Two-person skin assessment builds a foundation for pressure injury prevention.
- Pressure injury (PI) care bundles help to reduce variations in care and improve outcomes.
- PI care bundles should include risk assessment, support surface selection, patient turning, incontinence management, and nutrition.
An interview with Debra Crawford, BA, ADN, RN, CWOCN, CFCN. Crawford is the team and wound, ostomy, continence (WOC) nurse at Mercy Health Saint Mary’s Campus in Grand Rapids, Michigan.
Patient spotlight: The takeawayThe intensive review process at Mercy Health Saint Mary’s Campus has provided valuable insight into the causes and prevention of pressure injuries (PIs). For example, one middle-aged male patient was in so much pain after his leg surgery that he didn’t want to move. The result: an avoidable PI on his heel. The review process determined that he didn’t receive adequate pain medication to turn and position him properly. “He got angry when anyone tried to relieve the pressure on his heels,” says Crawford, “but if we had been on top of his pain medication, we could have prevented it. That’s the kind of thing that we can bring out in our review process and is a good takeaway for the nursing staff.” |
Intensive care unit (ICU) nurses face many challenges when caring for their patients and must sometimes focus on immediate life-saving interventions. Unfortunately, protecting the skin can get bumped down the priority list and lead to serious problems later.
“The skin is the largest organ in the body and deserves a lot of attention,” says Crawford. “When it breaks down, patients are prone to infection—and people can die from infection—so we can’t forget it.”
Another concern is that the Centers for Medicare and Medicaid Services (CMS) doesn’t reimburse for the treatment of hospital-acquired stage 3 and 4 pressure injuries (PIs). “In the ICU, we can no longer save a patient’s life today and worry about the skin tomorrow,” Crawford says.
The process: Two sets of eyes are better than one
PI prevention in the ICU at Mercy Health Saint Mary’s Campus begins the moment a patient is admitted. All patients receive a two-person nursing assessment that includes examining the entire skin. The assessment is repeated when a patient is transferred to another unit, and anytime a patient has been off a unit for more than 2 hours.
Risks are also evaluated and documented. Factors that make ICU patients especially vulnerable to PI include:
- some critical-care drugs, such as vasopressors, which can cause ischemia and tissue necrosis
- decreased level of consciousness
- lack of mobility and difficulty turning
- use of multiple medical devices that can cause pressure on the skin, such as respiratory devices and automatic blood pressure cuffs
- hemodynamic instability that’s worsened with physical movement
- history of surgery lasting longer than 3 hours
- need to leave the ICU for long periods, such as for dialysis or imaging procedures
- poor nutritional status before admission and possibly during hospitalization.
After each assessment, ICU nurses flag at-risk patients and those with skin changes in the electronic health record for a consult with a WOC nurse. “Sometimes it turns out to be nothing of concern, like a mole,” Crawford says, “but I would rather the nurses be vigilant than let anything questionable go.”
Skin championsHaving a unit-based skin champion is critical to a successful PI-prevention program. At Mercy Health Saint Mary’s Campus, staff nurses who learn best practices are highly effective skin champions in the ICU, as well as in medical-surgical, perioperative, and other units, according to Cox. One advantage is that skin champions engage their fellow staff nurses peer-to-peer. They also advocate for performance improvement, serve as on-the-spot resources, and motivate other staff nurses to take personal ownership in preventing PIs. |
The review: Diving deep
Despite the ICU’s best efforts, not all PIs are avoidable, according to Crawford. Unfortunately, no CMS criteria exist to determine if a PI was preventable. When a PI occurs at Mercy Health Saint Mary’s Campus, a collaborative team performs an intensive deep-dive review to determine if it was preventable. The team includes:
- clinical nurse specialists and leaders
- department manager and other hospital leadership
- WOC nurses
- unit skin champions
- nutritionist
- risk-management representative.
The review process includes the Indiana University Health Pressure Ulcer Prevention Inventory, which is an objective tool that determines if a PI could have been prevented. It includes these elements:
- Braden Scale for Predicting Pressure Sore Risk
- documented staff assessments
- whether appropriate interventions were performed based on the assessments.
“The Indiana University Health Pressure Ulcer Prevention Inventory minimizes subjectivity in judging whether our staff is doing a thorough job,” Crawford says. “We don’t encounter any surprises, and we’ve found that some PIs were unavoidable.”
Are all PIs avoidable?According to the 2010 National Pressure Ulcer Advisory Panel Consensus Conference, not all pressure injuries (PIs) are avoidable. With unanimous consensus, the panel declared that most—but not all—PIs are avoidable. The panel also determined that PIs may occur in some cases when a patient’s condition and risk status was thoroughly assessed, and appropriate interventions, evaluation, and revision of interventions were taken. |
SCALE: Skin changes at life’s end
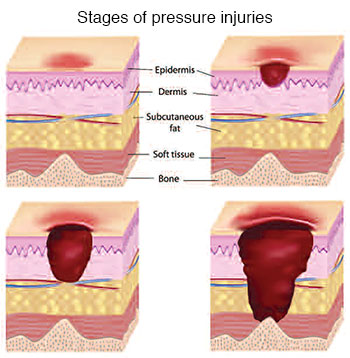

The key: Staff nurses
ICU staff nurses play a vital role in the deep-dive review process. They present their insight about the patient using the situation, background, assessment, and recommendation (SBAR) technique, which facilitates brief, organized, and clear communication about the patient.
“Not every detail gets documented in the chart,” Crawford says, “SBAR allows nurses to provide the real-world view, and their perspective of the patient and the situation.”
The team then presents the facts from the documentation, and they determine what can be done to prevent similar incidents in the future. Their findings are shared in written, photographic, and verbal form with leadership and all units.
Prevention: Build a foundation
Crawford believes that an effective review process and PI-prevention program is built on the foundation of the two-person skin assessment upon admission. “If you do your due diligence in the beginning, then you can say with certainty where the injury occurred, and investigate and address how it could have been prevented,” she says.
ResourcesNational Pressure Ulcer Advisory Panel. Best Practices for Prevention of Device-related Pressure Injuries in Critical Care Pittman J, Beeson T, Terry C, et al. Unavoidable pressure ulcers: Development and testing of the Indiana University Health Pressure Ulcer Prevention Inventory. J Wound Ostomy Continence Nurs. 2016;43(1):32-8. |
Catherine Spader is a medical and healthcare writer and editor in Littleton, Colorado.


















3 Comments.
It is most challenging to be able to have two RNs doing the skin checks. So, then the RN will ask a PCA (patient care associate) as her second choice to assist. They both are required to look at the skin but because the PCA is not allowed to assess, they can only call out what they believe the RN needs to look at again.
The greatest benefit of finding pressure injuries on admission is not having to own them! If they are found later, it cannot be determined if it was POA (present on admission or community acquired) and thus the facility owns it. It will then be determined to be a HAPI (hospital acquired pressure injury).
Debra Crawford, MSN, RN, CWOCN, CFCN
Team Leader, Wound, Ostomy, Continence Nurse
Mercy Health Saint Mary’s Campus
I would like to know what challenges you have come across in two nurse skin checks. What worked well?
For my team, it has not be much of a challenge to complete a two person skin assessment on the night shift as it is on the dayshift.