusetts General Hospital in Boston. She is a mentor in the Clinical Leadership Collaborative for Diversity in Nursing program of the University of Massachusetts and Massachusetts General Hospital.
Selected references
Catalano K. Preventable hospital acquired conditions: the whys and wherefores. Plast Surg Nurs. 2008;28(3):158-161.
Cochran S. Care of the indwelling urinary catheter: is it evidence based? J Wound Ostomy Continence Nurs. 2007;34(3):282-288.
Elpern EH, Killeen K, Ketchem A, Wiley A, Gourang P, Omar L. Reducing use of indwelling urinary catheters and associated urinary tract infections. Am J Crit Care. 2009:18:535-541. http://ajcc.aacnjournals.org/cgi/content/abstract/18/6/535. Accessed April 5, 2010.
Gould, CV, Umscheid CA, Agarwal RK, Kuntz G, Pegues, DA; the Healthcare Infection Control Practices Advisory Committee. Guideline for Prevention of Catheter-Associated Urinary Tract Infections 2009. Centers for Disease Control and Prevention, 2009. http://www.cdc.gov/hicpac/pdf/CAUTI/CAUTIguideline2009final.pdf. Accessed April 5, 2010.
The Joint Commission. Critical Access Hospital: 2012 National Patient Safety Goals. http://www.jointcommission.org/cah_2012_npsgs. Accessed Jan. 6, 2012.
Mion L. Pay for performance: will it add to the perfect storm in health care or provide safe sailing? Geriatr Nurs. 2008;29(4):236-239.
Newman D. The indwelling urinary catheter: principles for best practice. J Wound Ostomy Continence Nurs. 2007;34(6):655-661.
NHS Quality Improvement Scotland. Best practice statement, June 2004: urinary catheterisation and catheter care. 2004. http://www.nhshealthquality.org/nhsqis/files/Urinary_Cath_COMPLETE.pdf. Accessed April 5, 2010.
Pronovost P, Goeschel C, Wachter R. The wisdom and justice of not paying for “preventable complications.” JAMA. 2008;299(18):2197-2199.
Stokowski LA. Preventing catheter-associated urinary tract infections. Medscape Today. February 3, 2009. http://www.medscape.com/viewarticle/587464_4. Accessed April 5, 2010.
Wald H, Kramer A. Nonpayment for harms resulting from medical care. JAMA. 2007;298(23):2782-2784.
Welton J. Implications of Medicare reimbursement changes related to inpatient nursing care quality. J Nurs Adm. 2008;38(7/8):325-330.
















3 Comments.
I can assure you, my husband is in a nursing home with Multiple Sclerosis. His last bout with a U.T.I., the 4th I. Four months! He arrived on Friday IN SEPTIC SHOCK from the NURSING HOME!! The bag was bone dry. Yes, he has lost cognitive abilities, standing , sitting, swallowing since the pandemic things truly got worse. Just when you think it’s not possible. The staff feels people with M.S. like the way they live. True the staff said this to my daughter. We don’t have a leg to stand on. They don’t notice when his bag has blood in it n he has a uti or when he has it rusty red. They pretend it must have just happened. I have found him soaked in his own urine with a catheter in place. It backed up. This was pre pandemic. He was taken care of at home for 22 of the 32 years he has had M.S.. Families have no recourse as CMS doesn’t hold the facility responsible for the large number of uti. S of one person or 10 patients. Nobody is monitoring the nursing home care. I’ve seen M.S. patients die because of the u.t.i. infections. Nursing home staff don’t take the toileting of patients seriously. They hand it off to a unskilled aide barely making minimum wage and not much more. It’s a job. Ignorance causes the u.t.i.. maintenance of a car gets more attention from the people who claim they care. Not many want the job so we get the people who just see the easy paycheck when they wear blinders. They handle the catheter once a month and ignore the daily care. He keeps ending up in the hospital who we know they don’t want this on their plate!
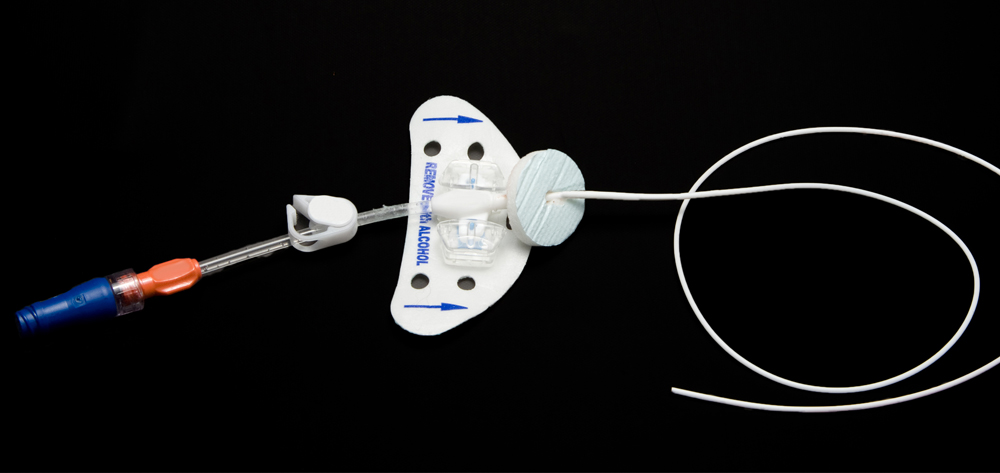
The image used is a peripherally inserted central line (PICC)
What’s happened to basic common sense re: cath care. When I see nurses, aides, PTs and other so-called ‘professionals’ hoisting a bag of urine above the patient’s knees, I cringe. I haven’t worked in a facility in years that does meatal care, pushes fluids or keeps I/O, and I’m mortified that the simplest of preventative measures have somehow disappeared from our ‘academia.’ Glad I’m almost done with nursing, because the whole field is a mess.