Embrace a spirit of inquiry to improve patient outcomes.
- As nurses, our code of ethics guides our practice and requires us to advance our profession through research and scholarly inquiry.
- Empowered nurses seek opportunities for practice improvement and share their findings with colleagues.
- This labor, delivery, recovery, and postpartum unit applied an evidenced-based practice to aid reduction of cesarean births.
Cesarean births (or cesarean deliveries) are associated with increased morbidity and mortality, as well as longer hospital stays and higher costs. Women experiencing their first pregnancy have a much higher cesarean birth risk than those having second or third babies. As part of the Healthy People 2020 goals, the U.S. Centers for Disease Control and Prevention set a target rate for cesarean delivery at 23.9% for nulliparous term singleton vertex births.
Jefferson Health, which received its second Magnet® recognition in 2023, focuses on performance-driven outcomes and encourages nurse empowerment via evidence-based practice (EBP) and research. The outcomes we achieve with EBP result directly from nurses who lead patient care by driving process improvement. (See EBP defined.)
EBP defined
According to de Groot and colleagues, evidence-based practice (EBP) requires the following five steps:
- Ask a searchable question about a patient, problem, or outcome.
- Acquire the evidence within the literature.
- Appraise the evidence and decide whether it’s high-quality and valuable.
- Apply the best available evidence in practice.
- Assess the outcomes.
Approximately 1,000 births occur per year in our hospital’s labor, delivery, recovery, and postpartum (LDRP) unit. All rooms provide equipment to care for mother and baby before, during, and after the birth. We strive to keep the baby in the room with the mother rather than moving them to a separate nursery setting.
The problem
Delivering quality care while maintaining patient safety is the LDRP unit’s number one goal. However, in October 2019, the LDRP cesarean birth rate rose to 36.0% (above the targeted 23.9%). Compared to full-term vaginal deliveries (>37 weeks’ gestation), cesarean births are associated with long-term risks for the mother, the baby, and subsequent pregnancies. Research indicates several reasons for high cesarean birth rates, including low priority to enhance the mother’s ability to successfully deliver vaginally, a determination that the baby seems large, unsuccessful induction, the need for continual fetal monitoring, and a more tolerant attitude toward surgery and epidural analgesia.
Although at times an essential and lifesaving surgery, cesarean births can also put mothers and babies at unnecessary risk of short- and long-term health problems when performed without a medical need. Vaginal births help mothers avoid risks associated with major abdominal surgery, such as severe bleeding, scarring, blood clots, infections, reactions to anesthesia, delayed ambulation, and long-lasting pain.
One bedside clinical nurse on our LDRP unit used EBP to help reduce cesarean birth rates and improve patient outcomes.
Ask the question
While studying to become a midwife, an LDRP staff nurse attended a conference where she learned about Spinning Babies®, an EBP designed to help increase the incidence of vaginal births by reducing the number of cesarean births. Knowing the cesarean birth rate on her floor was higher than the national goal, she spoke to her leadership team about Spinning Babies. Leadership supported learning more about the program.
Acquire and appraise the evidence
A committee formed to learn about Spinning Babies and how it might improve their practice. A literature search indicated that techniques used by Spinning Babies reduce the need for cesarean birth.
A retrospective study by Melo and colleagues of 2,614 women whose babies were in a breech position found that using the Spinning Babies method successfully repositioned babies in about half the patients; 85% delivered vaginally with few complications. A similar systematic review of eight studies by Hofmeyr and colleagues found the method’s effectiveness in more than half of 1,308 attempts.
The leadership team contacted the Spinning Babies organization, which agreed to host two labor skills workshops to provide this specialized physiologic labor education to some of the LDRP nurses. (See What is Spinning Babies?)
What is Spinning Babies®?
