Success depends on collaborating with your orientation team and speaking up when you need help.
Before you started your new job, your employer gave you a snapshot of what your average day might look like, how preceptorship works, and some of the unit challenges. What you may not fully understand is that orientation can be stressful, and that you’ll have a lot to learn in a limited time. So, be prepared. Your orientation success depends on collaborating with your onboarding team, asking questions, and speaking up for yourself.
Information overload
During the first few weeks of orientation, you’ll receive mountains of information. It will come from human resources and leadership. And it will come during general nursing orientation in lectures on policies, procedures, skills, and standards of care. Then you’ll be hit with your unit-specific education where you’ll be exposed to a new environment, coworkers, preceptors, guide-lines, and culture. (See Preceptor match.)
Preceptor match
Before your start date, your educator and nurse manager will match you with a preceptor based on several factors. Ideally, they will choose among nurses who have:
- completed a preceptor workshop
- expressed interest in preceptorship
- demonstrated unit-required skill competency.
The educator and nurse manager will then talk with these nurses to determine how they currently feel about precepting. Any who are overwhelmed in their current nursing duties or have a scheduling conflict won’t make a good match.
In some cases, the educator and nurse manager will try to match nurses with similar backgrounds. For example, a former emergency department (ED) nurse who’s now an experienced postanesthesia care unit (PACU) nurse will onboard a nurse who’s transitioning from the ED to the PACU. The preceptor will have in-sight into the challenges of this transition and can help the new nurse navigate them.
All of this information can be challenging and confusing, whether you’re a novice or an experienced nurse. Novice nurses may feel insecure and lack confidence; experienced nurses may be un-settled by new policies and procedures. Don’t assume that if you’re an experienced nurse that your transition to a new organization will be easy. Prepare yourself to be thrown off balance as you learn new ways of performing familiar tasks.
Addressing concerns
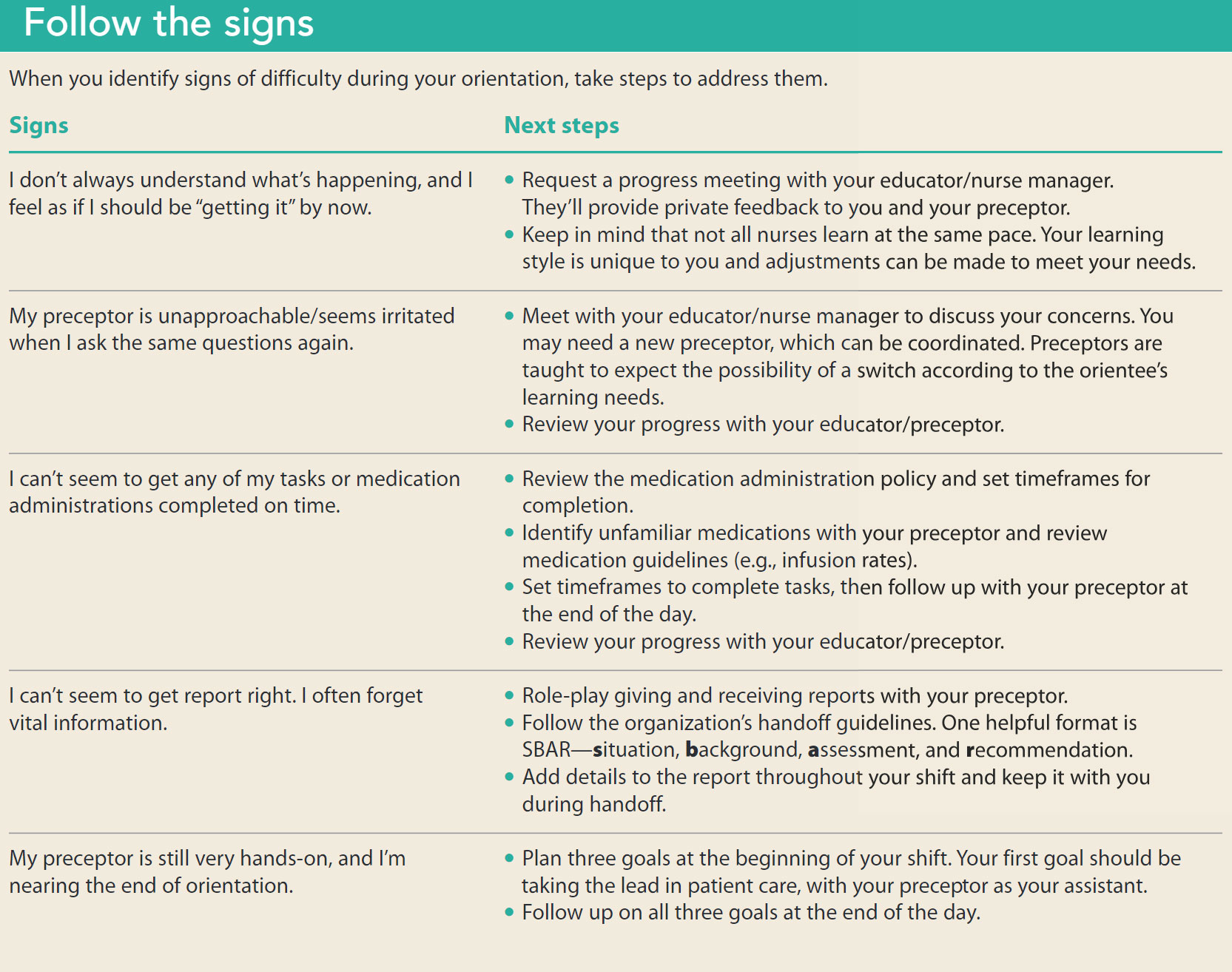
Over the course of your orientation, you’ll be expected to meet medication safety, assessment, and demonstrated skills objectives. You may struggle to connect all the dots, or you may find that you can’t recollect information your preceptor has told you several times. Does this mean that you aren’t progressing? Or are you overwhelmed? (See Follow the signs.)

