A community hospital’s initiative improves patient outcomes.
Takeaways:
- Few practice guidelines focus on in-hospital ST-elevation myocardial infarctions (STEMIs).
- Challenges related to inpatient STEMIs include delays in several areas—including recognition, electrocardiogram interpretation, STEMI team or rapid response team activation, transfer to a percutaneous coronary intervention-capable hospital—and lack of inpatient STEMI processes and protocols.
- A hospital developed a STEMI protocol project that streamlined, standardized, and improved care delivery.
MOST current ST-elevation myocardial infarction (STEMI) practice guidelines focus on recommendations for patients who present to the emergency department (ED), leaving in-hospital STEMIs overlooked. However, inpatient STEMIs recently received attention as studies have identified this patient population as high risk for adverse clinical outcomes. According to a report from the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines by O’Gara and colleagues, approximately 25% to 40% of acute myocardial infarctions are STEMIs, and of those 5% to 6% occur in-hospital. Patients who develop a STEMI while hospitalized have worse outcomes than those presenting to the ED with the same condition. In addition, 60% of those who experience inpatient STEMI have an atypical presentation, which hinders early identification.
Adhering to evidence-based guidelines and protocols can help ensure consistent inpatient STEMI management, quick identification, timely care, and improved patient outcomes.
Inpatient STEMIs: Clinical challenges
Challenges related to inpatient STEMIs include delayed recognition, delayed electrocardiogram (ECG) interpretation, delayed STEMI team or rapid response team activation, delayed transfer to percutaneous coronary intervention (PCI)– capable hospitals, lack of inpatient STEMI processes and protocols, and care providers who may delay transfer through factors such as obtaining additional consults. (See STEMI standard of care.)
The nonuniformity of inpatient STEMI management can create confusion and delay in patient care, potentially increasing complications and mortality rates. The 2013 American Association of Cardiology/American Heart Association STEMI clinical practice guidelines highlight the importance of improved inpatient STEMI outcomes, with particular emphasis on non-PCI–capable hospital transfer initiatives and treatment protocols. Standardized nurse-driven, evidence-based protocols have been shown to improve clinical outcomes of inpatient STEMIs. However, when few in-hospital STEMIs occur, protocols aren’t always followed. STEMI drills can help increase protocol familiarity, particularly in units that typically don’t care for these patients.
For patients who’ve had an ST-elevation myocardial infarction (STEMI), the standard of care is myocardial reperfusion using percutaneous coronary intervention (PCI) or thrombolytic agents. PCI is preferred, and time is of the essence. The American Association of Cardiology/American Heart Association reperfusion time standard, established in 2004, has become a national core quality measure for The Joint Commission.
• If a patient presents to a PCI–capable hospital, the standard is reperfusionwithin 90 minutes from arrival.
• If the hospital isn’t PCI–capable, the patient should be transferred to a facility that is and reperfused within 120 minutes from arrival at the first hospital. This standard is commonly referred as “door-to-reperfusion” time.
• If a STEMI is identified after admission, the same goals apply for both PCI– (90 minutes) and non-PCI– (120 minutes) capable hospitals; however, the reperfusion start time begins with a STEMI positive electrocardiogram.
A community hospital meets the challenge
In 2014, nursing leaders at a non-PCI–capable community hospital recognized that a protocol was needed to improve the recognition, management, and transfer of inpatient STEMIs. (See Literature review.) In that calendar year, eight inpatient STEMIs were identified. All had delays in obtaining an ECG and identifying STEMI. Only three of the eight patients were transferred to a PCI hospital for reperfusion therapy, and they had a reperfusion time greater than 120 minutes from STEMI ECG. The other five patients received conservative medical management that didn’t include thrombolytics because of patient-family preference or provider recommendation.
Project design
This evidence-based practice project focused on developing a clinical initiative to improve inpatient STEMI care. The medical cardiology advanced practice RN was charged with leading the project, which included four objectives that were divided into three phases (gap analysis, project development, and project rollout) and completed within 16 months. The objectives were:
1. Identify current organizational inpatient STEMI practice gaps.
2. Develop an inpatient STEMI protocol.
3. Develop an inpatient STEMI protocol educational program.
4. Develop an inpatient STEMI policy.
Phase 1—Gap analysis. The first objective was to identify current organizational practice gaps in inpatient STEMI management. Background information, organizational reports, and data analysis provided the foundational evidence for the need of the project. The project leader analyzed inpatient STEMI data for the previous 2 years to evaluate the practice, knowledge gaps, patient outcomes, and internal resources as well as processes for transferring patients to a PCI–capable hospital.
The area of greatest opportunity for improvement was inefficient patient transfers. The project leader realized the need to “think outside the box” and involve the chief of the local fire department to establish an efficient transfer process. This partnership was essential to creating seamless interhospital transfers and ensuring clinical practice change sustainability.
