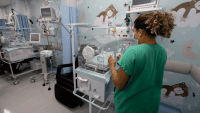
Billing by nursing intensity: One way to ease understaffing?
Re: “Hospital nurse staffing for dummies” (March 2013): Perhaps changing how nurses’ time is billed would help relieve understaffing. Most hospitals treat nursing services as a cost, along with rooms, meals, and housekeeping. This approach creates an incentive to minimize this cost. But the work required of RNs, LPNs, and CNAs varies not just with the number of patients but with patient acuity. Higher-acuity patients require more time and a greater skill set. My understanding is that ICU stays are billed for higher acuity, unlike stays on other units; even if a hospital wished to staff non-ICU units according to acuity, it would nevertheless bill a flat rate per patient regardless of acuity.
What’s needed is a direct link between good staffing levels and reimbursement on all hospital units. John Welton suggested one way to do this: Change nursing services from a cost center to a revenue center by billing according to nursing intensity. (“Mandatory Hospital Nurse to Patient Staffing Ratios: Time to Take a Different Approach,” Online Journal of Issues in Nursing, September 30, 2007). This way, payment for nursing services would accurately reflect time nurses spend with the patient and on the patient’s behalf, as well as the skills required. Making a direct connection between services rendered and payment for those services might be easier for hospital managers and boards to accept than ethical- and evidence-based arguments, as this approach confronts the financial issue head on.
A related concern is nurses’ lack of autonomy and power in determining adequate staffing. Creating a direct financial link between nursing intensity and reimbursement demonstrates the vital role of nurses in keeping a hospital a going concern, and suggests staff nurses should have a larger say in determining staffing levels.
I hope a future American Nurse Today article will explore the relationship of nurse staffing to billing. For instance: What issues would prevent hospitals from billing by nursing intensity on all units? Does the nursing department have to change from a cost center to a revenue center to allow such billing? Do current state and federal laws, Medicaid and Medicare rules, or insurance rules prevent it? Does the Affordable Care Act address this issue? Given hospital administrators’ concern over costs, the true costs of nurses’ time and skills need to be itemized and reimbursed—and reflected fully in the bottom line.
Stephanie Bank, BSN, RN
Maryville, Tennessee
Helping new nurses feel more connected to the nursing unit
I enjoyed “Building a sense of community on nursing units” (March 2013). The unit I currently work on has more new nurses than experience nurses. Our experienced nurses try to make sure each new nurse fits into the unit’s culture. Recently, though, some of our new nurses have been feeling overwhelmed and are ready to terminate employment. They believe their workloads are excessive and feel disconnected from the unit. I know that feeling, because I once had it myself. To help reduce these feelings, we’ve been hosting welcoming celebrations where we introduce new nurses to the staff to ease their transition from graduate nurse to professional nurse.
To build a sense of community on nursing units, nursing leaders need to focus on employee rounding, social networking, employee recognition, empowering the staff to create interventions for challenges, and onboarding of new nurses. I hope to implement these actions on my unit soon by sharing this article with my tenured coworkers and nurse manager.
Tracey L. Clayton, BSN, RN, CVRN
Houston, Texas
We welcome your comments. You may submit letters to the editor electronically at www.AmericanNurseToday.com, or by mail to: Letters to the Editor, American Nurse Today, c/o HeatlhCom Media, 259 Veterans Lane, Doylestown, PA 18901. Please include your full name, credentials, city, state, and daytime phone number or e-mail address. Letters should contain no more than 250 words and will be edited for grammar, length, content, and clarity. All letters are considered American Nurse Today property and therefore unconditionally assigned to American Nurse Today.