Preventing, assessing, and treating trauma suffered by families of a hospitalized loved one.
Takeaways:
- 14% to 50% of family members with loved ones in an intensive care unit (ICU) may develop post-ICU syndrome-family (PICS-F).
- Family presence, family education, family/patient diaries, and family participation in care can help prevent PICS-F.
- Nurses in acute care settings can act early to prevent PICS-F.
- Nurses in ambulatory and community settings can assess and begin treatment for PICS-F.
By K. Renee Twibell, PhD, RN, CNE; Amber Petty, BSN, RN, CCRN; Amanda Olynger, BSN, RN, CCRN; Sheila Abebe, DNP, APRN, FNP-BC
Jennifer* leaned wearily against the bathroom wall and murmured, “What happened to my life, my world? How could this be? It’s like a bad dream.” Her distressed reflection in the mirror offered no word of explanation for how her daughter’s 3-week hospitalization could change life so drastically.
Jennifer and Megan are a family of two, sharing a home that has a small garden, enjoying friends, and working. When the phone call came about Megan’s car accident, Jennifer suddenly found herself in a new, unknown world of lab tests and ventilator settings.
When Jason, an experienced intensive care unit (ICU) nurse, asks Jennifer how she’s doing, Jennifer blurts out with unexpected emotion, “I don’t know how I’m doing! It’s all a blur—lying here beside her bed each night, alarms ringing, no sleep, different caregivers every day, no visitors because she’s in isolation…. How do you think I am doing?” Jason touches Jennifer’s arm lightly and nods, prompting her to add tearfully, “And today we move to a long-term care facility, and no one will even tell me if she’s going to live or die!”
Jason recognizes that Jennifer is at risk for post-intensive care syndrome in family members.
PICS and PICS-F defined


Symptoms
PICS-F begins with a perceived or actual threat to the life or physical integrity of a family’s loved one who’s hospitalized in a critical care unit. During hospitalization, family members may begin to have symptoms of PICS-F, but it’s typically not diagnosed until the symptoms persist for at least 1 month after the patient is discharged. (See Recognizing symptoms.) Symptoms can interfere with home and work responsibilities and make caring for loved ones after discharge difficult.


Timeline and prevalence
PICS-F symptom intensity varies, so the syndrome’s trajectory fluctuates. Acute symptoms may last for months, even years; PICS-F data show that symptoms can persist for 8 years, the longest period for which the data exists.
Estimates of the prevalence of PICS-F typically range from 14% to 50%. This wide range may be related to differences in how the syndrome is defined across settings, different assessment approaches, different times when assessment occurs, and different patients and families. For example, the prevalence of PICS-F is as high as 80% when families have to make surrogate end-of-life decisions with inadequate support and as high as 65% if the patient dies.
Risk factors
Factors that heighten the risk of developing PICS-F include patient and family characteristics, as well as the critical care unit’s environmental characteristics. (See Knowing the risk factors.) The characteristics most amenable to nurses’ preventive actions are those in the critical care environment and those related to family’s needs.
