Learn what more than 4,000 nurses from across the country are saying about important issues—from bullying to COVID-19 to salary.

Survey highlights
- Of the respondents, 85% say the COVID-19 pandemic hasn’t changed their career plans.
- More than half of respondents (55%) report salary increases in the past 12 months, and 61% received a raise within the past year.
- More than half of respondents (56%) report an increased workload in the past 12 months (compared to 60% in 2019).
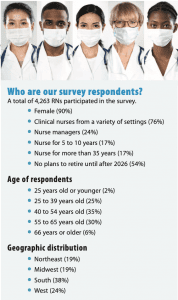
- A total of 4,263 RNs responded to the survey.
COVID-19 and the nursing workforce
Little national data exist that measure how the COVID-19 pandemic may affect the nursing shortage. According to the Nursing Trends and Salary Survey, 85% of respondents say the pandemic hasn’t changed their career plans, 11% plan to change their job or specialty, and 2% plan to leave nursing. In light of COVID-19, this may sound like good news; however, with nearly 3 million employed RNs across the country, even 2% is a big loss. The survey also found that one-third (33%) of those changing jobs or leaving nursing are from the south, including states hardest hit by the pandemic, such as Florida and Texas.
More than two-thirds (69%) of respondents say they’re satisfied with their employer’s response to COVID-19, with 23% being totally satisfied. More than half (58%) say their organization is well prepared or extremely prepared to handle a surge in patients from a pandemic, natural disaster, or other reason for a sudden influx of patients. However, that means over 40% don’t think their organization is prepared.
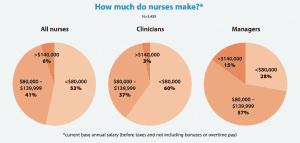
Pay and perks
Of the respondents, 41% earn $80,000 to $139,999 per year. This includes 37% of clinicians and 57% of managers. More than half (55%) of respondents reported a salary increase in the past 12 months, down from 62% in 2019.
A total of 69% of respondents said they’re satisfied with their salary/compensation, and 75% report satisfaction with benefits provided by their organizations. A full 87% of respondents receive paid time off, including sick time and vacation.
Top benefits include:
- Paid time off 85%
- Health insurance 82%
- Dental insurance 78%
- Retirement contributions 74%
- Vision insurance 68%
- Education funds 49%
Survey respondents left a total of 1,464 comments about how the pandemic is affecting them and their practice. Here’s a sampling.
• “I am more committed than ever to nursing…”
• “…the stress of working during the pandemic has strengthened the bonds of our team.”
• “The lack of visitors has been tough on patients who need moral support.”
• “Nurses don’t jump ship…”
• “It is fascinating to work in the time of a novel virus.”
• “A lot of nurses and doctors were put at a high risk because of lack of supplies.”
• “My hospital was very supportive of nursing staff and provided adequate training and PPE.”
• “There is much bullying and negativity for those unable to care for COVID patients due to physical limitations, i.e., age, im- munocompromised, pregnant.”
• “…there will be long-term effects of the stress and trauma that will affect the profession for years to come.”
• “It is redefining healthcare as we know it. My hope is that nurs- es’ voices will be heard and honored…”
Turnover and recruiting
Recruiting RNs has improved slightly. In 2019, 64% of manager respondents said recruitment had become more difficult in the previous 12 months. That number dropped to 59% in this year’s survey. However, 45% of manager respondents report an increase in open positions in the past 12 months, and 50% say RN turnover has increased during that same period. According to manager respondents, the most in-demand specialties are critical care and ED.
Here’s some insight into nurses and length of employment.
- Many respondents (78%) aren’t currently seeking another employer in the next 3 months.
- Less than half (42%) plan to stay with their current employer for 5 years or more.
- More than half (52%) have worked for their current employer for 5 years or less.

What turns a nurse’s head toward another employer?
Most respondents (84%) are satisfied with their current job, but higher pay and an improved setting are the top reasons nurses would accept another position. Survey respondents who aren’t currently looking for another employer were asked to choose up to three options that would make them change jobs. Money was the most common choice (62.5%). Almost one-third (31%) say they would change for a different type of job/more meaningful work, and 30% say they would make a change for a more positive work environment. On a possibly related note, more than half (56%) of respondents report that their workload has increased in the past 12 months.
