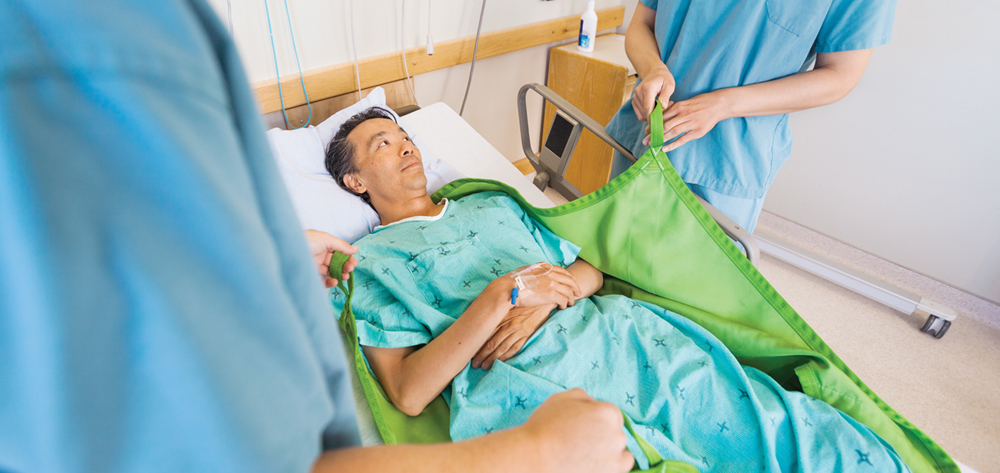
To avoid injuring their patients and themselves, healthcare providers must get in the habit of using safe patient handling and mobility (SPHM) technology. In this supplement, national experts share their perspectives and best practices on topics ranging from dealing with bariatric patients, managing slings, and assessing a patient’s mobility to transforming the culture, building the business case for an SPHM, and developing a successful SPHM program.
Download a PDF of the entire supplement here.
Since safe patient handling and mobility (SPHM) efforts began more than a decade ago, data show dramatic reductions in caregiver injuries after a safe patient handling and mobility (SPHM) program is implemented. So why doesn’t every healthcare facility have one?
The first reason is cost. An SPHM program requires a substantial outlay. Second, SPHM program results have been inconsistent. Tales abound of equipment bought but not used because it’s too much trouble to fetch it from the closet, or because no one can locate the necessary sling. Finally, SPHM program value costs are clear but benefits are hard to quantify.
This article addresses these issues by laying out the basic elements of a successful SPHM program. These elements can be divided into two broad categories—determining out what you need and making it happen. (See Simplifying the equation.)
Determining what you need
Start by estimating how many patients on a given unit are totally dependent on the nurse to lift or mobilize them. Then estimate how many patients on the unit need partial assistance with mobility activities, such as toileting or moving from bed to chair.
For each patient category, estimate the numbers and types of mobilization each will need over the course of an average stay. Types of mobilization include boosting, turning, moving from bed to chair, assisting with ambulation, and so on. For these categories and frequencies of mobilization tasks, figure out how much and what types of equipment are needed to eliminate variation in practice and standardize how to safely accomplish the task.
In practice, most people develop rules of thumb or use intuition and experience rather than calculating the four types of information described above. Also, vendors of handling and mobility equipment have experience in determining required equipment.
I’ve observed three different approaches to supplying the equipment needed to mobilize patients:
- installing overhead lifts—ceiling tracks to which lifting slings are attached
- using portable lifts—floor-mounted structures for mobilizing patients that can be moved around as needed
- going the “equipment light” route—using a low-tech system that combines slide sheets, limb lifters, and slide boards to mobilize patients instead of using ceiling-mounted or portable floor lifts.
Any of these approaches will work to mobilize patients and reduce caregiver injuries if the healthcare organization can get staff to use them.
Compliance rate
When designing and implementing an SPHM program, the compliance rate is the key variable an organization is driving. The compliance rate is defined as the number of mobilizations for which SPHM equipment is actually used, divided by the number of mobilizations for which it should be used. The compliance rate is critical because it drives program benefits.
A rate of 0% means the equipment is never used and isn’t producing benefits. A rate of 100% means caregivers are using the equipment every time they should be, creating the maximum possible value from the SPHM program.