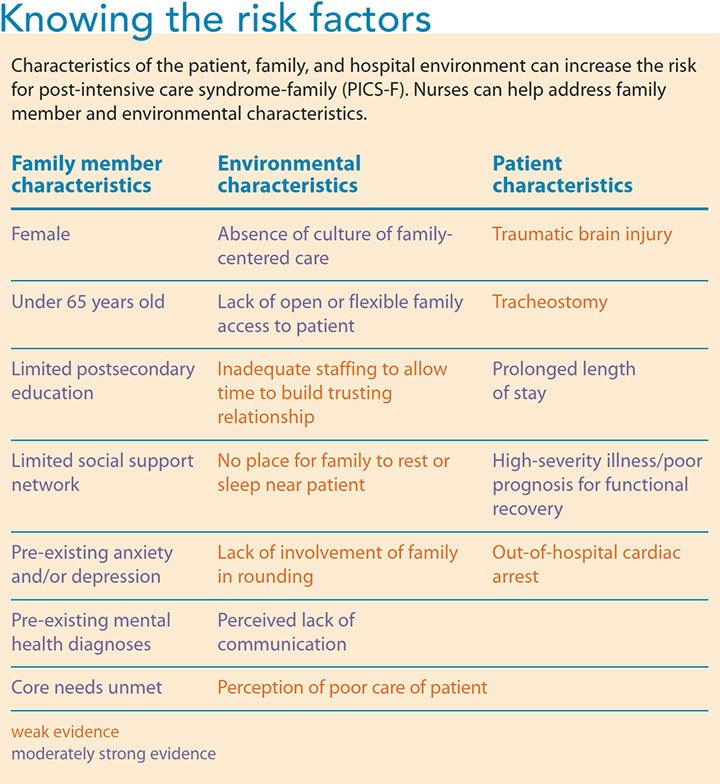

Jason recognizes Jennifer’s risk factors related to her age, gender, Megan’s tracheostomy, the severity of Megan’s injuries, and Jennifer’s unmet need for information. He notices Jennifer’s anxiety and fatigue and asks if she has a history of anxiety, depression, or post-traumatic stress disorder(PTSD).
Assessment
During a patient’s hospitalization, nurses may detect early symptoms and risk factors for PICS-F, but screening tools to predict its development don’t yet exist. Research studies use scales (such as the Hospital Anxiety and Depression Scale, Impact of Events Scale, Center for Epidemiologic Studies—Depression Scale, Stanford Acute Stress Reaction Questionnaire, and the Davidson Trauma Scale) to measure anxiety, depression, and PTSD.
Lack of valid screening tools appropriate for use at the bedside means PICS-F can go unrecognized and untreated. However, nurses can evaluate and document patient and family characteristics that increase risk by asking family members to rate environmental characteristics of the hospital unit and the extent to which the healthcare team is meeting their key needs. (See What families need.)


Prevention interventions
Guidelines from the Society for Critical Care Medicine (SCCM) offer specific family-centered interventions during hospitalization for critical illness. The guidelines and research support four key interventions—family presence, family education, patient/family diaries, and family participation in care—that may mitigate or prevent the development of PICS-F.
Family presence
Providing the family with liberal access to the patient—even during life-threatening events such as resuscitations—addresses the family’s need for proximity to the patient and timely information. This evidence-based best practice is supported by multiple studies and several healthcare organizations, such as the American Association of Critical-Care Nurses (AACN), the American College of Critical Care Medicine, and SCCM. AACN offers evidence-based guidelines for family presence in critical care units.

Lack of communication is the leading complaint of dissatisfied family members during critical illness. Letting them be with the patient and sharing timely information in the family’s language builds trust. Nurses have five routine opportunities to provide updates to families at the bedside.
- Bedside report: Family members and patients can listen to nurses’ end-of-shift handover report, ask questions, and make suggestions for care.
- Five minutes at the bedside: Nurses sit for at least 5 minutes near the beginning of each shift to listen to patients and families, to provide emotional support and information, and to set goals.
- Communication boards: Nurses can update boards posted in patients’ rooms to convey goals and planned tests or procedures for the day.
- Hourly rounding: When nursing personnel round on patients and families every hour, they can offer updates and listen to questions.
- Narrating care: As nurses deliver bedside care, they can talk about what they’re doing and why as a way of educating the family and sharing real-time information. For example, Jason can say to Jennifer, “I’m checking Megan’s drain, and it looks like the bleeding has stopped after the platelets we gave her.”
Healthcare team support of family members is especially important during ICU admission. One study found that up to half of parents who had a child admitted to a pediatric ICU had negative, intrusive memories from the early hours of hospitalization. Mothers who had the opportunity to talk about their feelings at the time of the admission had significantly lower PTSD stress scores at 8 months.
Jason sits by Jennifer and asks how the healthcare team can communicate better and what information she needs right now. She requests a family conference before Megan is transferred to long-term care.
