Proper diagnosis and treatment can improve a patient’s quality of life
Takeaways:
- Approximately 16% to 18% of postmenopausal women develop urinary incontinence.
- Many women too embarrassed to discuss urinary incontinence with their healthcare providers, leading to isolation and depression when they limit their activities and social interactions.
- Providing a comfortable atmosphere will help patients open up about their symptoms.
By Christina Tso, DNP, FNP-BC, CRP, and Wah Lee, DO, MS

Some women experience vaginal dryness, vaginal atrophy, night sweats, and hot flashes. Others also may experience lower urinary tract dysfunction, specifically, urinary incontinence (UI). Defined as involuntary urine leakage, UI can present as stress UI (SUI), urgency UI (UUI), or mixed UI (MUI). Many menopause symptoms can become debilitating, affecting a woman’s quality of life, including her social life, psychological health, sense of well-being, and ability to function.
About 16% to 18% of postmenopausal women develop UI. Many are too embarrassed to discuss the condition with their healthcare providers and some believe it’s a normal part of aging that they have to live with. The result can be isolation and depression when they limit their activities and social interactions because of UI.
Nurses are key to ensuring patients receive the care they need.
A thorough knowledge of UI and its treatment options allows nurses to answer patients’ questions and make referrals as necessary. In addition, providing a comfortable atmosphere will help patients open up about their symptoms.
Types of UI
SUI is the most common type of UI. Caused by insufficient support of the urethra, it’s characterized by involuntary urine loss associated with coughing, sneezing, or physical activity.
UUI’s primary symptom is urine leakage accompanied by a strong desire to void. Myogenic and neurologic factors (including increased afferent activity, decreased inhibitory control in the central nervous system or peripheral ganglia, and increased sensitivity to efferent stimulation in the detrusor) may contribute to UUI (also called overactive bladder).
Many women have MUI, which includes urinary frequency, urgency, and stress incontinence. To determine which condition the patient has, urodynamic diagnostic testing combined with subjective and objective findings are reviewed. (See Diagnostic gold standard.)
Diagnostic gold standard


Etiology of UI
Menopause has been implicated in the etiology of many urogenital complaints, including dysuria, frequency, nocturia, and urgency. The epithelial tissues of the urethra, trigone, bladder, and vaginal walls contain estrogen and progesterone receptors. The reduction in estrogen that occurs as a result of menopause leads to thinning epithelium, weakening tissue, and decreasing blood flow and vaginal wall elasticity.
Thinning epithelium can cause reduced urethral closure, decreased bladder sensation, and recurrent urinary tract infection. Decreased blood flow and reduced vaginal wall elasticity can lead to dyspareunia (painful intercourse), a shortened vagina, and easily traumatized vaginal epithelium that may cause postmenopausal bleeding. In addition, loss of cellular glycogen and decreased lactic acid can alter vaginal pH, changing it from acidic (pH 4 to 5) to alkaline (pH 6 to 8), which increases the susceptibility to pathogens.
Other causes of UI in the postmenopausal population include pelvic organ (bladder, uterus, rectum, or small intestine) prolapse and hysterectomy or any other reproductive system surgery. Also, victims of rape may experience UI resulting from physical and psychological effects of the trauma.
UI treatment options
Treatment should begin with a voiding diary (also known as a bladder diary) to record a patient’s urination habits and activities. The diary should reflect:
- when and how much the patient urinates
- urinary leakage and what the patient was doing when it happened (for example, running, biking, laughing)
- sudden urges to urinate
- how often the patient wakes at night to use the bathroom
- type and volume of food and beverage intake
- any pain or problems experienced before, during, and after urinating (for example, sudden urges, difficulty urinating, dribbling urine, feeling as if the bladder is never empty, weak urine flow).
Management and treatment of UI includes products that make it possible for patients to participate comfortably in social activities as well as medication, behavior modification, surgery, and alternative therapies.
Protective products and devices
Incontinence underwear—disposable or washable and reusable—has a waterproof liner and built-in cloth pad to absorb large amounts of urine. Available in daytime and nighttime (designed to hold more urine) styles, the absorbent underwear protects skin from moisture and controls odor.
