Professional identity and role clarity are essential components.
Takeaways:
- Professional role clarity is integral to successful interprofessional collaborative practice.
- Role-based collaborative practice by all stakeholders deepens and broadens the knowledge for decision making related to patient care.
- Nurse executive knowledge about the clinical enterprise, the business, and operations is key to advancing an interprofessional collaborative practice approach.
The pandemic has tested the strengths and weaknesses of the nation’s healthcare delivery system. It pushed both human and material resources to the brink and magnified the necessity for all team members to work together. It forced us to scrutinize our clinical and management practices, question their efficacy, and innovate in real time. In other words, the pandemic gave us no other alternative than to collaborate, while amplifying the value of a unified approach.
Interprofessional practice (IPP) serves as just such a unifying approach. It’s defined as a collaborative practice where healthcare providers work inter- and intraprofessionally as well as with patients and their families. Collaborative practice within an interprofessional framework embodies communication and decision-making, which allows separate and shared knowledge and skills of diverse providers to synergistically influence care. Interprofessional practice is a way “to be,” not a thing “to do.” Why, then, is it not used more widely?
Nurse executives need to understand the answer to that question, as well as concepts essential for successful IPP, such as shared professional identity and role-based collaboration, so they are better positioned to implement IPP in their organizations.
IPP barriers and facilitators
Interprofessional practice has had its share of hurdles. They occur at the organizational level, where reimbursement structures for different professions determine which services get reimbursed; at the team level, where traditional professional hierarchies interplay; and at the individual level, where a lack of trust in the collaborative process exists. These hurdles lead many to say that IPP is too difficult, upsetting, conflict-inducing, and time-consuming. However real these issues are, they mustn’t stand in the way of collaborative IPP.
A misunderstanding about IPP exits—it’s seen as optional, rather than as a professional obligation. IPP success requires clarity about the values and obligations of the professional role, which transcend the specific discipline. It requires each team member to understand and appreciate their unique role contributions and the roles of others. Role clarity guides how each member contributes and interacts within and among interprofessional teams. This is an important step given professional education and experience variations. Role clarity fosters an environment vital for open and transparent dialogue and decision-making based on best evidence and experience from multiple sources. This approach diminishes territorialism among team members and boosts the potential for cultural transformation.
Shared professional identity
Interprofessional practice success requires that members of each profession have a shared role identity. The professional role represents a commitment to a basic set of agreed-upon obligations and longstanding principles that all professions must uphold. They include autonomous, self-directed decision-making; a science-based body of knowledge; standards of practice and a code of ethics that justify autonomous decision-making; and a commitment to serve the public. In this way, members of different professions share an important bond.
The Model of the Professional Role helps individual team members visualize role obligations and depicts how they interrelate. The four professional roles—leader/decision-maker, scientist, practitioner, transferor of knowledge—function interrelatedly and dynamically. You can’t have one without the others. The model shows the integration and alignment of the basic rules of a profession that lead to a role-, science-, standards-, and ethics-driven practice and highlights a common identity grounded in shared professional role obligations. (See Model of the professional role.)
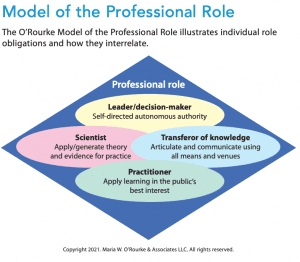

All professions have self-directed authority and autonomous decision-making practice (leader/decision-maker), base their practice on science and evidence (scientist), transfer knowledge to advance the practice (transferor of knowledge), and ensure core discipline-specific knowledge and safeguard those they serve (practitioner). Each profession must internalize these role components, recognize them as a common denominator of all professions, and use them as the basis of their unique professional focus. (See Knowledge transfer.)


Professional practice model
If IPP involves engaging with others by understanding their role and unique contribution, then it follows that you must understand and articulate your own role. A professional practice model (PPM) can help professionals with role clarity by providing the structures and processes that ensure the privileges and obligations granted to a profession are upheld and operational. In essence, a PPM links professional role clarity and practice excellence to quality care.
Professional obligations aren’t theoretical. When practiced, they benefit the patient. They apply to all nurses, irrespective of their position in an organization. A PPM provides the framework for aligning professional role obligations, scopes of practice, standards, and ethics. It also serves as a vehicle for achieving American Nurses Credentialing Center Magnet® recognition. Embedding a PPM into an organization depends on facilitating collaboration and aligning with organizational goals.
Role-based collaboration
Collaboration, an essential feature of IPP, isn’t new to nurses. Historically, nurses have always engaged in interdisciplinary collaboration and worked toward shared goals related to patient care. Working with pharmaceutical, medical, and social work professionals helps broaden and deepen nurses’ practice knowledge base.
Within the interprofessional team, clinicians address patient care issues while managers run systems and operational interference so team members’ knowledge and skills can be used to their fullest. IPP allows for the inclusion of other voices with a stake in patient care and expands the conversation to include knowledge and expertise beyond the clinical arena. The stage is then set for valuing professional practice, strengthening relationships, supporting collaboration, and sharing knowledge among all stakeholders.
