Quick treatment results in a good outcome.
Takeaways:
- Angiotensin-converting enzyme inhibitors can increase the release of bradykinin, which can increase tissue permeability with dilatation of the vessels and result in angioedema.
- Bradykinin-induced angioedema is a life-threatening complication that involves airway obstruction and can progress to death.
- Off-label use of fresh frozen plasma has been shown to be effective for severe acute bradykinin-induced angioedema when resistance to epinephrine, steroids, and antihistamines occurs.
Marcus Green* is a 45-year-old Black man with a 5-year history of hypertension who takes his blood pressure medication on the way to work. About 20 minutes after taking it this morning, his tongue begins to feel heavy and his lips and tongue begin to swell. He drives himself to the emergency department (ED).
History and assessment
Jane Jackson, Mr. Green’s nurse, conducts a quick assessment, noticing the swelling. When she learns that Mr. Green is taking lisinopril for his hypertension, she realizes he’s likely experiencing angioedema. She obtains vital signs and, per protocol, starts oxygen at 2 liters/minute via nasal cannula. Mr. Green’s vital signs are BP 98/60 mmHg, heart rate 128 bpm, respiration rate 24 breaths/minute, oxygen saturation 98%, and axillary temperature 98.1°F (36.7°C).
Mr. Green is alert and oriented, but he’s becoming increasingly anxious and his lips and tongue continue to swell. Jane starts ECG monitoring; inserts an 18-gauge peripheral I.V. in his right arm; and administers epinephrine, methylprednisolone, and diphenhydramine, as ordered, but without effect.
Clinical management
Concerned that Mr. Green may rapidly deteriorate, the ED provider asks an anesthesia provider to perform a fiberoptic nasal intubation to protect the patient’s airway. The anesthesia provider doesn’t give Mr. Green a benzodiazepine or medication for pain because it may cause sedation and impede spontaneous breathing. However, the anesthesia provider does order 2 units of fresh frozen plasma (FFP) I.V.
After two unsuccessful intubation attempts, the anesthesia provider administers glycopyrrolate 0.2 mg I.V. to decrease Mr. Green’s excessive bronchial secretions and prevent bronchospasm. Mr. Green remains alert and cooperative and the airway is secured nasally with an endotracheal tube. He’s immediately given propofol 200 mg I.V. as a general anesthetic, and the respiratory therapist places him on a ventilator. Mr. Green is taken to the ICU where his angioedema subsides in 4 hours and he’s extubated 24 hours later. He’s discharged home 3 days later, and his provider prescribes losartan, an angiotensin-receptor blocker.
