Use this unique educational format to enhance learning and engage students.
Connecting theoretical undergraduate nursing classroom instruction to clinical practice requires faculty who can help draw direct links between these two educational elements. Clinical conferences provide a unique format for accomplishing this goal.
What are clinical conferences?
Clinical conferences involve small group discussions where students acquire knowledge, develop critical-thinking and decision-making skills, and build confidence. These faculty-facilitated conferences can occur before (pre-clinical), during (mid-clinical), or after (post-clinical) a clinical experience. Each type allows students to link theory to practice via discussion, collaboration, reflection, and clarification of information. (See Clinical conference types.)
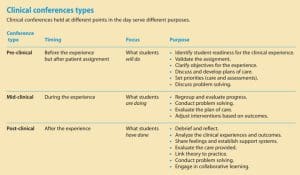


Faculty conduct conferences based on type, clinical objectives, student academic level, and clinical unit. Pre-clinical conferences are held at the beginning of the experience after patient assignments, which allows faculty to gauge readiness, clarify expectations, and offer guidance. Mid-clinical conferences are ideal for 12-hour experiences and most occur in the middle of the shift. Post-clinical conferences typically occur at the end of the clinical day.
Mohn-Brown proposed an innovative option in which clinical conferences might be held as seminars on a different day and in a new environment, while still functioning as a continuation of the clinical experience. According to the author, the extra time provided students with opportunities to reflect on their performance and prepare to integrate and apply knowledge in student presentations or student-led discussions during the seminar. McCord Tierney and Abott suggest conducting dedicated clinical conferences independent of clinical days as an effective way to overcome low participation due to student fatigue and to enhance the development of clinical knowledge and judgment.
Clinical conferences typically are held in person, but they can be conducted using virtual platforms. Use of virtual or online clinicals and clinical conferences has grown in response to space limitations as a result of COVID-19 restrictions. Petrovic and colleagues describe these online post-clinical conferences as student-centered asynchronous discussion and learning environments with varying degrees of instructor involvement. They allow for rich reflective dialogue that promotes student engagement and learning. Using a delayed web-based audio-video alternative permits extended time for student reflection while also including instructor and peer-to-peer interaction to facilitate learning.
Why are clinical conferences important?
The theory of constructivism supports using clinical conferences to combine previously learned concepts with new knowledge. The theory proposes that learners actively construct new knowledge by reflecting on and integrating new and existing knowledge, while faculty serve as facilitators.
Clinical conferences enhance learning, engage students, promote critical-thinking skills, aid professional development, and improve clinical reasoning and judgment. Successful conferences require planning, but faculty must remain flexible to accommodate learning and the exchange of meaningful experiences. A learner-centered teaching strategy can help improve students’ knowledge and skills, build their confidence, and prepare them for practice in increasingly complex healthcare environments. To ensure students actively participate in clinical conferences, faculty must implement innovative teaching strategies to promote learning and integrate theory into practice. While facilitating the conference, faculty can model professional behavior and identify individual student needs.
As students’ progress along the curriculum, they’ll begin to think independently and link theory to practice. Using Bloom’s taxonomy (remember, understand, apply, analyze, evaluate, create) as a guide, faculty should evaluate teaching strategies to ensure they’re appropriate for the group’s academic level and learning needs.
How do clinical conferences work?
Although clinical conferences have few associated costs, meaningful exchanges between faculty and students (and among students) require a commitment to potential practice adjustments. They involve careful facilitation by faculty and active participation by students. (See Roles and responsibilities.)
Roles and responsibilities
Faculty members and students have distinct responsibilities for ensuring meaningful clinical conferences.
Faculty role
- Have a plan.
- Be flexible and adaptable to situations, such as emergencies or changes in a patient’s condition.
- Set a positive tone for the clinical experience.
- Establish expectations for the conference.
- Create an environment conducive to openness, trust, sharing, and discussion.
- Support and encourage students.
- Maintain group focus.
- Allow time for reflection.
- Provide constructive feedback.
- Promote student learning related to course objectives and outcomes.
- Facilitate the transfer of knowledge.
- Model professional behavior.
Student roles
- Arrive on time.
- Be prepared.
- Be open-minded.
- Engage in discussion.
- Be receptive to constructive feedback.
- Demonstrate professionalism.
Faculty can use the conferences as an opportunity to reinforce knowledge, introduce new concepts, identify gaps, and evaluate learning needs. They can use constructive feedback to help students develop critical-thinking and decision-making skills. Students benefit as they begin to integrate theory into practice, build on existing knowledge, and create new knowledge. They can reflect on their performance and identify areas that require improvement. The conferences also provide students with opportunities to collaborate while they build individual confidence. In addition, students become socialized to the profession and the nursing role.
Students should view clinical conferences as extensions of the teaching–learning environment, and faculty should clearly state objectives, set expectations, and encourage participation. However, faculty inexperience can present a challenge to conducting meaningful clinical conferences. A lack of clarity regarding conference expectations may result in a disorganized session with no clear objectives. Students may not view the clinical conference as an opportunity to learn, and a lack of appropriate direction may leave them feeling overwhelmed.
How do faculty keep students engaged?
