Build an infrastructure that supports competence and professional growth.
- Through shared governance, nurses are encouraged to participate in organizational decision-making to satisfy professional obligations.
- Incorporating ethical competence and professional development into everyday nursing practice is imperative to fulfilling ethical obligations for optimal patient care.
- A nursing ethics core council increases ethical sensitivity and knowledge and provides an opportunity to use ethics resources, engage in ethical decision-making, and take ethical action.
Ethics and crisis standards of care
Does a professional code of ethics matter?
Ethics for nurses in everyday practice
Learning Objectives
- Describe ways to increase nursing education and participation
in ethics education. - Discuss how to support nurses’ ethical competence on an individual level.
- Explain steps organizations can take to support nurses’ ethical competence.
The author, planners, and peer reviewers of this CNE activity have disclosed no relevant financial relationships with any commercial companies pertaining to this activity. See the last page of the article to learn how to earn CNE credit.
Expiration: 4/1/26
According to the American Nurses Association (ANA) Code of Ethics for Nurses with Interpretive Statements (the Code), “the nurse has authority, accountability, and responsibility for nursing practice; makes decisions; and takes actions consistent with the obligation to promote health and to provide optimal care.” The Code’s fifth provision describes a nurse’s duty to maintain competence and pursue professional growth, noting the difference between competence (a baseline foundation for acceptable practice) and professional growth (an ongoing process for moving beyond the minimum standard of practice). Provision 6 describes the nurse’s duty to act as a moral agent for creating ethical environments. In 2021, the ANA Center for Ethics and Human Rights released a position statement, “Nurses’ Professional Responsibility to Promote Ethical Practice Environments,” which directs nurses to “enhance their awareness of and sensitivity to the ethics content of challenges they face in their practice and take ownership of their own ethical competence to address these challenges.” (See Nursing ethics infrastructure.)
Nursing ethics infrastructure
No consensus exists on a definition for ethical competence, but Lechasseur and colleagues concluded that the concept has six fundamental components:
- Ethical sensitivity
- Ethical knowledge
- Ethical reflection
- Ethical decision-making
- Ethical action
- Ethical behavior
Koskinen and colleagues proposed a new model for interprofessional ethical competence, which includes the following three themes:
- Ethical attitude
- Ethical basis
- Ethical culture
They also offered the following three methods for promoting ethical competence:
- Leadership
- Reflection
- Time for talk
The Code of Ethics for Nurses with Interpretive Statements and nursing ethics literature indicate a need for support to help nurses fulfill their ethics obligations. Poikkeus and colleagues conducted a systematic review of existing literature to identify how nurse leaders and colleagues can best support nurses’ ethical competence at the individual and organizational levels.
Support at the individual level included the following:
- Education
- Participation in ethical decision-making
- Reading books and articles related to ethics
- Reflection
- Use of ethical codes
Support at the organizational level included the following:
- Clinical ethics committee meetings
