Understand women’s unique risks and symptoms to ensure early identification and treatment of CVD.
Takeaways:
- Cardiovascular disease (CVD) remains the leading cause of mortality in women; women of color are at greater risk for CVD than white women.
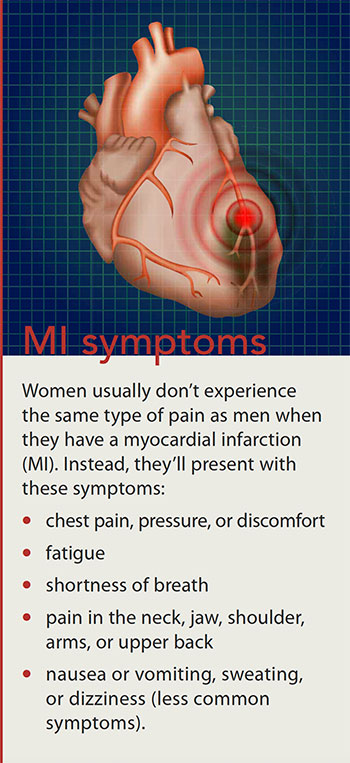
- Women’s symptoms of myocardial infarction are vague and easy to miss.
- To maintain ideal cardiovascular health, women should consume a diet consisting primarily of fruits, vegetables, whole gains, and low fat sources of protein, participate in moderate exercise at least 150 minutes per week, sleep 7 hours per night, and reduce stress.
- In women at risk or high risk for CVD, medications may be needed when lifestyle interventions alone fail.
By Melanie Kalman, PhD, RN, CNS, and Margaret Wells, PhD, RN, APN-BC
Cardiovascular disease (CVD), which includes diseases of the heart, brain blood supply, and vascular system, is the number one cause of death in the United States. About 2,200 American adults die of CVD every day—that’s one out of every three deaths. Almost 2 million Americans live with CVD, which can lead to myocardial infarction (MI), strokes, heart failure, renal disease, and peripheral artery disease.
Despite improvements in treatment, CVD remains the leading cause of mortality in women. (See By the numbers.) Women—and many healthcare providers—lack knowledge about CVD risk factors and MI symptoms unique to women, which leads to late recognition and inadequate treatment.


Risk factors

Natural estrogen in premenopausal women is believed to be cardioprotective, but replacement estrogen taken during menopause doesn’t help prevent CVD. Researchers are asking why, if estrogen is cardioprotective, we’re seeing more MIs in younger women. No clear answer exists. However, younger women who have MIs are more likely to be obese or to have hypertension, tachycardia, or type 2 diabetes, but that doesn’t completely answer the question.
Women of color are at greater risk for CVD than white women. Black women in the United States are at higher risk for an MI than all other women, and many experience an MI at a younger age. Because they may have no symptoms, they have higher rates of sudden cardiac death. Typically, Hispanic and Black women have more comorbidities (such as diabetes, hypertension, and obesity) than white women. When black women present to the emergency department (ED), they’re less likely than white women to be treated using the American Heart Association (AHA) guidelines. This is particularly true for younger women of color, who are less likely to be prescribed angiotensin-converting enzyme (ACE) inhibitors and beta-blockers after an MI. Furthermore, prevention efforts, such as healthy eating or exercise programs, are less likely to be recommended to women of color.
MI symptoms
Many women aren’t aware that their MI symptoms may be different from those of men. For example, women may have prodromal symptoms for up to a year prior to a cardiac event. (See Prodromal symptoms.) Researchers believe that men develop blockages in their main cardiac arteries but that women develop blockages in the main arteries as well as smaller cardiac arteries (coronary microvascular disease), resulting in different MI symptoms. Chest pain is still the number one symptom of MI in women, but it’s not the “elephant sitting on your chest” type of pain frequently experienced by men; instead, women feel it as pressure or discomfort. (See MI symptoms.) Women’s symptoms are vague and easy to miss, by both women and healthcare providers.
Several factors contribute to women’s higher MI morbidity and mortality rates. Women (and some healthcare providers) may believe that CVD is a “man’s disease,” so they ignore symptoms and delay seeking treatment. In some cases, they delay going to the ED up to 2 hours longer than men; women of color delay going to the hospital longer than white women. Although women’s awareness of CVD risk has improved, a knowledge gap still exists, and it’s even larger for women of color and those who live in rural areas.