Family education
Family education strengthens coping strategies and reduces anxiety, depression, and the risk of PICS-F. Education can occur informally when nurses assess family members at the bedside as being at risk for PICS-F. More structured family education programs, provided by an interprofessional team that includes a psychologist or psychiatrist, can deliver information on PICS-F, new coping skills, strategies for self-care, and cognitive-behavior techniques. Written information serves to reiterate key content.
Nurses can coach family members to develop self-awareness and ask for support when they need it, so that they can stay balanced throughout their loved one’s recovery. In addition, family members may benefit from a written list of community resources for support after leaving the hospital. (See Resources.)


Patient/family diaries
Family diaries kept at the bedside can help mitigate or prevent PICS-F. Nurses take the lead, documenting events, the patient’s condition, and vital educational points. Families then make their own entries in the diaries; interprofessional team members also may contribute. These diary entries can help reinforce real memories, not imagined ones. Nurses can give the diary to the family when the patient is discharged from the ICU; most patients and families report reading the diaries after discharge. Although research shows significantly less PICS among patients who keep diaries, the effect on PICS-F isn’t yet clear.
Family participation in care
Nurses can engage family members in providing emotional support to the patient. One study revealed that patients wanted family members to talk with them about life outside of the ICU. Some family members can safely provide hygiene care, assist with range-of-motion exercises, and provide oral fluids or food. In many cases, family members experience less stress when they know what their loved one will need after discharge and develop confidence that they can provide that care. Most important, family members can be involved in decision-making if the patient is unable to participate in decisions. Surrogate family decision-makers need extensive information, dialogue, support, and affirmation to prevent PICS-F.
Treatment interventions
Treatment can begin when symptoms of PICS-F are noted at least 1 month after patient discharge. In addition to family education, two interventions may help—interprofessional post-ICU clinics and family support groups.
In some parts of Europe, post-ICU clinics have been used for decades, but outcomes measurement is weak. These outpatient clinics, led by nurses or an interprofessional team, typically focus on patient mobility and mental health/cognitive needs; however, recently, family members have started to attend some clinics. Family members may be assessed for post-ICU adjustment difficulties, acquire education on PICS-F, and receive resources or referrals to providers or support groups for follow-up. Research should explore how post-ICU clinics can more comprehensively include families to address PICS-F.
Family support groups provide validation and a sense of belonging. Participants gain practical knowledge from those ahead of them in the healing process, and they can learn self-care strategies and share resources for trauma resolution. Support groups, which can be nurse-led or lay-led, usually aren’t held at a hospital, so family members with PICS-F can avoid painful memories. SCCM has developed the THRIVE initiativeto improve patient and family support after critical illness, including a post-ICU community of volunteer peer-led support groups.
Jason talks with Jennifer at Megan’s bedside about PICS-F and gives her a list of local support groups and a brochure about leaving the ICU. He contacts the nurses who will care for Megan in the long-term care facility and asks them to observe Jennifer and to refer her to community resources if needed. Jason asks Jennifer for permission to contact her primary care provider and explain what Jennifer is experiencing.
Nurses’ role in ambulatory care
When patients transition out of the hospital, PICS-F management must occur in ambulatory care and community settings. Healthcare personnel in these settings may need education on PICS-F to screen family members. Key questions on an initial assessment may include:
- How would you rate your current physical functioning compared to before your loved one’s hospitalization?
- How would you rate your current cognitive functioning, including your memory, compared to before your loved one’s hospitalization?
- How would you rate your current emotional functioning, including anxiety and depression, compared to before your loved one’s hospitalization?
- Have you been sleeping adequately? Any insomnia or nightmares?
- Have you been able to return to work and your normal daily activities?
- Have you been more fearful or anxious lately?
- Have you noticed any “triggers” associated with the hospitalization that may be causing increased stress, anxiety, or worries?
If healthcare personnel recognize symptoms of PICS-F 1 month or more after a family member’s ICU stay, follow-up questions may include:
- What resources are you aware of that provide emotional and mental health support during times of adjustment in life?
- What resources have you accessed so far and what care have you received?
- What’s been most effective at improving your physical, cognitive, and mental functioning since your loved one was hospitalized?
