We’ve entered the third year of a global pandemic combined with increasing staff shortages, and nurses continue to demonstrate their fortitude, compassion, and professionalism. This year’s All Pro Nursing Team Award submissions proved that point. Over 40 teams shared their stories, projects, successes, and plans for the future. We asked them to describe a successful project (including its impact on patient care or the work environment) and to explain how they’re incorporating lessons learned from the pandemic in anticipation of future crises. Projects ranged from COVID-19 testing and vaccination initiatives to unit reorganization to meet patient surges, clinical ladders to promote professional growth, and nurse wellness programs to enhance nurse physical and mental health.
What stood out among the winning teams was their ability to build on their important work in the midst of a global pandemic. Rather than narrowing their focus to the essentials (understandable given the circumstances), these teams innovated and created new processes and systems to support their colleagues, enhance care, improve outcomes, and advocate for patients.
The staff at American Nurse Journal salutes nurses around the world for their dedication to excellent patient care and compassion for their colleagues. Your work inspires us. Thank you to all the teams that took the time to submit their stories and congratulations to this year’s All Pro Nursing Team Award winners.
Julie Cullen is the managing editor of American Nurse Journal.
Winner
Mercy Medical Center Emergency Department
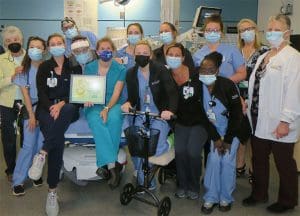

Increased recognition
The organization’s current ladder saw only three nurses advance, so the ED team created a ladder focused on emergency nursing skills (triage, competence in more than one patient population). After launching the new ladder in late summer of 2021, two nurses have been promoted and two more are working on their portfolios. “Even more exciting is that the nurses are working on projects and initiatives that mean something to them,” said Stumbroski.
Growth opportunities
Similar to most new graduate nurses around the country, those starting their first job in the Mercy ED had limited clinical experience because of the pandemic. With six new graduates starting in the ED in September 2021, the department created nine biweekly hands-on learning sessions related to various topics, including emergency airway management. “The new nurses loved these sessions,” said Stumbroski. “They felt like they had a safe place to ask questions and express concerns.” Each new graduate was paired with a primary and secondary preceptor. Weekly meetings provided opportunities to review achievements, goals for the next week, and areas for additional focus.
Improved working environment
ED staff identified additional supplies as their top need. Among the many issues resolved in meetings between nurses and leadership were additional Mobilab printers on the unit, computers on wheels, and a plan to remove nonfunctioning computers. Discussions with bio-med led to hiring an ED-specific equipment technician to troubleshoot issues and manage supply inventory.
Outcomes
Currently, the Mercy Medical Center ED has four nurses on the clinical ladder and two preparing to submit their portfolios. The department has only four vacancies, a waiting list of new graduates ready to join the team, and four nurse externs hired for summer 2022. All of the new graduates who started in 2021 have passed orientation and are moving toward growth opportunities. “Overall, the unit’s pulse is positive,” said Stumbroski. “Morale is much better. In fact, one nurse who went to agency nursing has already asked to return to Mercy.”
Stumbroski shared four lessons she and her team have learned during the pandemic that they can apply to future crises: have fun and spark joy, continue to grow and learn, teamwork makes the dream work, and this too shall pass. “We believe it’s essential not to lose sight of the mission and vision of the unit and organization,” explained Stumbroski. “Getting caught up in the negative aspects of a crisis brings down morale and leaves people feeling helpless. Having a focus, like ProjectED, helped minimize the focus primarily being on the pandemic.”
First Runner-Up
TriHealth Corporate Nursing Administration and Corporate Clinical Education


Helping Hands allowed nurses from non-bed roles to provide acute care support. The team created a sign-up process, assigned nurses as appropriate, provided tip sheets and orientation, and communicated incentives. A concierge component allowed non-nurses to serve as runners, staff temperature stations, and assist with other tasks that don’t require a nursing license.
Staffing Models allowed for an experienced nurse to oversee a team of nurses providing care for a group of patients. Nurses who had been away from direct care offered support by completing tasks such as bathing, turning, administering medications, and answering call lights. To reduce time in the classroom, provide social distancing, and fast track onboarding, the education team added virtual learning.
The team’s COVID-19 Information Sharing project included a series of animated educational videos to address nurses concerns about the COVID-19 vaccines. Before the videos were shared, only 38% of RNs responding to a survey said they would definitely receive a vaccine. After the videos, 87% of the system’s nurses opted to receive the COVID-19 vaccine. You can read more about this project here.
Second Runner-Up
Naval Medical Center Portsmouth Team America


The team’s senior nurse leaders provided daily site management and creative staffing models to increase vaccination capabilities by 75%. Team America’s Vaccination Preparation Team assimilated into the existing civilian workforce to help accurately prepare and track vaccines, which led to over 7,200 daily vaccines (an average rate of 700 doses per hour). Using an innovative electronic vaccine tracker, the team achieved real-time awareness of prepared vaccine doses, leading to zero wasted doses and maximum vaccine use.
Of particular note, this diverse team of 15 nurses had never worked together before. They came from different clinical specialties and had varying levels of nursing experience. Their adaptability allowed them to quickly become a team focused on the mission.
Third Runner-Up
Emory Healthcare PLAN Council


At the beginning of the pandemic, PLAN Council work was placed on hold, but the members asked to resume system-level meetings. The executive sponsor and council members recognized the value of their work and collaborated with senior nursing leadership for approval to continue supporting nurses. They resumed their work just 2 months after the pandemic began.
To address factors related to the pandemic, the council streamlined their processes to reduce the number of council members (while still maintaining representation) and the time needed to conduct business. Meetings became virtual and actually saved the Emory system $8,580 each month. Because of the council’s advocacy, 221 nurses advanced in the PLAN during 2020. And despite the stress associated with the pandemic, nursing engagement in the PLAN increased. In addition, the council updated the PLAN to give nurses more opportunities for professional development, advancement, and increased compensation.
Honorable Mention
Edward Hospital Pulmonary Medicine Unit


Maury Regional Medical Center Palliative Care Team


Duke University Hospital HBC Ambulatory Leadership Team


The Ohio State University Buckeye Wellness Innovators





















1 Comment.
Thanks for letting us know about the significant and inspiring role these teams are doing. Their actions, as well as the actions of many on the frontlines of care delivery are notable and admirable.