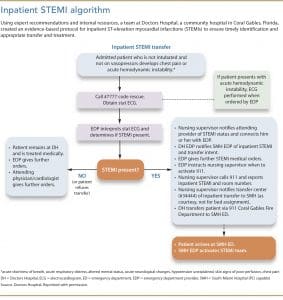
Phase 2—Project development. This phase included the second and third objectives. The second objective was developing a protocol for nonpharmacologic management and interhospital transfers of inpatient STEMIs via fire rescue by activating 911. The project leader reviewed standards of care and national guidelines for STEMI management and collaborated with other entities within the health system to cross-reference practices. A protocol was then created based on evidence, internal resources, and expert recommendations. (See Inpatient STEMI algorithm.)
The third objective was developing an educational program for staff to boost clinical management confidence and enhance practice change understanding. The content covered atypical inpatient STEMI presentation, the importance of rapid recognition and patient transfers, and an overview of the inpatient STEMI protocol. A reference poster depicting the protocol was created for each inpatient nursing unit, and clinical nurse educators were trained to provide ongoing education as needed.
Phase 3—Project rollout. The fourth objective included staff education rollout and new policy implementation. The policy delineates the process to follow when an inpatient STEMI is identified and describes patient inclusion criteria (inpatient units only) and clinical indications for protocol activation. The project leader initially facilitated all educational sessions with providers and nursing staff at select committee and staff meetings and one-on-one as needed.

A literature review conducted using three major electronic databases (PubMed, Ovid, and MEDLINE [ProQuest]) and the keywords “inpatient STEMI,” “myocardial infarction,” “hospitalized patient,” “reperfusion,” “guidelines,” and “ST elevation MI,” yielded 11 articles and three primary sources of high relevance.
• A retrospective single-center study conducted in 2013 by Dai and colleagues evaluated inpatient ST-elevation myocardial infarctions (STEMIs) over 5 years. The results highlighted the atypical presentation of this condition and found that patient survival to discharge was lower for inpatient compared to outpatient STEMIs—60% vs. 96%.
• A 2014 study conducted by Garberich evaluated the benefit of using a standardized treatment protocol for managing inpatient STEMIs. The results suggested that implementing a protocol may positively impact clinical outcomes.
• A 2014 study by Kaul and colleagues identified variables associated with treatment outcomes of inpatient STEMIs. The results of this large multicenter (62,021 cases in 303 hospitals) observational retrospective study provided valuable insight into the patient characteristics observed in the inpatient STEMI population.
Measures of success
After implementing this initiative, nurses were more likely to activate the rapid response team when a patient presented with new-onset chest pain or had an acute change in hemodynamic status. Six months after implementation, a 20% increase of rapid response team activations (in response to clinical deterioration and noncardiopulmonary arrest events) was noted. Three inpatient STEMIs were identified during this time. One of the three patients reported chest pain and the other two presented atypically. All three patients had an ECG that was interpreted by the ED physician within 10 minutes of symptom onset. These patients were transferred and reperfused within 50 minutes from symptom onset (well below the 120-minute national standard). During rapid response debriefing, the nursing staff reported protocol ease of use and confidence following patient management steps.
Roadblocks
The biggest barrier to project success was multi-stakeholder collaboration. The project leader established an e-mail distribution group (including key collaborators, department leaders, administrators, and providers) to address mass communication delivery. Executive leaders’ support was crucial to project success because their approval was needed to progress from one phase of the project to the next. A timeline with established goals and tasks was developed and distributed to pertinent collaborators to ensure timely milestone completion.
STEMI protocol implications
The STEMI protocol project has streamlined, standardized, and improved care delivery by establishing effective inpatient alert systems, securing a collaborative relationship with the local fire department, instituting a treatment protocol and policy, and developing a staff educational program to help increase knowledge and awareness of inpatient STEMIs. To close the gap between outpatient and inpatient STEMI clinical outcomes, hospitals should implement an evidence-based protocol to ensure a structured approach to manage care. The protocol can help reduce clinical management uncertainties, improve reperfusion times, and reduce length of stay, adverse outcomes, and mortality.

Katty Guevara is an APRN supervisor/medical cardiology APRN at Doctors Hospital in Coral Gables, Florida.
Selected references
Antman EM, Anbe DT, Armstrong PW, et al. ACC/AHA guidelines for the management of patients with ST-elevation myocardial infarction—executive summary: A report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Writing committee to revise the 1999 guidelines for the management of patients with acute myocardial infarction). Circulation. 2004;110(5):588-636.
Dai X, Bumgarner J, Spangler A, Meredith D, Smith SC, Stouffer GA. Acute ST-elevation myocardial infarction in patients hospitalized for noncardiac condition. J Am Heart Assoc. 2013;2(2):e000004.
Garberich RF, Traverse JH, Claussen MT, et al. ST-elevation myocardial infarction diagnosed after hospital admission. Circulation. 2014;129(11):1225-32.
Kaul P, Federspiel JJ, Dai X, et al. Association of inpatient vs outpatient onset of ST-elevation myocardial infarction with treatment and clinical outcomes. JAMA. 2014;312(19):1 999-2007.
O’Gara PT, Kushner FG, Ascheim DD, et al. 2013 ACCF/AHA guideline for the management of ST-elevation myocardial Infarction:A report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines. Circulation. 2013;127(4):e362-425.



















