Few things cause as much angst for a nurse as placing a patient in a restraint, who may feel his or her personal freedom is being taken away. But in certain situations, restraining a patient is the only option that ensures the safety of the patient and others.
As nurses, we’re ethically obligated to ensure the patient’s basic right not to be subjected to inappropriate restraint use. Restraints must not be used for coercion, punishment, discipline, or staff convenience. Improper restraint use can lead to serious sanctions by the state health department, The Joint Commission (TJC), or both. Use restraints only to help keep the patient, staff, other patients, and visitors safe—and only as a last resort.
Categories of restraints
Three general categories of restraints exist—physical restraint, chemical restraint, and seclusion.
Assessing and documenting patient restraint incidents
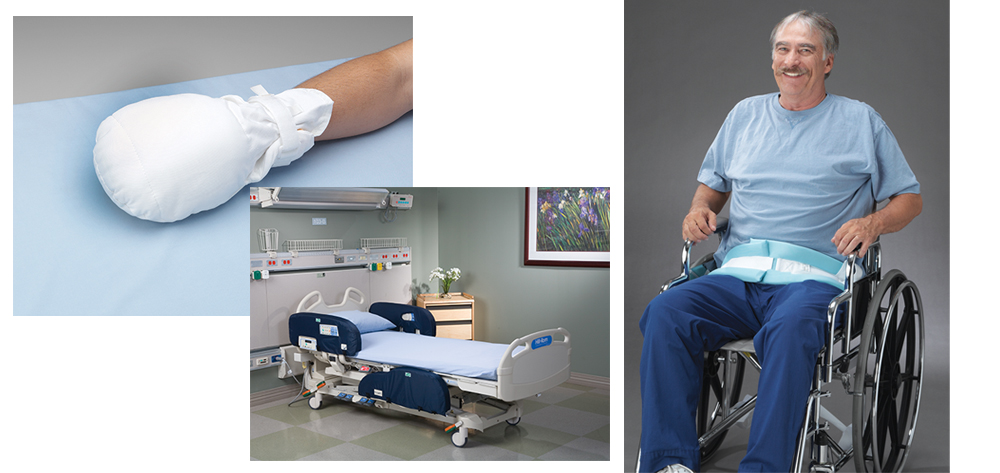
Enclosure bed: A protective and calming restraint
Physical restraint
Physical restraint, the most frequently used type, is a specific
intervention or device that prevents the patient from moving freely or restricts normal access to the patient’s own body. Physical restraint may involve:
- applying a wrist, ankle, or waist restraint
- tucking in a sheet very tightly so the patient can’t move
- keeping all side rails up to prevent the patient from getting out of bed
- using an enclosure bed.
Typically, if the patient can easily remove the device, it doesn’t qualify as a physical restraint. Also, holding a patient in a manner that restricts movement (such as when giving an intramuscular injection against the patient’s will) is considered a physical restraint. A physical restraint may be used for either nonviolent, nonself-destructive behavior or violent, self-destructive behavior. (See What isn’t a restraint?)
Restraints for nonviolent, nonself-destructive behavior. Typically, these types of physical restraints are nursing interventions to keep the patient from pulling at tubes, drains, and lines or to prevent the patient from ambulating when it’s unsafe to do so—in other words, to enhance patient care. For example, a restraint used for nonviolent behavior may be appropriate for a patient with an unsteady gait, increasing confusion, agitation, restlessness, and a known history of dementia, who now has a urinary tract infection and keeps pulling out his I.V. line.
Restraints for violent, self-destructive behavior. These restraints are devices or interventions for patients who are violent or aggressive, threatening to hit or striking staff, or banging their head on the wall, who need to be stopped from causing further injury to themselves or others. The goal of using such restraints is to keep the patient and staff safe in an emergency situation. For example, a patient responding to hallucinations that commands him or her to hurt staff and lunge aggressively may need a physical restraint to protect everyone involved.
