Focus on safety and trust.
- Research indicates that many nurses who joined teams during the pandemic feel less connected to other team members.
- With intentional work that restores trust and psychological safety, leaders can rebuild team cohesiveness.
Maria works as a perioperative director in a large academic medical center. Until the COVID-19 pandemic, she managed a cohesive team with many seasoned staff members. Unfortunately, most of the experienced nurses retired during the pandemic. Today, Maria’s team consists primarily of new graduates and nurses on travel contracts. She sees that staff members lack connection with one another. She’s challenged with bringing a new team together after the old team fell apart.
Maria’s situation isn’t unusual. Early in the pandemic, many nurse leaders marveled at the sense of teamwork and collaboration among staff. Fast forward to today, and they find themselves in a different place. Two sustained years of fighting the pandemic caused massive disruption to healthcare teams. In 2021, according to Berlin and colleagues, nurse turnover skyrocketed, and many seasoned nurses retired. Today’s nursing teams include less experienced nurses and nurses on travel or agency contracts. Most team rituals disappeared because of social distancing, and even onboarding occurred remotely. Nurses no longer ate together, and the team didn’t celebrate special events such as birthdays and baby showers. In addition, nurses socialized less outside of work. Maria sees her team members struggle to find meaning in their work, and they lack the social glue that rituals provided to keep them together.
Research indicates that many nurses who joined teams during the pandemic feel less connected to other team members. Wearing personal protective equipment made it difficult to read facial expressions and sometimes recognize and talk with other staff members. Healthcare has always been a team sport, especially in perioperative nursing. Nurses rely on one another to deliver safe and quality care, and team backup is essential.
The good news for Maria is that with intentional work she can rebuild teamwork. She can start by restoring trust and psychological safety. Without these two essential ingredients, Maria will struggle to rebuild a high-functioning team.
Psychological safety and trust
Leaders haven’t always understood how trust and psychological safety impact team functioning. Google began research in this area in 2011 as part of Project Aristotle. Leaders’ experience with the workforce at Google indicated that hiring the best software engineers didn’t always lead to the best team synergy or outcomes. When researchers studied 180 teams, they found that psychological safety and trust mattered more than individual expertise. These findings were consistent with work by Lencioni, who found that the primary drivers of team dysfunction were an absence of trust and psychological safety.
Edmondson, a researcher at Harvard, was the first to identify the importance of psychological safety on healthcare teams. In her dissertation work, she found that when team members feel psychological safety, they’re more likely to admit medical errors. Edmondson defines psychological safety as an individual’s belief that they can show who they are without fear of negative consequences.
Psychological safety and trust are closely linked. A lack of trust on a team slows every decision, communication, and relationship. For Maria and many healthcare leaders today, team member changes and a resulting lack of connection create barriers to building trust. As the leader, Maria will have to create a learning environment where nurses feel comfortable expressing their opinions, discussing problems, and recommending solutions.
Fortunately, leaders like Maria can take positive action by building a supportive team culture that helps transition new graduate and travel nurses into the perioperative unit. For example, she can institute a comprehensive orientation that provides clear role definition. In addition, Maria can increase her presence on the team to observe the nurses in practice and provide timely and effective performance feedback. Actively communicating constructive feedback promotes learning, resulting in a stronger sense of psychological safety with increased positive behaviors, attitude, and performance. These actions promote a culture of teamwork and demonstrate to the nurses that Maria is willing to invest in them and their psychological safety. (See Rating psychological safety.)
Rating psychological safety
To evaluate psychological safety, Edmonds identified seven critical statements that leaders can ask team members to rate on a Likert scale of “strongly disagree” to “strongly agree.”
- If you make a mistake on this team, it is often held against you.
- Members of this team can bring up problems and tough issues.
- People on this team sometimes reject others for being different.
- It is safe to take a risk on this team.
- It is difficult to ask other members of this team for help.
- No one on this team would deliberately act in a way that undermines my efforts.
- Working with members of this team, my unique skills and talents are valued and utilized.
Building a culture of teamwork
Some leaders hesitate to evaluate sensitive topics, such as trust and psychological safety, because they think they already know the problems or they fear difficult feedback. But you need baseline data to help the team learn and grow. If you don’t ask, you won’t know what to start, stop, or continue doing to build a culture of teamwork.
