How nurses can screen, intervene, and provide appropriate referrals.
- Nonsuicidal self-injury is a commonly hidden behavior among adolescents
- Screening in primary care and schools provides optimal opportunities for early intervention.
- Brief interventions, such as motivational interviewing, can increase the motivation for change and the likelihood that adolescents will accept treatment.
You enter the exam room to take vital signs for a 15-year-old boy. When you ask him to remove his jacket to take his blood pressure, you’re shocked to see multiple severe scars on his left arm. When you ask about the scars, he tells you that they’re from tree branches hitting his arms while off-trail bike riding. You notice that the scars are linear and that his right arm has no scarring. You suspect that his injury history isn’t accurate. What’s your next step?
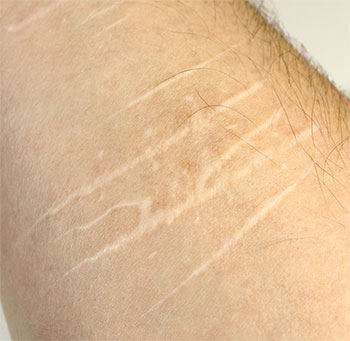

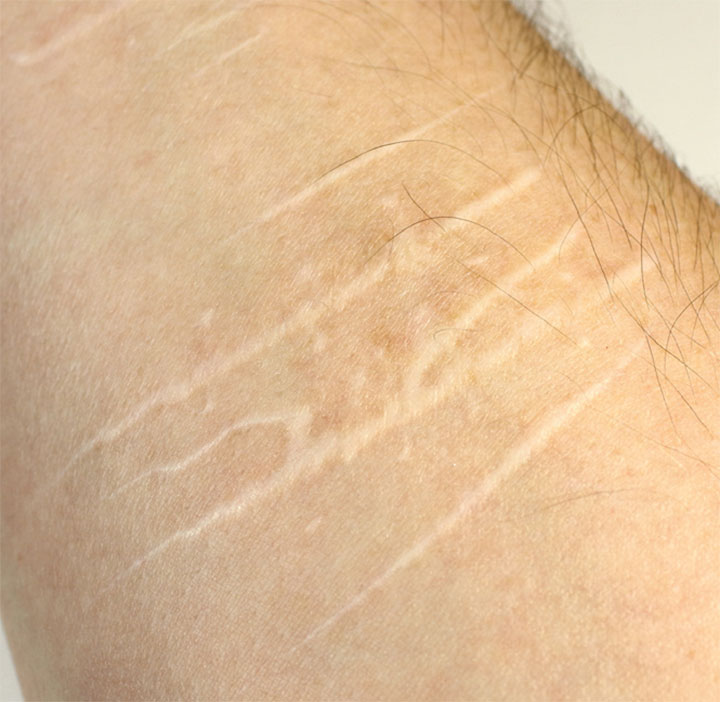
Types of self-injury
Self-injury includes hitting, scratching, cutting, burning, pinching, and inserting objects under the skin. Cutting is the most common self-harm behavior. Injury can appear as hash marks on an arm from objects such as a broken soda can, staples, scissors, and knives. Typically, the individual hides the wounds with long sleeves or jewelry. Some people who self-injure choose locations that aren’t typically seen in public, such as the inner thigh or abdomen. Although cutting is the most common type of self-injury, assessing for other forms, such as bruising from hitting (which is more common in males) is important.
With no intervention or treatment, self-injury usually persists and may increase. A high association exists between self-injury and psychiatric diagnoses such as depression, anxiety, substance use, and borderline personality disorder. Treatment includes addressing the underlying cause and developing new coping strategies, which usually requires referral to a mental healthcare professional.
Levels of severity
Mild forms of tissue damage usually appear as red marks as a result of light scratching, hitting, biting, or self-rubbing. This trauma can fade quickly, making it difficult to see in an exam. Moderate levels that cause deeper tissue damage and bleeding include scratching, repeated scab removal, or cutting that doesn’t requiring suturing. This level of self-injury also includes higher impact hitting or pinching that results in bruising. Severe levels of self-injury cause deeper tissue damage; they include cutting that requires suturing, burning, insertion of objects into the skin, and bone-breaking. Although mild and moderate forms of tissue damage can be hidden from view by clothing and jewelry, severe forms require medical attention.
