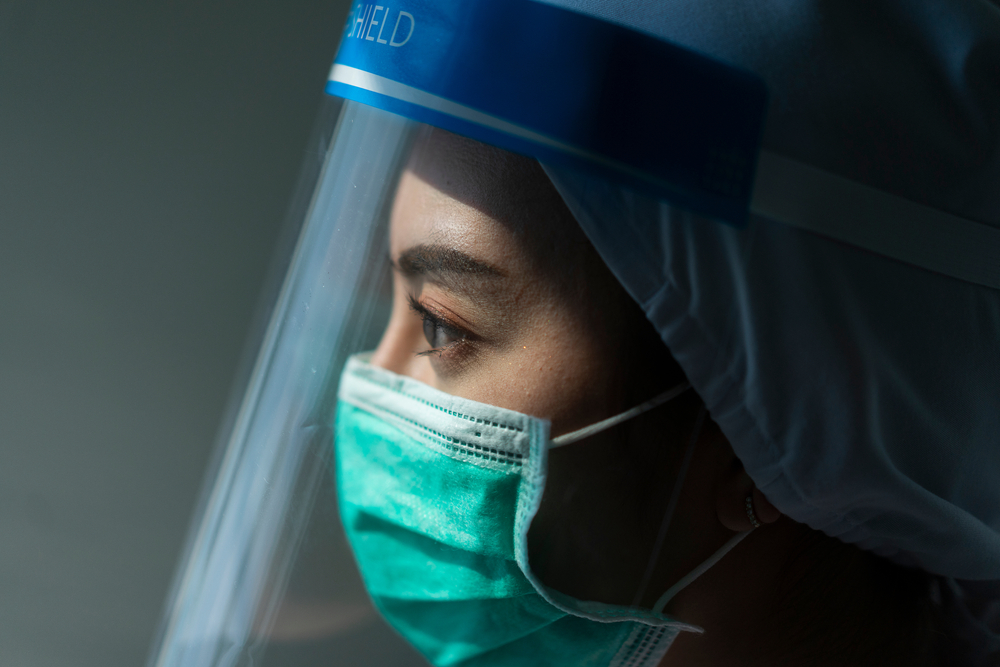
Decision-making during a healthcare crisis.


Tough decisions may need to be made about which patients should be given medical treatment and when, if at all. Other tough decisions include reporting for duty, testing healthcare workers, quarantine, diminished patient privacy, and scarce resource allocation. In fact, what we consider to be healthcare ethics may be turned upside down. Because a severe influenza pandemic puts hospitals under extreme stress—only so many beds, ventilators, nurses, and physicians will be available—more patients may require medical attention than can be fully treated.
An ethical consensus exists that healthcare workers have a prima facie duty to work because of everything that has been invested in them, because of their unique position (not just anybody can replace them), because society looks to them to serve this function, and because they went into this profession and are expected to go to work. However, the obligation of healthcare workers isn’t absolute. If a hospital can’t provide even a basic level of safety for its employees, it’s not a place to treat patients—it’s a hub to exacerbate the problem.
One difficulty we all face is access to sufficient personal protective equipment (PPE). An example of a simple, practical way to share resources is what the governor of New York proposed as a response to needs related to the COVID-19 pandemic: Because the disease strikes different areas of the country at different times, we can shift access to PPE and ventilators by sharing them with areas in greatest need (and no area of the country should be deprived of the minimum needed to serve its patients). But sharing would have to be not only fair, but national—such decisions must be made on a national level.
Triage is the process of sorting patients in a time of crisis to determine who receives what level of medical attention. How hospitals sort patients to determine treatment priority and what criteria are used pose major issues. Decisions on the allocation of healthcare resources are, at their core, moral decisions and sit within the framework set out by classical biomedical ethics. Healthcare is always in tension between what care and therapy can in theory be offered and which patients they’re offered to. Although not always explicit in everyday prioritization decisions, provision of care to one patient or group of patients often means that another goes without as we negotiate the balance between beneficence and distributive justice. However, when healthcare resources are acutely overwhelmed, the utilitarian principle of the greatest good for the greatest number is preeminent.
The principles behind decision-making are that it should be open, transparent, accountable, and reasonable. Under the last criterion, reasonableness, the guidance suggests that decisions should be rational, based on best evidence (not arbitrary), and practical. Such principles are advanced by the U.S. Centers for Disease Control and Prevention ethical subcommittee, but they have additional criteria: consistent application of guidelines, treating all patients alike, minimizing individual interpretation [author’s emphasis], and decision-maker impartiality and neutrality.
– Leah Curtin, RN, ScD(h), FAAN, Executive Editor, Professional Outreach, American Nurse Journal
Reference
Kinlaw K, Barrett DH, Levine RJ. Ethical guidelines in pandemic influenza: Recommendations of the Ethics Subcommittee of the Advisory Committee of the Director, Centers for Disease Control and Prevention. Disaster Med Public Health Prep. 2009;3(suppl 2):S185-92.