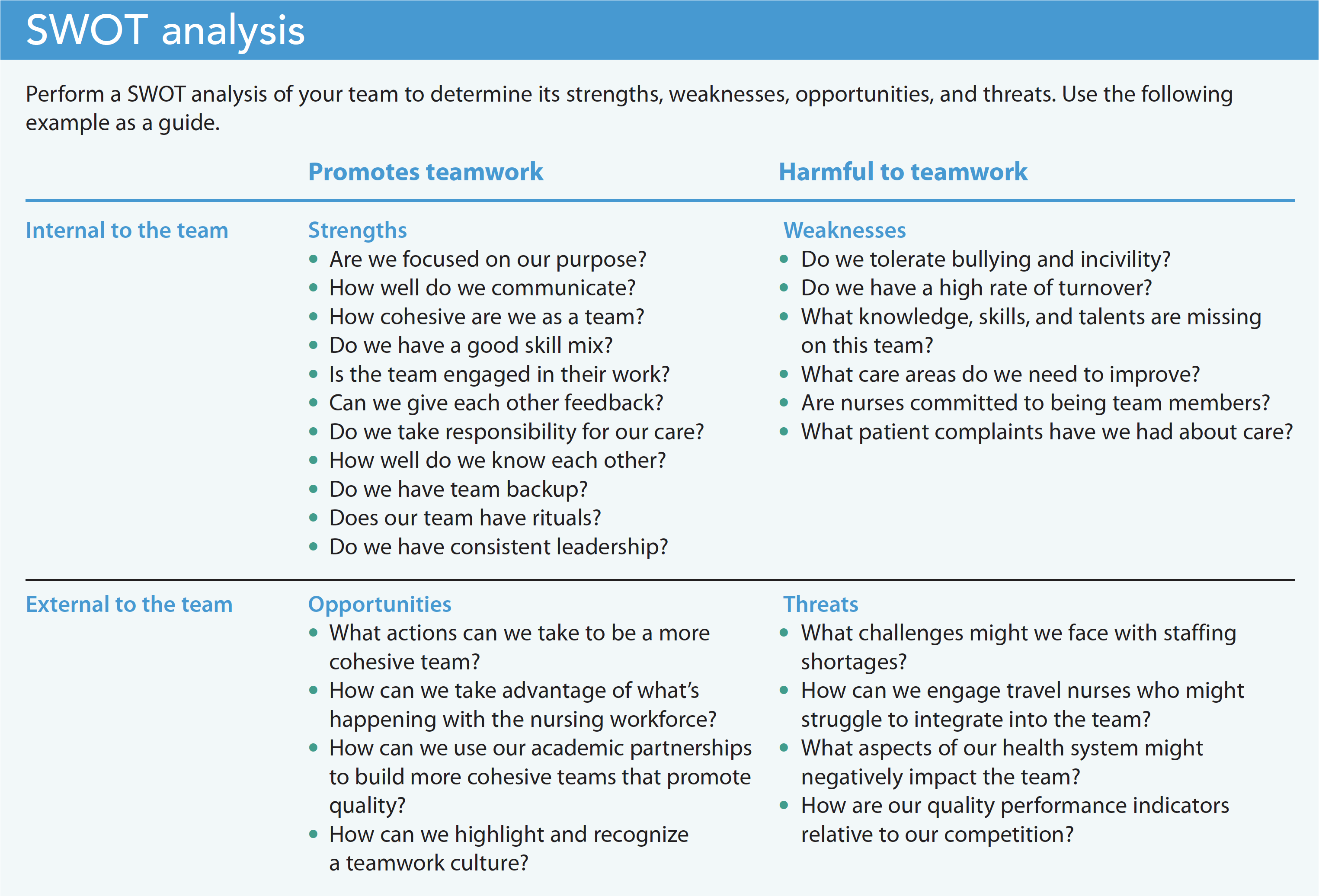
Maria needs to recognize that team culture evolves and changes over time. When assessing the culture, Maria can perform a SWOT (Strengths, Weaknesses, Opportunities, Threats) analysis with her team to determine how well they work together. With the results, she can develop plans to rebuild a teamwork culture, focusing on key areas of concern such as communication, backup, skills gaps, rituals, connectedness, and purpose. (See SWOT analysis.)
Avoiding team dysfunction
During a turbulent time, such as the pandemic, dysfunctional team behaviors can become normalized. Without psychological safety, new team members may be reluctant to speak up about deviant behaviors and practices. This is especially true with the influx of so many recent graduates who may lack the mentorship they need to feel psychologically safe on a team. Maria must spend time with new nurses and role model the kind of feedback that should take place on teams, such as asking questions when they’re unsure about a policy or practice and seeking advice about their professional performance. Maria should demonstrate that the nurses can talk about mistakes and errors without fear of punishment and that it’s okay to ask for backup when they feel overwhelmed. In addition, Maria can encourage new nurses to offer suggestions for improvement and share concerns.
Two key contributors to team dysfunction are the inability of teams to effectively deal with conflict and the tolerance of incivility and bullying. Nurses frequently view conflict as a bad thing. Seeing constructive conflict as an opportunity for improvement requires a paradigm shift for some nurses who strive for team harmony and prefer to bury discord. Navigating through conflict provides opportunities for team growth and helps team members gain skills and confidence in constructively managing disagreement.
Maria also must assess the team for signs of bullying and incivility. A zero-tolerance culture for bullying is the most effective prevention strategy. Staff require education about the behaviors that constitute bullying to help break the silence. Dysfunctional teams present challenges to promoting a culture of nurse well-being crucial in a post-COVID environment. (See Bullying red flags.)
Bullying red flags
Thompson noted the following warning signs that might indicate bullying and incivility within a team:
- Talking behind others’ backs rather than directly resolving conflicts.