AHA guidelines
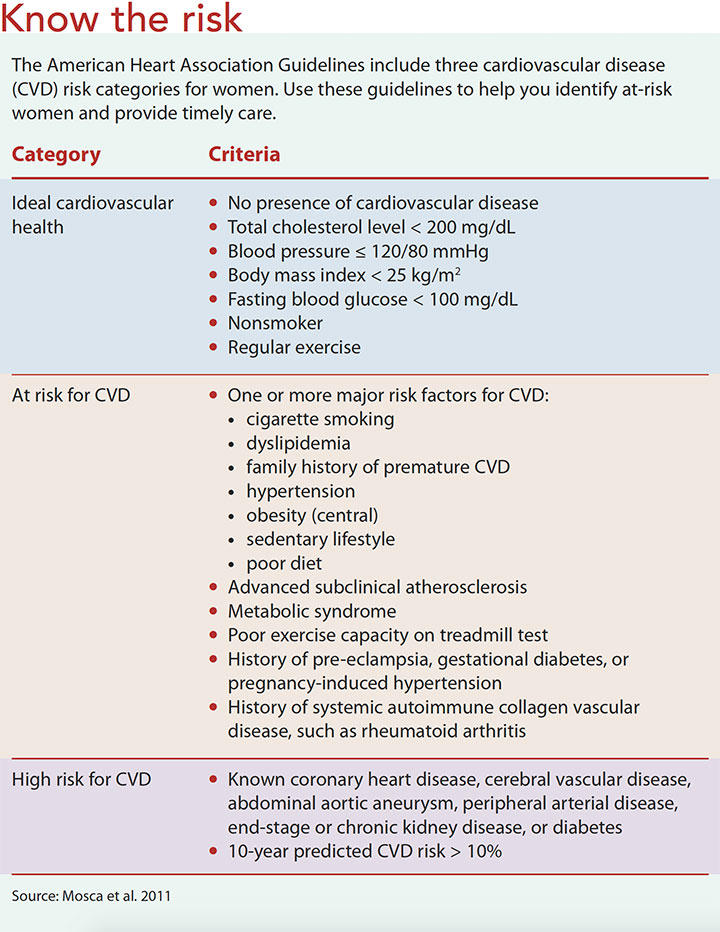
The 2011 updated AHA guidelines for the prevention of heart disease in women identify three risk levels: ideal cardiovascular health, at risk, and high risk. (See Know the risk.) Women who have ideal cardiovascular health have no presence of CVD, total cholesterol level < 200 mg/dL, blood pressure ≤ 120/80 mmHg, body mass index < 25 kg/m2, and fasting blood glucose < 100 mg/dL. At-risk women have one or more major risk factor for CVD—cigarette smoking, dyslipidemia, family history of premature CVD, hypertension, obesity, and a sedentary lifestyle. Other women deemed to be at risk are those with a history of pre-eclampsia, gestational diabetes, pregnancy-induced hypertension, or systemic autoimmune collagen vascular diseases (such as rheumatoid arthritis). Women designated as high risk have known coronary heart disease, cerebral vascular disease, abdominal aortic aneurysm, peripheral vascular disease, end-stage or chronic kidney disease, diabetes, or a 10-year predicted CVD risk ≥ 10%.
The gold standard of treatment and risk reduction for all women, regardless of their risk category, is adhering to a healthy lifestyle, including diet, exercise, adequate sleep, stress reduction, and smoking cessation.
Diet
Let your patients know that the ideal diet consists primarily of whole grains, vegetables, fruits, and protein sources low in saturated fats, such as lean meats and tofu. The AHA recommends no more than 6% of daily calories (about 13 grams) should come from saturated fats found in foods such as red meat, chicken with the skin, cheese, and butter, and that processed breads and baked goods made with refined flour and sugar should be avoided.
The AHA supports the Dietary Approaches to Stop Hypertension (DASH) eating plan for weight loss and hypertension control. Reading food labels can help people reduce sodium, sugar, and saturated fat consumption because it might reveal, for example, that something like a “healthy soup” is actually high in all three. The DASH plan recommends eating no more than 2,400 mg of sodium per day. In general, processed foods such as deli meats, canned soups, and frozen meals are very high in sodium and should be avoided.
