Central line–associated bloodstream infections (CLABSIs) are among the most common hospital-acquired infections. Patients diagnosed and treated for CLABSIs require additional therapies and interventions, have longer stays, and face an increased risk of serious harm or death.
CLABSIs also raise healthcare costs. Over the past several years, most insurers have stopped reimbursing healthcare organizations for the increased costs of treating CLABSIs and certain other preventable conditions. Because nurses access and maintain these central lines, we’re in a key position to understand the risks of these infections—and we’re in a key position to prevent them.
Defining CLABSI
In 2001, the Centers for Disease Control and Prevention (CDC) defined CLABSI as a primary bloodstream infection in a patient with a central line in place during the 48 hours before infection, when no other infection source exists. The agency points out that some infection sources can be occult; therefore, CLABSI surveillance sometimes may overestimate the incidence of catheter-related bloodstream infections.
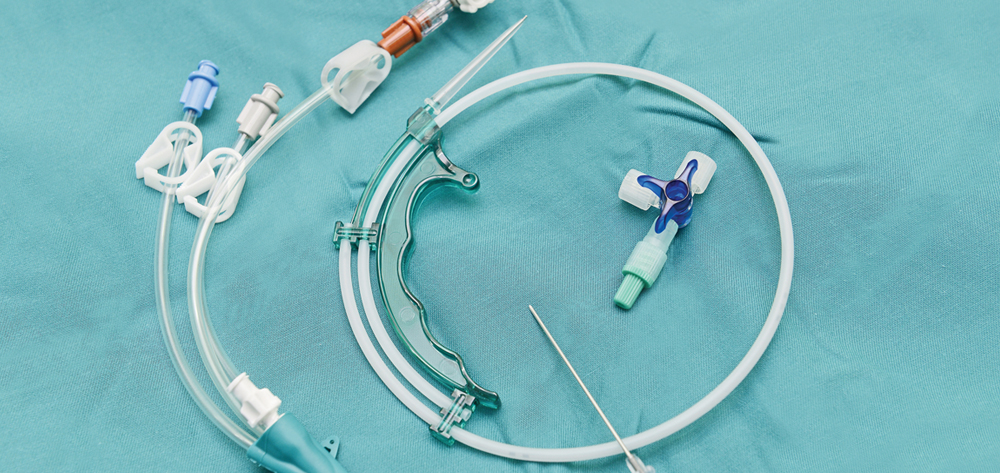
Understanding the types of vascular-access catheters available can increase your knowledge of CLABSI prevention strategies. (See Types of vascular-access catheters.)
Evidence-based guidelines for CLABSI reduction
Several national organizations regularly release evidence-based guidelines on CLABSI prevention, including the CDC, Infusion Nurses Society, and Society for Healthcare Epidemiology of America. This article summarizes the main recommendations in the CDC’s 2011 “Guidelines for the prevention of intravascular catheter-related infections.” These recommendations stress that healthcare organizations can achieve the greatest improvement when using multiple evidence-based strategies in a bundled approach. They also highlight the importance of collecting and reporting performance data on bundle elements to benchmark against other organizations and drive improvement.
- Train clinicians who insert and maintain catheters about the indications for catheters, proper insertion and maintenance procedures, and infection-control measures.
- Use the catheter with the fewest lumens necessary; infection risk increases with more access points.
- Perform hand hygiene and maintain aseptic technique before and after insertion and care of intravascular catheters.
- Use maximal sterile barrier precautions during catheter insertion, including a cap, mask, sterile gown, sterile gloves, and full-body sterile drape.
- Use a cap, mask, gloves, and a small sterile, fenestrated drape for peripheral arterial catheter insertion. Use maximal barrier precautions when inserting a catheter at the femoral or axillary site; these sites have higher infection risks.
- Disinfect the insertion site with greater than 0.5% chlorhexidine with alcohol prep before inserting a central venous catheter (CVC) or arterial catheter and during dressing changes. Allow the prep to dry completely before inserting the catheter or applying a new dressing.
- Use ultrasound-guided placement to reduce the number of insertion attempts and complications.
- Avoid routine catheter replacement to help prevent infection.
- Use a sterile transparent, semipermeable dressing for short-term CVCs, or a sterile gauze dressing if the site is bleeding or the patient is diaphoretic. Change gauze dressings every 2 days and transparent dressings every 7 days. With a tunneled catheter, change the transparent dressing once a week until the site heals. Change dressings as needed—for instance, when they’re loose, soiled, or damp.
- Report changes to the catheter-insertion site, including pain on palpation, redness, warmth, or purulent drainage.
- Use 2% chlorhexidine wash for daily skin cleaning.
- Use sutureless devices to secure catheters.
- Use antiseptic ointment at hemodialysis-catheter sites after insertion and after each dialysis session. Don’t use antiseptic ointment on other types of CVCs because it may promote fungal infections and antibiotic resistance.
- Replace continuous infusion tubing no more often than every 96 hours but at least every 7 days. Change blood-product or fat-emulsion tubing every 24 hours; change propofol tubing every 6 to 12 hours.
- Change needleless connectors at least as often as tubing.
- Keep all components of the I.V. system or transducer system sterile, and minimize the number of entries.
- When accessing the catheter, use an appropriate antiseptic and access only with sterile devices.
- If CLABSI rates don’t decline despite use of core strategies, use a chlorhexidine-impregnated sponge dressing for patients older than 2 months and antiseptic/antibiotic-coated catheters for all patients.
CDC recommendations also stress the critical importance of removing catheters when they’re no longer needed. As nurses, we should speak up to other healthcare team members when a patient’s catheter is no longer necessary. In collaboration with the multidisciplinary team, we can have a dramatic impact in reducing preventable infections by implementing CDC recommendations rigorously.
Selected reference
O’Grady NP, Alexander M, Burns, LA, et al.; Healthcare Infection Control Practices Advisory Committee. Guidelines for the prevention of intravascular catheter-related infections. Am J Infect Control. 2011;39(4 Suppl 1):S1-34.
Cass Piper Sandoval is a clinical nurse specialist in adult critical care at the University of California San Francisco Medical Center.
Click to read the next article: Preventing surgical-site infections