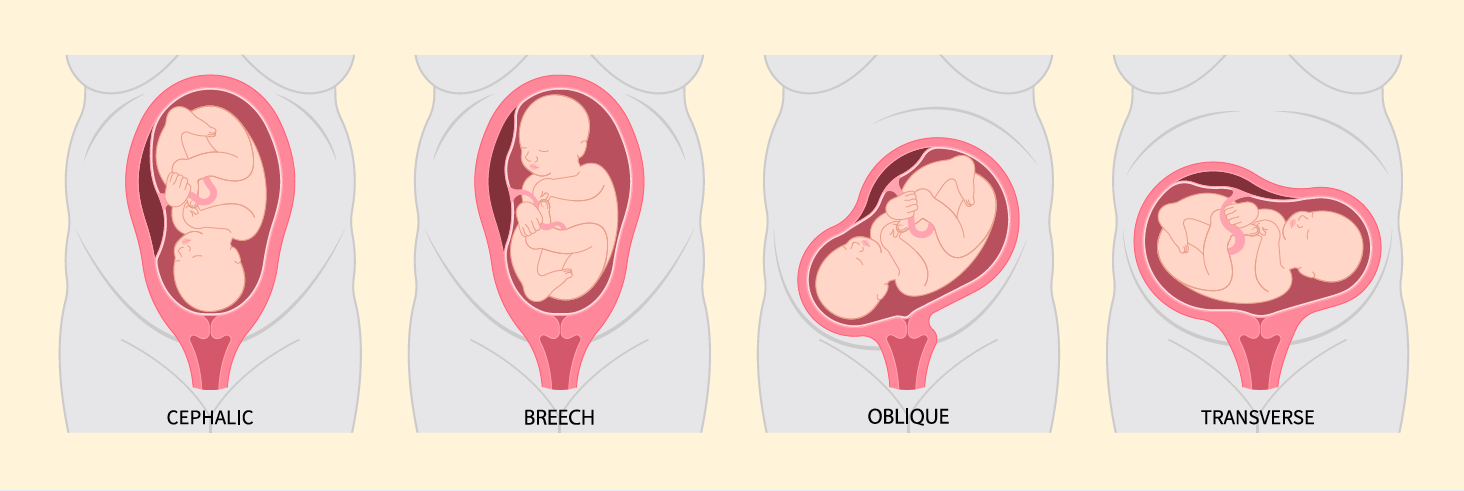
A common labor and delivery complication occurs when the baby’s head doesn’t properly engage into the mother’s pelvis. The fetus may be in an abnormal position, such as breech or posterior. The Spinning Babies initiative, developed by Gail Tully, CPM, uses anatomy and physiology to allow the baby to “release” rather than “be delivered” by mechanical manipulation or force.
Spinning Babies begins with observing fetal movements to predict positioning in late pregnancy. As mothers labor, babies rotate and descend through three levels of the pelvis. If the fetus is in a suboptimal position, or the mother has tight muscles, labor can be difficult. Spinning Babies uses body balancing techniques (the Three Balances) to make room for the baby and equalize the muscles, fascia, ligaments, and joints around the uterus. The exercises help to maintain flexibility so the uterus and pelvis have more room for the baby, rather than increasing medications or turning to surgery.
If after applying the Three Balances the fetus remains in a suboptimal position once labor starts, Spinning Babies uses other techniques to help temporarily enlarge and soften the pelvic opening.
Apply the best evidence
In January 2020, the LDRP unit hosted two 8-hour Spinning Babies workshops for 25 nurses. The instructor provided expert hands-on instruction, and each nurse left with a handout detailing all of the techniques and a certificate of completion along with continuing education units. Learning objectives for the workshop included the following:
- How to promote optimal fetal position
- The hard and soft tissues of the pelvis
- Daily Essentials and Rest Smart activities in pregnancy
- The 3 Principles of Spinning Babies
- Body balancing techniques—Jiggle, Forward-Leaning Inversion, and Side-lying Release
- Identifying signs of progressing and non-progressing labor
- Pelvic level solutions
- Laboring and birthing positions
The participating nurses became the unit’s Spinning Babies champions and were asked to train other nurses and providers. They also created an education board for the unit, which staff and patients continue to use as a reference. Immediately after the training, the champions spent 6 months sharing their knowledge and assimilating it into practice with the unit. The unit’s professional development specialist works with the nurse champions to provide education to incoming residents.
