Key takeways
|
A debilitating disease marked by swelling, tenderness, and synovial joint destruction, rheumatoid arthritis (RA) can lead to severe functional disability and poor quality of life, imposing substantial burdens on patients and their caregivers. (See Who gets RA?)
What’s more, the disease is linked to systemic comorbidities, such as cancer, infections, and cardiovascular and mental health conditions. These comorbidities increase mortality and shorten life expectancy. And while more aggressive treatments have decreased the incidence of extra-articular RA manifestations, the disease also can affect the eyes, lungs, kidneys, skin, hematopoietic system, blood vessels, nervous system, and salivary glands. Evidence suggests that both genetics and environmental factors play a role in RA development.
Once focused in acute-care settings, care of patients with RA has moved into home and ambulatory settings. However, patients in these venues don’t always have access to a nurse practitioner (NP) or rheumatology RN who can provide specialty care. This article highlights the importance of early diagnosis, discusses current therapeutic recommendations for managing pain and achieving remission, and describes RNs’ role in caring for these patients in the community.
Early diagnosis
Early diagnosis (within 6 months of RA symptom onset) coupled with aggressive treatment reduces the risk of joint damage and disability, helps maintain joint integrity, and enhances productivity and quality of life. However, with no diagnostic gold standard available, early diagnosis can be challenging.
Before development of the antibodies against citrullinated peptides (ACPA) test, rheumatoid factor (RF) was the only laboratory test available to diagnose RA. The ACPA test promotes early, accurate diagnosis, with a specificity of 90% to 97%. On the other hand, the RF test is relatively sensitive (70% to 75%) but rather nonspecific (as low as 50%) because other rheumatic and nonrheumatic conditions (such as Sjögren’s syndrome and hepatitis C infection) may trigger positive RF tests. Abnormal erythrocyte sedimentation rate (ESR) and C-reactive protein (CRP) results can help assess treatment response, but these inflammatory markers aren’t useful in diagnosing early-onset RA.
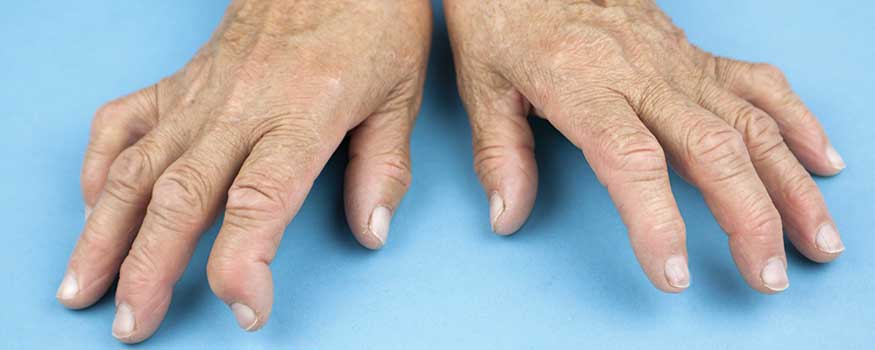
Many clinical features of RA—joint deformities, rheumatoid nodules, and joint erosion on X-ray—don’t appear in early disease stages. However, pain and swelling in fingers and toes have high sensitivity for RA (94.6%) early in the disease, but specificity of only 15.3%.
Given the difficulty of accurate early diagnosis, clinicians commonly rely on a combination of a history consistent with inflammatory arthropathy (for example, morning stiffness lasting an hour or longer) and physical findings of joint swelling in classic RA patterns (symmetrical involvement of small joints). RA diagnosis may be made even without a positive RF/ACPA test.
Early aggressive treatment
Before 1980, the pyramid approach to RA treatment started with aspirin or other nonsteroidal anti-inflammatory drugs. Disease-modifying anti-rheumatic drugs (DMARDs), such as methotrexate, were reserved for patients with severe disease or those who didn’t respond to conservative treatment. Reluctance to prescribe DMARDs stemmed from lack of knowledge about early aggressive treatment to minimize permanent joint damage, unfamiliarity with optimal dosing, and few effective drugs with high benefit-to-risk ratios. As a result, many patients became disabled 10 to 20 years after diagnosis due to severe joint deformities and extra-articular manifestations.
