Key takeaways
|
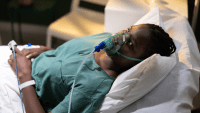
After a car accident, Robert arrives at the emergency department with multiple traumatic orthopedic injuries, including painful rib factures. He tells you he was recently released from an inpatient treatment center for heroin addiction and is being treated with buprenorphine/naloxone. Robert’s rib fracture pain, which is difficult to control, interferes with his breathing. In the context of Robert’s maintenance therapy for opioid addiction, what do you do for his acute pain?
Opiate abuse and addiction is a growing epidemic in the United States. Medications like methadone or buprenorphine combined with naloxone are used as maintenance therapy to address this epidemic. Researchers have investigated how these medications affect pain control in the perioperative period for planned procedures, but there’s little data for the treatment of acute unplanned pain like that experienced by Robert.
This article addresses the inpatient treatment of acute traumatic pain in patients receiving the most common opioid maintenance treatments—methadone or buprenorphine combined with naloxone.
Patients’ rights in pain management
A joint statement from the American College of Emergency Physicians, American Pain Society, American Society for Pain Management Nursing, and the Emergency Nurses Association asserts that all patients need to be treated appropriately for pain, including those with addictive disease.
Without treatment, pain may result in tachycardia, hypertension, and increased myocardial demand, along with decreases in lung volumes, cough, gastric emptying, and bowel motility. Untreated pain also can lead to muscle spasm, impaired muscle mobility and function, as well as anxiety and fear. In trauma patients with multiple injuries, like Robert, any of these added insults can delay recovery.
While treating Robert, keep in mind that that he’ll continue to struggle with his underlying chronic pain throughout the acute pain event. In fact, most patients receiving maintenance therapy for opioid addiction are opioid tolerant after just 1 week, so address baseline opiate requirements to prevent complete withdrawal and provide adequate analgesia. Work closely with Robert’s outpatient prescriber to identify his dosing and current treatment plan. This not only will help to manage his acute pain, but also will help with the transition back to maintenance therapy.
For more on treatment programs, see the infographic.
Special considerations for chronic opioid therapy
While methadone is indicated for pain management, it’s more widely prescribed to prevent opioid withdrawal symptoms and can be safely continued during acute pain treatment with other therapies and appropriate monitoring.
Methadone’s long half-life and slow elimination from the liver creates a risk of interacting with other drugs long after the analgesic effects of 4 to 6 hours have worn off. Any drugs that inhibit CYP450 metabolism will decrease the clearance of methadone and increase risk of respiratory depression. Monitor your patient’s corrected QT interval (QTc) for prolongation, which can be exacerbated when methadone is given with haloperidol, diazepam, ciprofloxacin, droperidol, levofloxacin, or moxifloxacin. Maintain normal magnesium and potassium levels with supplements to help avoid cardiac arrhythmias while using methadone.
The combination of buprenorphine and naloxone is not indicated for use as a pain medication. Naloxone, which is added to bu prenorphine to deter abuse of the drug, has poor oral bioavailability, but it’s highly available when administered intravenously. So if someone attempted to crush and inject this combination of buprenorphine and naloxone, the naloxone would negate the effects of the buprenorphine at the opiate receptor.
Initially, baseline doses of buprenorphine and naloxone may need to be reduced for full opiate agonists to take effect and treat acute pain. Buprenorphine and naloxone may displace full agonists, reducing activation of the receptors and precipitating opiate withdrawal. Mild opiate withdrawal may appear as lacrimation, rhinorrhea, yawning, sneezing, coughing, piloerection, restlessness, or tremor.
If your patient experiences withdrawal, continue with acute pain treatment. Both the baseline opiate dosing for addiction treatment and any new opiates prescribed will treat the withdrawal and pain. Determine when the patient took the last dose of buprenorphine and naloxone and closely monitor for oversedation for 72 hours after the last dose, particularly when adding opiates such as hydrocodone or hydromorphone to the pain-control regimen regimen, which can cause respiratory depression. The antagonist included in the buprenorphine and naloxone combination may require higher doses of opioids for adequate pain control but will also wear off sooner, increasing the risk of respiratory depression.
Pain can be treated along different pathways, making multimodal therapy key to addressing acute pain. (See Initiating pain control.)
Tips for multimodal therapy
Treatment using multimodal therapy requires patient education, treatment flexibility, and multidisciplinary collaboration. Keep the following tips in mind to ensure a good outcome for your patient.
• Start education and interdisciplinary coordination immediately and include weaning from opiates for acute pain, instructions for administration, drugs to avoid, and necessary follow-up.
• Use consulting resources such as acute pain services and substance abuse experts early to take full advantage of their knowledge.
• Encourage deep breathing, incentive spirometry, and ambulation to reduce risks of pneumonia and infection.
• Treat the pain appropriately with the right drug. For instance, neuropathic pain is more responsive to a drug like an antiepileptic rather than an opiate.
• When increased pain control is needed, try adding a drug from another class rather than relying on increased dosing from one class. This is particularly relevant when opiate receptors are unavailable to agonists, which might be the case for someone on maintenance therapy.
• Don’t underestimate the value of adjunct therapies such as acu – punc ture, guided imagery, and massage therapy.
Getting the upper hand on pain control
For patients like Robert with acute injuries, using multimodal therapy, while considering individual opiate requirements, history, and response, will gain better pain control that leads to improved outcomes.
Jennifer Yeager is a trauma nurse practitioner at University Hospital, Madison, Wisconsin. Kelly D. Rosenberger is assistant professor and director of the University of Illinois at Chicago College of Nursing– Rockford Campus.
Selected references
Center for Substance Abuse Treatment. Medication-Assisted Treatment for Opioid Addiction in Opioid Treatment Programs. A Treatment Improvement Protocol (TIP) 43. HHS Publication No. (SMA) 12-4214. Rockville, MD: Substance Abuse and Mental Health Services Administration; 2012.
Chapman JLR, Lalkhen AG. Postoperative analgesia. Anaesth Intensive Care Med. 2016;17(3):144-50.
Cheng YJ. Lidocaine skin patch (Lidopat® 5%) is effective in the treatment of traumatic rib fractures: A prospective double-blinded and vehicle-controlled study. Med Princ Pract. 2016;25(1):36-9.
Jensen CD, Stark JT, Jacobson LL, et al. Improved outcomes associated with the liberal use of thoracic epidural analgesia in patients with rib fractures. Pain Med. 2016. [Epub ahead of print.]
Ladha K, Patorno E, Huybrechts KF, et al. Variations in the use of perioperative multimodal analgesic therapy. Anesthesiology. 2016;124(4):837-45.
Vadivelu N, Lumermann L, Zhu R, et al. Pain control in the presence of drug addiction. Curr Pain Headache Rep. 2016;20(5):35.