This organization’s infrastructure supports clinical inquiry.
Takeaways:
- Nursing has the responsibility to provide evidence-based practice that meets patient, family, and community expectations.
- New knowledge, innovations, and improvements in patient care, nursing practice, and the work environment are hallmarks of organizations that have received Magnet® recognition.
Organizations that have received American Nurses Credentialling Center (ANCC) Magnet Recognition® integrate evidence-based practice (EBP) and research into clinical and operational processes. Improvements in patient care, nursing practice, and the work environment are hallmarks of these organizations. ANCC states that “Magnet organizations have an ethical and professional responsibility to contribute to patient care, the organization, and the profession in terms of new knowledge, innovations, and improvements.” Part of meeting that responsibility means fostering inquiry among nurses.
At Penrose-St. Francis Healthcare Services (PSFHS), a non-profit 522-bed acute care facility in Colorado Springs, Colorado, we encourage clinical nurses not only to ask the questions to help us meet strategic nursing goals but also to answer them. PSFHS is part of Centura Health in Colorado and Western Kansas, the area’s largest hospital and healthcare network delivering advanced care to more than half a million people each year. PSFHS earned Magnet designation in 2014 and 2019 and is working toward its third designation.
Our journey to operationalize the Magnet new knowledge, innovations, and improvement component includes developing an infrastructure to support nursing and collaborative research with an EBP council led in partnership with our nurse scientist.
Developing an infrastructure
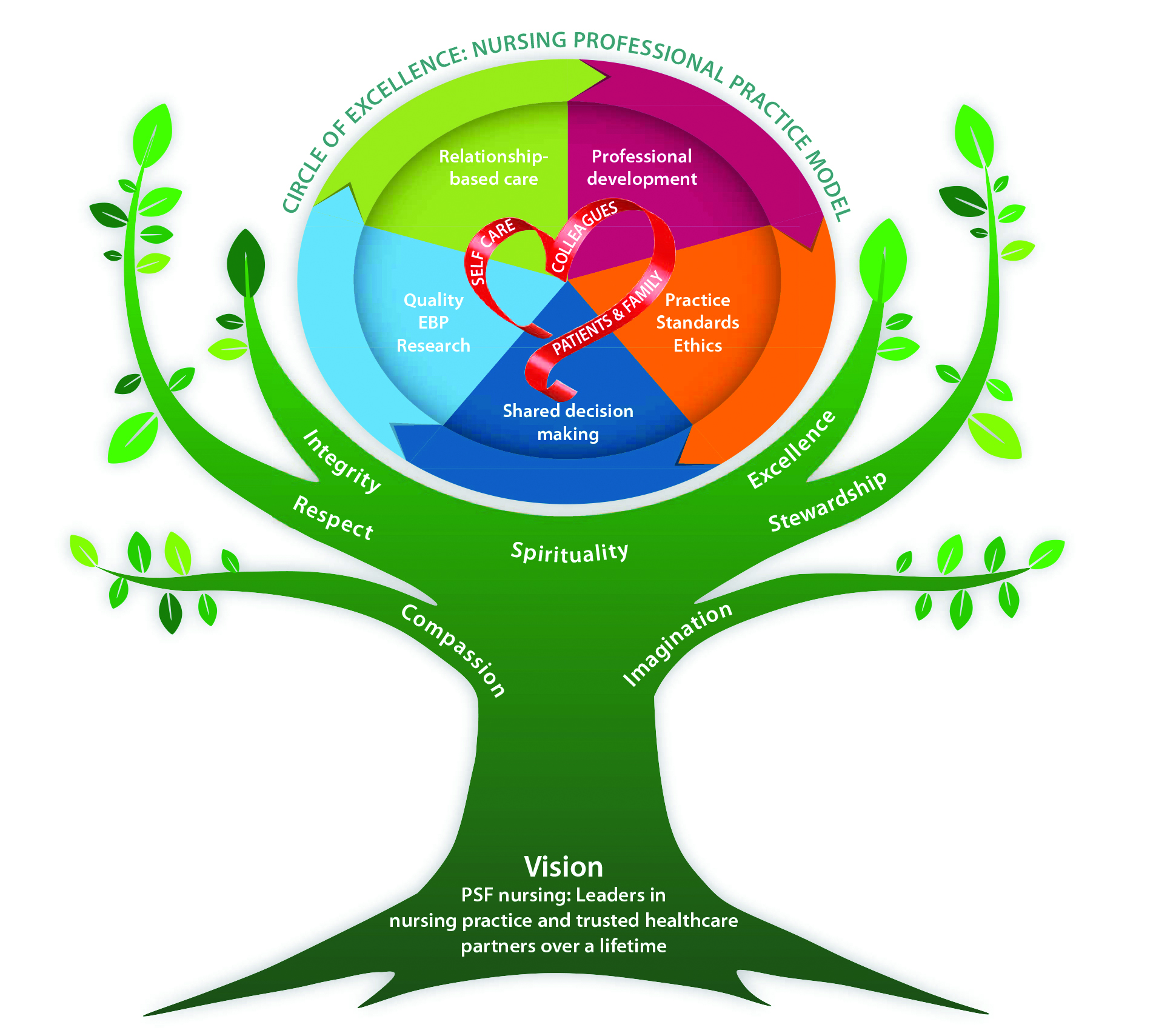
How does an organization bring an attitude of inquiry to the bedside nurse? At PSFHS, we developed a professional practice model (PPM) that symbolizes our beliefs, values, theories, and systems for nursing practice. (See Circle of excellence.) We’re grounded in our mission to “extend the healing ministry of Christ by caring for those who are ill and by nurturing the health of the people in our communities.” Our PPM provides a framework that describes the factors needed for nurses to ask questions about clinical practices they want to change. (See 4 components of clinical inquiry.)
