On January 12, 2010, a major earthquake struck Haiti. That evening, Project Medishare (a nonprofit agency based in Miami) began an emergency relief effort. A United Nations storage tent at the Port-au-Prince Airport in Haiti’s capital was transformed into a busy emergency hospital where 225 severely injured persons began to receive treatment. High-quality nursing care became essential to the relief effort.
Ready to contribute
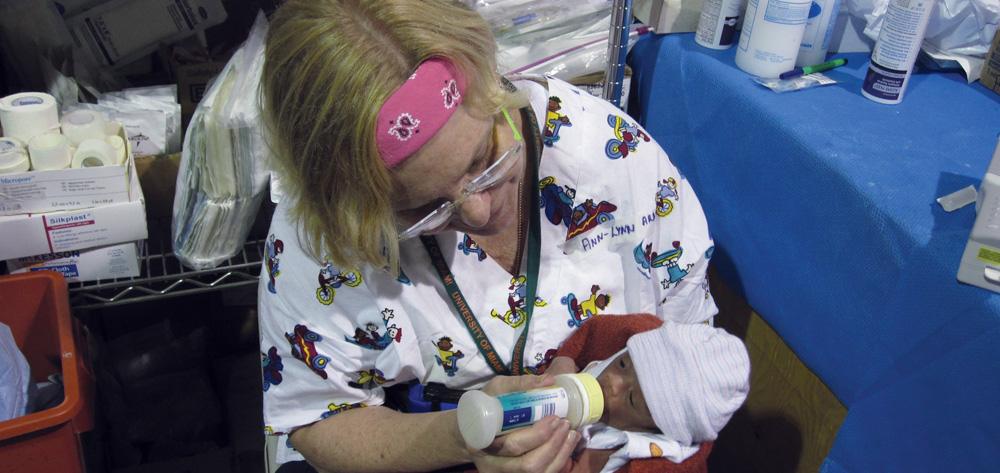
I immediately began to explore volunteer options while planning how to balance work responsibilities and preparing for travel. Five weeks after the quake, I went to Haiti to work with Project Medishare as part of a group of healthcare professionals from the Greater Miami Jewish Federation. After arriving, we were taken to the University of Miami Field Hospital near the airport. The compound included three large tents, which housed an adult trauma center, a pediatric trauma center, an operating room, a wound-care area, and sleeping facilities. I was assigned to the pediatric tent, where I worked 12-hour shifts. I was buoyed by the environment of collaboration and teamwork among nurses, physicians, pharmacists, physical therapists, translators, social workers, soldiers, and missionaries. (See Tending to a tiny quake victim by clicking on the PDF icon above.)
Gratitude and hope
Among our patients and their families, I encountered gratitude and a positive spirit. Patients rarely complained, despite critical injuries and few comforts. Every child I cared for made a lasting impression. They included a 13-year-old girl who had to have both legs amputated, a baby burned in a cooking accident, a 9-year-old boy recovering from an appendectomy, an 11-month-old baby diagnosed with acquired immunodeficiency syndrome (AIDS), and a young boy with broken legs who anxiously awaited surgery in the United States.
My first day’s assignment included 35 children with a wide range of problems. I quickly bonded with the healthcare team and fell into a rhythm of caring and problem solving. The wide variety of our patients’ ailments created a diverse environment that called for continuous problem solving. We dealt with amputations, burns, failure to thrive, HIV/AIDS, fractures, crush injuries, malaria, labor and delivery, malnutrition—and more. Many patients had been rendered homeless or orphaned by the quake; others
didn’t know where family members were. We provided postoperative care, end-of-life care, and emotional support for the anxious and grieving.
Volunteers must collaborate with the local population in a spirit of joint effort and solidarity. As in most disasters, local citizens were central to the Haitian relief effort and successful recovery. Haitians worked beside us, lending support and invaluable information and familiarizing us with cultural norms and perspectives despite their personal losses and tragedies.
Living conditions
Each volunteer was given a cot in a large sleeping tent. Amenities included outdoor showers, portable toilets, bottled water, and meals ready to eat (MREs). One must bring sleeping bags, personal supplies, and desired food provisions from home.
The quake’s aftershocks constantly reminded us of the disaster and the ongoing danger, so even after our 12-hour shifts ended, we had little opportunity to escape its reality. Satisfying rest was limited and we were always on alert for a pending emergency call.
Also, we had to be prepared for changes in schedules and travel plans due to the unpredictable nature of the situation. Communications with the outside world weren’t always reliable or consistent. Even our departure from Haiti turned into an adventure: We were left stranded on the airport tarmac after a 4.8 earthquake disabled the runway lights.
Working with “workarounds”
If you decide to volunteer, be prepared for the unknown and approach the experience with creativity and flexibility. In the United States, healthcare professionals work in highly regulated environments with adequate resources. But in other countries, especially after a disaster, expect a much different situation. Scarcity of structure, information, and supplies necessitates a high level of professional autonomy and critical thinking—and the need to create “workarounds.” Equipment and supplies (mostly donated) aren’t always ideal and may need to be adapted on the fly. In Haiti, we faced such problems as lack of documentation systems and tools, a dearth of pediatric medications, supplies with labels from many countries and languages, and incompatible I.V. equipment. These conditions required constant attention to detail and problem solving.
Also be prepared to function in multiple roles as dictated by the situation. One day, you may be viewed as a novice; the next, you may be called on to take charge. Besides being a caregiver, you may need to serve, for instance, as errand runner or supply agent. During a disaster, ethical standards for nursing practice also may shift. (See Ethical perspectives during a disaster by clicking on the PDF icon above.)
Bound for home, hopeful for the future
When I got back from Haiti, I was tired but extremely satisfied with our efforts. I’d passed through the gamut of emotions—excitement, fear, anxiety, camaraderie, frustration, fatigue, and love—and gained a renewed perspective on life. The experience had been intense and immensely gratifying, largely because of the relationships I’d built with Haitians and my coworkers.
Volunteers continue to donate their time and money to the Haiti relief effort. Donations to reputable relief organizations are still crucial, as is on-site volunteerism. Rebuilding and education efforts for clinics, hospitals, community services, and resources will be in demand there indefinitely.
Project Medishare offers numerous opportunities for healthcare volunteers. The volunteer environment is continually evolving and changing. Project Medishare has moved its pediatric care in Haiti from airport tents to Bernard Mevs Hospital in Port-au-Prince. The wards are air-conditioned, and volunteer quarters are located in a real building. Ultimately, the pediatric census will be maintained at 40 beds. Activities will include active training of Haitian doctors and nurses in delivering high-acuity and critical pediatric care. Miracles are happening every day.
I feel I received so much more from the people of Haiti—and the experience as a whole—than I gave to them. My desire to return there and continue to support relief efforts remains strong.
Selected References
Bayard D. Haiti earthquake relief, phase two—long-term needs and local resources. N Engl J Med. 2010;362:1858-1861.
Ginzburg E, O’Neill W, Goldschmidt P, de Marchena E, Pust D, Green B. Rapid medical relief—Project Medishare and the Haitian earthquake. N Engl J Med. 2010;362(10):e31.
Merchant R, Leigh J, Lurie N. Health care volunteers and disaster response: first be prepared. N Engl J Med. 2010;362(10):872-873.
Merin O, Nachman A, Schwaber M, Kriess Y. The Israeli field hospital in Haiti—ethical dilemmas in early disaster response. N Engl J Med. 2010; 362(11):e38.
Ann-Lynn Denker is director of the Center for Nursing Excellence at Jackson Health System in Miami, Florida.