A medical intensive care unit implements mentorship to ease the transition from novice to practicing nurse.
Takeaways:
- After orientation is complete, newly hired nurses seek additional support from their peers.
- Mentorship programs can effectively support the emotional and professional health of novice nurses.
- Learn how to build a mentor program that meets the unique needs of new hires, supports a healthy work environment, and helps retain staff.
When adjusting to the fast-paced, frequently stressful atmosphere of a critical care unit, even the most knowledgeable nurses experience insecurity, uncertainty, and fear of failure. Patricia Benner’s novice-to-expert model describes a ladder of nursing skill acquisition (which can be aided by preceptors during orientation), but it doesn’t address the emotional journey involved. Mentor programs can positively influence new hires by supporting their emotional and professional health after formal training. Mentorship also is associated with increased career advancement and improved job satisfaction, which may increase nurse recruitment and retention.
The medical intensive care unit (MICU) at the University of Vermont Medical Center in Burlington developed and implemented an informal mentorship program to help support novice nurses as they transition into their staff roles.
Mentorship in action
In 2014, as a member of the practice council, I was tasked with conducting a survey of newly hired MICU nurses to assess challenges they face after orientation. In response to the survey, 33% of new nurses said they didn’t feel supported. Of those who did feel supported, many identified challenges and offered suggestions for improving the unit’s treatment of new hires; 100% of respondents felt that having a mentor might ease the transition from orientation to practice. The practice council reviewed the survey results and chose to move forward with creating a mentor program for new hires. I volunteered to research and build the program objectives, goals, and resource content. The council voted on the concepts and named me mentor coordinator. I formalized the materials and began recruiting mentors from among unit staff.
Newly hired MICU nurses complete a 14-week orientation called the Critical Care Nurse Internship, which includes class time, online exams, and a preceptorship. I designed the program to begin after orientation ends, when most new nurses reported a lack of support. The program’s objectives and goals were compiled in a reference guide that encourages mentors to share their expertise and experience, promote self-awareness, provide helpful feedback, and motivate their mentees. (See Guide for success.) As the mentor coordinator, I organized meetings and collected data about the program. I stepped down as mentor coordinator; that role still exists and is shared by two staff nurses. As full-time bedside nurses, they must complete their coordinator responsibilities in addition to regularly scheduled shifts (not to exceed 40 hours a week).
Guide for success
The University of Vermont Medical Center medical intensive care unit (MICU) mentor program reference guide offers mentoring best practices. Here’s an outline and summary of the guide’s contents.
| Reference Guide Outline | Content Summary |
|---|---|
| Definitions | • This section defines mentoring terms, including those specific to the MICU program. For example: MICU mentor—An advisor and supporter who shares knowledge and wisdom and is willing to invest time and energy to assist in the professional growth of your mentee. |
| Program objectives | • Provide support to our interns, easing them through the transition from orientation to staff nurse. • Increase retention rates of new staff members by creating a more supportive environment. • Contribute to a change in unit culture; creating more mentor relationships will help create a more welcoming, supportive atmosphere. |
| Expectations for mentors | • Provide support, advice, and assistance to your mentee using the toolkit as a guide to develop your relationship. • Make a conscious effort to adhere to the check-in schedule designed with the mentor coordinator and mentee. • Alert the mentor coordinator to any scheduling issues or changes in your ability to commit to the program. • Treat your relationship as a friendship and adhere to an expectation of confidentiality. |
| Program structure | • A mentor program can be formal or informal. The MICU’s program, which is designed to support interns as they transition to staff nurses, is informal and long-term. |
| Phases of mentorship | • The MICU mentor program is broken down into beginning, middle, and closing phases based on the Academy of Medical-Surgical Nurses’ Mentor Guide. |
| Examples of effective mentoring techniques | • External influences include the mentorship program model, mentorship support, and tools for successful mentor relationship tools • Internal influences include gender, personality, experiences, time availability, and learning and teaching styles. |
| External and internal influences on mentorship | • This section includes definitions of mentoring techniques. For example: Accompanying—making a commitment in a caring way and taking part in the learning process along with the mentee. |
| Core competencies of leaders and mentors | • This section explains the mentor competencies—self-awareness, strategic vision, and effective communication—developed by the Robert Wood Johnson Foundation Nurse Fellows program. |
| Tips for mentoring success | • Recommendations for successful mentoring include: o role modeling behavior |
| Check-in schedule | • Check-in schedules, based on mentor and mentee communication preferences and availability, are established at the initial mentee/mentor/mentor coordinator meeting. |
Informal approach
Formal mentorships typically have a defined end date and the mentor and mentee are matched by a third party. The MICU mentor program follows an informal model, which allows for a more natural, long-term relationship.
