The nurse’s role at point of care
Takeaways:
- Short peripheral and midline catheters can be essential to accomplishing patient therapeutic regimens.
- Nurses must be competent to recognize signs and symptoms of peripheral vascular access device-related complications at any juncture in the life of the device and be prepared to intervene during insertion, management, and removal.
- All vascular access devices are subject to complications that may cause patient harm, impaired quality of life, and increased morbidity and mortality.
EDITOR’S NOTE: This article was developed in partnership with the Infusion Nurses Society (ins1.org), and the Infusion Therapy Standards of Practice, published in the Journal of Infusion Nursing (2016), were used as a guiding reference. Watch for an article on complications of central vascular access devices in our October issue.
PERIPHERAL vascular access device (VAD) use is widespread in inpatient and outpatient settings. Short peripheral catheters (SPCs), commonly called “I.V.s,” are the most widely used VADs worldwide. International data indicate that more than 1 billion SPCs are used annually in hospitalized patients. A resurgence in the use of midline catheters provides yet another option for peripheral venous access. In the United States, at least 85% of hospitalized patients receive some form of I.V. therapy. Although the use of peripheral VADs allows patients to receive I.V. therapy, which can be life-sustaining or even life-saving, the devices also present a challenge when managing associated complications.
Sequelae and complications
SPCs and midline catheters are two devices used to obtain peripheral venous access. SPCs are catheters less than 3″ (7.6 cm) long. Midlines are catheters inserted into the upper arm via the basilic, cephalic, or brachial vein, with the internal tip located level to or near the level of the axilla and distal to the shoulder.
The sequelae of peripheral VAD complications, including tissue injury, infection, emboli, and extravasations, can lead to impaired quality of life and increased morbidity and mortality. All peripheral venous access catheter types are subject to complications that can occur at any juncture in the life of the device.
Peripheral VAD-associated complications can be attributed to a number of patient-related risk factors, such as age, developmental stage, disease state, presence of immunosuppression or immunodeficiency, type of therapy and infusatn, prolonged hospitalization, and the presence of concurrent infections. Practice-related risk factors include multiple venipuncture attempts, poor insertion technique/traumatic insertion, inappropriate catheter size and length in relationship to the vessel, failure to adequately secure the catheter, inadequate maintenance, poor hand hygiene, and poor sterile technique.
Preventing and mitigating complications
Nurses play an important role at specific points of care in the life of peripheral VADs:
- insertion
- care, use, and maintenance
- discontinuation.
Ongoing assessment to detect complication onset and to initiate corrective action and therapeutic management when complications occur are essential at each point.
Insertion complications
Skillful insertion of a peripheral VAD ensures patient safety and proper device functioning. A poor insertion technique can place the patient at risk for insertion-related complications, including infection, tissue or vessel damage, therapy delay, and, rarely, catheter embolism. Failures or complications at the point of insertion also may require additional insertions, increasing the risk for infection and vessel depletion.
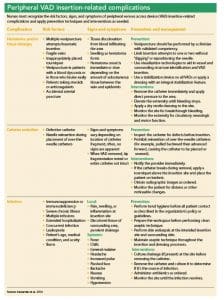
Insertion-related infection can result from inadequate handwashing, workspace preparation, or skin antisepsis before insertion and failing to maintain aseptic technique throughout the process. Vessel, nerve, and tissue damage can occur if the catheter isn’t adequately secured or if probing or multiple insertion attempts occur. Hematomas arise when an adjacent vessel is pierced or when the vein is penetrated through the vessel’s back wall. Catheter embolism can occur if the needle is reinserted into over-the needle catheters during cannulation, shearing or severing the catheter. In addition to patient injury, these failures add to the overall financial impact for the patient and the healthcare organization. (See Peripheral VAD insertion-related complications.)