Exercise
According to the U.S. Department of Health and Human Services (DHHS) Physical Activity Guidelines for Americans, women should strive for a minimum of 150 minutes per week of moderate-intensity exercise, such as brisk walking. These guidelines are in DHHS’s review process; an update may be available at the end of 2018. The AHA guidelines recommend 150 minutes per week of moderate exercise or 75 minutes per week of vigorous exercise. Examples of vigorous-intensity exercise include running, fast cycling, fast swimming, and heavy shoveling or digging. Two days per week of muscle-strengthening activities that involve all major muscle groups offer additional cardiovascular benefit. For weight loss, women should participate in at least 60 to 90 minutes of moderate-intensity physical activity—such as brisk walking, dancing, house cleaning, and gardening—on most days of the week.
Adequate sleep
The American Academy of Sleep Medicine and the Sleep Research Society recommend that healthy adults sleep 7 or more hours per night. Recommend that your patients go to bed and get up at the same time every day; remove electronic devices from the bedroom; avoid alcohol, caffeine, and large meals before bedtime; and get regular exercise.
Stress reduction
Reducing stress can be challenging for many women. Suggest that patients try meditation, yoga, listening to music, and walking. For success, stress-reduction plans should be individualized; for example, walking a dog might relieve stress in one person but be stress-inducing in another.
Smoking cessation
Cigarette smoking is contraindicated for a heart-healthy lifestyle. If your patient smokes, help her develop a cessation plan. Start by establishing her readiness to quit. Until she says she’s ready to quit, provide education that outlines the risks associated with smoking. Then, when she’s ready, work with her to develop a plan and direct her to supportive resources, including the “Create my quit plan” tool and “Smokefree Women”. The latter site has tools such as text messages (including ones specific for pregnant women), mobile apps, and a craving journal.

AHA guidelines and medication
The AHA guidelines suggest adding medications when lifestyle interventions alone fail to achieve optimal blood pressure, glycosylated hemoglobin (A1C), and low-density lipoprotein (LDL) cholesterol levels. The patient’s provider should consider prescribing medications when blood pressure is ≥ 140/90 mmHg for most women or ≥ 130/80 mmHg for those with diabetes or chronic kidney disease. The guidelines recommend including a thiazide diuretic medication unless contraindicated. If women are at high risk, treatment also should include a beta-blocker, an ACE inhibitor, or an angiotensin II receptor blocker. The guidelines also recommend LDL-lowering medications such as statins for women with diabetes whose A1C levels are < 7%, at-risk women whose LDL is < 130 mg/dL, high-risk women whose LDL is < 100 mg/dL, and in some high-risk women whose LDL is < 70 mg/dL.
For most women who’ve had a cardiac event, angiotensin II receptor blockers, beta-blockers, and spironolactone should be prescribed. Avoid aspirin therapy in women younger than 65 years old with ideal cardiovascular health because of bleeding risk; however, it should be considered in high-risk women and in those over 65 years old when their blood pressure is controlled and the benefit of stroke and MI prevention outweighs the risk of bleeding. The AHA guidelines also recommend treating women who have atrial fibrillation with aspirin, warfarin, or dabigatran. Postmenopausal hormone therapy and antioxidant and folic acid supplements are class-three interventions that aren’t useful or effective and may even be harmful.
Nursing implications
Many cardiovascular health disparities exist related to race, ethnicity, and gender, particularly among Black and Hispanic women. Culturally sensitive care and education about CVD risk factors and MI symptoms enhance patient adherence to prescribed treatment plans.
When discussing healthy lifestyle changes, assess patients’ change readiness and what’s important to them by using motivational interviewing techniques. Develop individualized care plans, offering patients options for maintaining their health. For example, logging food intake and daily exercise may work best for some patients, while others may prefer using smartphone apps to encourage adherence to treatment plans and medication regimens. Research is needed to determine the effectiveness of these apps.
For those who are interested in support groups, provide resources and information. Also, direct women to the Go Red for Women website to learn more about heart disease, discover ways to live healthy, and participate in activities to spread the word about women and heart disease.
Despite education, patients don’t always follow treatment plans. When that happens, explore possible reasons, such as lack of access to primary care providers, time constraints, and resistance to lifestyle modifications. Be nonjudgmental when exploring these reasons, and collaborate with the patient to revise the treatment plan.