Research among mentored nursing students shows that mentees value the absence of strict guidelines to allow for maximum autonomy and flexibility according to individual needs and priorities. In the MICU program, new nurses select their mentors and together they determine the duration of the mentorship. In addition, the program doesn’t require the mentor to share the same schedule as the mentee, and in-person meetings are recommended but not required; instead, mentors and mentees can communicate via phone or email.
Mentor selection
When new nurses near the end of orientation, the mentor coordinators introduce them to the program. They’re given a workbook that outlines the program’s objectives and goals and offers suggestions about how to find the right mentor, including examining learning styles (for example, verbal vs. hands-on), knowledge gaps, and professional goals. Identifying their needs helps mentees recognize mentors who will suit them. Some new nurses choose mentors they’ve already developed a rapport with and look up to professionally, or the coordinator may make suggestions based on the mentee’s learning preferences, professional goals, and schedules. For example, if a new nurse wants guidance on end-of-life care, the coordinator might pair him or her with a mentor who has experience with palliative care. For mentees who want to regularly work with their mentors, the coordinator compares schedules and makes suggestions based on how often shifts overlap.
After a mentor is selected, the pair meets with the coordinator to outline expectations, confirm contact information, and establish a meeting schedule. These mentor-mentee meetings (check-ins) provide an opportunity for the new nurse to discuss personal challenges, ask for advice, or simply chat with the mentor. Check-ins occur at least once a week for the first month after orientation.
Outcomes
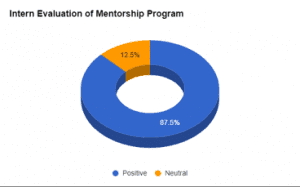
The mentor program has provided an added structure to new nurses’ transition into the MICU and helped to establish a mentoring culture among the unit staff. The mentor coordinators continue to gain valuable feedback via surveys aimed at assessing how well the program is meeting its objectives. Since the program began in 2014, all new nurses who responded to the surveys indicated that it has met its chief objective: Providing support to new nurses and easing them through the transition from orientation to staff nurse. Over 87% of survey respondents described their mentorship experience as positive. The remaining respondents indicated that they received support from other staff members and felt the program was unnecessary. These responses were categorized as neutral because they didn’t indicate a negative outcome but suggest that the unit is developing a mentoring culture. (See Positive outcomes.)
Staff retention was another objective of the program as turnover can affect the cohesiveness of the work environment, burden remaining staff, and negatively impact patient care. After new nurses are hired in the MICU, they’re asked to remain employed in the unit for at least 2 years. Since the program began, 70% of participating new nurses remain employed on the unit; only 10% left it before their 2-year contract was complete.
Positive outcomes
A survey of new nurses (interns) after participation in the University of Vermont Medical Center medical intensive care unit mentor program found that most (87.5%) said the experience was positive, while 12.5% said they found the program unnecessary because they received adequate support from other unit staff members.
Intern evaluation of mentorship program
Positive = 87.5%
Neutral= 12.5%
Other = 3.3%

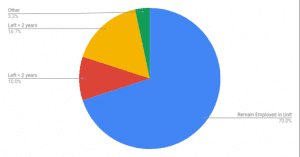
Since the introduction of the program, 70% of participating nurses have remained on the unit.
Left > 2 years = 16.7%
Left < 2 years = 10.0%
Remain employed in unit = 70.0%

Tips for success
Mentor program success depends on continuing assessment and leadership support.
Assessment
As part of the mentee survey, new nurses were asked how long they feel mentorship should continue to provide support: 50% of respondents recommended 2 to 3 months of support after orientation, 33% recommended up to 6 months, 8.3% recommended 1 month, and the remaining had different durations. Based on this new information, the mentor coordinators now ask mentors to support their mentees for a minimum of 2 to 3 months after orientation.
Leadership support
The mentor coordinator role has proven essential to the ongoing success of the program. And management support has been crucial to ensure the coordinator is allocated time and resources to meet with new nurse participants, update materials, and assess best practice solutions. Evidence shows that mentorship can be effective only if the unit and its leaders make a firm commitment to support it. According to Race and Skees, 84.8% of healthcare organizations view nursing staff retention as an imperative, but little evidence suggests that this attitude translates into operational practice. By dedicating hours to the coordinator role and developing a mentor program, leaders will reap long-term benefits of increased job satisfaction and retention.