Assess the outcomes
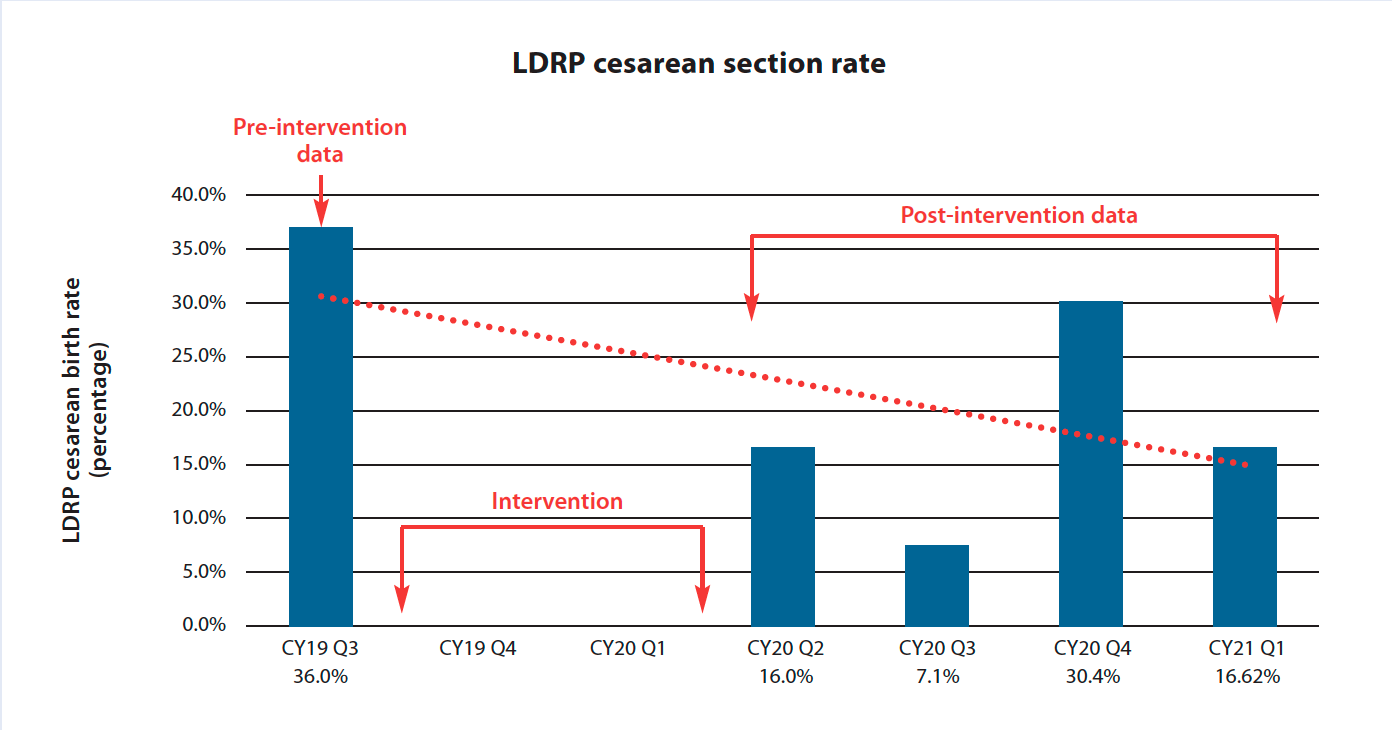
The LDRP unit achieved an average 51% reduction in its cesarean birth rate. These rates are trended monthly and currently hover between 23% and 25% compared to the pre-implementation 36%. Staffing models remain the same. The LDRP unit plans new classes for summer 2024. Nurses and providers continue to support the Spinning Babies program. (See Outcomes.)
Outcomes
Implementation of the evidence-based Spinning Babies® protocol has helped to reduce the cesarean birth rate in the labor delivery, recovery, postpartum (LDRP) unit at Jefferson Stratford Hospital. The increase in cesarean births in the fourth quarter of 2020 is the result of a low number of total births.