Risk factors and motivations
Risk factors for nonsuicidal self-injury can be divided into mental disorders, environmental, and personal. (See Know the risks.) In addition, many psychological motivations may be behind nonsuicidal self-injury. Two common motivations are attempts to cope and self-punishment. The patient may have difficulty dealing with stress or working through emotions such as rejection and worry. For example, an adolescent girl who feels “numb” after arguing with her mother may burn herself with a lit cigarette to feel something. Or a young man may bang his head against the wall to punish himself after approaching a girl for a date and being rejected.


Screening, brief intervention, referral
Screening adolescents during outpatient visits will facilitate the identification and treatment of nonsuicidal self-injury. One recommended method is screening, brief intervention, and referral to treatment (SBIRT). This three-step method is designed for use in primary care settings to screen for substance use and abuse, and it also has been used for depression and anxiety. It’s comprehensive, patient-focused, and easy to use, and it has been validated for use in adolescents. Before using this method, you and your colleagues should complete training. (See SBIRT training.)
SBIRT training
| Screening, brief intervention, and referral to treatment (SBIRT) is one approach you can take when you suspect your adolescent patient may be using nonsuicidal self-injury to cope with stress. Before implementing it in your care setting, access these opportunities for training. |
| Course | Website | Format |
|---|---|---|
| SBIRT | samhsa.gov/sbirt | Face-to-face and online |
| Improve clinical skills in SBIRT for substance use problems | sbirttraining.com | Online |
| Ohio Mental Health Addiction Services (MHAS): SBIRT | http://mha.ohio.gov/Treatment/SBIRT | Face-to-face and online |
| Community Catalyst: Training resources for the implementation of screening, brief intervention, and referral to treatment (SBIRT) | communitycatalyst.org/resources/publications/document/SBIRT-Training-Options-December-2015.pdf?1451325946 | Face-to-face and online |
| Institute for Research, Education & Training in Addictions (IRETA): SBIRT for adolescents | ireta.org/improve-practice/addiction-professionals/online-courses/sbirt-for-adolescents/ | Online |
| Adolescent SBIRT curriculum | sbirt.webs.com/curriculum | Online |
| Massachusetts Health Promotion Clearinghouse: Adolescent SBIRT toolkit for providers | massclearinghouse.ehs.state.ma.us/BSASSBIRTPROG/SA1099.html | Booklet |
| Pacific Southwest ARRC eLearning: 4 hour SBIRT training (continuing education) /td> | psattcelearn.org/courses/4hr_sbirt/ | Online |
| SBIRT: A brief clinical training for adolescent providers | http://hospitalsbirt.webs.com/adolescent-providers | Online |
Currently, little research exists for using SBIRT for nonsuicidal self-injury, but some researchers have hypothesized that it’s generalizable to this population because repetitive nonsuicidal self-injury and substance use both induce a desired and potentially addictive feeling. This feeling leads to the pattern of reward and reinforcement that’s fundamental to addictive disorders.
Screening
Screening using a valid, reliable method takes 1 to 5 minutes. It can be done verbally or with a written form completed by the patient or healthcare professional. Studies show that shame and embarrassment often are associated with self-injury, so be sensitive, empathic, and patient. Developmentally, adolescents aren’t yet adults, but they want autonomy. This developmental struggle may cause them to feel awkward or intimated when talking to an adult. In addition, the adolescent may lack the self-awareness or ability to clearly verbalize thoughts and feelings. Silence is common, and gentle probing may be required.
You can verbally screen using either direct or indirect questions. A direct approach may be more appropriate for adolescents around age 17 or if you’ve already built a trusting relationship. Use an indirect approach with younger adolescents. With the direct approach, simply ask, “Do you intentionally cause pain to yourself” or “Do you hurt yourself intentionally to feel pain?” If you need to be indirect, start with a question such as: “I’ve had some people tell me that they bite, hit, or cut themselves when they feel bad or stressed. Has this ever happened to someone you know or maybe to you?” The key is respect and sensitivity.