- Making belittling comments or criticizing colleagues in front of others.
- Not sharing important information with a colleague.
- Isolating or freezing out a colleague from group activities.
- Making snide or abrupt remarks.
- Refusing to be available when a colleague needs assistance.
- Committing acts of sabotage that deliberately set up team members for a negative situation.
- Raising eyebrows or making faces in response to colleagues’ comments.
- Failing to respect colleague privacy.
- Breaking confidences.
Coaching teams to promote well-being
For years to come, researchers will study the long-term impact of COVID-19 on the nursing workforce and teams. The pandemic has impacted mental health profoundly, especially in acute care environments. In perioperative areas, elective surgeries were postponed, so Maria may have staff who were redeployed to critical care or COVID units. Recent American Nurses Association research indicates that COVID-19 has been especially devastating for younger nurses who transitioned into the profession during the pandemic, with 66% of nurses under 35 reporting feeling anxious, and 43% reporting feeling depressed. These numbers are far higher than other age groups.
Effective team coaching can help Maria promote nurse well-being. She should start by normalizing the anxiety and stress that nurses may feel as a result of their pandemic experiences, ensuring that team members take breaks, and encouraging them to share resilience strategies. Being physically, mentally, and emotionally present will support Maria’s coaching efforts and give her opportunities to listen to staff concerns. Being present also will enable Maria to spot signs of moral distress or compassion fatigue so she can make appropriate referrals.
If possible, Maria should consider creating physical spaces nurses can use to de-stress. She also can ask for input from the team about scheduling strategies that respect their time outside of the unit and allow for rest and recovery. In addition, Maria can incorporate well-being check-ins as part of team meetings and promote programs that teach mindfulness, self-compassion, and self-care. She also can help team members re-establish rituals and build connections and personal relationships with one another.
If Maria stays vulnerable and uses supportive empathy, she’ll encourage team members to have crucial well-being conversations. When she asks, “What do you need?” nurses will be more open to honestly answering because they’ve experienced Maria’s investment in their well-being.
Looking toward a brighter future
Coming together after falling apart isn’t easy, but it’s crucial for many nursing teams. A lack of connection to team members has led many nurses to feel as if they’re dispensable and that their organization doesn’t value their well-being. To effectively rebuild her team, Maria must create a psychologically safe team culture where members trust one another. Team members must feel personally valued for their contributions and believe that their well-being is a priority. The pandemic has been challenging for nurse leaders. They must effectively navigate through the fallout of a turbulent time and move their teams into a brighter future.
Rose O. Sherman is an adjunct professor at the Marian K. Shaughnessy Nurse Leadership Academy, Case Western Reserve University in Cleveland, Ohio, and author of The Nuts and Bolts of Nursing Leadership: Your Toolkit for Success and The Nurse Leader Coach: Become the Boss No One Wants to Leave. You can read her blog at emergingrnleader.com. Tanya M. Cohn is an associate professor of practice and a consulting nurse scientist at Simmons University in Boston, Massachusetts.
References
American Nurses Foundation. Pulse on the Nation’s Nurses Survey Series: COVID 19 Two Year Assessment Survey. 2022. nursingworld.org/~492857/contentassets/872ebb13c63f44f6b11a1bd0c74907c9/covid-19-two-year-impact-assessment-written-report-final.pdf
Berlin G, Lapointe M, Murphy M. Surveyed nurses consider leaving direct patient care at elevated rates. McKinsey. February 17, 2022. mckinsey.com/industries/healthcare-systems-and-services/our-insights/surveyed-nurses-consider-leaving-direct-patient-care-at-elevated-rates
Davis C. Nearly 30% of RNs are at risk of leaving their organization, new analysis reveals. www. HealthLeaders. September 30, 2021. healthleadersmedia.com/nursing/nearly-30-rns-are-risk-leaving-their-organization-new-analysis-reveals
Edmondson A. The Fearless Organization: Creating Psychological Safety in the Workplace for Learning, Innovation, and Growth. New York, NY: Wiley; 2018.
Edmondson AC. Psychological safety and learning behavior in work teams. Admin Sci Q. 1999;44(2):350-83. doi:10.2307/2666999
Lencioni P. Overcoming the Five Dysfunctions of a Team: A Field Guide for Leaders, Managers, and Facilitators. San Francisco, CA: Jossey-Bass; 2005.
re:Work. Google. rework.withgoogle.com/print/guides/5721312655835136
re:Work. Tool: Foster psychological safety. Google. rework.withgoogle.com/guides/understanding-team-effectiveness/steps/foster-psychological-safety
Thompson R. Enough! Eradicate Bullying and Incivility in Healthcare: Strategies for Front Line Leaders. Incredible Messages Press; 2019.
Wang H-F, Chen Y-C, Yang F-H, Juan C-W. Relationship between transformational leadership and nurses’ job performance: The mediating effect of psychological safety. Soc Behav Personality. 2021;49(5):e9712. doi:10.2224/sbp.9712
American Nurse Journal. 2022; 27 (11). Doi: 10.51256/ANJ112213