Simple strategies can help with transition to practice.
Takeaways:
- Many nurses who graduated in 2020 and 2021 (in the midst of the pandemic) found themselves caring for acutely ill patients shortly after they entered practice.
- Workforce evidence collected through the Nurse Wellbeing at Risk survey indicates that the youngest nurses are experiencing more mental health and well-being challenges.
- Including resilience content into new graduate residency programs can help prevent the long-term consequences of untreated stress, anxiety, and depression among these nurses.
Kate* coordinates a new graduate residency program. For the past 2 years, she’s noticed that recent graduates in the program seem more anxious and fearful during their professional transition. She validated these observations when she conducted a focus group with new graduate nurse preceptors, who agreed with her assessment. Kate has decided to integrate content into the new program to help nurse residents build resiliency and manage their fears and anxiety more effectively.
Kate’s observations about new graduates’ increased stress and anxiety are well-founded. Graduates in 2020 and early 2021 transitioned into practice during a challenging time. The COVID-19 pandemic overwhelmed many health systems, and significant parts of residency programs were remote with less face-to-face support. Many of these new nurses hadn’t been in clinical settings for months before graduation, and when they transitioned to practice, they found themselves caring for acutely ill patients with COVID-19 and unpredictable trajectories. Not surprising, workforce evidence collected during the pandemic through the Nurse Wellbeing at Risk survey indicates that the youngest nurses (Generation Z born between 1997 and 2015) are experiencing more mental health and well-being challenges than older generations.
Even before the pandemic, data from the American Psychological Association indicate that the Generation Z cohort reported far lower baselines of excellent or very good mental health compared to previous generations. Data from the large sample participating in the Nurse Wellbeing at Risk survey indicate that Generation Z nurses were the most likely (57.3%) to report that COVID-19 negatively impacted their overall well-being. Gen Z also was the least likely (only 23.5%) to report effectively managing work-related stress and anxiety or to decompress after work (only 19.2% could).
Kate’s decision to build resilience content into the new graduate residency program is wise. As the National Academy of Medicine noted in their 2019 report on clinician burnout, nurses may resist seeking help when they’re stressed and fearful because of stigmatization. Kate is proactive in her efforts to build a more resilient nursing workforce. The fallout of untreated stress, anxiety, and depression among nurses has serious long-term consequences.
Why we become fearful and anxious
The reasons for our fear and anxiety aren’t always well understood and can have many root causes. Exposure to stressful events where we don’t feel physically or psychologically safe can be a trigger. Inherited traits also can be a factor. Fear and anxiety frequently occur together, but the terms aren’t interchangeable. Fear relates to a known or understood threat (real or imagined); anxiety arises from an unknown, unexpected, or poorly defined threat. During the pandemic, nurses are experiencing fears about personal safety and anxiety about the many unknowns.
The rising levels of fear and anxiety among younger populations have been linked to social media. In the highly acclaimed documentary, Social Dilemma, researchers reported correlations between lowered mental health among Generation Z and the widespread introduction of social media sites in the early 1990s. To boost self-esteem and feel a sense of belonging in their social circles, young people post content with the hope of receiving positive feedback. They search for validation on the internet, which serves as a replacement for the meaningful connections they might otherwise make in real life. When that fails to happen or when people feel left out, they may experience stress and anxiety. Knowing this, Kate will want to include content about social media’s impact as part of the discussion about resilience.
Strategies designed to promote resilience serve as an essential antidote to managing fear and anxiety. Martin E.P. Seligman, PhD, director of the Positive Psychology Center at the University of Pennsylvania, is an expert in this area and has worked with military personnel to build their resilience before entering combat. Resilience strategies are critical for young people. The philosopher Fredrick Nietzsche wisely noted that what doesn’t kill us makes us stronger. Survey findings indicate that Generation X and Baby Boomer nurses report higher well-being and resilience levels during the pandemic. Nurses in these generational cohorts have more life experience and have confronted more adversity than younger nurses. We know from resilience research that we anchor every new challenging experience against past experiences. We can draw energy from remembering how we overcame those challenges. Most Generation Z nurses have less experience with adversity, so helping them manage their fears and build resilience is crucial.
Taking charge of emotions
Learning to effectively manage emotions in high-stress nursing environments requires time, practice, and patience. Nurses who haven’t developed positive coping skills before entering a residency program may find this process even more challenging. However, developing those skills can help them manage fear and anxiety. The first step is acknowledging that fears and anxieties exist and investigating the cause. The key is recognizing feelings, understanding why they’re important, and acknowledging their effect. Knowing the causes of anxiety, worry, or stress puts these feelings into perspective.
One way to gain perspective is to think of two nesting circles, as described by Covey. The outer circle is an individual’s Circle of Concern and the internal circle is their Circle of Influence. (See Focus on influence.)
Focus on influence
These circles represent everything that may be important to a nurse or that causes them to worry. The Circle of Influence holds things that the nurse can either directly or indirectly influence. Within this circle, a change in thoughts or actions can improve the situation. When focusing on the Circle of Influence, nurses live in the present and envision a better future. The Circle of Concern is for everything out of the nurse’s control. They can’t control the weather, other people’s actions, the past, or death. When they focus on the Circle of Concern, the fear grows and tends to control thoughts and actions.
