Gentle peer reminders, incentives, and fun lead to success.
Takeaways:
- Hand hygiene is the best way to prevent the spread of healthcare associated infections but nurse and other healthcare provider adherence with hand hygiene practices continues to be a challenge.
- Using an interactive audit and feedback strategy via an innovative “splat” game helped improve hand hygiene adherence in this large academic medical center.
Hand hygiene is the best way to prevent the spread of healthcare-associated infections (HAI) in hospitals. However, hand hygiene adherence among nurses and other healthcare providers is a challenge. Several types of hand hygiene campaigns have been implemented in organizations, including new signage, reminders, audits, and updated hand hygiene dispensers and locations. These interventions may yield short-term improvement, but to maintain improvement over time, hand hygiene practice must be engrained into a unit’s culture.
The hand hygiene compliance scores for nursing staff in the neuroscience stepdown unit at our large academic medical center was less than the hospital’s target of 90%. In response, a hand hygiene campaign, using an interactive “splat” game, was developed by a nurse and implemented by nursing staff.
Interactive learning
Previous studies have used various forms of educational games to improve healthcare workers’ knowledge and adherence to infection prevention and control practices. Akl and colleagues published a systematic review to assess the effectiveness of educational games on healthcare professionals’ performance. One study included in the review (Burke) used a game based on the “Family Feud” television show and reported that the group randomized to the game had statistically higher scores on the knowledge test (p = 0.02). Another study (Telner) compared game-based learning using the “Snakes and Ladders” board game with traditional case-based learning. Although significant improvement in knowledge didn’t occur after 3 months with either intervention, participants in the board game group reported higher levels of enjoyment during learning.
Implementation science literature shows that interactive strategies can contribute to better performance and adherence to evidence-based practices by healthcare workers. In addition, audit and feedback strategies have been shown to improve adherence by providing routine actionable feedback on an individual’s behavior.
Let’s play
Hand hygiene compliance is a key quality indicator in our hospital, so the splat game was supported by nursing unit leadership, which is an important component to any successful project. For this game, which was played over the course of 1 month, each staff member (RNs, nursing assistants, and hospital unit coordinators) was given five small, laminated “splat” cards at the beginning of their shift. Each card had a picture of a germ and a reminder to perform hand hygiene. During the course of each shift, nursing staff were encouraged to audit their peers and colleagues for missed hand hygiene opportunities. When a staff member noted a peer or colleague not performing hand hygiene when entering or exiting a room, a card was handed to them as a gentle reminder. Nursing staff could give a card to any healthcare professional on the unit, including other nurses, physicians, advanced practice providers, speech therapists, occupational and physical therapists, and pharmacists. (See Splat cards.)
At the end of the shift, healthcare workers and providers handed in their cards to the charge nurse and a new game began for the next shift. Those with no cards at the end of the day were entered into a raffle to win a prize during safety week. The first person on each shift to give all their cards away and not obtain any cards in return were given coffee gift cards donated by the medical director.
And the winner is…
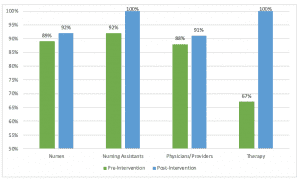
This campaign helped improve peer-to-peer accountability and adherence to hand hygiene in a fun, nonthreatening way. At our hospital, hand hygiene adherence is measured through observation audits completed by two dedicated hand hygiene auditors. After implementing the game, overall hand hygiene adherence on the unit increased from 87.2% in fiscal year 2017 to 90.4% in fiscal year 2018. Compliance has continued to improve since then and is currently 96.4% year to date. In addition, when hand hygiene compliance increased, the unit Clostridium difficile infection rate decreased from 16.87% (6 months before the intervention) to 3.72% (6 months after the intervention). (See Everyone wins.)
The game itself wasn’t expensive; the main items needed are laminated cards, but creating the cards was time-consuming. We also incurred costs associated with the prizes distributed to raffle winners. Overall, nursing leadership and staff agree that the benefits of improving hand hygiene adherence outweigh the cost of the game’s supplies.
Challenges
The most significant challenge with any improvement project is achieving staff buy-in and engagement. One potential disincentive to engagement is staff perception that receiving a splat card is a punitive measure rather than a helpful peer-to-peer reminder. To help reduce the potential for this barrier, we permitted any healthcare workers who didn’t want to “actively” play the game to remain “passive” players. This meant that although they wouldn’t hand out cards, they would still be responsible for proper hand hygiene. We also found that identifying a champion on each shift helped facilitate staff engagement.
Future plans
This campaign has proven effective at helping to improve healthcare worker hand hygiene compliance on our neuroscience stepdown unit. Nursing leadership has initiated plans to expand the game to additional units.
Anna Southerland is a nurse manager of operations at Duke University Hospital in Durham, North Carolina. Staci Reynolds is an assistant professor at Duke University School of Nursing and an infection prevention clinical nurse specialist at Duke University Hospital.
References
Abdulmajed H, Park YS, Tekian A. Assessment of educational games for health professions: A systematic review of trends and outcomes. Med Teach. 2015;37(Suppl 1):S27-32.
Akl EA, Kairouz VF, Sackett KM, et al. Educational games for health professionals. Cochrane Database Syst Rev. 2013;3:CD006411.
Burke CT. The influences of teaching strategies and reinforcement techniques on health care workers’ learning and retention [PhD thesis]. Hattiesburg: University of Southern Mississippi, 2001.
Chan WV, Pearson TA, Bennett GC, et al. ACC/AHA special report: Clinical practice guideline implementation strategies: A summary of systematic reviews by the NHLBI implementation science work group: A report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. J Am Coll Cardiol. 2017;69(8):1076-92.
Gujral H. Survey shows importance of hand washing for infection prevention. Am Nurse Today. 2015;10(10):20. myamericannurse.com/survey-shows-importance-hand-washing-infection-prevention
Koo E, McNamara S, Lansing B, et al. Making infection prevention education interactive can enhance knowledge and improve outcomes: Results from the Targeted Infection Prevention (TIP) Study. Am J Infect Control. 2016;44(11):1241-6.
Read M, Chandler K. Boosting the success of a hand-hygiene campaign. Am Nurse Today. 2015;11-12. myamericannurse.com/wp-content/uploads/2015/10/ant11-Essence-Supplement-1027-Hand.pdf
Telner D, Bujas-Bobanovic M, Chan D, et al. Game-based versus traditional case-based learning: Comparing effectiveness in stroke continuing medical education. Can Fam Physician. 2010;56(9):e345-51.
World Health Organization. Evidence for hand hygiene guidelines. who.int/gpsc/tools/faqs/evidence_hand_hygiene/en





















1 Comment.
Hand washing is the best practice in preventing care-related infections. It is a fundamental procedure to limit the transmission of microorganisms in the care environment. Organizations must seek strategies to increase adherence and fairness to this good practice.
Piero Pantaleo – RN, Oncology Clinical and Palliative Care Nurse