Current RA treatment recommendations focus on early aggressive therapy. For example, clinicians should initiate DMARDs (preferably methotrexate) immediately after diagnosis, with the goal of achieving remission or low disease activity. Patients who don’t respond to traditional DMARD monotherapy may be candidates for combination therapy, such as multiple traditional DMARDs or concomitant biologic agents, such as tumor necrosis factor inhibitors (TNFis); examples of TNFis include etanercept, infliximab, and adalimumab. The current treatment model has dramatically reduced severe joint deformities and extra-articular manifestations.
Patients receiving these agents require close monitoring for adverse effects. For example, methotrexate is associated with hepatotoxicity and bone marrow suppression, so patients taking this drug should undergo complete blood counts and liver enzyme tests every 2 to 3 months. And because of the immunomodulating actions of biologics that increase the risk of certain infections, patients taking TNFis and other biologic agents should be tested for latent tuberculosis and receive pneumococcal, zoster, and influenza vaccinations before beginning treatment. (See Recommended drug therapies for RA.)
Multidisciplinary approach
Patients with extensive joint damage need ongoing treatment and close monitoring, along with instructions to adhere to prescribed drug therapy. These actions are best coordinated through a multidisciplinary approach. Depending on the individual patient’s needs, the team may include a rheumatologist, rheumatology NP, RN, pharmacist, physical therapist, occupational therapist, podiatrist, physician assistant, and social worker. To help ensure optimal physical and psychosocial functioning and quality of life, the team provides education and support based on the patient’s goals.
Some multidisciplinary models include specialized arthritis programs, ongoing management, triage, rural consultant support, and telemedicine. Given the lack of reimbursement for hospitalization, most multidisciplinary programs are conducted in outpatient and community settings as day-patient programs. In the United States and across Europe, nurses have become an integral part of the multidisciplinary team, engaging in tasks traditionally performed only by rheumatologists. (See NPs’ impact on RA care.)
Providing care in the community
With limited availability of rheumatology NPs and rheumatology RNs in home health care, some long-term care facilities, hospices, schools, and faith-based organizations employ RNs to manage and coordinate the plan of care established by the rheumatologist or NP.
So RNs must be knowledgeable about RA pathophysiology, treatment, and management. We’ll use the nursing process steps of assessment, diagnosis, planning, implementation, and evaluation as a guide for managing patients and, as applicable, their caregivers.
Conduct an initial assessment
During your initial assessment of the patient and caregiver, establish goals and expected outcomes for successful disease management. Many patients with RA experience anxiety, anger, frustration, and depression. When you recognize these emotions, encourage the patient to discuss them with the rheumatologist or NP.
Key nursing actions at this stage are to establish a therapeutic relationship with the patient and caregiver, assess their understanding of RA and its management, and evaluate their physical, emotional, and psychological well-being.
Identify appropriate nursing diagnoses
RA signs and symptoms vary with disease severity. Note joint swelling and pain, morning stiffness, and deformities. Pain and deformities may limit the patient’s ability to perform activities of daily living (ADLs), which may lead to frustration, low self-esteem, and poor quality of life. Evaluate family dynamics as well as ethnic and cultural influences on the patient’s perception of RA and self-care abilities.
Use the information you’ve gathered to identify appropriate nursing diagnoses. Common ones for patients with RA are pain and discomfort, activity intolerance and impaired mobility, self-care deficits, fall risk, ineffective coping, altered body image or role performance, ineffective health maintenance, nonadherence to the therapeutic regimen, and caregiver role strain.
Collaborate in care planning
Work with the patient and caregiver to set measurable short- and long-term goals to achieve expected outcomes based on the nursing diagnoses. Evaluate their readiness to learn and motivation to participate in care. As you do this, be sure to:
• reinforce the multidisciplinary team approach to care
• discuss psychological factors related to RA, such as depression, anxiety, and stress
• explain drugs used to treat RA
• discuss nonpharmacologic approaches, such as joint protection, heat and cold therapy, range-of-motion exercises, and complementary and alternative therapies, as prescribed by the provider.
To enhance your effectiveness, ask open-ended questions, be sensitive to cultural preferences and family communication styles, and avoid arguing with the patient or caregiver.
Implement the plan
After devising a plan of care, implement evidence-based strategies based on established priorities, and provide patient education. Explain to the patient and caregiver that RA is a progressive chronic systemic disease that eventually may affect ADLs. Discuss the importance of adhering to prescribed drug therapy and nonpharmacologic treatment to control pain. Because of the remitting and relapsing nature of RA, review signs and symptoms of flares with the patient and caregiver.