Ultimately, it’s in a collaborative framework where clinical knowledge and practice from different disciplines, in conjunction with management knowledge and practice, converge to achieve common goals essential to a functioning organization. Interprofessional teams can address multifaceted issues as members come together to address department and systemwide concerns. For example, COVID-19 vaccination requirements and mask policies directly and indirectly impact clinical care, management, education, finance, equity, and diversity. The knowledge and experience of each team member can meet challenges and develop solutions from a dynamic system-wide approach that includes all voices.
Goal alignment
Exemplary professional practice successfully integrates a PPM and the care delivery system. To strengthen this connection, initiatives to improve practice must align with operational initiatives. This approach aligns with the principle that a link exists between raising the standard of care (level and type) and meeting the standard of practice (competence and skill).
This principle can be upheld by investing in the systems and processes essential to maintain the nursing standard of practice, which promotes an IPP collaborative approach. For instance, bedside rounding is key to the transfer of knowledge about a patient’s condition and the related plan of care. The dialogue’s structure includes an explicit reference to the use of the standard of practice that guides the nurse’s performance—talking through the decision-making and nursing process (“I intend to meet with the physical therapist to collect additional data to update my patient assessment and review the revised plan to ensure we’re in alignment with the patient’s goals.”)
This standards-driven approach helps team members appreciate the thinking process behind actions, and it deepens the dialogue about how to improve or stabilize the patient’s physical, social, and psychological condition. Placing standards at the front of the dialogue requires that team members discuss their own standards of practice so they’re met. In nursing, a PPM provides the structure and processes to support interprofessional thinking and decision-making as well as the full engagement of all stakeholders.
Nurse executive role
Nurse executives are critical to establishing a PPM and articulating its value across the organization. Their clinical, business, and operations understanding provides a broad cohesive knowledge base. When shared, this knowledge helps everyone understand that clinical practice is at the heart of the business. The nurse executive role is key to system and process enhancements that improve business and practice initiatives. When nurse executives share their expertise and contribute to finding solutions that result in quality care and practice excellence across provider roles, they have far-reaching impact beyond nursing.
Successful nurse executives must practice authentic leadership that builds trust and fosters transparency within the team. This kind of essential leadership strategically tackles issues with team members who engage in interprofessional collaborative practice. Using this approach, we can identify and address multisystem facilitators and barriers to create sustainable solutions. However, the efforts of the nurse executive alone can’t attain sustainable solutions. It takes a practice approach that includes the clinical professionals as well as finance, operations, information technology, and other stakeholders who share their expertise within an interprofessional collaborative practice.
Make it an obligation
Linking IPP to the professional role obligation of knowledge transfer makes it required, not optional. IPP entails the challenge of changing our behaviors. Team members must make more than a promise to collaborate, partner, and cooperate; they must demonstrate it with their behavior. In this way, role relationships and clarity, built on professional values and obligations, converge to become a driving force behind the work of the team, which in turn enhances team performance and ultimately patient care.
Maria W. O’Rourke is president and chief executive officer at Maria W. O’Rourke & Associates, LLC, in Larkspur, California.
References
Bonnice B. A nursing leadership challenge: Making the integration of professional practice standards into nursing operations a reality. Nurse Lead. 2019;17(3):207-14. doi:10.1016/j.mnl.2019.03.003
Buckland R. Medical student volunteering during COVID-19: Lessons for future interprofessional practice. J Interprof Care. 2020;34(5):679-81. doi:10.1080/13561820.2020.1822790
Goldman J, Xyrichis A. Interprofessional working during the COVID-19 pandemic: Sociological insights. J Interprof Care. 2020;34(5):580-2. doi:10.1080/13561820.2020.1806220
Green BN, Johnson CD. Interprofessional collaboration in research, education, and clinical practice: Working together for a better future. J. Chiropr Educ. 2015;29(1):1-10. doi:10.7899/JCE-14-36
Landstrom GL. Interprofessional practice: Just a trend or worthy investment? Nurse Lead. 2019;17(3):220-4. doi:10.1016/j.mnl.2019.03.004
Luzinski C. Exemplary professional practice: The core of a Magnet® organization. J Nurs Adm. 2012;42(2):72-3. doi:10.1097/NNA.obo13e3318243352a
O’Rourke MW. Rebuilding a professional practice model: The return of role-based practice accountability. Nurs Adm Q. 2003;27(2):95-105. doi:10.1097/00006216-200304000-00003
Reeves S, Xyrichis A, Zwarenstein M. Teamwork, collaboration, coordination, and networking: Why we need to distinguish between different types of interprofessional practice. J Interprof Care. 2018;321(1):1-3. doi:10.1080/13561820.2017.1400150
Shirey MR, White-Williams C, Hites L. Integration of authentic leadership lens for building high performing interprofessional collaborative practice teams. Nurs Adm Q. 2019;43(2):101-12. doi:10.1097/NAQ.0000000000000339
UCLA Health. Professional practice model. uclahealth.org/nursing/professional-practice-model
Key words: Professional role clarity, Interprofessional practice, Professional role identity formation, Professional practice model



