Care, use, and maintenance complications
Detecting and preventing care-, use-, and maintenance-related SPC and midline catheter complications require nursing vigilance. Routine patient and peripheral VAD assessment is necessary to help ensure the patient doesn’t experience any of the many use-associated complications. However, extended SPC and midline catheter use and patient-related risk factors can increase the challenge of preventing complications such as catheter occlusion, infection, infiltration or extravasation, skin injury, and phlebitis.
Occlusion. Catheter occlusions typically are associated with central VADs, but SPCs and midline catheters also can be affected. Occlusions can increase the risk of catheter-related bloodstream infections (CR- BSI) and cause delays in the therapeutic regimen. All catheters must be flushed and locked appropriately to maintain patency and decrease the risk of CR-BSI.
Infection. Infection is a serious, potentially life-threatening peripheral VAD complication, and prevention is essential to patient safety. Peripheral VAD–related infections present as localized site infections or systemically as bacteremia or septicemia, which are considered catheter-related if the same microorganism is isolated both in the blood and on the catheter surface. CR-BSIs are frequently considered exclusive to central VAD use; however, patients with SPCs and mid-line catheters also are vulnerable.
Infiltration and extravasation. Infiltration is the inadvertent instillation of infusate into the tissues external to the vessel; extravasation is the inadvertent instillation of vesicant solution into the tissues external to the vessel. Infusates (infusions) are all parenteral solutions administered into the vascular system. Vesicants are defined as agents or infusions capable of causing tissue damage. Infiltration or extravasation can be caused by damage to the vein intima, fragile patient vasculature, catheter migration external to the vessel, or thrombus formation that causes vessel rupture or retrograde flow exiting through the catheter insertion site. Catheter malpositioning external to the vessel may occur during or after insertion.
Skin injury. Loss of skin integrity occurs for a variety of reasons, including patient age and disease state. Some patients are sensitive to skin-preparation agents or elements contained in dressing materials. Nurses should assess for allergies and must follow manufacturer instructions when using any products on the patient’s skin. To help prevent skin injury, special attention should be paid to the dry time required for antiseptic and site-preparation solutions, careful application of the transparent dressing by not stretching, and gentle dressing removal.
Phlebitis. Phlebitis is inflammation of the vein, which may be accompanied by pain, erythema, edema, streak formation, and/or palpable cord. It’s caused by endothelial cell inflammation of the vessel and is classified as chemical (chemicals in the infusate), mechanical (presence of the catheter within the vessel, catheter pistoning or movement, inadequate vein-to-catheter ratio, or traumatic insertion), or bacterial (presence of infection and inflammation affecting the vein wall). (See Peripheral VAD care, use, and maintenance complications.)




Discontinuation complications
Complications associated with peripheral VAD discontinuation include excessive bleeding, infection at the catheter insertion site after catheter removal, and, although rare, catheter embolism. Of these, infection and catheter embolism present the greatest risk for mortality or significant injury. Nurses and other healthcare personnel must be knowledgeable and diligent when discontinuing a VAD and never deviate from standards of practice.
Vigilant care
Peripheral VAD-associated complications pose serious risks for patients, the extent of which may result in prolonged illness, extended lengths of stay in a healthcare setting, permanent physical damage, or even death. Knowledgeable, highly skilled nurses are instrumental in mitigating and preventing peripheral VAD-associated complications. Vigilant assessment and intervention at the point of catheter insertion, throughout the duration of catheter use, and at catheter discontinuation help ensure the safe care patients deserve.
The authors work at the Infusion Nurses Society in Norwood, Massachusetts. Dawn Berndt is the clinical education and publications manager and Marlene Steinheiser is the director of clinical education.
Selected References
Alexander M, Corrigan A, Gorski LA, Phillips L, eds. Core Curriculum for Infusion Nursing. 4th ed. Philadelphia, PA: Lippincott Williams & Wilkins; 2014.
Alexandrou E, Ray‐Barruel G, Carr PJ, et al. International prevalence of the use of peripheral intravenous catheters. J Hosp Med. 2015;10(8):530-3.
Infusion Nurses Society. Infusion therapy standards of practice. J Infus Nurs. 2016;39(suppl 1):S1-S159.