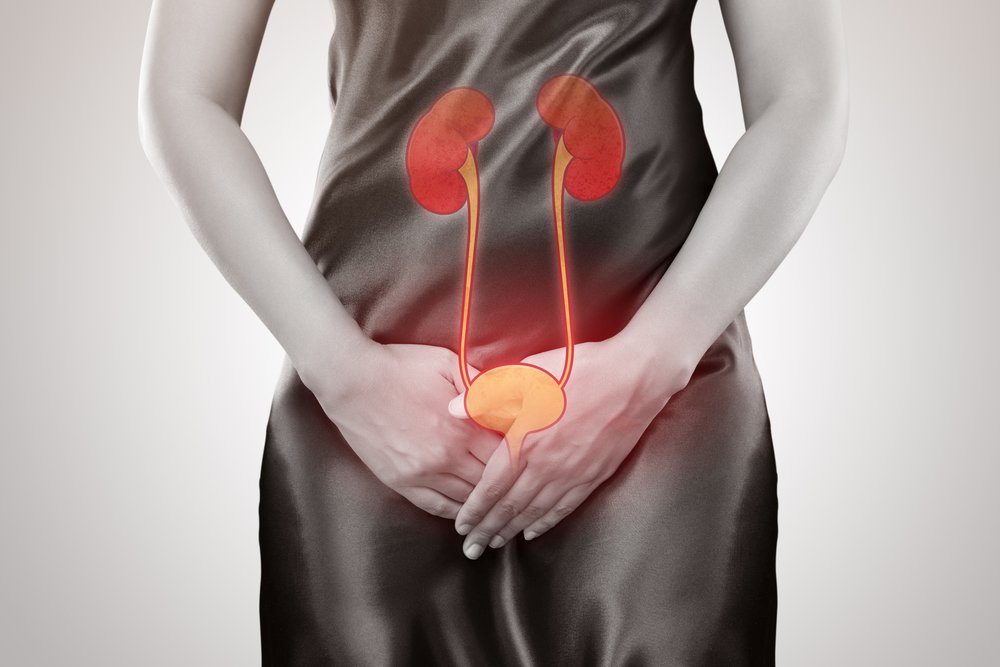
An often-neglected area of
women’s healthcare is utero-vaginal prolapse and urinary symptoms.
PROLAPSE
Most women develop minimal
dropping of the uterus but have no symptoms. However, I have always been
surprised how some women with almost no visible prolapse complain of a sense of
dropping, and on the other hand I have had patients with a really advanced
stage of prolapse who seem to be completely unaware of any problem at all.
Treatment should always start
with prevention, but this requires education of women in their early
childbearing years.
· Early prevention starts with
pregnancy, especially during delivery, with the obstetrician doing all she can
to safeguard against excessive stretching, tearing, and damaging. Tears and an
episiotomy require meticulous repair.
· Other potential causes that can be
addressed include avoiding excessive weight gain, treating a chronic cough
(invariably meaning avoiding smoking), and keeping the bowels regular to
prevent chronic constipation.
· Pelvic floor exercises, tightening
and loosening the pelvic muscles can be of value. A trick I have taught my
patients over the years is, every time they are driving and stop at a red
light, to squeeze the vagina tight as if trying to keep something in, and to
hold the squeeze until the light turns green. Try it. It is not as simple as it
sounds.
· After menopause there is a little
evidence that local or systemic HT may be of some benefit.
· Truly symptomatic uterovaginal
prolapse that does not respond to any of the above may be a good reason to
consider a surgical repair. I certainly endorse this approach; only make
certain that you use a good gynecologic surgeon or urogynecologist
(gynecologist with special specialty training in bladder and pelvic floor). Another
good tip – apply local vaginal estrogen for a few weeks before surgery. It is
quite amazing how it improves the quality of the tissue and makes for a better
repair.
URINARY SYMPTOMS
STRESS INCONTINENCE
Everything I describe above
for uterovaginal prolapse applies to the problem of the bladder that leaks
uncontrollably when you cough, run, sneeze, or have any muscular exertion.
One difference is the value of
hormone therapy (HT). Contrary to what we would have expected, there is
evidence that combinations of estrogen and progestogen after menopause may
actually make stress incontinence worse.
Another difference is when it
comes to surgery. Here I certainly suggest you use the services of a skilled
urogynecologist because diagnostic tests are necessary to confirm if and what
type of surgery is necessary. Moreover, surgery for stress incontinence these
days is invariably performed with an abdominal approach, except for special
circumstances.
Let me emphasize that stress
incontinence is not a normal part of aging, can be excessively disruptive to
quality of life, and should not be neglected. Expert help is available, so make
use of it.
OVERACTIVE BLADDER/URGE
INCONTINENCE
OAB and urge incontinence are
not the same, but close. OAB is a condition of urge to urinate that may or may
not be associated with leaking, but usually involves over eight voids per day
and usually at night as well (nocturia).
You don’t need to worry too much about the difference; your concern is if you
have symptoms of “need to go”, frequency, or urge and then leaking before you
get to the toilet. The urogynecologist will work out the cause. One thing to
exclude will be recurrent bladder infections.
Nonpharmacologic strategies
for avoiding recurrent infections include emptying the bladder after
intercourse, wiping front to back after a bowel movement, and even trying
regular intake of cranberry juice.
Strategies for dealing with
overactive bladder include:
· Restrict fluids and avoid bladder
irritants like caffeine drinks.
· Bladder retraining involves similar
exercises as I described for stress incontinence. The pelvic muscles must be
contracted as the first symptom of urge rears its ugly head.
· There are a large number of
FDA-approved medications. These include drugs with names like Ditropan, Detrol,
Vesicare, and Enablex. Some come as pills, others as patches.
· Botulinum (Botox) injections are
also sometimes of value.
Once again, my message is that
if women have these symptoms, they should seek help and improve their quality
of life.
Have a wonderful week.
Wulf Utian MD PhD DSc
Author; CHANGE YOUR MENOPAUSE – Why one size does not fit all. http://www.amazon.com/Change-Your-Menopause-size-does/dp/0982845723/