A small level of investment in SPHM equipment makes little difference in the compliance rate or program results. Without the right amount or type of equipment available, an organization can’t standardize a new mobilization process, so the equipment gets used for relatively few mobilizations. With higher investment levels, using the equipment becomes part of caregivers’ routine, so the compliance rate goes up.
Making it happen
A successful SPHM program requires leadership commitment, nursing commitment, and an education and training plan. Leadership commitment is needed to approve SPHM equipment purchase, design of training plans, and time away from duty for training. Such commitment is best obtained by creating a business case to describe the proposed SPHM program and quantify its total costs and benefits, including return on investment (ROI). (See “Making the business case for a safe patient handling and mobility program” in this report.)
The entire nursing staff must be committed, especially the chief nursing officer, who has to approve the time required for staff training and education. Nursing commitment should be easy to get if the business case has identified the program’s potential for reducing caregiver injuries, increasing staff availability for duty due to injury reduction, and improving nursing retention and satisfaction.
An education and training plan addresses which SPHM technology is purchased, installed, and deployed and when and where it’s installed and deployed; who gets trained, at what level of training, and when training takes place; and how program data will be tracked and monitored to determine if it’s achieving the intended results. In many cases, training accounts for half or more of total SPHM program costs.
Levels of expertise
Three levels of expertise in using SPHM equipment and methods exist:
- A facility champion can “train the trainers” and aid program design and revision (adjusting the deployed equipment or training if needed). To be effective, this person needs both extensive training and experience.
- A super user (such as a unit peer leader at the Veterans Health Administration) can train other caregivers in the unit and answer questions. Reaching this level of expertise requires in-depth training.
- A general caregiver knows how to use SPHM technology and methods but may not be qualified to train others.
Why feedback is important
Feedback is crucial for tracking and monitoring the SPHM program to determine how well it’s working. Successful programs use two types of feedback. Compliance rate monitoring gives some reassurance that caregivers actually are using SPHM technology when they should be. Such monitoring may be done indirectly by requiring annual staff certification to ensure they know how to use the equipment. Direct methods include observing the unit to see if caregivers use appropriate SPHM methods. Some newer types of equipment come with devices to measure how many times they’re used.
Program result monitoring, on the other hand, depends on SPHM program goals. These vary by
facility but may include reduced caregiver injuries from patient handling, decreases in pressure
ulcers and patient falls, increased patient and staff satisfaction, and improved staff retention. The business case and ROI for the SPHM program should identify which program results create the most value. Methods for monitoring these results should be created if they don’t already exist.
Most SPHM programs monitor workers’ compensation costs from caregiver injuries related to patient handling. Usually, this necessitates connecting incidence data on the types and causes of injuries (such as on the Occupational Safety and Health Administration’s Form 300) with costs associated with those injuries (found in the workers’ compensation system).
Any equipment strategy (overhead lifts, portable lifts, “equipment light” or a combination) can drive a high compliance rate and favorable program results. But using more efficient lifting methods and equipment might yield additional program benefits from time savings. Stanford University Medical Center compared the average time for a chair-to-bed transfer
using ceiling lifts vs. portable lifts. On average, a ceiling-lift transfer was completed before the portable-lift transfer even began. These data were used to justify ceiling lift installation in Stanford’s new hospital.
Monitoring SPHM program results and comparing them against the potential results quantified in the business case are crucial for ensuring the program is working as designed and the organization is realizing the projected ROI. When results vary from the ranges identified in the business case, the cause must be identified and remedial action must be taken.
Understanding and implementing the essential elements of an SPHM program will help you ensure that your organization’s program is successful and can truly achieve better outcomes for caregivers and patients.
Selected references
Department of Veterans Affairs, Veterans Health Administration. VHA Directive 2010-032. Safe Patient Handling Program and Facility Design. June 28, 2010. www.va.gov/vhapublications/
ViewPublication.asp?pub_ID=2260. Accessed July 3, 2014.
Hodgson MJ, Matz MW, Nelson A. Patient handling in the Veterans Health Administration: facilitating change in the health care industry. J Occup Environ Med. 2013;55(10):1230-7.
John Celona is a principal at Decision Analysis Associates, LLC, in San Carlos, California. He is the author of Decision Analysis for the Professional, 4th ed.