Circle of excellence
The Penrose St. Francis Health Services nursing professional practice model is grounded in a circle of excellence.

4 components of clinical inquiry
At Penrose-St. Francis Healthcare Services, clinical inquiry consists of four components to improve health for patients, families, and communities.
- Research begins with a question and uses systematic, scientific inquiry to answer it. Research generates new knowledge and is integral to professional practice.
- Evidence-based practice uses the best scientific evidence, integrated with clinical experience and patient values and preferences, to ensure the best possible patient care.
- Process and quality improvement allows nurses to improve systems at the local level using Plan, Do, Check, Act to monitor performance and improve outcomes.
- Innovation involves applying creativity or problem-solving skills to adopt a new product or service to meet a need.
Many nurses are new to the research process, so having a nurse scientist on the council provides the guidance we need to understand research basics. The council also includes the chief nursing officer (CNO), who serves as the executive sponsor; clinical educators; advanced practice RNs; representatives from local nursing schools; the Magnet program coordinator; and clinical nurses. As the executive sponsor, the CNO demonstrates leadership support for research, EBP, quality improvement (QI), and innovation to drive patient outcomes improvement.
To advance nursing and interdisciplinary collaboration and to transform care, the council supports a culture of inquiry by connecting the dots so bedside nurses can fix a clinical practice problem using research, EBP, QI, and innovation. This is accomplished by providing an environment for sharing ideas; discussing lessons learned from participating in research, EBP, QI, or innovation; facilitating dissemination of findings; and providing continuing education programs (such as EBP boot camps and abstract writing seminars) to refine skills and new knowledge.
Relationships with nursing schools
Relationships with nursing school faculty and other disciplines, such as business and healthcare therapy faculty, maximize resources, enhance opportunities for staff to stay current in their practice, increase research productivity, and provide more opportunities for innovation. These relationships, led by the CNO, have allowed us to develop joint research programs that benefit faculty and nurse teams who work collaboratively. The schools develop research projects, and PSFHS staff have access to participate.
Current research projects include developing a post-cardiac event perceived risk assessment tool and studying resiliency of nurses caring for patients with COVID-19. We’re also working with the University of Hiroshima to examine the effects of exercise on cognitive status in breast cancer survivors. The outcomes of these relationships have increased grant funding and opportunities to co-sponsor research, which not only improves patient outcomes but provides research training for our future generation of nurses.
Integrating new graduates
PSFHS engages newly licensed RNs (NLRNs) during their residency program by identifying a clinical problem to solve in their units that will improve patient outcomes. The project aims to inspire lifelong learning and leadership skills by reinforcing that NLRNs can make a difference from the beginning of their careers. While working on a project, they develop decision-making and leadership skills and work collaboratively as a team to create strategies for incorporating research and evidence into their practice. After completing their residency program, the NLRNs present their project to their peer group and nursing leadership, and they submit abstracts to local and national conferences.
Here’s an example of a recent project: The NLRNs on an orthopedic surgical unit found that 41% of patients experienced constipation after discharge, so they developed an evidence-based constipation-prevention brochure. They provided education to other nurses and included the brochures in patient discharge packets. Their work resulted in nurses discussing constipation with patients at discharge. After the intervention, only 20% of discharged patients reported constipation in their follow-up phone calls.
Tying it all together
As a Magnet organization, we strive to integrate research, EBP, QI, and innovation into our clinical and operational processes and disseminate findings internally and externally (a requirement for Magnet-designated organizations). Annually, PSFHS participates in our system’s EBP, Research, and Innovation Conference, chaired by our nurse scientist. (See A forum for professional growth.)
A forum for professional growth
The Centura Health system Evidence-based Practice, Research, and Innovation Conference provides a forum for facilities and provider practices to present evidence-based practice, quality improvement, and research achievements. At the conference, nurses
- share data and receive peer feedback
- attend sessions that provide valuable information to replicate in their hospitals
- practice presentation skills and develop the expertise needed to discuss research
- learn how to answer audience questions
- establish contacts with other nurses, foster relationships, and potentially motivate each other to work across the hospital system to create environments that support clinical inquiry.
Presentations can then be submitted for consideration by professional organization conferences, such as the annual American Nurses Credentialing Center National Magnet Conference®.
In addition, PSFHS co-hosts and sponsors the annual Reaching for the Peak of Practice: EBP and Research Conference, presented in partnership with the nursing school, local hospitals from other health systems, and a local professional nursing organization. This conference provides another forum for nurses to explore introductory, intermediate, and advanced topics about implementing and integrating EBP, best practices, and other healthcare innovations that improve outcomes.
The journey continues
Nurses have a responsibility to engage in EBP that meets the expectations of patients, families, and communities. We have the privilege and expertise to advance the art and science of our profession. With so much required to keep nursing relevant, we tend to forget that an infrastructure exists to support EBP and keep our organizations from spinning their wheels every few months. Through inquiry, we help extend the science of nursing practice beyond intuition and ensure access to knowledge, both potential and realized, in the framework of caregiving.
Stacy Kreil is vice-president of nursing and assistant chief nursing officer at Penrose-St. Francis Health Services in Colorado Springs, Colorado.
References
American Nurses Credentialing Center. 2019 Magnet® Application Manual. Silver Spring, MD: American Nurses Association; 2017.
Ives Erickson J, Pappas S. The value of nursing research. J Nurs Adm. 2020;50(5):243-4. doi:10.1097/NNA.0000000000000876
Reed PG, Crawford Shearer NB. Nursing Knowledge and Theory Innovation: Advancing the Science of Practice. New York City, NY: Springer Publishing Company; 2017.


















