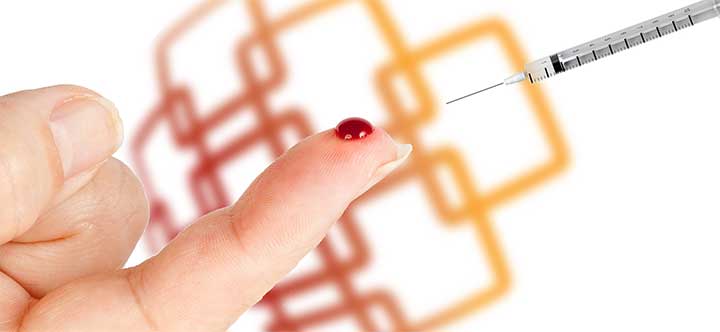
Near the end of a 12-hour shift in the emergency department, I left the triage area to help a colleague having trouble drawing blood from a patient. It was a moment that changed my life.
Seconds later, my gloved index finger was bleeding. I had sustained a deep puncture wound from a needle protruding from an overfilled sharps disposal box. That was 1998. By early 1999, I learned that I had contracted HIV and hepatitis C. The incident signaled the beginning of the end of my 26-year career as a front-line nurse and, for some time, transformed me from caregiver to patient.
Primary line of defense
Despite, or more likely because of, this profound crisis, I found a will and a way to channel my energy. I became an advocate for protecting healthcare workers from preventable needlestick injuries. By putting a face to the issue and telling my story to professional colleagues, nursing leaders, and lawmakers, I played an active role in getting legislation passed in many states, including Massachusetts, where I was president of the state nurses association. In partnership with the American Nurses Association, I became one of many people advocating a national reform that resulted in the passage of the national Needlestick Safety and Prevention Act (NSPA) in November 2000.
Although safety devices are now recognized as a primary line of defense and despite the NSPA-imposed mandate that employers provide safety devices, needlesticks and other types of preventable sharps injuries continue to be a major problem. In part, that’s because some employers fail to meet their legal obligation. And in part, it’s because nurses who work for these employers don’t take action.
Individual nurses must safeguard their own health and safety. Prevention starts with proper training and use of safety devices, but nurses also must understand the differences among the safety products available. I encourage you to seize the opportunity provided by the federal legislation to participate in evaluating and selecting safety devices in your own practice settings.
Below is an overview of the three major product categories and some simple criteria for evaluating devices.
Retro-fitted devices
Retro-fitted safety devices were developed as a quick fix to help institutions comply with legislation. Manufacturers adapted conventional sharps devices with add-on pieces, often with little or no input from clinicians. Today, these devices account for about 95% of all safety devices.
Retro-fitted devices have typically been designed by adding a shield, cap, or sheath to a conventional sharps device or the needle itself. Many nurses find the retro-fitted add-on pieces cumbersome and complain that they interfere with the ability to safely activate the safety mechanism. To activate the safety mechanism, the user often has to place a hand in close proximity to the used needle to move the sheath forward or place a cap over the sharp. This design has the potential to expose the clinician to the very hazard that the product was created to prevent.
Admittedly, retro-fitted devices are an improvement over sharps devices with no safety features. They provide added protection and, when activated correctly and permanently engaged, they do reduce exposures. But I’ve heard anecdotes about retro-fitted devices on which the safety feature has been removed, is not activated, or doesn’t stay activated, thus exposing the needle.
Of the three product types, retro-fitted devices are the most difficult to operate. But they are popular because they allow institutions to comply with the law at a low cost. These devices cost about half as much as the more sophisticated automatically retractable devices.
Automatically retractable devices
Automatically retractable devices feature a built-in mechanism to permanently disable the needle after use. Currently, these devices are available with syringes that operate in a manner similar to a ballpoint pen. The operator depresses the plunger, and when the injection is completed, the needle automatically retracts into the barrel, rendering it safe. The device is simple to use, and the mechanism is passive; that is, the clinician doesn’t take any action to activate the safety feature.
As with any new device, training is needed. Improper use can result in medication and body fluids being aerosolized during the retraction process. Cost considerations often prevent institutions from purchasing automatically retractable devices, despite their reputation for optimal safety. Another drawback is the fixed needle configuration that precludes needle changes.
Manually retractable devices
Manually retractable devices provide protection and performance advantages over retro-fitted devices and cost about the same. They also allow needle changes. The first devices were designed for angiocaths and winged steel needles. The safety feature is integral to the design; there are no add-on pieces or obstructing parts. These devices are easy to use. They require minimal training and little or no change in manual technique.
A recent addition to this category includes manually retractable syringes that look and function like traditional syringes. These devices operate with a simple “push, pull, snap” method. With hand and fingers safely positioned behind the needle, the clinician administers the dose, pushing the plunger in and then pulling the plunger back. This causes the needle to retract into the barrel. The operator then snaps off the plunger, permanently disabling the device. Because the user controls the mechanism at all times, this design lowers the risk of aerosolization.
These devices are cost-effective: Not only is the price similar to that of retro-fitted devices, but accurate dosing control and reduced hazardous waste volume and disposal cost may result in savings.
Evaluating and selecting devices
The NSPA gives nurses the right to be involved in the evaluation and selection of the safety devices used in their institutions, but many nurses don’t know that they are entitled to participate. If you do participate, use a process that allows a comparison of products from each available design category: retro-fitted, automatically retractable, and manually retractable.
Also, establish evaluation criteria before the pilot testing process begins. Dr. June Fisher of the University of California, San Francisco, suggests remembering key criteria by using the acronym PEST (Passive, Easy, Simple, Throughout). A good device should:
• be passive (that is, require no action to activate the safety feature)
• be easy to use
• be simple
• remain activated throughout its use.
When all safety devices meet these criteria, preventable injuries will decline.
Taking care of yourself
As caregivers, nurses have an obligation to provide patient-centered care. But in the process, nurses often neglect their own needs. One thing I try to teach my students about health and safety practices is the importance of taking care of themselves first, so they can effectively care for their patients.
Almost 6 years after the enactment of legislation designed to address the needlestick problem, needlestick injuries continue, though at a lower rate. We must continue to make progress toward preventing these injuries. Complacency is simply not acceptable at any level in the healthcare system.
Nurses can and should play an active role in reducing these injuries by becoming involved in the evaluation and selection of safety devices in their practice setting. Your involvement can influence the device-selection process and improve the overall safety of your work environment.
Karen A. Daley, PhD(c), MPH, RN, FAAN, is currently a PhD candidate at Boston College and the immediate past president of the Massachusetts Center for Nursing.