- Collaboration and communication
- Professional guidelines and standards
- Supportive environments
- Training programs
- Written ethics policies and procedures
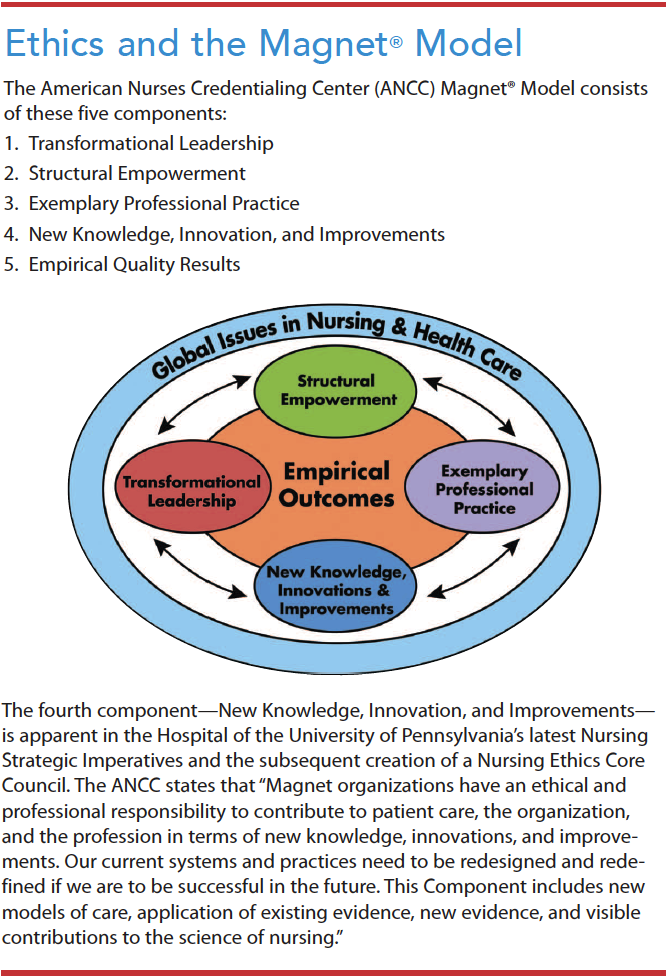
The Hospital of the University of Pennsylvania (HUP) has an active interprofessional ethics committee and ethics consultation service, but before 2019, its nursing shared governance lacked a formal ethics infrastructure. HUP’s shared governance structure incorporates key components of the American Nurses Credentialing Center (ANCC) Magnet Recognition Program®, which are reflected in HUP’s Nursing Strategic Imperatives: Priorities for the Future of Nursing (2019–2023). These imperatives support ethical competence among nursing staff.
A clinical nurse and a nurse leader collaborated to create the HUP Nursing Ethics Core Council (NECC) to increase nursing representation and participation in ethics education and deliberation and to support ethical competence using the existing shared governance infrastructure.
Shared governance
In the 1980s, O’Grady and Finnigan introduced the concept of shared governance by outlining a systematic infrastructure and model for the nursing profession. Nursing shared governance is founded on the premise that nursing professionals have accountability for decisions made within their role, particularly as they pertain to competence, education, quality, and practice. More recently, O’Grady and Clavelle suggested a focus on professional governance that emphasizes accountability, professional obligation, collateral relationships, and decision making, and where nurses take ownership of decisions and actions made within their organizations.
HUP’s bylaws describe shared governance as “the foundation for nurses at all levels to share in organizational decision making,” which enables nurses to align with HUP’s professional practice model—Care, Lead, Innovate. In 2018, existing hospital nurse leadership structures (including unit councils, evidence-based practice groups, core councils, nursing leadership committees, and the board of nursing) re-evaluated and revised the nursing strategic imperatives using the ANCC Magnet® Model and clinical staff feedback. Clinical staff, vital stakeholders, and members of the shared governance infrastructure provide influential input into institutional planning and decision making. (See Ethics and the Magnet® Model.)
Nursing strategic imperatives
HUP’s nursing strategic imperatives encompass investing in nursing, the patient and family experience, and teamwork. Each imperative has ethical underpinnings and coincides with an institutional need for advancing ethical knowledge, engaging patients and families to clarify values, and sharing best practices from multiple service lines and levels. In 2019, the NECC was established and embedded into HUP’s shared governance infrastructure. (See Strategic imperatives.)
Nursing ethics core council
HUP has an interprofessional hospital-wide ethics committee, as required by the 1992 Joint Commission on Accreditation of Healthcare Organizations standards, but few nurses participate. A nursing ethics special interest group (SIG) was created to increase the presence of a “moral space,” a concept described by Hamric and Wocial as an extension of institutional ethics with four requisite characteristics: individuals serving as ethics resources must be knowledgeable, known, available, and sanctioned. Other than the SIG, which offers a safe, moral space for staff to discuss ethical concerns, no formal nursing ethics infrastructure existed.
