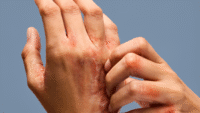
One of your patient’s family members asks you about the itchy rash on his forearms. He shares that 2 days ago he came into contact with a poison ivy plant while weeding his garden, and he’s worried his case of poison ivy may be contagious to the patient. Would you know how to respond? First, you have to understand reactions to poison ivy.
About poison ivy, oak, and sumac
Each year between 10 and 50 million Americans will experience an allergic skin reaction after exposure to a group of plants known as the Toxicodendrons—poison ivy, oak, and sumac—making this the most common allergic reaction in the United States. About 85% of Americans are allergic to urushiol, the toxin found in these plants.
Signs and symptoms
The allergic contact dermatitis that follows exposure to urushiol is a delayed hypersensitivity reaction. Symptoms usually appear 12 to 48 hours after exposure, beginning with itching, followed by a red rash. There may be swelling and vesicles, which may break and drain serous fluid. The blisters and rash commonly appear in streaks, where the plant contacted the skin. After about a week, the reaction enters a sub-acute phase and the blisters begin to dry. Severe itching is experienced throughout the reaction, making it difficult to sleep.
Misconceptions
Many misconceptions exist about poison ivy, oak, and sumac. Here are three common ones:
Misconception: Poison ivy is contagious.
Fact: Poison ivy is not contagious. Poison ivy is an allergic reaction to urushiol (the toxin found in poison ivy, oak, and sumac plants). The only way to develop a case of poison ivy is through direct contact with the plant, or by touching a fomite, such as clothing or gardening tool, that has been contaminated with urushiol.
Misconception: Scratching will “spread” the rash.
Fact: Scratching will not move the rash from one area of skin to another. The rash can appear on different parts of the body at different times. Urushiol penetrates thin skin easier than thick skin, therefore the onset of symptoms will occur more quickly on the facial skin than on the forearm. Likewise, an area with a large urushiol exposure produces a rash more quickly than an area with a small exposure. Patients should avoid scratching to help reduce the chance of a secondary infection caused by bacteria from the fingernails.
Misconception: Blister fluid or drainage can “spread” the rash.
Fact: The blister fluid, and any drainage from a poison ivy affected site, does not contain the plant’s toxin, urushiol, and this fluid will also not “spread” the rash.
Treatment
Treatment centers on controlling the symptoms of poison ivy, oak, and sumac reactions by using prescription strength steroid creams, calamine lotion, baths with colloidal oatmeal, and wet-to-dry dressing changes. These treatment options provide temporary relief, and have to be applied repeatedly throughout the 16 to 18 day (or longer) allergic reaction.
Another nonprescription treatment is Zanfel, a patented soap mixture of ethoxylate and sarcosinate surfactants that removes urushiol from the skin. A randomized, double-blind, study of 24 urushiol-sensitive adults demonstrated that an objective score combining redness, skin firmness, and blistering was reduced 48, 96, and 144 hours after exposure to urushiol in patients who washed with Zanfel vs. with a placebo. In another randomized, double-blind, placebo-controlled study of 20 urushiol sensitive subjects, Zanfel was found to effectively treat allergic contact dermatitis, which was experimentally induced with naturally occurring urushiol. This study also found that Zanfel is effective as a post-exposure prophylaxis measure. Most people require only one use to relieve itching and put the body in a position to heal.
Systemic steroids have been the standard of treatment for severe cases of poison ivy, oak, and sumac. Steroid dose packs should be avoided, as they do not contain a high enough dose or a sufficient duration of time. With widespread or systemic reactions, steroids can be used in conjunction with Zanfel.
Providing information
It’s important to provide people with information about poisonous plant identification, prevention, and treatment options. Addressing misconceptions can reduce anxiety and help patients and family members avoid unnecessary changes to their daily activities.
Daniel J. Boelman is a customer service manager at Zanfel Laboratories, Inc., in Clive, Iowa.
Selected references
American Academy of Dermatology. Poison ivy, oak and sumac. http://www.aad.org/skin-conditions/dermatology-a-to-z/poison-ivy#.UWBrKRlU9Ok. Accessed April 8, 2013.
Boelman DJ. Emergency: treating poison ivy, oak, and sumac. Am J Nurs. 2010;110(6):49-52.
Brodell RT, Williams L. Taking the itch out of poison ivy. Are you prescribing the right medication? Postgrad Med. 1999;106(1):69–70.
Davila A, Lucas J, Laurora M, Jacoby J, Reed J, Heller M. A new topical agent, Zanfel, ameliorates urushiol-induced Toxicodendron allergic contact dermatitis. Ann Emerg Med. 2003;42(4)Suppl:S98. Abstract.
Epstein WL, Guin JD, Maibach HI. It’s always poison ivy time. Patient Care. 1997;31(7):40-56.
Resnick SD. Poison-ivy and poison-oak dermatitis. Clin Dermatol. 1986;4(2):208-12.
Fisher AA. Poison ivy/oak/sumac. Part II: Specific features. Cutis. 1996;58(1):22-4.
Stankewicz H, Cancel G, Eberhardt M, Melanson S. Effective Topical Treatment and Post Exposure Prophylaxis of Poison Ivy: Objective Confirmation. Ann Emerg Med. 2007;50(3)Suppl:S26-S27.
Stephanides SL, Moore C. Plant poisoning, Toxicodendron. eMedicine. 2007.
Usatine RP, Riojas M. Diagnosis and management of contact dermatitis. Am Fam Physician. 2010;1;82(3):249-55.
Williford PM, Sheretz EF. Poison ivy dermatitis. Nuances in treatment. Arch Fam Med. 1994;3(2):184-8.