Learn how to foster patient empowerment, engagement, and activation.
All clinical nurses strive to provide person-centered care (PCC) that meets the patient’s and family’s preferences and needs. (In this article, family is defined as the patient’s preferred support people). More than simply individualizing care, PCC should empower and engage patients so that they’re activated (ready) for discharge and can manage their health. New evidence emphasizes the significance of patient empowerment and engagement models of care as the new standard for PCC to ensure optimal patient outcomes.
Rather than patient-dependent care (adhering to medical advice, prescriptive care, and medications), patients and families should be fully engaged in medical care decisions and activities. This engagement is particularly important in telemedicine and when using eHealth technology, which is rapidly becoming common in the current, and hopefully post, pandemic environment.


Self-reflection on patient engagement
Before you can promote patient engagement, you must determine your own values about it. Some nurses haven’t been taught this specific content, and depending on experience, each nurse will have a different perspective. The power dynamic in healthcare has traditionally been paternalistic, where we (the providers) know best. Patients haven’t always spoken up about their health, preferences, and values. However, recent patient-led PCC initiatives have encouraged patients to consider “nothing about me without me.”
Take a moment to ask yourself these questions to determine your personal beliefs about patient and family engagement:
- What were the norms and beliefs I had about health when I was growing up?
- Do I believe patients are capable of managing their own care?
- Do I manage my own care, or do I defer to the provider?
- Do I see involving patients and their families in decision making as a burden or as an opportunity?
- What are the benefits I’ve experienced when involving patients in making decisions about their own care?
- Is it okay for a patient not to be empowered, engaged, or activated?
Now that you’ve identified your beliefs about engagement, review the benefits of empowerment, engagement, and activation.
Empowered patients
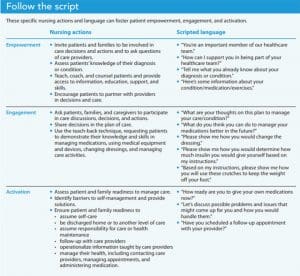
Empowering patients requires explicitly inviting them and their families to participate in all discussions, decisions, and care processes. Nurses can create a relationship and environment for instruction, education, and inclusion in decision making by providing patients with key facts about their condition or situation and continuously building their self-management skills. Empowered patients are goal-oriented. They say, “I’m part of the healthcare team.” Providers who empower patients say, “You’re an important member of our healthcare team.”
Specific nursing interventions that promote empowerment include assessing the patient’s current level of knowledge about their health status, evaluating for potential barriers to empowerment, explicitly telling the patient and family that their questions and input are valued and expected, providing education and information specific to the patient’s level of health literacy, helping patients build self-awareness, and understanding behavior patterns to improve confidence and competence in self-management. At this stage, ask patients what they already know about their condition or diagnosis, ask how you can help them be a part of the healthcare team, and encourage their input. (See Follow the script.)
Engaged patients
Engagement requires that nurses include patients and families in all discussions about treatment plans, medications, and discharge plans. For example, ask patients what they think about the care plan or how they think they can better manage medications in the future.
Nursing interventions that foster engagement include using teach-back methods to ensure a patient’s level of knowledge, attitude, or skill in managing medications, treatments, or self-care protocols and advocating for patients and families to be included in rounding and discharge planning. In addition, nurses should continually evaluate patient engagement with care decisions and activities and remove any barriers. For example, ask them to demonstrate changing a dressing, using crutches properly, or calculating an insulin dosage. These demonstrations will provide information about how activated (ready) they are to assume self-care.
Activated patients
Help patients and families take action to manage their health, assist them in maintaining behaviors and stretching further so they can anticipate what’s next in their health journey, and support them in taking charge of medication, treatment, diet, and exercise plans. Fully activated patients know who to call for appointments or emergencies. Encourage patients to be their own advocates.
Specific nursing interventions related to activation include validating that the patient and family have the necessary knowledge, attitude, and skills to manage their health at home, confirming that they feel ready for discharge, addressing perceptions of readiness, preventing relapse or readmission, and handling new or challenging situations as they arise.
Problem solving and planning for difficult situations help patients maintain their self-care behaviors. For example, ask how they feel about going home and if they’re ready to administer their own medications. In addition, discuss potential problems they may encounter and how to tackle them.