With support from the chief nurse executive and the board of nursing, the director of ethics conducted a current state assessment to determine ethics needs within the department of nursing. Through a series of focus groups with frontline nurse leaders and clinical nurses, the director of ethics identified a deficit in ethical competence. This finding mirrored internal survey data and observations during monthly SIG sessions. Nurses demonstrated a desire for more ethics education and a need to increase knowledge about the Code, foundational ethics principles, and strategies for managing complex patient situations. HUP created the NECC to address these gaps and integrated it into the current nursing shared governance model.
The NECC encourages the advancement of ethical and moral knowledge across practice areas. The council, guided by the nursing strategic imperatives, aligns with the Code and focuses on the delivery of safe, high-quality patient- and family-centered care in accordance with professional ethical standards. Its members work to promote and provide education that enhances ethical competence in nursing practice, which can lead to empowered, autonomous nurses and excellent patient outcomes.
Recruitment and council structure
NECC leadership sought diverse membership from different clinical experience levels, service lines, and backgrounds. Per HUP’s shared governance bylaws, all clinical nurses in good standing are eligible to serve as members of core councils, and membership is mutually agreed upon by the nurse, their direct supervisor, and specific council requirements. Core councils include a nurse executive, a nurse manager, a clinical nurse specialist/clinical practice leader (CNS/CPL), a chair, a chair-elect, and a diverse representation of nurses. Thirty clinical nurses applied to serve as members of the NECC inaugural cohort, and 14 were selected. Applicants submitted their resume and a personal statement explaining their interest in the council and their proposed contribution. A small group of nurse leaders, including the director of ethics, a clinical nurse, a nurse manager, two CNS/CPL representatives, and a nursing professional development specialist, reviewed and scored the applications and determined the council’s final makeup.
NECC members serve 2-year terms with an option to extend for 1 additional year. Members must attend at least 80% of council activities as required by shared governance bylaws, including monthly council meetings, monthly SIG sessions, and special ad hoc events and educational opportunities, such as grand rounds and guest lectures. Current NECC leadership consists of the director of ethics, the ethics manager, a nursing professional development specialist, a CNS/CPL representative, a chair, and a chair-elect. Core Council chairs sit on the board of nursing, and the chair mentors the chair-elect for 1 year before transitioning out of the roll. The NECC chair also sits on the hospital-wide, multidisciplinary ethics committee, which is chaired by the director of ethics.
NECC structure, goals, and outcomes
The NECC offers opportunities to invest in clinical nurses by providing ethics-focused education and programming, promoting patient- and family-centered care, and encouraging teamwork.
Investing in nursing
To advance knowledge and expertise, all new NECC members receive an education bundle that consists of foundational articles, a copy of Fowler’s Guide to the Code of Ethics for Nurses with Interpretive Statements, and a recommendation for free email subscriptions to Bioethics Today and The Hastings Center. By the end of their first year, council members must complete the EdX Introduction to Bioethics course, a Georgetown University online educational module that reviews foundational ethics concepts in healthcare. Leadership also encourages council members to pursue professional development opportunities, including attending the National Nursing Ethics Conference, an annual collaborative event focused on ethical discourse and networking within the nursing ethics community.
The nursing ethics SIG, a monthly discussion group for clinical nurses and others, features various experts and themes. The SIG provides a safe, moral space to discuss ethical concerns, develop knowledge and skills to address everyday ethical issues, and identify strategies to live the Code. The NECC sponsors the monthly series and coordinates speakers; sessions are open to everyone, regardless of discipline. In addition to speakers, the SIG functions as an open forum for nurse-led discussion of value-laden ethical issues. Past attendees have included clinical nurses, nurse leaders, nursing students, advance practice providers, and research coordinators.
Patient and family experience
To better connect and engage with patients, council members and other staff learn about the diverse patients, families, and communities they serve. For example, all inaugural NECC members participated in the Serious Illness Care Program. This 3-hour program, facilitated by the hospital’s palliative care service, provided communication tools to help nurses discuss patient goals and values directly with them and their families. Currently, the council is working on a person-first initiative. This evidence-based strategy aims to reduce stigma by using language that puts the person before a condition or behavior when talking about medical and mental health conditions. Council members offer individualized interventions (rounding in clinical areas, huddles, and demonstration of person-first language) based on practice area needs.