The success of this program reflects directly on the practice council’s original commitment to support the mentor coordinator role and the veteran staff nurses who continue to volunteer as mentors, diligently working to provide support to new nurses and building a healthier work environment one mentorship at a time.
Emily Glassman is an RN III mentor coordinator in the medical intensive care unit at the University of Vermont Medical Center in Burlington.
References
Andersen T, Watkins K. The value of peer mentorship as an educational strategy in nursing. J Nurs Educ. 2018;57(4):217-24.
Aubrey R, Cohen P. Working Wisdom: Timeless Skills and Vanguard Strategies for Learning Organizations. San Francisco, CA: Jossey-Bass Publishers, Inc.; 1995.
Benner P. From novice to expert. Am J Nurs. 1982;82(3):402-7.
Brediger R. Developing a mentor program for our cardiovascular ICU. Crit Care Nurse. 2009;29(2):112.
Chiu YL, Chung RG, Wu CS, Ho CH. The effects of job demands, control, and social support on hospital clinical nurses’ intention to turn over. Appl Nurs Res. 2009;22(4):258-63.
Edmunds MW, Scudder LE. Turnover in nursing: Why nurses plan to leave their jobs. Medscape. January 8, 2010. medscape.com/viewarticle/714327
Hnatiuk CN. Mentoring nurses toward success. Minority Nurse. March 30, 2013. minoritynurse.com/mentoring-nurses-toward-success
Lombardo C, Wong C, Sanzone L, Filion F, Tsimicalis A. Exploring mentees’ perceptions of an undergraduate nurse peer mentorship program. J Nurs Educ. 2017;56(4):227-30.
Nowell L, White DE, Mrklas K, Norris JM. Mentorship in nursing academia: A systematic review protocol. Syst Rev. 2015;(4):16. ncbi.nlm.nih.gov/pmc/articles/PMC4342164
Nursing Solutions, Inc. 2016 National Healthcare Retention & RN Staffing Report. March 2016. avanthealthcare.com/pdf/NationalHealthcareRNRetentionReport2016.pdf
Race TK, Skees J. Changing tides: Improving outcomes through mentorship on all levels of nursing. Crit Care Nurs Q. 2010;33(2):163-76.



















3 Comments.
How do I get the workbook and assessments. I would live to make a mentoring program where i work.
Hi Stacey! Unfortunately they are not available for distribution but The Academy of Medical Surgical Nurses (AMSN) has great resources on their website including a mentor guide, mentee guide, and guide for a site coordinator.
As a nurse, I must agree that the approach to post-orientation new hires needs to be approached with fresh eyes among our health care peers. Through observation I have noticed this profession has a tendency to “eat their young”, however this mindset is not conducive when our shared profession is looking at higher demands of skilled nursing professionals while more nursing professionals are facing “burnout” and poor retention among health care organizations. To meet the growing demands within our profession we need to openly approach a new mindset to not only help train our new fellow professionals, but ensure they have the tools that are needed to grow and face the challenges of our ever growing patient population due to the increased longevity our population is experiencing. By creating a culture of mentorship within a department is a great way to promote such growth for our newly developing health care professionals. This culture needs to be nourished and promoted among other departments help retain quality professionals, as proven by the statistics your article provided.
As these programs for mentorship post-orientation are implemented though, mentorship for the mentors may be needed. Mentors should demonstrate leadership skills such as decision making, prioritizing, and delegating, and to ensure that these skills are honed to perfection resources need to be available to the mentors either via class time, electronic or in a classroom, reading material, and any other tool necessary to ensure the mentor can efficiently communicate and mentor the new healthcare professional (Kennedy, 2019). By ensure the mentor has been given the right tool kit to provide a professional mentorship for the new health care professional, mentee can excel and grow to be an asset to the unit.
References
Kennedy, A. (2019). Nurse preceptors and preceptor education: implications for preceptor programs, retention strategies, and managerial support. Medsurg Nursing. 28(2), 107-113. Retrieved from https://6o3243erg-mp02-y-https-search-proquest-com.prx-herzing.lirn.net/nahs/docview/2213045136/71B0E5E6C6CF4127PQ/5?accountid=167104