A product resembling a tampon is made of a wad of absorbent fibers and a collapsible silicone structure with a nonabsorbent polypropylene covering. It helps support the urethra to prevent accidental leaks but doesn’t inhibit urination and won’t move or fall out during bowel movements.
Mechanical devices such as pessaries support the urethra to prevent or reduce urinary leakage. Pessaries, which come in various sizes and can be used to support vaginal prolapse, are professionally fitted by trained healthcare providers. They should be removed, cleaned, and reinserted regularly to prevent infection. Some of the devices, such as ring pessaries, can be removed and reinserted by the patient. They are similar to a diaphragm and can be removed or left in place for sexual intercourse. Gellhorn pessaries, on the other hand, can’t be easily removed and they can’t be left in for intercourse. They require professional cleaning and reinsertion at least once every 3 months. If any pessary is left in place for too long, the patient may develop excessive discharge and pressure injuries.
Behavior modification
Behavior modification, such as developing a voiding schedule and avoiding bladder irritants (for example, caffeine, carbonated beverages, and spicy foods) are first-line UI treatments. Other recommendations include weight loss, managing fluid intake, and pelvic floor muscle training.
Pelvic floor muscle training strengthens support of the urethra, vagina, and rectum to reduce UI symptoms. It can be delivered with or without assistive devices such as weighted vaginal cones, biofeedback, or electrostimulation. Electrostimulation improves muscle tone and helps stimulate the sensation of the pelvic floor muscles to enhance muscle control. It also reduces the detrusor contraction in women with UUI, which also can be treated with sacral neuromodulation and external electrodes.
Estrogen
Because systemic estrogen, which is effective in treating vaginal atrophy, is no longer recommended, localized estrogen is suggested. Localized estrogen, available as a cream, intravaginal pill, and vaginal ring, has slow-release estradiol, which is associated with fewer adverse effects than systemic estrogen. However, it can cause endometrial stimulation, uterine bleeding, breast tenderness, and other negative effects. Treatment results in rapid symptom relief, with significant improvement after about 2 weeks; the full effect on vaginal atrophy takes up to 6 weeks.
Anticholinergic drugs and UUI
Anticholinergic drugs, the most commonly used drugs to treat UUI, target specific areas of the peripheral nervous system to block the action of acetylcholine. These drugs act on cholinergic receptors in the brain, secretory glands, heart, and smooth muscle (such as the bladder) by occupying receptor sites at parasympathetic nerve endings. In addition to providing an antispasmodic effect on smooth muscle to relieve symptoms, they also decrease urinary frequency and pain during urination associated with infections such as cystitis and urethritis. In addition, anticholinergic agents are given to increase bladder capacity in enuresis, paraplegia, or neurogenic bladder.
Contraindications for anticholinergic drugs include conditions with symptoms that might be aggravated by the drugs, including myasthenia gravis, hyperthyroidism, glaucoma, tachyarrhythmia, myocardial infarction, and heart failure unless bradycardia is present. The medications shouldn’t be given to women with hiatal hernia or other conditions that contribute to reflux esophagitis because they may delay gastric emptying, relax the cardioesophageal sphincter, and increase esophageal reflux.