Chemical restraint
Chemical restraint involves use of a drug to restrict a patient’s movement or behavior, where the drug or dosage used isn’t an approved standard of treatment for the patient’s condition. For example, a provider may order haloperidol in a high dosage for a postsurgical patient who won’t go to sleep. (If the drug is a standard treatment for the patient’s condition, such as an antipsychotic for a patient with psychosis or a benzodiazepine for a patient with alcohol-withdrawal delirium, and the ordered dosage is appropriate, it’s not considered a chemical restraint.) Many healthcare facilities prohibit use of medications for chemical restraint.
Seclusion
With seclusion, a patient is held in a room involuntarily and prevented from leaving. Many emergency departments and psychiatric units have a seclusion room. Typically, medical-surgical units don’t have such a room, so this restraint option isn’t available. Seclusion is used only for patients who are behaving violently. Use of a physical restraint together with seclusion for a patient who’s behaving in a violent or self-destructive manner requires continuous nursing monitoring.
Determining when to use a restraint
The patient’s current behavior determines if and when a restraint is needed. A history of violence or a previous fall alone isn’t enough to support using a restraint. The decision must be based on a current thorough medical and psychosocial nursing assessment. Sometimes, addressing the issue that’s underlying a patient’s disruptive behavior may eliminate the need for a restraint.
Also, caregivers must weigh the risks of using a restraint, which could cause physical or psychological trauma, against the risk of not using it, which could potentially result in the patient harming him- or herself or others. Input from the entire care team can help the provider decide whether to use a restraint.
Alternatives to restraints
Use restraints only as a last resort, after attempting or exploring alternatives. Alternatives include having staff or a family member sit with the patient, using distraction or de-escalation strategies, offering reassurance, using bed or chair alarms, and administering certain medications.
If appropriate alternatives have been attempted or considered but have proven insufficient or ineffective or are deemed potentially unsuccessful, restraint may be appropriate. A provider order must be obtained for patient restraint. Be sure to update and revise the care plan for a restrained patient to help find ways to reduce the restraint period and prevent further restraint episodes.
Reducing restraint risks
Restraints can cause injury and even death. In 1998, TJC issued a sentinel event alert on preventing restraint deaths, which identified the following risks:
- Placing a restrained patient in a supine position could increase aspiration risk.
- Placing a restrained patient in a prone position could increase suffocation risk.
- Using an above-the-neck vest that’s not secured properly may increase strangulation risk if the patient slips through the side rails.
- A restraint may cause further psychological trauma or resurfacing of traumatic memories.
To help reduce these risks, make sure a physical restraint is applied safely and appropriately. With all types of restraints, monitor and assess the patient frequently. To relieve the patient’s fear of the restraint, provide gentle reassurance, support, and frequent contact. Monitor vital signs (pulse, respiration, blood pressure, and oxygen saturation) to help determine how the patient is responding to the restraint.
Changing the culture
The American Psychiatric Nurses Association’s position statement on the use of restraint suggests a unit’s philosophy on restraint use can influence how many patients are placed in restraints. Interacting with patients in a positive, calm, respectful, and collaborative manner and intervening early when conflict arises can diminish the need for restraint. Facility leaders should focus on reducing restraint use by supporting ongoing monitoring and quality-improvement projects.
To help ensure a restraint is applied safely, nurses should receive hands-on training on safe, appropriate application of each type of restraint before they’re required to apply it. Such training also should occur during orientation and should be reinforced periodically.
The goal is to use the least restrictive type of restraint possible, and only as a last resort when the risk of injury to the patient or others is unacceptably high. Consider using restraint only after unsuccessful use of alternatives, and only as long as the unsafe situation occurs. Remember—restraint use is an exceptional event and shouldn’t be a part of a routine protocol.
Selected references
American Psychiatric Nurses Association. APNA Position Statement on the Use of Seclusion and Restraint. Original 2000; revised 2007; revised 2014. www.apna.org/i4a/pages/index.cfm?pageid=3728. Accessed November 4, 2014.
