An intervention to enhance nurse leader engagement and coping ability
- Positive thinking skills training may present an innovative opportunity to combat stress and improve coping.
- Nurse leaders exposed to a positive thinking skills intervention experienced increased engagement, improved ability to cope with stress, and presumed improvement in quality of work life.
- Positive thinking skills training is a low-cost intervention and serves as a potentially valuable tool to help healthcare organizations support leaders, nurses, and ultimately patient care.
Most nurses report experiencing moderate-to-high levels of stress, which can lead to burnout and job dissatisfaction. However, stress experienced by unit nurse leaders reaches beyond themselves to affect the nurses they serve and potentially patient care. Addressing nurse leader stress could have significant impact on nurse leaders themselves and their organizations.
Positive thinking skills training may present an innovative opportunity to combat stress and improve coping. In 2013, Bekhet and Zauszniewski developed a scale to measure what they defined as positive thinking, “a cognitive process that creates hopeful images, develops optimistic ideas, finds favorable solutions to problems, makes affirmative decisions, and produces an overall bright outlook on life.” Although some people seem to have an innate ability to use positive thinking strategies, research by Bekhet and Mohammad-Najar and colleagues demonstrates that the skill of positive thinking can be taught.
The effectiveness of this training on nurse leaders hadn’t been previously examined, so we conducted a research study to determine whether positive thinking skills training would increase nurse leaders’ engagement and ability to cope with stress and whether improvements could be sustained.
What we did
We used a cross-over controlled design, and the organization’s Institutional Review Board reviewed and approved the study.
We invited unit nurse leaders (nurse managers, assistant nurse managers, and nurse educators) who had been in their positions for at least 6 months to participate in the study. Their positive thinking skills training bundle included a 1-hour in-person positive skills class, daily homework assignments to practice new skills for 1 month, and 28-days of affirmations delivered via text to their work phones. (See About the participants.)
The interactive positive skills class encouraged self-reflection and introduced the idea of engaging in purposeful positive thinking. The class began with exercises to engage participants and open their minds to positive events happening around them that they might not notice. The class instructors provided an overview of Bekhet and Zauszniewski’s eight positive thinking skills (Transforming, Highlighting, Interrupting, Noting, Knowing, Initiating, Nurturing, and Generating). After learning to identify and focus on the positive and the skills, the instructors presented the group with different scenarios they might encounter as nurse leaders and brainstormed possible positive responses. Finally, the participants were introduced to Achor’s five activities to promote happiness: practicing gratitude, journaling, exercise, meditation, and random acts of kindness. (See Think your way to positivity.)
To promote accountability and help hardwire the behavior change, we gave participants daily homework for the 4 weeks after the in-person class. The participants received a log for documenting which of Achor’s five activities they participated in each day. At the end of each week, the participants submitted their log. The homework encouraged participants to engage in the activities they learned in the class and to practice the skills and ultimately hardwire them into their daily habits.
Throughout the study, the research team sent positive affirmations to participants’ smartphones at random times throughout the workday. The goal was to provide unexpected reminders to refocus on the positive aspects of each day.
To gauge the effectiveness of the intervention bundle, participants completed the Positive Thinking Skills Scale (PTSS), the Brief Resilient Coping Scale, and a Workforce Engagement survey. The PTSS measures the frequency with which participants use positive thinking skills. Scores range from 0 to 24, with higher scores indicating more frequent use. The BRCS measures the ability to cope with stress. Total scores range from 4 to 20, with a higher score indicating better coping ability. The Total Engagement score measures workforce engagement. Total scores range from 6 to 30, with higher scores indicating more engagement. We administered the scales before the intervention and then after 1 month, 3 months, and 6 months.
What we learned
During the 4 weeks after the in-person class, participants documented daily activities to promote happiness. They practiced gratitude most frequently, followed by exercise, conscious acts of kindness, and meditation; journaling was the least commonly used activity.
The baseline PTSS score (M=14.68, SD=4.26) was significantly lower than the 1-month (M=19.58, SD=3.89, p<0.001), 3-month (M=19.08, SD=3.72, p<0.001), and 6-month post-intervention scores (M=19.08, SD=3.91, p<0.001). We found no significant difference in the PTSS scores between the 1-month, 3-month, and 6-month time points, demonstrating that the participants sustained their increased use of positive thinking skills for 6 months after the intervention.
The baseline engagement score (M=26.47, SD=3.30) was significantly lower than the 3-month post-intervention score (M=28.03, SD=2.76, p=0.003). We found no significant difference in the engagement scores between any other combination of time points.