Inquiry and professional development
Nursing professional development requires the continuous process of learning and then applying that new knowledge to the nurse’s patient care role. The Code of Ethics for Nurses with Interpretive Statements (the Code) remains our foundational, non-negotiable guide for providing high-quality patient care by participating in EBP, research, quality improvement, informatics, patient-centered care, patient safety, cultural sensitivity, and interprofessional collaboration. We demonstrate an understanding of the Code when we implement change via EBP, which involves integrating research with clinical expertise and the patient’s values and expectations to provide the best possible outcomes.
The improved cesarean birth rate on our LDRP unit occurred because of a practice change prompted by one nurse’s courage to embrace her spirit of inquiry. She understands that as a nurse, she’s obligated to advance the nursing profession through scholarly inquiry and EBP implementation.
The authors work at Jefferson Health. Elizabeth E. Zwillinger is manager of clinical excellence and Magnet. Julia Burke is a nursing professional development specialist.
American Nurse Journal. 2023; 18(9). Doi: 10.51256/ANJ092350
References
Callicutt D, Walker M. Getting involved in your professional nursing organization. J Nurses Prof Dev. 2020;36(4):248-9. doi:10.1097/NND.0000000000000650
Crumley C. The benefits of active engagement in nursing professional organizations: A view from here. J Wound Ostomy Continence Nurs. 2020;47(6):547. doi:10.1097/WON.0000000000000700
Echevarria IM. Make connections by joining a professional nursing organization. Nursing. 2018;48(12):35-8. doi:10.1097/01.NURSE.0000547721.84857.cb
de Groot M, van der Wouden JM, van Hell EA, Nieweg MB. Evidence-based practice for individuals or groups: Let’s make a difference. Perspect Med Educ. 2013;2(4):216-21. doi:10.1007/s40037-013-0071-2
Gonzalez Acosta D. Educating nursing staff on evidence-based maternal positioning to promote fetal descent during the first and second stages of labor. Master of Science in Nursing Project. San Francisco: University of San Francisco School of Nursing and Health Professions; 2023. repository.usfca.edu/capstone/1555
Hofmeyr GJ, Kulier R, West HM. External cephalic version for breech presentation at term. Cochrane Database Syst Rev. 2015;2015(4):CD000083. doi:10.1002/14651858.CD000083.pub3
Keag OE, Norman JE, Stock SJ. Long-term risks and benefits associated with cesarean delivery for mother, baby, and subsequent pregnancies: Systematic review and meta-analysis. PLoS Med. 2018;15(1):e1002494. doi:10.1371/journal.pmed.1002494
Nenko I, Kopeć-Godlewska K, Towner MC, Klein LD, Micek A. Emotional factors, medical interventions and mode of birth among low-risk primiparous women in Poland. Evol Med Public Health. 2023;11(1):139-48. doi:10.1093/emph/eoad013
Pullen RL Jr. Professional identity in nursing practice. Nursing Made Incredibly Easy! 2021;19(2):55-6. doi:10.1097/01.NME.0000732012.99855.78
Rosenstein MG, Chang S-C, Sakowski C, et al. Hospital quality improvement interventions, statewide policy initiatives, and rates of cesarean delivery for nulliparous, term, singleton, vertex births in California. JAMA. 2021;325(16):1631-9. doi:10.1001/jama.2021.3816
Treyster L. My drug-free VBAC during Covid. J Perinat Educ. 2022;31(1):6-7. doi:10.1891/JPE-2021-0030
Tully G. Monthly update: How to shorten labor, integrating Spinning Babies®, and more! Spinning Babies. January 6, 2021. spinningbabies.com/monthly-update-how-to-shorten-labor-integrating-spinning-babies-and-more
Waslia D, Nanik C. Effectiveness of moxa and hypnobirthing therapy for improvement of breech in trimester III for pregnant women. JOMIS (Journal of Midwifery Science). 2021;5(1):1-9.