Education
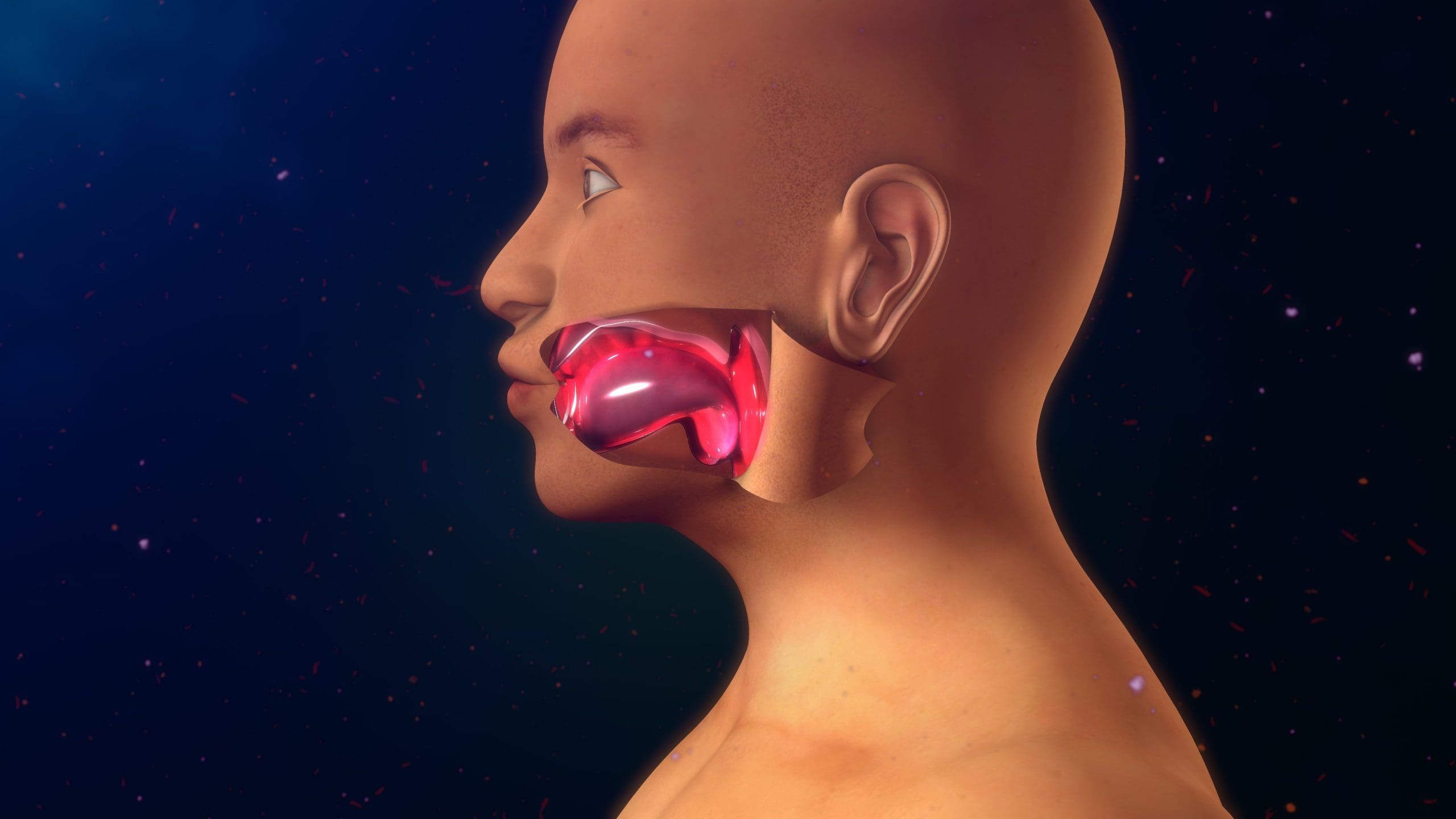
Angiotensin-converting enzyme (ACE) inhibitors such as lisinopril can cause bradykinin-induced angioedema (increased release of the enzyme bradykinin, which can cause increased tissue permeability with dilatation of the vessels and swelling). In the United States, 30% to 40% of angioedema diagnoses in the ED are related to ACE inhibitors, with 0.1% to 2.2% being life-threatening.
Typical signs of angioedema related to ACE inhibitors include lip, face, and tongue swelling without rash or itching. However, the larynx and pharynx also can be involved. In most cases, angioedema resolves without complications in a few days, but Mr. Green’s respiratory manifestations made prompt treatment essential.
No standardized treatment for bradykinin-induced angioedema exists, but the off-label use of FFP has been shown to be an effective treatment for severe episodes. Bradykinin responds to the kininase II in FFP, which is identical to ACE.
Unfortunately, in one reported case, despite a patient receiving epinephrine, methylprednisolone, and diphenhydramine, followed by I.V. FFP, their symptoms progressed and 2 hours later intubation was required, as was the case with Mr. Green. Therefore, nurses should follow the research in this area. AN
*Name is fictitious. To view a list of references, visit myamericannurse.com/?p=71927.
Veronica Y. Amos is an assistant director of the nurse anesthesia program and assistant professor at the University of Maryland School of Nursing in Baltimore.
References
Bernstein JA, Cremonesi P, Hoffman TK, Hollingsworth J. Angioedema in the emergency department: A practical guide to differential diagnosis and management. Int J Emerg Med. 2017;10(1):15.
Hirschy R, Shah T, Davis T, Rech MA. Treatment of life-threatening ACE-inhibitor-induced angioedema. Adv Emerg Nurs J. 2018;40(4):267-77.
Chaaya G, Afridi F, Faiz A, Ashraf A, Ali M, Castiglioni A. When nothing else works: Fresh frozen plasma in the treatment of progressive, refractory angiotensin-converting enzyme inhibitor–induced angioedema. Cureus. 2017;9(1):e972.
Salem D, Alchakaki A. Treatment of severe ACE inhibitor angioedema: Current and future therapies. Consultant360. 2016;56(2):134-7. consultant360.com/articles/treatment-severe-ace-inhibitor-angioedema-current-and-future-therapies