- In what area of your adjustment do you most need additional support?
Aiding a transition to a new world
PICS-F can diminish family members’ quality of life after a loved one’s critical illness. Nurses in acute-care settings can act early to prevent it, and nurses across the care continuum can be educators and spokespersons about PICS-F. Astute nursing assessment, care coordination, nurse-family relationship building during the ICU stay, and connections with community resources after patient discharge can mitigate the effects of PICS-F and offer families serenity, even in what might be a new world post-ICU.


K. Renee Twibell is an associate professor in the school of nursing at Ball State University and a nurse researcher at Indiana University (IU) Health Ball Memorial Hospital in Muncie. Amber Petty is a clinical nurse at IU Health Ball Memorial Hospital. Amanda Olynger is a clinical nurse at IU Health Ball Memorial Hospital. Sheila Abebe is an assistant professor in the school of nursing at Ball State University and a board-certified family nurse practitioner at IU Health Business Solutions.
*All names are fictitious.
Selected references
Adelman RD, Tmanova LL, Delgado D, Dion S, Lachs MS. Caregiver burden: A clinical review. JAMA. 2014;311(10):1052-60.
Beg M, Scruth E, Liu V. Developing a framework for implementing intensive care unit diaries: A focused review of the literature. Aust Crit Care. 2016;29(4):224-34.
Coombs M, Puntillo KA, Frank LS, et al. Implementing the SCCM family-centered care guidelines in critical care nursing practice. AACN Adv Crit Care. 2017;28(2):138-47.
Curtis JR, Treece PD, Nielsen EL, et al. Randomized trial of communication facilitators to reduce family distress and intensity of end-of-life care. Am J Respir Crit Care Med. 2016;193(2):154-62.
Davidson JE, Aslakson RA, Long AC, et al. Guidelines for family-centered care in the neonatal, pediatric, and adult ICU. Crit Care Med. 2017;45(1):103-28.
Davidson JE, Harvey MA, Schuller J, Black G. Post-intensive care syndrome: What it is and how to help prevent it. Am Nurse Today. 2013;8(5):32-8.
Davidson JE, Jones C, Bienvenu OJ. Family response to critical illness: Postintensive care syndrome-family. Crit Care Med. 2012;40(2):618-24.
Davidson JE, Zisook S. Implementing family-centered care through facilitated sensemaking. AACN Adv Crit Care. 2017;28(2):200-9.
Dettling-Ihnenfeldt DS, De Graaff AE, Nollet F, Van Der Schaaf M. Feasibility of post-intensive care unit clinics: An observational cohort study of two different approaches. Minerva Anestesiol. 2015;81(8):865-75.
Garrouste-Orgeas M, Coquet I, Périer A, et al. Impact of an intensive care unit diary on psychological distress in patients and relatives. Crit Care Med. 2012;40(7):2033-40.
Harvey MA. Mitigating PICS. Society of Critical Care Medicine. 2016. sccm.org/Communications/Critical-Connections/Archives/Pages/Mitigating-PICS.aspx
Harvey MA, Davidson JE. Postintensive care syndrome: Right care, right now…and later. Crit Care Med. 2016;44(2):381-5.
Hetland B, Hickman R, McAndrew N, Daly B. Factors influencing active family engagement in care among critical care nurses. AACN Adv Crit Care. 2017;28(2):160-70.
Huggins EL, Bloom SL, Stollings JL, Camp M, Sevin CM, Jackson JC. A clinic model: Post-intensive care syndrome and post-intensive care syndrome-family. AACN Adv Crit Care. 2016;27(2):204-11.
Huynh TG, Covalesky M, Sinclair S, et al. Measuring outcomes of an intensive care unit family diary program. AACN Adv Crit Care. 2017;28(2):179-90.
Hwang DY, El-Kareh R, Davidson JE. Implementing intensive care unit family-centered care: Resources to identify and address gaps. AACN Adv Crit Care. 2017;28(2):148-54.