Barriers and perceptions
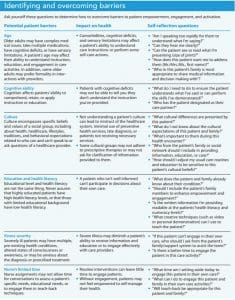
Although it’s relatively easy for nurses to integrate empowerment, engagement, and activation into their usual care routine, some barriers may block full implementation. The patient’s age, cognitive ability, culture, education, health literacy, and illness severity, as well as nurse time limitations, may interfere with empowerment and engagement and negatively affect patient activation. (See Identifying and overcoming barriers.)
Consider using Stichler and Pelletier’s 21-item survey to measure a patient’s and family’s levels of empowerment, engagement, and activation. It can help you determine the patient’s readiness for discharge from the hospital and identify gaps in knowledge or skill that may need to be reinforced before discharge.
Engage patients, improve outcomes
With empowerment and engagement, you can ensure that patients have the knowledge and skills they need to manage their health and care at home. Studies have demonstrated improved patient, provider, and organizational outcomes as a result of empowering and engaging patients and their families. Improvements have been documented in satisfaction levels with inpatient care, decreased costs and lengths of stay, decreased re-admissions, better adherence to provider prescriptions and instructions, and greater ability to perform self-care. Clinical nurses also report feeling more professional satisfaction with the structure and processes of empowerment and engagement and witnessing the outcome of patients who are better prepared for self-care.
The authors work at Sharp HealthCare Caster Institute for Nursing Excellence in San Diego, California. Luc R. Pelletier is a clinical nurse specialist. Jaynelle F. Stichler is a consultant in research and professional development, professor emerita at San Diego State University, and founding co-editor of HERD: Health Environments Research & Design Journal.
References
Agha AZ, Werner RM, Keddem S, Huseman TL, Long JA, Shea JA. Improving patient-centered care: How clinical staff overcame barriers to patient engagement at the VHA. Med Care. 2018;56(12):1009-17. doi: 10.1097/MLR.0000000000001007
Daruwalla Z, Thakkar V, Aggarwal M, Kiasatdolatabadi A, Guergachi A, Keshavjee K. Patient empowerment: The role of technology. Stud Health Technol Inform. 2019;257:70-4.
Elliott J, McNeil H, Ashbourne J, Huson K, Boscart V, Stolee P. Engaging older adults in health care decision-making: A realist synthesis. Patient. 2016;9(5):383-93. doi: 10.1007/s40271-016-0168-x
Hawley ST. Cultural challenges to engaging patients and shared decision making. Agency for Healthcare Research and Quality. September 17, 2015. effectivehealthcare.ahrq.gov/sites/default/files/hawley-presentation.pdf
Heath S. What are facilitators and barriers to older patient portal use? Patient Engagement Hit. October 24, 2017. patientengagementhit.com/news/what-are-facilitators-and-barriers-to-older-patient-portal-use
Náfrádi L, Nakamoto K, Schulz PJ. Is patient empowerment the key to promote adherence? A systematic review of the relationship between self-efficacy, health locus of control and medication adherence. PLoS One. 2017;12(10):e0186458. doi: 10.1371/journal.pone.0186458
Parnell TA, Stichler JF, Barton AJ, Loan LA, Boyle DK, Allen PE. A concept analysis of health literacy. Nurs Forum. 2019;54(3):315-27. doi: 10.1111/nuf.12331
Pekonen A, Eloranta S, Stolt M, Virolainen P, Leino-Kilpi H. Measuring patient empowerment—A systematic review. Patient Educ Counsel. 2020;103(4):777-87. doi: 10.1016/j.pec.2019.10.019
Pelletier LR, Stichler JF. Ensuring patient and family engagement: A professional nurse’s toolkit. J Nurs Care Qual. 2014;29(2):110-14. doi: 10.1097/NCQ.0000000000000046
Pelletier LR, Stichler JF. Patient-centered care and engagement: Nurse leaders’ imperative for health reform. J Nurs Adm. 2014;44(9):473-80. doi: 10.1097/NNA.0000000000000102
Risling T, Martinez J, Young J, Thorp-Froslie N. Evaluating patient empowerment in association with eHealth technology: Scoping review. J Med Internet Res. 2017;19(9):e329. doi: 10.2196/jmir.7809
Stichler JF, Pelletier LR. Psychometric testing of a patient empowerment, engagement, and activation survey. J Nurs Care Qual. 2020;35(4):E49-57. doi: 10.1097/NCQ.0000000000000452
Yeh MY, Wu SC, Tung TH. The relation between patient education, patient empowerment and patient satisfaction: A cross-sectional-comparison study. Appl Nurs Res. 2018;39:11-7. doi: 10.1016/j.apnr.2017.10.008