Nurses advocate for meeting older adults’ needs and wants.
As the number of people over 65 years old continues to grow in the United States, so too is a movement to provide better age-specific care and truly focus on what older adults say they want in their lives and in their healthcare experiences. Nurses are among those leading and advocating for these efforts, as well as working to ensure older adults can get the right level of care as their health status and life circumstances change.
According to U.S. Census Bureau data for the year 2020, the number of adults 65 years old and over is projected at 56 million, those 85 and older at about 6.7 million, and those 100-plus at around 92,000. Totals in each age category are projected to increase at least through 2060.
Beyond the numbers, many older adults are focused on aging in place. They want to remain in their homes or preferred communities.


Meanwhile, long-term care facilities requiring skilled nursing continue to close around the country. Of those remaining, the number of beds for Medicaid-eligible residents are limited, often requiring long wait times, and private-pay beds are expensive, said Tracie Harrison, PhD, RN, FAAN, FGSA, a professor at The University of Texas at Austin School of Nursing and director of the Center for Excellence in Aging Services and Long Term Care. Independent living, physical rehabilitation, and post-acute facilities, however, are among those that are expanding.
Senior housing specialists also see the development of more multigenerational, senior co-housing, and other types of active living communities.
Regardless of where older adults live, nurse gerontology experts say more nurses with specialized knowledge are needed to provide care to those 65 and older as they continue to age and contend with more health issues.
In the community
Nurses are key to developing and implementing effective, innovative programs, and one such effort is Community Aging in Place – Advancing Better Living for Elders (CAPABLE), co-created by Sarah Szanton, PhD, ANP, FAAN, professor and director of the Center for Innovative Care in Aging at Johns Hopkins School of Nursing, and a Maryland Nurses Association member. The program currently is offered at 27 sites in 15 states and Australia.
CAPABLE is designed to help older adults improve their mobility, functionality, and ability to live independently, which can reduce hospitalizations and healthcare costs. Older adults who want to participate develop their own action plans and work with
a registered nurse, an occupational therapist, and
a handyperson to achieve their goals, said Alice Bonner, PhD, RN, director of Strategic Partnerships for CAPABLE.

Bonner describes the 4 to 5 months-long program as focusing on motivational interventions. For example, a provider may tell a patient that he has to lower his blood pressure, but that patient may be more concerned about his empty refrigerator at home or his chronic pain.
“Nurses [who are on a CAPABLE team] don’t walk into a home and start talking about medical issues—although they may come up,” said Bonner, an ANA Massachusetts member. “They ask older adults to tell them something about themselves, what they like to do, and what they want to be able to do. It’s an opportunity to engage in real conversations with people and support their goals to remain in charge of their lives, live independently safely, and improve the quality of their lives.”
For example, if someone’s goal is to be more mobile or cook, nurses and other members of the team work with clients to brainstorm ideas, such as adding an extra banister leading to stairs, using heating pads to reduce pain, and lowering shelves in the kitchen. Along with offering adaptive strategies, nurses also may recommend tools and resources, such as transportation to buy groceries or visit a community center.
“People want the flexibility, independence, and autonomy to live at home,” Bonner said. “They want the familiarity of being near their friends, their faith-based organization, or their barbershop and to engage in community life. And older adults want to contribute—whether it’s volunteering in libraries or schools or participating in intergenerational programs.”
CAPABLE is aimed at helping people adapt to changes and age in their communities, which Bonner said is “the wave of the future.” She’s currently focused on reaching out to Medicare Advantage plans, health systems, and other organizations to expand the program. Additionally, she sees nurses as having a great role in addressing the needs of older adults in their communities.
Age-friendly acute care
Over the past several years, leaders at Anne Arundel Medical Center (AAMC) in Annapolis, Maryland, have made a concerted effort to provide evidence-based, specialized care to its geriatric population. First, AAMC joined the Nurses Improving Care for Healthsystem Elders (NICHE) program to strengthen staff expertise as it prepared to open its 30-bed acute care of the elderly (ACE) unit in 2013.
“When you are 45, 65, or 85, your needs and desires are different,” said Lil Banchero, MSN, RN, senior director of the AAMC Institute for Healthy Aging and the ACE unit. The average age of patients on the ACE unit is 85, and they have complex care needs.
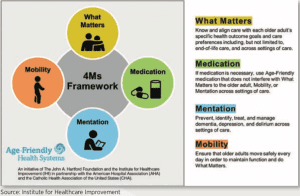
To further individualize and enhance care on the unit, AAMC became one of five pioneering organizations to join the Age-Friendly Health Systems Initiative in 2017. At the core of this national and growing initiative, with 271 recognized participants and 122 exemplars as of January 2020, is the 4Ms Framework for Age-Friendly Care: what matters to patients; ensuring medications don’t interfere with quality of life; addressing mentation-related issues, including delirium and depression; and promoting mobility (see infographic, page 52).
Everyone working in the ACE unit must undergo annual NICHE training to stay current on best practices. Nurses are encouraged to obtain certification in geriatric nursing, according to Banchero.
“We also created a position called a mobility tech, who focuses on making sure all residents are up and moving every day—and not just going from the bed to the chair,” she said.
Other interventions include:
• Every resident undergoes screening for delirium.
• Patients participate in group “ACErcise” sessions with a physical therapist to improve their mobility and strength. This intervention has the added bonus of improving mentation and alleviating social isolation that can occur when someone is hospitalized. Patients also are encouraged to eat together and engage in activities like playing cards.
• Pharmacists check for high-risk medications and possibly reducing the number of medications when patients are admitted. Pharmacists also review medications with patients and their caregivers at the bedside upon discharge. (Some patients have been admitted with 20 to 30 medications.)
• To encourage and track hydration, often a critical need in this population, patients are given easy-to-hold cups with clearly visible lines showing amounts.


