Twenty-two percent: That’s how many frontline RNs in the United States said, in a response to a recent McKinsey survey, that they may leave direct patient care within the next year. Why? And what can be done about it?
At any given time, of course, a certain number of nurses are going to retire or decide to try something new. But in 2019, the figure for turnover was only 15.9%, according to Nursing Solutions Inc.’s 2020 NSA National Health Care Retention and RN Staffing Report.
The most important reason for the difference in the current survey, not surprisingly, is the ongoing pandemic; almost three-quarters of those surveyed had dealt with COVID-19. Although many managers have made significant efforts to provide support, nurses suffered great physical and psychological stress even as they cared for the sick and dying. Sixty percent of those who said they were planning to leave said COVID-19 played a role, citing insufficient staffing, rising workloads, the heavy emotional toll—and, often, lack of support.

On the brighter side, 17% said they are more likely to stay in the nursing profession given their experiences during COVID-19. Economic considerations—pay, stability, and flexibility— were mentioned most often. What may be more interesting, though, is what came next: support of management, impact on lives, and professional pride.
COVID-19 was a once-in-a-century event (we hope); the extraordinary demands of this period were unprecedented. And in many ways, healthcare adapted admirably, introducing new ways of working, such as the greater use of virtual care. Nevertheless, there are lessons to be learned. One is that healthcare leaders should not be thinking about getting back to the pre-COVID normal, but rather about building anew.
Here are three priorities the survey identified that can help nurses—strengthening both the profession and the US healthcare system.
Understand what nurses value. One thing that stands out is the role of management and line support—it’s a reason to go for the leavers and a reason to stay for the remainers. Nurses value having input into decision making. Perhaps that explains why the most common responses to the question of what more could be done to support nurses were appropriate recognition and open communication (followed by more breaks and active monitoring of distress).
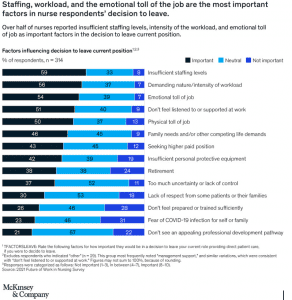
The evidence is clear: when nurses believe that their own health and well-being is valued, it makes a difference: 69% said management support would influence their decision on whether to stay. Not every healthcare facility can improve benefits, add staff, or pay for new technology. But listening to nurses? That’s something everyone can do.
It’s telling, for example, that while most nurses reported getting additional protective equipment, only a quarter said the same for mental health/well-being support, and a third additional compensation. One out of eight received no additional support of any kind. One thing that nurses particularly valued is scheduling flexibility. Among nurses who said they planned to continue with direct patient care, flexibility in hours/shifts was a key factor, just behind compensation and benefits. The implication is that hospital leaders may be surprised at the extent to which their workforce is receptive to new models such as picking up ad hoc short shifts.
Reimagine delivery models. More than 40% of frontline nurses have delivered care virtually within the last year, with the highest rates reported by nurses practicing in outpatient, ambulatory, and home-care settings. Roughly two-thirds of frontline nurses are interested in providing virtual care in the future—and 83% of those working in long-term care settings.
We believe there is great potential in new care models, such as telemedicine, and the greater use of digital tools. Indeed, virtual care may be particularly appealing to groups most likely to leave the workforce. By thinking in new ways, employers may be able to create hybrid schedules that could prove broadly attractive to nurses.
Expand opportunities for professional development. Demand for talent is increasing, and skillsets and capabilities required are shifting. COVID-19 accelerated the introduction of different staffing approaches, and nurses were largely enthusiastic. One interesting survey finding was the extent to which nurses “floated” across units, acuity levels and settings in 2020—more than 60%, almost double the pre-pandemic rate. About a third who floated are interested in continuing to do so.
In typical float pools, nurses migrate within specialties or acuity levels. But many of those surveyed were more excited about floating between them. Such flexible float pools could be useful in a wide variety of care settings. For this model to work, nurses need to have the relevant skills. In the survey, however, a third of frontline nurses said they aren’t confident that they have the skills necessary for future success; two-thirds said they would value additional training. They look to their employers for clearer clinical guidelines and training. The same outlook holds true for virtual care; there is high interest (65%), but concern about readiness.
COVID-19 has affected nurses deeply. The pressures of the pandemic have exacerbated workforce vulnerabilities—and thoroughly exasperated many nurses. No wonder that more than one in five are considering leaving frontline work. With imagination and commitment, though, COVID-19 could also be a catalyst for improvement in management, technology, and processes—and keep more nurses doing what they do best.
Gretchen Berlin is a senior partner in McKinsey’s Washington, DC, office. Molly Viscardi is a consultant in McKinsey’s Philadelphia office. The authors would like to extend a heartfelt thank you to the nurses on the frontlines who are caring for our patients and communities during this time.
Access more information from the report at mckinsey.com/industries/healthcare-systems-and-services/our-insights/nursing-in-2021-retaining-the-healthcare-workforce-when-we-need-it-most.



