Ethics programming highlights diverse perspectives and patient populations and encourages moral curiosity about the lived experiences of patients and their families, including those in historically marginalized populations. For example, to encourage discussion about mental health, NECC partnered with the psychiatry department to host a hospital-wide book discussion of Sandy Allen’s book A Kind of Mirraculas Paradise: A True Story about Schizophrenia. The author recounts family memories and interactions with their uncle who has schizophrenia. The council also partnered with the University of Pennsylvania’s medical ethics and health policy department for a screening and discussion of the documentary 5B, which highlights the first AIDS ward at San Francisco General Hospital in the 1980s. The film features nursing’s impact on vulnerable and marginalized populations during a public health crisis. Post-screening discussion reviewed themes analogous to the COVID-19 pandemic.
The 2021 SIG, “The Henrietta Lacks Project,” used Rebecca Skloot’s book The Immortal Life of Henrietta Lacks to focus monthly discussions on themes of narrative ethics, patient advocacy, health equity, and ethical issues surrounding biospecimens. This series broadened members’ understanding of systemic racism and bias by highlighting Henrietta’s and the Lacks family’s troubling experiences with healthcare and research. The 2022 SIG programming focused on the overarching theme “Good Ethics Starts with Good Facts,” which draws attention to the nurse’s ethical obligation as a source of information for patients, families, and interprofessional colleagues. All educational offerings address the human experience, whether in personal or professional contexts and from various perspectives.
Teamwork
With the goal of optimizing consistency, sharing and disseminating best practices, and driving outcomes, NECC offers opportunities to engage with staff of different disciplines, clinical experience, practice areas, and backgrounds. The SIG invites noncouncil members from all service lines and disciplines to participate in monthly sessions. The 2022 SIG series conceptualized healthcare professionals as conduits of information who must work collaboratively to evaluate the quality of information and communicate clearly with each other and patients. Sessions featured experts and thought leaders who spoke about responding to health-related misinformation and disinformation, resisting simple answers, and managing a misinformed patient.
In addition to traditional education methods, NECC leadership developed an Ethics Case Study Series (ECSS) to review real clinical cases and elicit perspectives from different practice areas so everyone could reflect on the current state and review best practices. Council members consider cases from their own practice, meet with the director of ethics and ethics manager to review the chosen case, and present the case study to the council. Together, Core Council members and leadership work through complex clinical cases to identify the following: a patient’s clinical course; a detailed telling of the core ethics questions; a description of relevant stakeholders and their respective values and perspectives; relevant ethics literature, including institutional policies, professional guidelines, ethical principles, and best practices; reflection and resolution; and discussion questions.
All ECSS participants have the opportunity to review complex cases and share best practices. Outcomes of this series are measured using the Perceived Ethical Confidence Scale, a four-item Likert scale survey that assesses confidence in four areas: identifying conflicting values, knowing role expectations, feeling prepared to resolve ethical conflict, and feeling able to do the right thing. Participants take the survey before and after the session to gauge effectiveness. Pre- and post-session data show that nurses had the highest confidence in identifying conflicting values, which increased over time during the ethics case study series. Scores didn’t decrease in any of the four areas of perceived ethical confidence.
NECC fosters psychological safety and encourages the cohort to share and discuss their experiences openly. Council members appreciate the opportunity to openly reflect with their peers on challenging cases and interactions with patients, families, and colleagues. Now—perhaps more than ever given a global pandemic, focus on racial injustice, and multifactorial distress—a space for intimate discussion and collegial connection serves a critical role. NECC provides a valuable platform for transforming nursing strategic imperatives into action. Council activities and outcomes represent institutional priorities of investing in nursing, the patient and family experience, and teamwork. They’re an essential addition to shared governance infrastructure.