Use the following strategies to enhance your effectiveness:
• Identify the preferred teaching method for and learning styles of the patient and caregiver.
• Educate them about the prescribed drug regimen to control pain and achieve remission.
• Reinforce the importance of medication adherence. Discuss adverse reactions, drug interactions, and use of herbal and complementary remedies with prescribed medications.
• Monitor medication efficacy and the patient’s tolerance.
• Promote participation in selfcare, including safety issues such as hot and cold therapy and coping with the stress or depression that may accompany RA.
• Review and obtain appropriate adaptive devices to help the patient perform ADLs.
• Provide consumer health material on RA and information about local support groups. (See Online resources for patients with RA.)
• Teach the patient and caregiver how to recognize and manage acute flares and systemic complications of RA.
• Urge them to keep follow-up appointments.
Evaluate outcomes
To determine if the expected outcomes and goals of care are being met, regularly evaluate how the plan of care is progressing.
• Monitor medication therapy, including efficacy, side effects, and signs and symptoms of RA flares (for example, changes in morning stiffness, fatigue, painful or swollen joints).
• Inform other multidisciplinary team members of the effectiveness of medications, nonpharmacologic measures, and disease progress.
• Collaborate with other multidisciplinary team members to help the patient or caregiver achieve unmet goals.
• Work with the patient and caregiver to refine goals as needed.
Your role in enhancing patient outcomes
Nurses in the community help patients with RA achieve the ultimate goal of remission or low disease activity. Based on the patient’s individual needs, encourage and assist him or her to establish health behaviors and activities that promote rest and exercise, reduce stress, and encourage independence.
Adeline Chu is an assistant professor of nursing in the School of Health Sciences at Seattle Pacific University and a clinical assistant professor in the Department of Biobehavioral Nursing and Health Informatics at the University of Washington in Seattle. Bernard Ng is chief of the Rheumatology Section at VA Puget Sound Healthcare System in Seattle and an associate professor of medicine in the Division of Rheumatology at the University of Washington in Seattle.
Selected references
Aggarwal R, Ringold S, Khanna D, et al. Distinctions between diagnostic and classification criteria? Arthritis Care Res. 2015;67(7):891-7.
Aletaha D, Neogi T, Silman AJ, et al. 2010 Rheumatoid arthritis classification criteria: An American College of Rheumatology/European League Against Rheumatism collaborative initiative. Arthritis Rheum. 2010;62(9):2569-81.
Birnbaum H, Pike C, Kaufman R, et al. Societal cost of rheumatoid arthritis patients in the US. Curr Med Res Opin. 2010;26(1):77-90.
Bongartz T, Nannini C, Medina-Velasquez YF, et al. Incidence and mortality of interstitial lung disease in rheumatoid arthritis: A population-based study. Arthritis Rheum. 2010;62(6):1583-91.
Chamberlain V. Patients with inflammatory arthritis: An opportunity for community nurses. Br J Community Nurs. 2011;16(6):268-73.
Crawford A, Harris H. Understanding the effects of rheumatoid arthritis. Nursing. 2015;45(11):32-8.
De Rycke L, Verhelst X, Kruithof E, et al. Rheumatoid factor, but not anti-cyclic citrullinated peptide antibodies, is modulated by infliximab treatment in rheumatoid arthritis. Ann Rheum Dis. 2005;64(2):299-302.
Dubucquoi S, Solau-Gervais E, Lefranc D, et al. Evaluation of anti-citrullinated filaggrin antibodies as hallmarks for the diagnosis of rheumatic diseases. Ann Rheum Dis. 2004;63(4):415-9.
Duffy M. Rheumatology Nursing: Scope and Standards of Practice. Silver Spring, MD: American Nurses Association; 2014.
Durham CO, Fowler T, Donato A, et al. Pain management in patients with rheumatoid arthritis. Nurse Pract. 2015;40(5):38-45.
Gibofsky A. Current therapeutic agents and treatment paradigms for the management of rheumatoid arthritis. Am J Manag Care. 2014;20(suppl 7):S136-44.
Gossec L, Combescure C, Rincheval N, et al. Relative clinical influence of clinical, laboratory, and radiological investigations in early arthritis on the diagnosis of rheumatoid arthritis. Data from the French Early Arthritis Cohort ESPOIR. J Rheumatol. 2010;37(12):2486-92.