If you want a more formal screening method, consider using an assessment tool. (See Assessment tools.) When considering one of these tools, keep in mind that some measure type and severity of nonsuicidal self-injury rather than screen for the behavior; make sure you understand the purpose of the tool before using it. Because depression and anxiety can coexist with nonsuicidal self-injury, other screening tools may be useful. Two well-known and reliable tools are the Patient Health Questionnaire-9 for depression and the Generalized Anxiety Disorder-7. They take only a few minutes to complete and are easy to use in busy primary care settings. Permission to use these tools can be obtained at phqscreeners.com/select-screener.
Nonsuicidal self-injury is a risk for suicide, so ask about any suicidal thoughts or past suicide attempts in adolescents who screen positive for this behavior.
Assessment tools
| These assessment tools can help you screen adolescent patients for nonsuicidal self-injury. However, keep in mind that the list is not inclusive and that many tools measure type and severity rather than screen for the behavior. |
Brief intervention
If your screening identifies a patient as positive for nonsuicidal self-injury, immediately provide brief therapy (5 to 30 minutes). Motivational interviewing is one approach widely used in substance abuse treatment. The goal is to motivate the patient to make changes. It consists of three components: collaboration, evocation, and autonomy.
Collaboration uses positive and nonjudgmental communication that encourages the adolescent to express experiences and perspectives about the behavior. For instance, you might say, “It seems that life is very stressful for you right now, and it appears that self-injury is helping you deal with your stress.” These types of statements equalize control so that you and the patient are partners. They also convey a level of understanding and allow the patient to elaborate or correct any misunderstanding about the behavior.
Evocation is the adolescent’s ability to express his or her own motivations to change the behavior. For example, the patient might respond, “Yes, cutting helps me with stress, but my arms look so terrible I can’t go swimming.” This acknowledgement gives you a hint that the patient has a reason to stop the behavior. You may feel the urge to provide education at this point, but resist it. Keep the spirit of motivational intervention by asking permission to provide information about consequences of nonsuicidal self-injury.
Autonomy allows the adolescent to have control over any decisions at that moment. If he or she doesn’t want the information you offer, leave the door open by saying, “I understand you’re not ready for this information. Please come back to see me if you decide you want help.” If the adolescent wants information, this is the moment you can educate compassionately. Continue the momentum by asking permission to discuss a plan for reducing or stopping the behavior. The key here is that the plan is created by the patient, not you. He or she makes a plan, and you encourage the ideas for change. Allowing an adolescent to have a personal choice can improve the motivation to seek help.
For severe levels of self-injury, make a mental health referral.
Referral
Adolescents who’ve reached a moderate or severe level of tissue damage may have trouble stopping or even reducing nonsuicidal self-injury. When the behavior reaches these stages, it becomes addictive and the patient should be referred for intensive therapy.
Your care setting should have a referral process in place to ensure a smooth transition. Note that both parental and adolescent permission may be needed for referrals; check your state laws regarding consent. If required, contact the adolescent’s parent or guardian and discuss the situation, but include the adolescent to maintain a trusting relationship.
Referrals should be made to adolescent psychotherapists (such as psychiatric social workers, advanced practice psychiatric nurses, psychologists, and marriage and family therapists) or adolescent psychiatric providers (adolescent psychiatrists, advanced practice psychiatric nurses, and physician assistants who work with adolescents). These specialized mental healthcare providers are trained in the appropriate approaches for treating adolescents.
Challenges that may prevent patients from following up with mental healthcare professionals include treatment and medication costs, lengthy wait time for an appointment, and transportation limitations. Assess the family’s financial ability to pay so you can make an appropriate referral. Be familiar with services in your area and keep an up-to-date list of clinics and clinicians that offer low-fee and free behavioral health services. They frequently help with the cost of medications and transportation. School guidance counselors and social workers can be helpful referral sources.