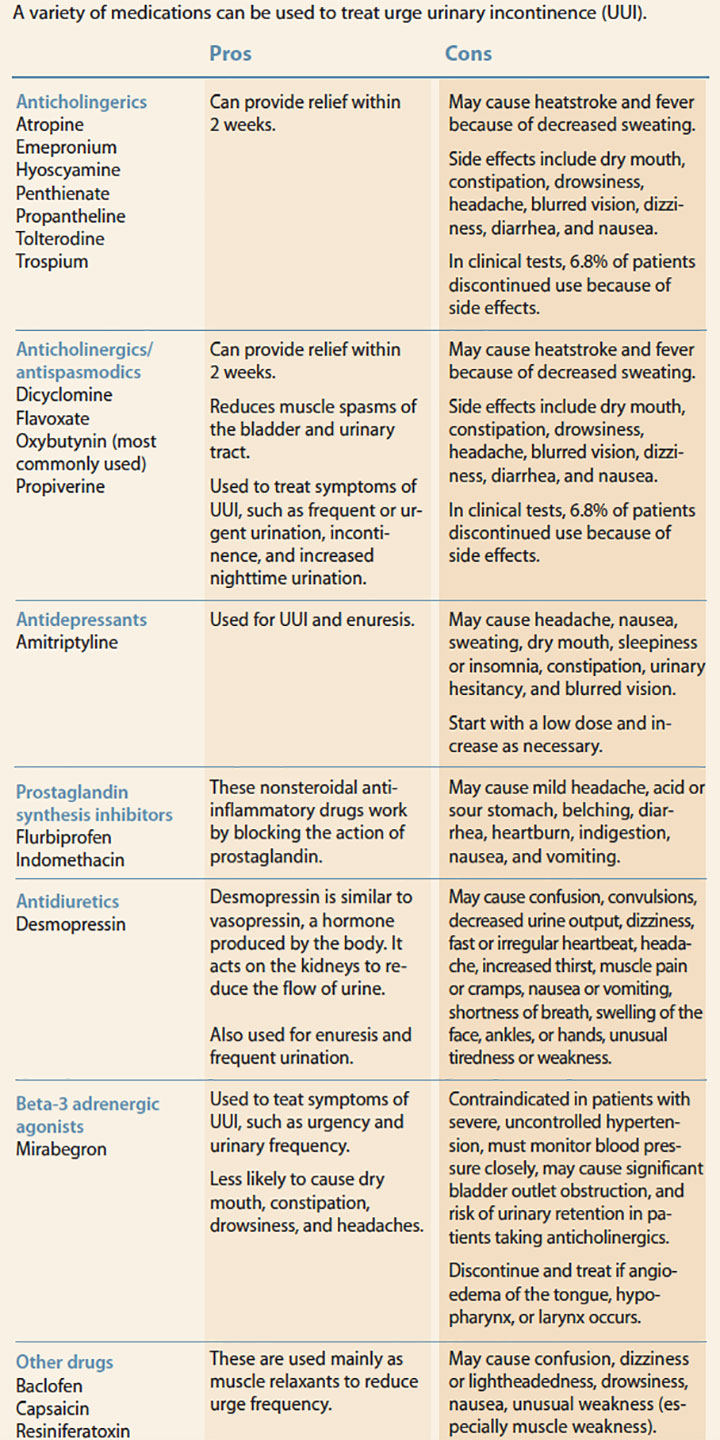
Other medications used to treat UUI include drugs with mixed actions, antidepressants, prostaglandin synthesis inhibitors, and antidiuretics. (See UUI medications.)
UUI medications

Surgical treatment—Sling procedures
Surgical approaches to lift and support the urethrovesical junction fall into two categories—sling procedures and bladder neck suspensions. Sling procedures (tension-free vaginal tape and transobturator tape) use a strip of synthetic mesh tape to create a sling placed under the urethra or bladder neck (the area of thickened muscle where the bladder connects to the urethra) to provide support and keep the urethra closed to prevent urine leakage under stress from actions such as coughing or sneezing. Sling procedures are mainly used to correct SUI, although they also may ease the symptoms of UUI.
No stitches are needed to attach a tension-free sling. Three small incisions are made to insert the sling—a 1-cm incision on either side of the lower abdomen and a 3-cm incision in the vagina to allow the sling to be placed. Body tissue holds the sling in place and eventually scar tissue forms in and around the sling to keep it from moving.
With the transobturator approach, a small incision is made in the vagina just under the urethra and two small openings are created, one in each groin. Narrow mesh carrier instruments are passed through each opening, and the mesh sling is then attached to each of the instruments. When the instruments are removed, the sling is pulled back through the incisions. After the sling is adjusted under the urethra, excess material is trimmed. Friction of the muscles and other tissues holds the sling in place. The incisions are sealed with skin glue or stiches and the vaginal incision is closed with absorbable stitches.
Recovery time varies, but the recommendation is 2 to 4 weeks before returning to normal activities, including heavy lifting or strenuous exercise, and 6 weeks before resuming sexual activity. Possible complications include erosion of the material, infection, and pain.