Risk reduction begins with education
Education is the cornerstone to reducing CVD risk and death among women. Remind your female patients of the MI symptoms unique to women, and explain that they should seek immediate medical care if they experience any of them.
To ensure early identification and treatment of women at risk for a cardiovascular event, all healthcare professionals should adhere to the AHA guidelines for all female patients regardless of race or ethnicity and provide culturally sensitive care. Empower at-risk women to make wise lifestyle choices, and support and encourage adherence to prescribed treatment plans.
Melanie Kalman is a professor in the college of nursing at Upstate Medical University in Syracuse, New York. Margaret Wells is a professor and nursing department chair at Le Moyne College in Syracuse, New York.
Selected references
American Heart Association. Heart and stroke statistics. 2018.
Barfield WL, Boyce CA. Sex, ethnicity, and CVD among women of African descent: An approach for the new era of genomic research. Glob Heart. 2017;12(2):69-71.
Dracup K, Moser DK, Pelter MM, et al. Rural patients’ knowledge about heart failure. J Cardiovasc Nurs. 2014;29(5):423-8.
Ladwig KH, Fang X, Wolf K, et al. Comparison of delay times between symptom onset of an acute ST-elevation myocardial infarction and hospital arrival in men and women <65 years versus ≥ 65 years of age: Findings from the Multicenter Munich Examination of Delay in Patients Experiencing Acute Myocardial Infarction (MEDEA) Study. Am J Cardiol. 2017;120(12):2128-34.
Mayo Clinic. Heart disease in women: Understand symptoms and risk factors. 2018.
Mehta LS, Beckie TM, DeVon HA, et al. Acute myocardial infarction in women: A scientific statement from the American Heart Association. Circulation. 2016;133(9):916-47.
Mosca L, Hammond G, Mochari-Greenberger H, et al. Fifteen-year trends in awareness of heart disease in women: Results of a 2012 American Heart Association national survey. Circulation. 2013;127(11):1254-63.
Mosca L, Benjamin EJ, Berra K, et al. Effectiveness-based guidelines for the prevention of cardiovascular disease in women—2011 update: A guideline from the American Heart Association. Circulation. 2011;123(11):1243-62.
Office of Disease Prevention and Health Promotion. Physical activity guidelines for Americans. 2008.
Schub T, Pravikoff D. 2016. Acute myocardial infarction in women. CINAHL Nursing Guide.
Wenger NK. Juggling multiple guidelines: A woman’s heart in the balance.
J Womens Health. 2016;25(3):213-21.
ant6-CE Cardio-515




















2 Comments.
Wow, I had no idea that more women have cardiovascular disease than men and is the leading cause of mortality. I just had my second child and with the weight gain, I’m noticing I’m having a lot of issues chasing my son around with the baby, so I’ve been considering working out. Thank you so much for the information about how I need to have 150 minutes of exercise per week to maintain good heart health.
The authors reviewed women and heart disease: risk factors, lifestyle changes, differences in presentation versus male counterparts, and pharmacologic intervention as recommended by the AHA guidelines.
A “Patient Story” helped highlight the recommendations as the patient experienced a non-STEMI for which she had a stent placed followed by recovery in the CCU. Unfortunately, there was no mention of the use of dual anti-platelet medications to manage acute coronary syndrome following stent placement. The 2016 AHA guidelines1 focus on the use of dual anti-platelet agents (aspirin plus P2Y12 inhibitor therapy) and emphasize the importance of appropriate pharmacologic agents with long-term follow up. The data are based on landmark trials that demonstrated statistically significant reduction in the occurrence of recurrence of culprit or non-culprit lesions. In the case, follow up medications with anti-hypertensives, statins, and ASA was stressed, but the use of dual anti-platelet therapy with a P2Y12 inhibitor was omitted. Nursing can have a major role in reminding patients to continue the use of long-term medication management to offer sustained risk reduction, and the authors missed a great opportunity in the case review to make that special point.
Sincerely,
Meenakshi Tomer, MS, CRNP,
1-Levine GN, Bates ER, Bittl JA, et al. 2016 ACC/AHA Guideline Focused Update on Duration of Dual Antiplatelet Therapy in Patients with Coronary Artery Disease. Circulation. 2016; 134: e123-e155.