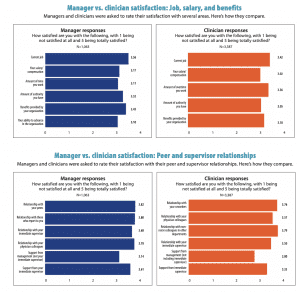
Job satisfaction
Satisfaction with current job, salary/compensation, benefits, and amount of authority were fairly comparable between clinicians and managers. Both groups also reported fairly high satisfaction with peer and supervisor relationships.
Insights from nurse managers
The nursing manager population is a mature one. Almost half (46%) of manager respondents are over 55 years old, and 40% are 40 to 54 years old.
One-fifth (20%) of manager respondents work in a community hospital, and 42% serve on a value-based purchasing committee or make purchasing decisions. Only 18% are certified in nursing leadership, which is similar to 2019. Among those certified, the most common certifications are the two available through the American Nurses Credentialing Center (Nurse Executive-Board Certified and Nurse Executive Advanced-Board Certified).
Primary role
• Director/assistant director 23%
• Unit/department manager 22%
• Charge nurse 12%
• Other 28%
Number of employees supervised
•<5 24%
• 6-10 18%
• 11-20 19%
• > 50 18%
Hours worked in a typical week
• 40 to 45 41%
• 46 to 50 20%
Key manager insights:
- Most report increased workload in the past 12 months (77%).
- Managers are least satisfied with advancement opportunities in the organization (32% rank this
1 or 2 vs. 3 or above, which indicates some level of satisfaction) and amount of time worked (31% rank this as 1 or 2).
- One-third of managers are totally satisfied (5 ranking) with the relationship they have with their immediate supervisor (35%) and support from that supervisor (35%).

Clinical nurse perspectives
More than one-third (35%) of clinical nurses are over age 55, and 34% are between ages 40 and 54. Only 3% of them are less than 25 years old.
Many respondents work in teaching hospitals (27%), followed by community hospitals (23%) and academic medical centers (15%). Certification among clinical nurses is growing, and 42% are certified in their specialty compared to 35% in 2019. Most (83%) have a bachelor’s degree or higher, and 65% aren’t seeking or planning to seek another degree in the next 6 months.
Key clinical nurse insights:
- Half report increased workload in the past 12 months.
- A third (33%) said assignments are not appropriate to meet patient needs at least 80% of the time.
- Nearly half (47%) of organizations don’t have a staffing committee.
- Clinicians are least satisfied with support from management other than immediate supervisor (42%).
- Clinicians were most satisfied with their relationships with coworkers, with 87% ranking this 3 or above.
Roles and specialties
- Acute care (60.5%) (unchanged from 2019)
- Clinical/staff nurses (62%)
- Advanced practice RNs (APRNs) (8%)
- NPs (of those who are APRNs) (78%)
Hours worked in a typical week
- Regular 12-hour shifts (47%)
- No overtime or >1 hour of overtime a week (54%)
- Overtime 1 to 3 hours a week (22%)
- Overtime 4 or more hours a week (24%)
Workplace violence
This year, we asked for more details about workplace violence occurrences in the past 2 years, including why an incident wasn’t reported, the type of report filed, and satisfaction with follow-up.
Bullying and violence among coworkers
Nearly four in ten (39%) of respondents report having been verbally assaulted by another employee or healthcare provider, up slightly from 35% in 2019. In 2020, 42% of managers and 38% of clinical nurses reported they had been verbally assaulted by a healthcare provider.
Almost one-fifth (18%) had been verbally assaulted or bullied by their manager.
About half of respondents (46%) say they intervened when they witnessed workplace bullying. Only 8% didn’t intervene (46% didn’t witness bullying during that time). Many (38%) reported the incident verbally. Of those who reported, only 27% were satisfied with how the situation was handled. One possible explanation for this low number may be that managers aren’t always able to share specific interventions with staff.
Managers were more likely than clinical nurses to complete both verbal and written reports. The most common reasons for not reporting were the belief that nothing would be done about the situation (44%) and fear of reprisal (39%). Managers were more likely to fear reprisal than clinical nurses.
The survey also found that less than 2% of respondents had been physically assaulted by another employee or healthcare provider. Less than one in ten (8%) reported experiencing sexual harassment, and 58% of those didn’t report the incident.
Survey respondents left a total of 1,323 comments about these contentious issues. Here’s a sampling.
- “Over the years, I’ve seen a big improvement in the way nurses are treated by physicians and coworkers. The general public is still a problem.”
- “Too many times managers and supervisors try to give the benefit of doubt to the bully.”