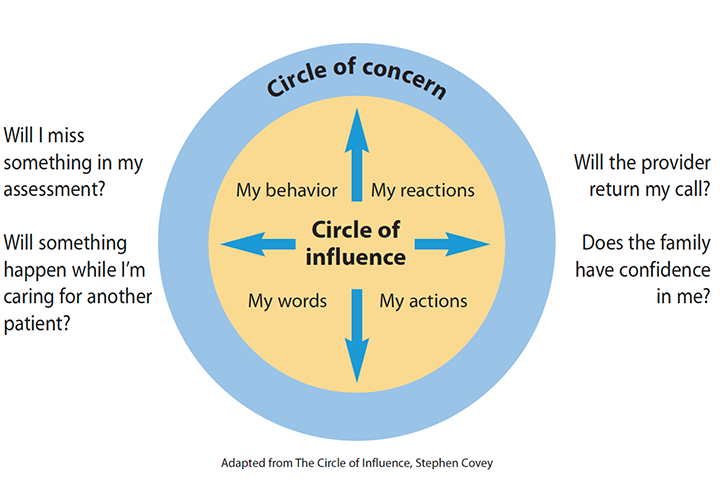

Many new nurses fear that a patient may die. They fear missing something or making a mistake. These fears are understandable. Patient acuity is trending higher, and many patients have more comorbidities. Healthcare staffing is limited, and timely communication with other disciplines can be challenging. These stressors contribute to fear.
To prevent fear from being the driving force of a nurse’s thoughts and actions, they should focus on their Circle of Influence. They can’t control how sick a patient is, but they can impact the patient’s current state by fulfilling orders, educating, and notifying the provider when the patient’s status changes. Nurses can’t make the provider call back, but they can keep calling and move up the chain of command until the patient’s needs are met. Nurses juggle multiple patients, but they can prioritize time based on patient acuity. Mistakes happen, especially among new nurses, but they can seek clarification, ask for help, and learn from their mistakes.
Fear and anxiety are natural human reactions to life’s challenges, but we can break the hold fear has on us and bring impactful changes to our situation by taking charge of our emotions.
Hardwiring resilience strategies
As an educator, Kate aims to guide new nurses through the transition from student nurse to safe, independent nurse. If new nurses don’t have hardwired resilience strategies, they can experience significant stress as they navigate challenging situations. Changes in the healthcare environment due to the pandemic may impact the effectiveness of Kate’s current program to reduce fear and anxiety. She knows she can’t control what others do or how they feel, but she can make changes and introduce strategies to help hardwire resilience.
Increase check-ins. Kate already holds scheduled check-ins, but the new residents’ increased fear and anxiety require her to be more involved, so she should increase check-in frequency. Building a relationship is the key to establishing trust. If Kate invests more time in quality conversations about residents’ struggles, including steps to overcome them, she can establish herself as a safe person they can turn to.
Normalize debriefing at work. When stressful events occur without an opportunity to process accompanying emotions, new nurses will feel more anxiety and fear. Their feelings begin to fester and can spin out of control. Kate should institute a debriefing protocol after certain high-stress events, such as the unexpected death of a patient. Even if the unit is busy, Kate can pull the involved staff aside for 5 or 10 minutes to assess their emotional state, discuss the event, and help staff process what occurred. Nurses need to know that they’re not alone and that what they feel is perfectly normal after being involved in or witnessing a stressful event.
Add a journaling requirement. Journaling can be an effective way for nurses to process what they experienced at work. It’s a simple but powerful tool for promoting thoughtful insight into lived experiences. Kate can provide a structure to journaling with questions such as:
- What went well?
- What didn’t go well?
- What did I feel when [scenario] occurred?
- What can I do differently next time?
- How did I get closer to my goals today?
- After looking back on my day, do I have questions about my patients, treatments, or interactions?
Add resilience workshops. Training days are standard in professional transition programs. They include a variety of lectures, simulations, and competency check-offs. Kate can modify one or two training days to include resilience workshops that teach how stress affects the body and address the prevalence of post-traumatic stress disorder and burnout symptoms among nurses. She should include case studies and exercises to help nurses understand their current stress levels and coping mechanisms, gain new techniques to manage stress better, and apply what they learned. In addition, Kate can include evidence-based resilience strategies such as connecting with friends, adequate sleep, healthy diet, exercise, and meditation.
Easing the distress
In designing and teaching resilience content in the new graduate transition program, Kate is taking future-focused steps to hardwire behaviors that reduce stress, anxiety, and fear. This type of nurse coaching always has been essential but perhaps now more than ever. If we fail to do this, we may lose some of our most highly skilled young nurses who decide that the mental health risks of being a nurse are just too high.
*Name is fictitious.
Access references at myamericannurse.com/?p=74156.
Rose O. Sherman is adjunct professor at the Marian K. Shaughnessy Nurse Leadership Academy, Case Western Reserve University in Cleveland, Ohio, and author of The Nuts and Bolts of Nursing Leadership: Your Toolkit for Success and The Nurse Leader Coach: Become the Boss No One Wants to Leave. You can read her blog at emergingrnleader.com. Alyse M. Labat is a clinical educator and the chief executive officer of Resilient Nursing. You can read her blog at resilientnursing.com.
References
American Psychological Association. Stress in America™: Generation Z. October 2018. apa.org/news/press/releases/stress/2018/stress-gen-z.pdf
Covey SR. The 7 Habits of Highly Effective People. New York City, NY: Simon & Schuster; 1989.
NurseGrid, Keener, HealthStream. Nurse Wellbeing at Risk. emergingrnleader.com/wp-content/uploads/2020/10/NurseWellbeingAtRisk-Final2020-web.pdf
National Academies of Sciences, Engineering, and Medicine. Taking action against clinician burnout: A systems approach to professional well-being. Washington, DC: The National Academies Press; 2019. doi:10.17226/25521
Seligman MEP. Building resilience. Harvard Business Review. April 2011. hbr.org/2011/04/building-resilience
Sherman RO. Keeping an eye on Generation Z nurses. Nurse Leader. December 3, 2020. ncbi.nlm.nih.gov/pmc/articles/PMC7713635/#bib3
The Social Dilemma. 2020. thesocialdilemma.com



