Alternative therapies
In addition to traditional treatment of UI, patients may wish to try alternative therapies.
- Acupuncture/electroacupuncture: This therapy involves inserting needles into specific points in the body that affect the nerves and muscles involved in bladder control.
- Hypnotherapy: A form of psychotherapy, hypnotherapy is used to create subconscious changes in the form of new responses, thoughts, attitudes, and behaviors. This access to the subconscious mind is thought to reestablish the connection between the bladder and the brain.
- Bowen technique: This hands-on therapy uses gentle pressure applied to specific points on the body with the goal of helping the body balance, repair, and reset itself.
- Reflexology: Reflexology massage targets reflex points on the feet, hands, and head used to relieve tension and treat illness. To treat UI, for example, the practitioner might massage the kidney point, which is the inner ankle bone between the two tendons that appear when the foot is flexed.
Nursing care
As a nurse, your approach to patients with UI can help them express their fears, worries, and embarrassment. Let patients know that they’re not alone and that UI isn’t something they have to live with. Provide education about protective products, pelvic floor muscle training exercises, behavior modification, and symptom management. And encourage them to learn more about their condition. (See Education—For you and your patients.)
Education-For you and your patients
| Visit these online resources to learn more about urinary incontinence (UI) and find patient education information. • National Institutes of Health. U.S. National Library of Medicine. You’ll find search results at this page for research about UI and its treatments. • Patient: Making Lives Better. In an article on urinary incontinence, you’ll find information about etiology, assessment, risk factors, and treatment. • Urology Care Foundation. This page includes downloadable patient education materials. • Urology Care Foundation. You can direct patients to this page so they can learn more about incontinence and treatment options. |
Reducing UI symptoms decreases stress and embarrassment, allowing patients to participate in family and social activities.
Christina Tso is a family nurse practitioner and clinical research professional at Northwell Health, formerly known as North Shore-LIJ Health System, and assistant professor of nursing for Hofstra Northwell School of Graduate Nursing and Physician Assistant Studies. Wah Lee, who is in private practice in New York, New York, holds board certification in physical medicine and rehabilitation and neuromusculoskeletal medicine.
Selected references
Brown ET, Krlin RM, Winters JC. Urodynamics: Examining the current role of UDS testing. What is the role of urodynamic testing in light of recent AUA urodynamics and overactive bladder guidelines and the VALUE study? Curr Urol Rep. 2013;14(5):403-8.
Culligan PJ. Nonsurgical management of pelvic organ prolapse. Obstet Gynecol. 2012;119(4):852-60.
Delancey JO, Ashton-Miller JA. Pathophysiology of adult urinary incontinence. Gastroenterology. 2004;126(suppl 1):S23-S32.
Lindahl SH. Reviewing the options for local estrogen treatment of vaginal atrophy. Int J Womens Health. 2014;6:307-12.
McClurg D, Pollock A, Campbell P, et al. Conservative interventions for urinary incontinence in women: An overview of Cochrane systematic reviews. September 1, 2016.
Patel M, Mellen C, O’Sullivan DM, LaSala CA. Impact of pessary use on prolapse symptoms, quality of life, and body image. Am J Obstet Gynecol. 2010;202(5):499.e1-4.
Stüpp L, Resende AP, Oliveira E, Castro RA, Girão MJ, Sartori MG. Pelvic floor muscle training for treatment of pelvic organ prolapse: An assessor-blinded randomized controlled trial. Int Urogynecol J. 2010;22(10):1233-9.
Waetjen LE, Feng WY, Ye J, et al. Factors associated with worsening and improving urinary incontinence across the menopausal transition. Obstet Gynecol. 2008;111(3):667-77.
Waetjen LE, Ye J, Feng WY, et al. Association between menopausal transition stages and developing urinary incontinence. Obstet Gynecol. 2009;114(5):989-98.
ant1-CE Urinary Incontinence-1214



















1 Comment.
My mother noticed that she’s suffering from incontinence because she’s starting to pee on the bed when she’s asleep. It’s interesting to know that menopause can cause this debilitating condition, so I might suggest her to go to a women’s specialist. I think that they may have some treatment options that she can get depending on what she has.