- “Nurses in my organization are being empowered to speak up about bullying… It’s not being tolerated anymore.”
- “I’m tired of reporting the incidents because management doesn’t do anything about it.”
- “It gets swept under the rug like it is an expected part of the job.”
- “I am gay and have been verbally abused and threatened by other employees. I have witnessed a patient being verbally abused because of their sexual orientation. I reported the incidents to immediate supervisors. Virtually nothing was done.”
- “Don’t be a silent victim. Silence will affect the quality of your practice.”
- “Nurses do not feel empowered or protected to report peer-peer violence.”
- “The adage ‘the customer is always right’ seems to count first and foremost over the safety and regard for nurses.”
Bullying and violence from patients and their families
Bullying and violence from patients and family members continues to be an issue. In 2019, 59% of respondents reported having been verbally assaulted by a patient. This year, 54% of respondents say they were verbally assaulted or bullied by a patient. Many (40%) reported the incident verbally.
The most common reasons for not reporting the incident were the belief that the incident wasn’t serious enough to report (51%) and that nothing would be done about the situation (40%). Of those who reported, only 56% were satisfied with how the situation was handled.
More than one-third (36%) of respondents say they had been verbally assaulted or bullied by a patient’s family member or visitor. Most (45%) reported the incident verbally.
Almost two in ten respondents (18%) report having been physically assaulted by a patient. Most (47%) made a verbal and written report, with 30% making only a verbal report. The most common reasons for not reporting were the belief that the incident wasn’t serious enough to report (50%) and that nothing would be done about the situation (40%). Of those who reported, only 48% were satisfied with how the situation was handled.
The survey also reveals that organizations are working to address these issues. Most respondents (78%) say their organizations have been supportive in reducing workplace violence. More than three-quarters (77%) have received or arranged for training in how to de-escalate patients, family members, or visitors who become agitated. Of those who have had training, 85% find the training helpful and 71% have applied the training in practice.
Respondents were asked to pick three aspects of nursing that are most important to them. The most popular responses were the following*:
• Salary (69%, down from 70% in 2019)
• Providing patient care (67%, up from 63% in 2019)
• Opportunity for career growth (51%, down from 54% in 2019)
• Flexible hours (50%, down from 53% in 2019)
Nurses added 215 additional responses, addressing such issues as patient and staff safety, having a voice and being heard, working at the top of scope of practice, feeling appreciated/valued, work-life balance, job security, opportunity to learn, and job satisfaction.
N=2,608
Catherine Spader is an author and healthcare writer/editor based in Littleton, Colorado.




















7 Comments.
When unit leadership does not have relevant degree or clinical experience and they are not on unit but make decisions is very frustrating. When staffing is not adequate, manager doesn’t understand the low amount of available staff affects patients, their care and safety of pts and staff. I work in Psychiatry and it’s an unpredictable environment.
It is leadership in some places who are involved or perpetrators of bullying. When you work in an environment where the color of your skin and your primary language becomes a liability, bullying by leadership is common. In the environment I work in, English speaking is a liability. The color of my skin ia a liability. Speaking up about how things are done and how they can be done better make me a target of leadership bullying. It is sad and really where do you turn for help in a culture where this is acceptable. HR says to speak with the unit director and the director defends leadership. Leadership then continues the bullying because in South Florida one of the prerequisite for a RN in this hospital to treated fairly requires the RN to be fluent in a specific language which is NOT English,
We have the same problem on California! Communication with non English speaking nurses (and some MDs) is so difficult and frustrating. This effects patient care.
Thank you for this overview of what’s important to nurses and the impact of bullying/violence in the workplace. The salary ranges were a surprise. I thought nurses were making more money than what you reported.
Speaking as an NP working from home, COVID has not changed my career plans. I don’t think it has affected my pay or perks, but I do have an increased workload, which may not directly result from COVID. However, somebody should survey nurses and NPs separately since the two jobs are not the same. As a nurse, I am sure being overworked, underpaid, understaffed, and underappreciated are still a reality, and likely more so due to COVID-19. I have rarely been bullied as an NP, but all too often as a practicing RN. I am very thankful to all the nurses who choose to remain at the beside. Thank you for all you do! I hope that 2021 improves all these critical areas mentioned, boosts your well-deserved salaries, and brings zero tolerance for bullying.
Too often we get all this information but no real answers.
Very informative. TY!! It would be helpful to know the areas of the country for the survey results especially for salary concerns.