Helmick CG, Felson DT, Lawrence RC, et al; National Arthritis Data Workgroup. Estimates of the prevalence of arthritis and other rheumatic conditions in the United States. Part I. Arthritis Rheum. 2008;58(1):15-25.
Lee DM, Schur PH. Clinical utility of the anti-CCP assay in patients with rheumatic diseases. Ann Rheum Dis. 2003;62(9):870-4.
MacKay C, Veinot P, Badley EM. Characteristics of evolving models of care for arthritis: A key informant study. BMC Health Serv Res. 2008;8:147.
Madigan A, FitzGerald O. Multidisciplinary patient care in rheumatoid arthritis: Evolving concepts in nursing practice. Baillieres Best Pract Res Clin Rheumatol. 1999;13(4):661-74.
Maillefert JF, Combe B, Goupille P, et al. Long term structural effects of combination therapy in patients with early rheumatoid arthritis: Five year follow up of a prospective double blind controlled study. Ann Rheum Dis. 2003;62(8):764-6.
Marion CE, Balfe LM. Potential advantages of interprofessional care in rheumatoid arthritis. J Manag Care Pharm. 2011;17(9 suppl B):S25-9.
Mendes A. Helping people with rheumatoid arthritis to live well. Br J Community Nurs. 2015;20(12):620.
Mussen L, Boyd T, Bykerk V, et al. Low prevalence of work disability in early inflammatory arthritis (EIA) and early rheumatoid arthritis at enrollment into a multi-site registry: Results from the catch cohort. Rheumatol Int. 2013;33(2):457-65.
Myasoedova E, Davis JM 3rd, Crowson CS, et al. Epidemiology of rheumatoid arthritis: Rheumatoid arthritis and mortality. Curr Rheumatol Rep. 2010;12(5):379-85.
Ndosi M, Vinall K, Hale C, et al. The effectiveness of nurse-led care in people with rheumatoid arthritis: A systematic review. Int J Nurs Stud. 2011;48(5):642-54.
Poh LW, He HG, Lee CS, et al. An integrative review of experiences of patients with rheumatoid arthritis. Int Nurs Rev. 2015;62(2):231-47.
Puolakka K, Kautiainen H, Möttönen T, et al. Impact of initial aggressive drug treatment with a combination of disease-modifying antirheumatic drugs on the development of work disability in early rheumatoid arthritis: A five-year randomized followup trial. Arthritis Rheum. 2004;50(1):55-62.
Raychaudhuri S. Recent advances in the genetics of rheumatoid arthritis. Curr Opin Rheumatol. 2010;22(2):109-18.
Sauerland U, Becker H, Seidel M, et al. Clinical utility of the anti-CCP assay: Experiences with 700 patients. Ann N Y Acad Sci. 2005;1050:314-8.
Singh JA, Saag KG, Bridges SL Jr., et al. 2015 American College of Rheumatology guideline for the treatment of rheumatoid arthritis. Arthritis Rheumatol. 2016;68(1):1-26.
Smolen JS, Aletaha D, Machold KP. Therapeutic strategies in early rheumatoid arthritis. Best Pract Res Clin Rheumatol. 2005;19(1):163-77.
Solomon DH, Bitton A, Fraenkel L, et al. Roles of nurse practitioners and physician assistants in rheumatology practices in the US. Arthritis Care Res. 2014;66(7):1108-13.
Solomon DH, Fraenkel L, Lu B, et al. Comparison of care provided in practices with nurse practitioners and physician assistants versus subspecialist physicians only: A cohort study of rheumatoid arthritis. Arthritis Care Res. 2015;67(12):1664-70.
Turesson C. Extra-articular rheumatoid arthritis. Curr Opin Rheumatol. 2013;25(3):360-6.
van Eijk-Hustings Y, van Tubergen A, Boström C, et al. EULAR recommendations for the role of the nurse in the management of chronic inflammatory arthritis. Ann Rheum Dis. 2012;71(1):13-9.
van Jaarsveld CH, Jacobs JW, van der Veen MJ, et al. Aggressive treatment in early rheumatoid arthritis: A randomised controlled trial. On behalf of the Rheumatic Research Foundation Utrecht, The Netherlands. Ann Rheum Dis. 2000;59(6):468-77.
van Venrooij WJ, Pruijn GJ. Citrullination: a small change for a protein with great consequences for rheumatoid arthritis. Arthritis Res. 2000;2(4):249-51.