Take action
HUP’s NECC serves as a model for other institutions interested in creating formal infrastructure to increase and support nursing ethical competence. NECC leadership regularly evaluates council activities and integrates feedback into future programming. Consider the following strategies to incorporate nursing ethics into your shared governance model:
- Seek executive and nurse leader support using data to demonstrate the need for increased ethics education.
- Embed an ethics group into an existing shared governance structure.
- Recruit a diverse council to maximize impact and involvement across the institution.
- Create a curriculum based on the Code and other established ethics resources.
A nursing ethics core council provides a place to increase ethical sensitivity and knowledge through thoughtful discussion of myriad ethical issues. From seemingly small, everyday decisions to supporting patients and families through times of crisis and change, a nursing shared governance council prepares clinical nurses to implement ethics resources, engage in ethical decision-making, and take ethical action.
The authors work at the Hospital of the University of Pennsylvania in Philadelphia. Erin Marturano is the ethics manager and Aliza Narva is the director of ethics.
American Nurse Journal. 2023; 18(4). Doi: 10.51256/ANJ042306
References
Allen S. A Kind of Mirraculas Paradise: A True Story About Schizophrenia. New York, NY: Scribner; 2018.
American Nurses Association. Nurses’ professional responsibility to promote ethical practice environments. 2021. nursingworld.org/~4ab6e6/globalassets/practiceandpolicy/nursing-excellence/ana-position-statements/nursing-practice/nurses-professional-responsibility-to-promote-ethical-practice-environments-2021-final.pdf
American Nurses Credentialing Center. Magnet Model – Creating a Magnet culture. nursingworld.org/organizational-programs/magnet/magnet-model
Center for Addiction Medicine and Policy. How to mitigate stigma. penncamp.org/education/mitigating-stigma/edX. Introduction to bioethics. edx.org/course/introduction-to-bioethics
Ethics of Caring. 9th National Nursing Ethics Conference. ethicsofcaring.org
Fowler MDM. Guide to the Code of Ethics for Nurses with Interpretive Statements: Development, Interpretation, and Application. 2nd ed. Silver Spring, MD: American Nurses Association; 2015.
Hamric AB, Wocial LD. Institutional ethics resources: Creating moral spaces. Hastings Cent Rep. 2016;46(S1):S22-7. doi:10.1002/hast.627
Iacobucci TA, Daly BJ, Lindell D, Griffin MQ. Professional values, self-esteem, and ethical confidence of baccalaureate nursing students. Nurs Ethics. 2013;20(4):479-90. doi:
10.1177/0969733012458608
Joint Commission on Accreditation of Healthcare Organizations. 1992 Accreditation Manual for Hospitals.
Koskinen C, Kaldestad K, Rossavik BD, Jensen AR, Bjerga G. Multi-professional ethical competence in healthcare – An ethical practice model. Nurs Ethics. 2022;29(4):1003-13. doi:10.1177/09697330211062986
Lechasseur K, Caux C, Dollé S, Legault A. Ethical competence: An integrative review. Nurs Ethics. 2018;25(6):694-706. doi:10.1177/0969733016667773
O’Grady TP, Clavelle JT. Transforming shared governance: Toward professional governance for nursing. J Nurs Adm. 2021;51(4):206-11. doi:10.1097/NNA.0000000000000999
O’Grady TP, Finnigan S. Shared Governance for Nursing: A Creative Approach to Professional Accountability. Rockville, MD: Aspen Systems Corp; 1984.
Penn Medicine. Serious illness care program. pennmedicine.org/departments-and-centers/department-of-medicine/divisions/program-in-palliative-care/education-and-training/serious-illness-care-program
Poikkeus T, Numminen O, Suhonen R, Leino-Kilpi H. A mixed-method systematic review: Support for ethical competence of nurses. J Adv Nurs. 2014;70(2):256-71. doi:10.1111/
jan.12213
Skloot R. The Immortal Life of Henrietta Lacks. New York, NY: Crown Publishing Group; 2011.
Key words: nursing ethics, shared governance, ethical competence