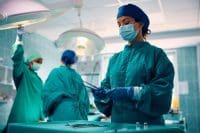
Four approaches can help promote effective communication and positive outcomes.
Takeaways:
- Authority gradients occur when individuals perceive differences in status that make them feel uncomfortable.
- When nurses don’t speak up, negative consequences can.
- Four approaches for strategically speaking up include: communicate in a positive, judgement free-way; close the loop; persist, especially when you perceive risk; and act local, aim systemic.
The healthcare system operates with several organizational, hierarchical, and authority-based structures necessary for patient care and other activities. However, these structures also can negatively impact patient, professional, and organizational outcomes. In particular, authority gradients, or perceived differences in status, can cause various communication breakdowns in direct and indirect care. For example, medication errors have occurred when professionals had concerns they didn’t feel comfortable expressing to a superior. These negative outcomes can be avoided when healthcare professionals, including frontline nurses, learn strategies for speaking up that help them navigate authority gradients and ultimately improve outcomes.
Authority gradients
Several factors influence the ability to speak up in the presence of authority gradients. A different discipline (physician, pharmacist) or a specific professional may intimidate a nurse and prevent them from speaking up. However, authority gradients based on experience, expertise, and levels also exist within disciplines. In nursing, for example, staff nurses, charge nurses, and nurse managers have different levels of authority. Staff nurses also may have official level differences (for example, staff nurse I, II, III) or they may have informal levels related to experience. Prior experiences with an individual or others with the same authority, personal characteristics, fear of retribution or of damaging a relationship, interpersonal dynamics, and others who can overhear also impact the ability to speak up.
The decision to say something is complex, dynamic, and situation-dependent. However, speaking up strategically and successfully navigating authority gradients can help diminish negative healthcare outcomes. (See Authority gradients: Negative outcomes.)


Navigation strategies
Four approaches to speaking up (positive, judgment-free communication; closing the loop; persistence; and acting locally for systemic change) can help nurses navigate authority gradients. These efforts promote safety cultures and positive outcomes. (See Speaking up.)
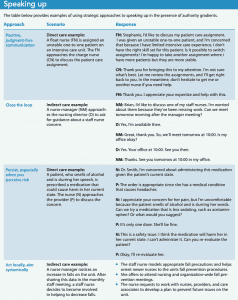

Positive, judgment-free communication
Just one conversation can enhance many patient and organizational outcomes, but negative, judgmental communication is unlikely to achieve its intended results. When you communicate concerns without making accusations, authority figures are more likely to remain open to your recommendations. However, if you approach a team member inappropriately, you risk offending them and they may not listen to your concerns. Conveying concern without judgment can include sharing information, introducing questions, and providing options or solutions.
Start by addressing the recipient of your message by their preferred name (informal first name or formal title). If you don’t know the person’s preferred name, respectfully ask.
Next, state your concern based on current observations or behaviors. Don’t dwell on past observations or assign any judgment; state the facts. The healthcare setting is fast-paced and stressful, so communicate respect by making a judgment-free observation, followed by an expression of concern.
After stating your concern, propose a different action or plan. Communicate your proposal carefully. Ensure the recipient also has an opportunity to offer their opinion and expertise, and encourage them to ask questions and provide feedback. If necessary, frame your concern as a personal learning opportunity. For example, if the recipient of your message has a history of struggling with feedback, it may be helpful to say: “Dr. Smith, I noticed that you didn’t complete the time-out checklist before the procedure. Can you help me understand why you didn’t complete it?” You also can explicitly state that you’re not questioning the recipient’s authority, and acknowledge their expertise and role.
When taking these steps, stay calm and use a positive tone of voice, even if you’re frustrated. In addition, show positivity and interest through body language to help ensure judgment-free communication. For example, make eye contact, nod your head, smile, and lean toward the receiver. Don’t cross your arms, roll your eyes, or frown. If possible, hold discussions in private when the receiver isn’t busy.
Close the loop
Communication in healthcare frequently is ambiguous, with messages hinted at rather than explicitly stated and understood. To combat this challenge, use closed-loop communication, which involves repeating a message back to the sender, who then confirms the message was received and interpreted correctly. Ideally, confirmation by the sender should be unambiguous and include an actual word or phrase, such as “yes” or “that’s correct.”
In closed-loop communications, it’s appropriate for either party to respectfully ask for clarification about the encounter. This skill takes practice, so rehearse it with your colleagues, family members, and friends.
Persist, especially when you perceive risk
Most healthcare professionals bring up issues only when they’re certain their concerns are justified. However, many concerns won’t be received and acted on appropriately. That means you must persist, especially when you perceive risk. In other words, escalate concerns when needed. To escalate concerns respectfully, follow the two-challenge rule: Voice your concern more than once by calmly restating the facts and focusing on direct observations or by obtaining an objective second opinion from another provider, manager, charge nurse, or staff nurse. The two-challenge rule emphasizes the importance of the concern and helps ensure messages are received. If needed, you also can CUSS in a firm, yet supportive manner: State that you’re Concerned, Uncomfortable, or that your concern represents a Safety issue and the line needs to be Stopped (immediate pause in activities).
Remain calm while implementing these approaches. As needed, escalate concerns using your facility’s chain of command.
Act locally, aim systemically
As you work locally on your unit or department to enhance care and improve the work environment, aim systemically when navigating authority gradients. To act locally, start with yourself and your immediate environment (your home unit).
Without even realizing it, you may be an authority figure and your behaviors influence those with or without authority. Model appropriate behavior. For example, thank others directly for raising concerns; encourage questions, explanations, and curiosity; show sensitivity to the potential impact your authority has on others; provide a personal narrative to demonstrate your own vulnerabilities; and operate with a team mentality.
In addition, your participation in unit-based committees and holding others accountable (using internal reporting systems, completing performance evaluations) can influence the facility’s safety culture. If possible, participate in interprofessional collaboration, including with individuals who have more (and less) authority than you. While you gain comfort at the local level, you also can participate in system-wide collaborations. Participating in shared governance structures and the decision-making process can help you learn to speak up appropriately.
Make an impact
Authority gradients comprise an unavoidable part of healthcare. To navigate them successfully, nurses must speak up strategically and promote safety cultures to make a positive impact on healthcare outcomes.
Hope Hubbard is an instructor at Watts College of Nursing in Durham, North Carolina. Jennifer Chicca is the senior manager at the National League for Nursing Commission for Nursing Education Accreditation in Washington, DC, and a part-time faculty member at the University of North Carolina Wilmington.
References
Clapper TC. TeamSTEPPS® is an effective tool to level the hierarchy in healthcare communication by empowering all stakeholders. J Commun Healthcare. 2018; 11(4):241-4. doi: 10.1080/17538068.2018.1561806
Patterson K, Grenny J, McMillan M, Switzler A. Crucial Conversations: Tools for Talking When Stakes Are High. 2nd ed. New York City, NY: McGraw-Hill Education; 2011.
Schwappach D, Richard A. Speak up–related climate and its association with healthcare workers’ speaking up and withholding voice behaviours: A cross-sectional survey in Switzerland. BMJ Qual Saf. 2018;27(10):827-35. doi:10.1136/bmjqs-2017-007388
Siewert B. Building a new culture of safety: Providing employees with the right environment and skills. HealthManage. 2017;17(5):388-90.
Siewert B, Swedeen S, Brook OR, Eisenberg RL, Hochman M. Barriers to safety event reporting in an academic radiology department: Authority gradients and other human factors. Radiol. 2018;288(3):693-8. doi:10.1148/radiol.2018171625