The white board provides personalized information about the patient, such as how they would like to be addressed; favorite sports teams or hobbies; what they don’t like, such as being cold; what they like, such as listening to music; and what their goals are, which may be to go home free of pain. Every nurse also documents what matters most to patients in the electronic health record, Banchero said.
“Providing age-friendly care requires a paradigm shift,” she said. “It’s part of our responsibility as healthcare professionals to be informative, truthful, and plan care that’s safe and matters most to patients.” AAMC continues to focus on rolling out the 4M components organization-wide.
Beyond a one-size-fits-all approach
“People can be similar in age—70 or 80 years old—but their needs and how they feel can run the gamut from vibrant to frail,” said Sabol, also a North Carolina Nurses Association member. “As a healthcare provider, you need to be careful to look at the older person as an individual, what they can do, and what matters most to them during every visit or interaction.”
And care must be holistic.
“In nursing, we get so focused on the biological and psychological aspects of care, that we

Yet another issue that nurses must consider is the shift to home-based care, and the difficulties it may place on family caregivers, according to Dunn.
“The reality is people want to be at home,” Sabol said. “Nurses and other healthcare providers need to be thoughtful about what family caregivers can do and cannot do and provide the education that’s needed long before discharge.”
That said, more nurses are needed throughout long-term care, including post-acute facilities where complex care is provided, according to Harrison.
“And one of the biggest challenges is how to provide the best care possible in long-term care if nurses are not invested in this [practice] area,” said Harrison, a Texas Nurses Association member.
Harrison believes building a long-term care workforce includes exposing student nurses to this challenging specialty earlier in their clinical rotations, as well as offering financial incentives and transition-to-practice programs for those willing to work in these facilities. She also believes it’s critical that nurses become knowledgeable about policies on aging and advocate for changes that benefit this population.
Nurse experts add that the surge in home care services, telehealth, wellness programs, and retail clinics will create even more opportunities and roles for nurses with geriatric knowledge. To that end, they emphasize that nurses must seek out ways to gain that knowledge. For example, Dunn noted that GAPNA offers numerous educational resources and advocacy opportunities for nurses.
Finally, a shared concern among nurse experts is the loss of expertise as more nurses within this specialty retire.
“We must work with our communities to meet the needs of the geriatric population,” Harrison said. “We can’t do it alone.”
— Susan Trossman is a writer-editor at ANA
Resources
Gerontological Advanced Practice Nurses Association: gapna.org
Nurses Improving Care for Healthsystem Elders: nicheprogram.org
Age-Friendly Health Systems Initiative:
johnahartford.org/age-friendly-health-systems-
initiative
CAPABLE: nursing.jhu.edu/faculty_research/
research/projects/capable
Center for Excellence in Aging Services and Long-Term Care: utlongtermcarenurse.com
ANA Enterprise efforts:
Delirium: Prevent, identify, and treat, a collaboration between ANA and the American Delirium Society: nursingworld.org/practice-policy/work-environment/health-safety/delirium
American Nurses Credentialing Center: Certifications: nursingworld.org/our-certifications



