Vliet Vlieland TP. Multidisciplinary team care and outcomes in rheumatoid arthritis. Curr Opin Rheumatol. 2004;16(2):153-6.
Watts RA, Mooney J, Barton G, et al. The outcome and cost-effectiveness of nurse-led care in the community for people with rheumatoid arthritis: A non-randomised pragmatic study. BMJ Open. 2015;5(8):e007696.
Dear Lillee,
MSN, RN FAAN
(Editor-in-Chief, American Nurse Today)
June’s edition of American Nurse Today featured a highly informative article regarding the management of rheumatoid arthritis (RA) in the community setting. Advances in pharmacologic management including disease-modifying anti-rheumatic drugs and biologic agents were presented, demonstrating the significant advances made in the management of this chronic and debilitating disease.
A number of the drugs presented in the article are used in the antineoplastic setting as well. It is imperative that healthcare workers involved in preparing and administering these agents for RA as well as those educating patients undergoing treatment understand the hazardous potential of these agents and implications for safety in the clinic and home settings. Chemotherapy and other antineoplastic agents are deemed hazardous as they possess genotoxic, carcinogenic, teratogenic and fertility impairing characteristics and are known to cause DNA and chromosomal damage in exposed healthcare workers. While methotrexate and leflunomide specifically are identified as hazardous agents, so too are some biologics. Nurses and those caring for these patients need to be aware of the toxicity profile associated with these agents and be aware of the drugs being used in their practice that are considered hazardous.
Consequently, organizations including OSHA, NIOSH, and ONS endorse adherence to personal protective equipment (PPE) recommendations when administering these agents regardless of route, dose, or indication. Wearing two pairs of chemotherapy-approved gloves and a single-use and a disposable gown with back closure made from low-permeable fabric is recommended for handling and administering these agents. Body fluids of patients receiving these agents do contain traces of active drug, therefore PPE recommendations apply to handling body fluids of patients for up to 48 hours after administration. More about NIOSH’s recommendations for preventing occupational exposure to antineoplastic and other hazardous drugs can be found in NIOSH’s report on safe handling and list of hazardous agents.
As the article alludes to, RA treatment is occurring in the ambulatory and home setting, which argues the need for patient education on how to protect themselves and their loved ones from accidental exposure. Priority teaching points include storage of antineoplastic agents and keeping them separate from other medications to avoid contamination, the need for gloves when handling contaminated body fluids, as well as proper linen and excreta handling.
ONS is committed to promoting safe medication administration and handling by clinicians involved in hazardous drug administration. We welcome any questions or comments you and your readers may have about the safety implications of administering RA agents. Thank you for the article and the opportunity to provide comments about ensuring safety of our nurses.
Best Regards,
Kathleen Wiley
MSN, RN, AOCNS


















13 Comments.
Can people have several types of arthritis?
My daughter was diagnosed with RA this year. So, I am learning more about it. She has been taking several of the common drugs used to treat RA. And also she has changed her diet because she gets a flare up when she eats certain things such as gluten, fried foods, coffee, and sugar. She is also trying PEMF therapy to reduce inflammation.
I was diagnosed with rheumatoid arthritis 5 years ago. I have stiffness, swelling, carpal tunnel syndrome, and intense pain. I was put on methotrexate and folic acid, I still suffer from stiffness and pain, but now they are saying I haven’t got it. I have osteoarthritis too. I don’t understand this so i look up online for Herbal treatment and a page redirected. me to Akanni Herbal Centre (www. akanniherbalcentre .com ). Few months into the treatment, I made a significant recovery. . After I completed the recommended herbal treatment plan, almost all my symptoms were gone
Which test must be done to find out if there’s RA?
updated. The quiz button is live. Please see the top of the article.
Apologies for the delay. 😉
Where is the CNE test for this article?
Will the CE quiz be coming soon?
I would like to take the post-test for the RA article, however I find no link to register and take the exam. I appreciate your assistance.
Susan Carlson
carlson.gnp@gmail.com
Where do I submit my exam answers??
I have severe RA and appreciated this article. I have suffered depression & severe fatigue which are symptoms that most of those I deal with, do not understand and do not know how to manage. Helping a patient’s family understand how they can be supportive and help, I believe are key to the client managing better.
Where is the post test???
I want to take the test for rheumatoid arthritis. I am a member and your white is impossible to get to this test. How do I get to the test.
how can I get CNE