The baseline coping score (M=15.83, SD=2.46) was significantly lower than the 1-month (M=17.69, SD=2.03, p<0.0001), 3-month (M=17.19, SD=1.86, p=0.003), and
6-month post-intervention coping scores (M=17.19, SD=2.11, p=0.001). We found no significant difference in participants’ ability to cope with stress between the 1-month, 3-month, and 6-month time points, demonstrating that participants sustained their increased coping ability at 6 months
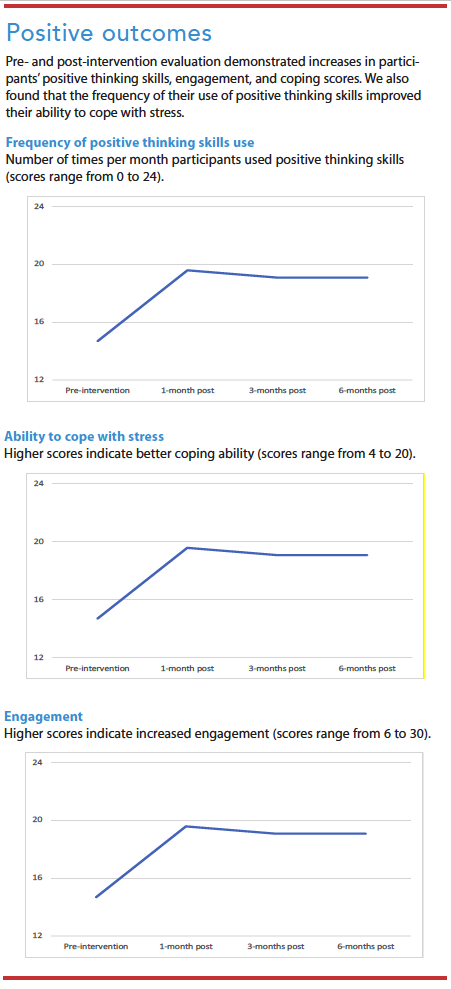
In addition to examining whether the ability to cope with stress differed at the four time points, we looked at the potential relationship between how frequently participants used positive thinking skills and their ability to cope with stress. As the frequency of practicing positive thinking skills increased, participants’ ability to cope with stress significantly increased (r=0.5212, p<0.00001). (See Positive outcomes.)
What the future holds
We believe this is the first study to examine the impact of person-centered interventions on improving nurse leaders’ engagement and ability to cope with stress.
The study showed promising results, but we encountered several limitations, including a relatively small sample size (54 participants). We invited all nurse leaders at the organization to participate, but several opted not to enroll, which introduced a potential self-selection bias. A larger sample size might have provided data more generalizable to the total nurse leader population. In addition, about 3 months into data collection, the COVID-19 pandemic began, drastically changing nurse leaders’ personal and work circumstances. Guiding teams through surges in workloads and patient acuity, and likely the pandemic itself, impacted participants’ levels of stress and engagement. Replicating the study without the influence of a global pandemic might provide different findings.
Future research beyond this study could examine whether nurse leaders’ improvement in engagement and ability to cope with stress has an impact on the direct care nurses they serve. Also, extending the intervention to direct care nurses and interprofessional healthcare teams might provide insight into whether it increases engagement and coping ability among populations outside of nursing leadership.
This study indicates that when nurses apply hands-on strategies to their daily lives and hardwire positive thinking into their daily routines, they exhibit more positive thinking, improved and sustained ability to cope with stress, and increased engagement. This low-cost intervention serves as a potentially valuable tool to help healthcare organizations support leaders, nurses, and ultimately patient care.
Amy Keller is a professional excellence specialist in nursing administration at TriHealth in Cincinnati, Ohio. Rachel B. Baker is a nurse researcher in nursing administration at TriHealth. Brandon Ballhaus is director of perioperative services at Good Samaritan Hospital in Cincinnati, Ohio. Sharon Brehm is senior director in nursing administration at TriHealth. Susan Hanselman (retired) was a project coordinator in nursing administration at TriHealth. Michele Huff is a manager of nursing quality in nursing administration at TriHealth.
American Nurse Journal. 2022; 17(12). Doi: 10.51256/ANJ122224
References
Achor, S. The Happiness Advantage: The Seven Principles of Positive Psychology that Fuel Success and Performance at Work. New York, NY: Broadway Books; 2010.
Bekhet AK. Online positive thinking training intervention for caregivers of individuals with ASD: Necessity, acceptability and feasibility. Issues Ment Health Nurs. 2017;38(5):443-8. doi:10.1080/01612840.2017.1279247.
Bekhet AK, Zauszniewski JA. Measuring use of positive thinking skills: Psychometric testing of a new scale. West J Nurs Res. 2013;35(8):1074-93. doi:10.1177/0193945913482191.
Mohammad-Najar N, Khoshnevis E, Banisi P. Effectiveness of positive thinking skills training on the hope and quality of life of drug-dependent people. Addict Health. 2017;9(3):120-8.
Munnangi S, Dupiton L, Boutin A, Angus LDG. Burnout, perceived stress, and job satisfaction among trauma nurses at a level I safety-net trauma center. J Trauma Nurs. 2018;25(1):4-13. doi:10.1097/JTN.0000000000000335
Sinclair VG, Wallston KA. The development and psychometric evaluation of the Brief Resilient Coping Scale. Assessment. 2004;11(1):94-101. doi:10.1177/1073191103258144
Tully S, Tao H. CE: Original Research: Work-related stress and positive thinking among acute care nurses: A cross-sectional survey. Am J Nurs. 2019;119(5):24-31. doi:10.1097/01.NAJ.0000557886.73585.d2
Key words:
positive thinking skills, nurse leaders, positivity, coping skills