American Psychiatric Nurses Association. Seclusion & Restraint Standards of Practice. May 2000; Revised May 2007; revised April 2014. www.apna.org/i4a/pages/index.cfm?pageid=3730. Accessed November 4, 2014.
Federal Register. Part II; Department of Health and Human Services, Centers for Medicare & Medicaid Services; Medicare and Medicaid Programs. 42 CFR Part 482; Medicare and Medicaid Programs; Hospital Conditions of Participation: Patients’ Rights; Final Rule. December 8, 2006. www.cms.gov/Regulations-and-Guidance/Legislation/CFCsAndCoPs/downloads/finalpatientrightsrule.pdf. Accessed November 26, 2014.
Joint Commission, The. Hospital Accreditation Standards. Provision of Care, Treatment and Services. Standards PC.03.05.01 through PC.03.05.19. 2010.
Joint Commission, The. Sentinel Event Alert. Issue 8, November 18, 1998. Preventing Restraint Deaths. www.jointcommission.org/assets/1/18/SEA_8.pdf. Accessed November 4, 2014.
Gale Springer is a mental health clinical nurse specialist at the Providence Regional Medical in Everett, Washington.
Read the next article: Choosing the right restraint



















9 Comments.
I woke up in post op.Last week after having surgery on my hand.im 58 first surgery.The nurse was attempting to remove my gown.im not sure who is doing what to me.I asked whats going on.She starts yelling at me stop being combative and other words.2 days later I call the surgeon office.i was given Hydro 5s …my hand was killing me.His nurse tells my wife take 2 but they will be gone faster.Really….so I went to different hospital and was treated properly. IS THIS NORMAL
I understand the need for judicious use of restraints but when lawmakers and other ignorant people get involved w things they no nothing about it makes my blood boil. My mother in law is DEAD because of the inability of her care center to use any kind of restraint. It’s pure stupidity to think that some of their recommendations can actually impact a patient w dementia. Bedrails would have saved my mother in law A serious head injury, years of broken bones and pain and suffering. Are we!going to stop putting restraints on our babies now too? Forget the side rails. Just reason w them. I really wish stupid people would mind their own business and stick to what they do know if anything!
My 97 Year old mom is in a dementia home and she is severely hobbled. She can barely use a walker. The nurses have removed the foot rests on her wheel chair and see is able to shuttle around the place while in her chair. But she has attempted on a number of occasions to stand from the chair (which she cannot do without help) and has ended up on the floor. Staff has indicated that the safety belt on the chair is a “restraint” and are not willing to use it. I think i found the solution which is nothing more than a tray table which attaches to the chair handles with simple Velcro. The tray is a great place to place food, drink and reading materials. So is this considered “restraints”?
Hello,
At the hospital where I work, we use Mitts. My administration is advising the staff, mitts are not considered a RESTRAINT & no need for Doctor’s order. As long as the mitts are not tied down.
A patient’s fingers are restricted and hands are restricted with mitts; without tie downs being utilized.
Will you please advise me on the National view or policies.
I was in a mental institution and was given a shot because of my behavior. I was not put in a room. Literally they gave me the shot and let me keep wandering. Now I have severe bruising on my face, including a bad black eye. They said I fell but should they not have taken me to a room instead of giving it to me standing up?
I would like information on restraining incubated patients. We do not want sedation to interefere with a patient’s ability to be awake enough to breath on there own to prepare for extbubation as soon as possible.
Most of these patients will attempt very hard to self extubate with the risk of severe injury to themselves.
Are the standards different for emergency critical care settings?
Hi. We’re the nursing staff at Providence Willamette Falls hospital and would like to have some information about administering IM meds to patients who are in restraints due to agitated and aggressive behaviours.
How many recommended staff members do es it take to restrain a patient safely?
Should a patient be released from restraints (due to violent behaviors) once they fall asleep? Or do you wait until they wake up to make an assessment for possible release at that time?