Some new graduates experience so much anxiety and stress during their transition into a professional role that they leave the profession. You can take steps to navigate the stress and reduce your anxiety.
As you progress through orientation, you’ll meet privately with your educator, preceptor, and unit nurse manager. These meetings, which should be supportive and collaborative, are great opportunities to discuss your performance and review your experience, assignments, and concerns. Don’t be afraid to speak up if something isn’t working. Maybe you and your preceptor aren’t a good match. The only way to solve that problem and ensure that you’re having the best learning experience is to communicate with the appropriate nurse leaders so they can help you.
What happens if I don’t “pass” orientation?
Your team of preceptors, educators, and nurse managers will explore alternatives to ensure your success. You might need to switch preceptors, ex-tend your orientation, or explore units more applicable to your learning style and competence.
What can I do to improve?
At the beginning of each shift, your preceptor will share the plan of the day. He or she also will ask how you think you’re doing. This is a great opportunity to get immediate feedback during each shift, share your thoughts, and plan goals for the next shift. In between, research what you learned, ask questions, and be open to feedback.
A note for preceptors
If you’ve signed up to be a preceptor, review orientation dates with your educator and nurse manager and let them know about any conflicts be-fore agreeing to take on an orientee. Generally, two preceptors—a primary and secondary—are ideal for a well-rounded experience. The secondary preceptor fills in when the primary preceptor isn’t available. Good communication between the two preceptors can go a long way toward meeting the orientee’s learning needs. (See Preceptor tips for orientation success.)


Team support
Collaboration with the nursing professional development team, preceptors, and the nurse manager is instrumental to facilitating your unique learning experience as you begin your new role. When challenges are detected early and the orientation plan is reassessed and adjusted, this team can help you meet your competencies while encouraging and supporting you
Michelle Perregrini is a nurse educator at New York–Presbyterian Hospital/ Weill Cornell Medical Center in New York City.
Selected References
Hezaveh MS, Rafii F, Seyedfatemi N. Novice nurses’ experiences of unpreparedness at the beginning of the work. Glob J Health Sci. 2013;6(1):215-22.
Sparacino LL. Faculty’s role in assisting new graduate nurses’ adjustment to practice. SAGE Open Nursing. 2016. journals.sagepub.com/doi/full/10.1177/2377960816635182
ant4-CareerWatch-325



