Jacob M, Horton C, Rance-Ashley S, et al. Needs of patients’ family members in an intensive care unit with continuous visitation. Am J Crit Care. 2016;25(2):118-25.
Kleinpell R, Buchman TG, Harmon L, Nielsen M. Promoting patient- and family-centered care in the intensive care unit: A dissemination project. AACN Adv Crit Care. 2017;28(2):155-9.
Kross EK. The importance of caregiver outcomes after critical illness. Crit Care Med. 2015;43(5):1149-50.
Kynoch K, Chang A, Coyer F, McArdle A. The effectiveness of interventions to meet family needs of critically ill patients in an adult intensive care unit: A systematic review update. JBI Database System Rev Implement Rep. 2016;14(3):181-234.
Khan BA, Lasiter S, Boustani MA. Critical care recovery center: An innovative collaborative care model for ICU survivors. Am J Nurs. 2015;115(3):24-31.
Needham DM, Davidson J, Cohen H, et al. Improving long-term outcomes after discharge from intensive care unit: Report from a stakeholders’ conference. Crit Care Med. 2012;40(2):502-9.
Post-intensive care syndrome. Society of Critical Care Medicine. 2013. myicucare.org/Thrive/Pages/Post-intensive-Care-Syndrome.aspx
Ullman AJ, Aitken LM, Rattray J, et al. Intensive care diaries to promote recovery for patients and families after critical illness: A Cochrane systematic review. Int J Nurs Stud. 2015;(7):1243-53.
Wolters A, Bouw M, Vogelaar J, Tjan D, van Zanten A, van der Steen M. The postintensive care syndrome of survivors of critical illness and their families. J Clin Nurs. 2015;24(5-6):876-9.
ant4-CE Family-322a




















2 Comments.
I am writing in regard to the article “Families and post-intensive care syndrome,” by K. Renee Twibell, Amber Petty, Amanda Olynger and Sheila Abebe, in the Vol. 13 No. 4 April 2018 issue. I was thrilled with the tools this article gave me to better care for the family of my critical care patients. The five routine opportunities to provide updates to families at the bedside are not only helpful to prevent post-intensive care syndrome-family (PICS-F); they help the patient receive the best possible treatment from the care team. The purpose of this letter is to show how frequently updating the family and providing a platform for questions and concerns helps the patient receive a higher quality of care.
The five routine opportunities to provide updates to families from the article—bedside report, five minutes at the bedside, communication boards, hourly rounding and narrating care—give family members a sense of comfort and control. Through talking to the family about their questions and concerns, there is also an opportunity for introspection from clinical staff and providers. There are holistic care approaches and areas of improvement that can only be identified by the family; they know the patient as an individual outside of the hospital. In addition, through answering questions that the family has, the nurses and providers have the opportunity to question the ways things are typically done and further individualize the care to the patient.
I am a new nurse—I have found, it is often the simple questions that family ask that have caused me to grow the most in my practice. My patient’s wife once asked me “why has my husband’s nutrition been stopped? Won’t he be getting weaker now?” Through careful thought and discussion with the care team, it was clear this was a necessary and temporary move, until the root cause of the patient’s abdominal pain was discovered and resolved. Through this family member’s question, it caused me to re-evaluate my priorities for the day. Yes, it is vital to find the root cause of a condition. However, if the root cause is discovered and resolved, and the patient is too weak to go home after the resolution, we have done them a disservice. This situation taught me that physical therapy should remain one of the priorities while awaiting a diagnosis.
Providing the best possible care is a priority in the minds of healthcare workers. Forming relationships with the family through giving them a platform to speak not only allows better communication, but it offers a sense of control when a loved one is in an intensive care unit. The five routine opportunities to provide updates to families at the bedside add to the prevention of PICS-F and keep healthcare workers introspective. Through introspection comes growth. With growth of the nursing and clinical staff, the patient may receive the highest quality of care possible.
Sincerely,
Karina Osswald, ADN, RN
Could type 2 diabetes be a component of the post-intensive care syndrome?
Best,
Victor