Meeting the needs of diverse learning styles requires faculty innovation and creativity when planning clinical conferences. To maximize student learning, Harrison Kelly and colleagues suggest using debriefing to promote reflection and feedback to assist students in future clinical experiences. Faculty may consider using the International Nursing Association for Clinical Simulation and Learning debriefing standard, which suggests structuring debriefing to facilitate future performance improvement, or engaging in “debriefing with good judgment,” where faculty share their expertise, provide critical feedback, and create a safe environment for students to discuss and reflect on their performance. Debriefing allows students to learn from their performance and provides an opportunity for the group to explore and express personal feelings and attitudes about patient care and staff interaction.
Various teaching strategies facilitate learning and keep students engaged, including the following:
Flip the conference
- Assign students to speak on specific topics, such as a patient diagnosis (diabetes, hemorrhage, anemia) or a nursing concept (safety, end of life care).
- Use Socratic inquiry, in which faculty pose questions that challenge students to engage in critical thinking and knowledge synthesis.
- Encourage students to share their experiences by summarizing events and interactions, including what went well and what could have been done differently.
- Use Ask me/Teach me, in which students ask questions to clarify misunderstandings or teach the group about something new they experienced or learned that day.
- Ask students to verbalize, prioritize, and discuss nursing diagnosis and patient-centered goals, including planned interventions and evaluations. Encourage them to plan alternate strategies in the event of unsuccessful interventions or unexpected outcomes
Student collaboration
- Use scaffolding case studies that show a progression from simple to more complex concepts and current patient care experiences or hypothetical cases related to classroom concepts to prompt discussion. Facilitate correlation of patient data to develop appropriate care plans.
- Discuss patient education and health promotion.
- Present legal, ethical, and clinical issues for discussion.
- Role-play a patient situation. Provide a scenario and assign students to roles (nurse, provider, patient, family member).
Reflecting on experience and actions
- Implement think-pair-share, which requires three stages of cooperative student action. Faculty organize students in pairs, assign them a question or topic, provide time to think and prepare, and then ask them to share ideas with the class.
- Apply critical incident methodology. In this recall-to-learn process, faculty lead students through a recollection of events to identify and explore significant variables that contributed to the successful or unsuccessful outcome that day. To conclude the exercise, faculty provide alternatives or explanations.
Enhance competence and confidence
Clinical conferences serve as a unique vehicle for integrating theoretical classroom concepts into practice. Nursing faculty who understand this and possess the appropriate skills can aid the transfer of knowledge and enhance student competence and confidence.
Joset Brown is an assistant professor at William Paterson University in Wayne, New Jersey. Dione Sandiford is a lecturer and clinical learning facilitator at Rutgers University School of Nursing in Newark, New Jersey.
References:
Brandon AF, All AC. Constructivism theory analysis and application to curricula. Nurs Educ Perspect. 2010;31(2):89-92.
Cooper KM, Schinske JN, Tanner KD. Reconsidering the share of a think-pair-share: Emerging limitations, alternatives, and opportunities for research. CBE Life Sci Educ. 2021;20(1):fe1. doi:10.1187/cbe.20-08-0200
Gubrud-Howe P. Teaching in the clinical setting. In: Billings DM, Halstead JA, eds. Teaching in Nursing: A Guide for Faculty. 6th ed. New York City, NY: Elsevier; 2020; 328-52.
Halstead JA. Frank B. Pathways to a Nursing Education Career: Educating the Next Generation of Nurses. New York City, NY: Springer Publishing Company; 2010.
Hannans J. Online clinical post conference: Strategies for meaningful discussion using VoiceThread. Nurse Educ. 2019;44(1):29-33. doi:10.1097/NNE.0000000000000529
Harrison Kelly S, Henry R, Williams S. Using debriefing methods in the postclinical conference. Am J Nurs. 2019;119(9):56-60. doi:10.1097/01.NAJ.0000580280.87149.12
Makhene A. The use of the Socratic inquiry to facilitate critical thinking in nursing education. Health SA. 2019;24:1224. doi:10.4102/hsag.v24i0.1224
McCord Tierney K, Abbott AA. Independent conference days: An innovative approach to clinical postconferencing. J Nurs Educ. 2020;59(4):239. doi:10.3928/01484834-20200323-13
Mohn-Brown E. Implementing quality and safety education for nurses in postclinical conferences: Transforming the design of clinical nursing education. Nurse Educ. 2017;42(5S Suppl 1):S18-21. doi:10.1097/NNE.0000000000000410
Petrovic KA, Hack R, Perry B. Establishing meaningful learning in online nursing postconferences: A literature review. Nurse Educ. 2020;45(5):283-7. doi:10.1097/NNE.0000000000000762
Philpot R, Smith W, Gerdin G, et al. Exploring social justice pedagogies in health and physical education through Critical Incident Technique methodology. Eur Physical Educ Rev. 2021;27(1):57-75. doi:10.1177/1356336X20921541
Steven A, Wilson G, Turunen H, et al. Critical incident techniques and reflection in nursing and health professions education: Systematic narrative review. Nurse Educ. 2020;45(6):E57-61. doi:10.1097/NNE.0000000000000796
Stokes LG, Kost GC. Teaching in the clinical setting. In Billings DM, Halstead JA. eds. Teaching in Nursing: A Guide for Faculty. 4th ed. Philadelphia, PA: Elsevier Saunders; 2011; 311-34.
Vezeau TM. In defense of clinical conferences in clinical nursing education. Nurse Educ Pract. 2016;16(1), 269-73. doi:10.1016/j.nepr.2015.10.006