Take the opportunity
You have an opportunity to intervene when you suspect your adolescent patient is using nonsuicidal self-injury to cope with stress and other mental health issues. The SBIRT method is one method you can use to assess, intervene, and refer your patients. Your approach requires patience, empathy, and sensitivity to encourage patients to open up so that you can provide the most appropriate treatment.
You ask the 15-year-old patient for permission to share information about scarring. He agrees, and you compassionately explain that in the past you’ve had people with similar scars tell you that they cut themselves when they were feeling stress. Then you ask, “Has this ever happened to someone you know, or could this be something you considered doing?” The patient acknowledges that he’s been cutting himself because he’s not doing well in school. You ask how he feels about this, and he tells you how embarrassing it is if someone notices his scars. He goes on to say that he’s been thinking about putting a tattoo over the scar to cover it up. Building on this discrepancy in the patient’s behavior and his feelings, you ask if he’s willing to see someone to help him find other ways to work through his stress. He says, “Yes, I’m ready to do something about this.”
Kimberly A. Williams is an associate professor at Kent State University College of Nursing in Kent, Ohio. Hannah Monsman and Jara Chadwell are honors students at Kent State University College of Nursing.
Selected references
MASBIRT TTA/Boston Medical Center. SBIRT in schools. 2018.
Nock MK, Favazza AR. Nonsuicidal self-injury: Definition and classification. In Nock MK ed. Understanding Nonsuicidal Self-injury: Origins, Assessment, and Treatment.Washington, DC: American Psychological Association; 2009:9-18.
Polanco-Roman L, Jurska J, Quiñones V, Miranda R. Brooding, reflection, and distraction: Relation to non-suicidal self-injury versus suicide attempts. Arch Suicide Res. 2015; 19(3):350-65.
Saraff PD, Trujillo N., Pepper CM. Functions, consequences, and frequency of non-suicidal self-injury. Psychiatr Q. 2015;86(3):385-93.
Substance Abuse and Mental Health Services Administration (SAMHSA).Screening, Brief Intervention and Referral to Treatment (SBIRT) in Behavioral Healthcare. April 1, 2011.
Substance Abuse and Mental Health Services Administration (SAMHSA), U.S. Department of Health and Human Services (DHHS) Center for Integrated Health Solutions. Motivational interviewing. February 22, 2011.



















1 Comment.
I am responding to an article from August 2018 Vol 13 No. 8 titled “Why do adolescents engage in nonsuicidal self-injury”, by Kimberly A. Williams. As an Emergency Department Nurse, I see many patients a day, and have seen multiple with old or new linear scars as addressed in the article. Being that I am only with my patients briefly before being discharged, I would like to respond in particular to the importance of the “Referral” process. Although referring a patient to a psychotherapist or specialized psychiatric provider are essential, getting an appointment can often take longer than expected, and could potentially end with the patient becoming noncompliant. I would like to propose an outlet that enables troubled adolescents to achieve stress relief while waiting to see a provider: group therapy.
Although self-harm is usually not linked to a patient wanting to end their lives, it is not unheard of, therefore we should treat self-harm just as intensely as we treat suicidal ideation or attempt. The Centre for Suicide Prevention published an article “Self-harm and Suicide” that focuses on the differences, and similarities, of self-harm and suicide. The article states the purpose of self-harm is “done to avoid suicidal impulses” (Klonsky, May, & Glenn, 2014) and goes on to express that eventually the efforts of self-harm are not an effective release for the victim, and that is when things could progress to suicide. According to the goodtherapy.org article “Self-Harm”, group therapy is a good way to allow patients of similar backgrounds to meet others, share their experiences, and know they are not alone in the world. Group therapy could also include the alternative methods of stress relief such as meditation, art expression, or musical therapy. The adolescent support groups would allow patients to make new friends, build each other up, and potentially reduce potential for self-harm to progress to suicide.
In conclusion, I agree with the direction that Williams is taking this issue. As a nation, we should all work together to provide better mental health care for our communities. I would like to see us work as a whole, and begin incorporating group and alternative therapies to our mental health patients using self-harm as an outlet for stress and coping, while waiting for appointments to become available with psychiatric specialists.
Sincerely,
Amber Autry, RN