Over 4,380 nurse clinicians and managers from across the United States shared their thoughts about their jobs, including salary, satisfaction, and workplace violence.
- Over 4,380 nurses completed the 2022 nursing trends and salary survey.
- More nurses are reporting incidents of workplace violence and are more satisfied with responses to those reports.
- Almost a third of respondents plan to seek new employment within the next 3 months.
*Editor’s note: Because of rounding, the total of some percentages may not add up to exactly 100%.
Trends and Salaries Interactive Results
2021 nursing trends and salary survey results
2020 nursing trends and salary survey results
American Nurse Journal’s sixth annual Nursing Trends and Salary Survey reflects some positive movement, such as improved response to reports of workplace violence and slightly higher job satisfaction. But challenges, such as ongoing staffing shortages and incidents of violence, continue. Fortunately, nurses seem ready to face those challenges: For the sixth straight year, most respondents (82% of 4,397) would choose nursing as their profession again. Here’s a closer look at some of the key survey findings, which include aggregate data and some comparisons between clinicians and nurse managers.
Staffing challenges
Unsurprisingly, a clear message from the survey is that staffing recruitment and retention remains a difficult challenge for clinicians and managers, although some results indicate a slight improvement. Open positions over the past year increased for about 63% of managers, down from 71% in 2021, and 61% reported increased RN turnover in the same time frame, down from 72% in 2021. Nearly two-thirds (64%) of managers reported that recruitment had become more difficult in the past year—lower than the 76% in 2021—and more than a quarter (27%) said RN turnover had decreased.
Survey headlines
- More nurses are reporting incidents of workplace violence and are more satisfied with the responses to those reports.
- Two-thirds of respondents said their workload had increased in the past year.
- About 63% of nurse manager respondents reported an increase in open positions over the past 12 months, down from 71% in 2021.
- Recruitment for those open positions remains difficult, with 64% of managers reporting that they found it more difficult in the past 12 months, down from 76% in 2021.
- More than half (56%) of survey participants reported that they were emotionally healthy or very emotionally healthy, with 17% reporting they were not emotionally healthy.
- Nearly a third (31%) plan to seek new employment within the next 3 months.
- Salary remains an important consideration when choosing an employer—56% (vs. 65% in 2021) of respondents could be persuaded by an offer of more money to leave their current employer.
- Respondents work an average of 43 hours per week.
- More than a quarter of participants (27%) recently experienced a patient who refused to have them serve as their assigned nurse.
Respondents’ future career plans indicate that staffing difficulties may continue. Nearly a third (31%) were currently seeking a job with another employer or planned to in the next 3 months, up from 23% in 2021. When asked how long they plan to stay with their current employer, 38% indicated 5 years or more, compared to 40% last year. Nearly 13% plan to stay less than a year, with another 27% planning on 1 to 2 years. The top three reasons why nurses wanted to leave their employers were dissatisfaction with salary (29%), dissatisfaction with work environment (22%), and better schedule (22%). (Participants could choose up to three.)
Money matters
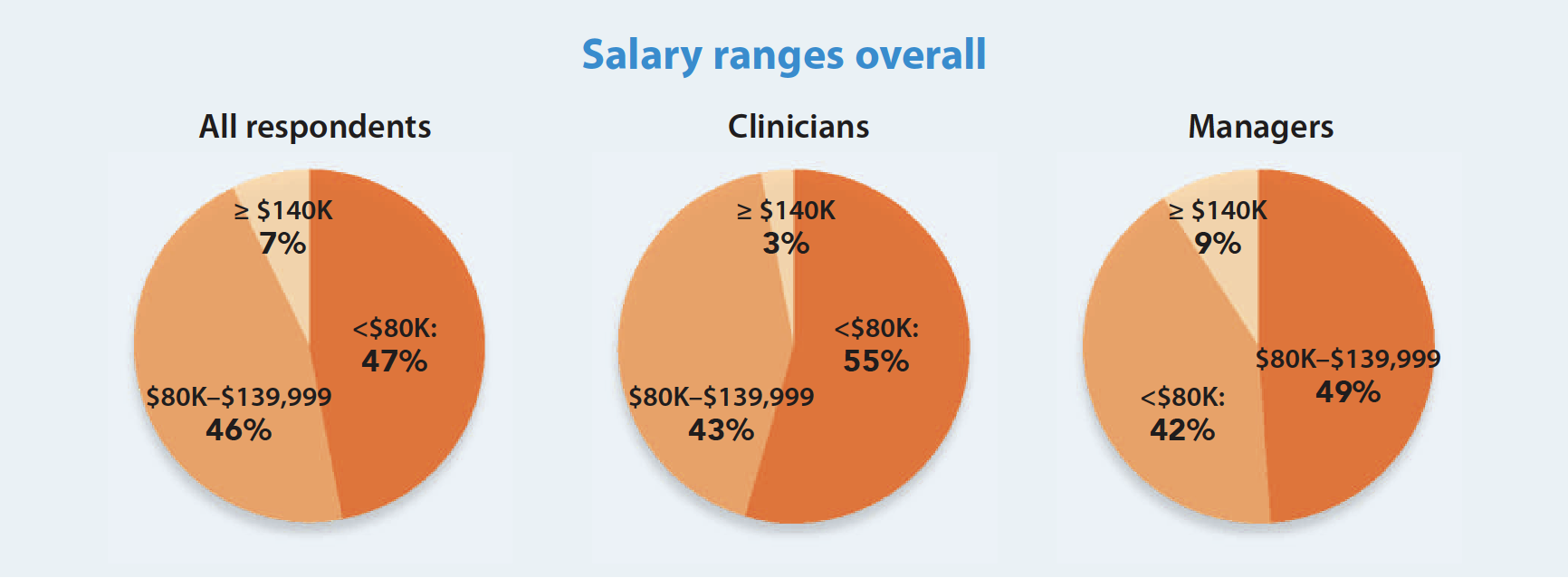
This year, 46% of nurses surveyed earned a salary between $80,000 and $139,999, up from 39% last year and 41% in 2020. Nearly half (47%) earn less than $80,000, and nearly two-thirds (62%) reported a higher salary compared to 12 months ago.

Raises reflect this trend toward higher salaries. More than half (54%) of respondents received a raise in the past year, with another 25% receiving one in the past 2 years. Clinicians were more likely than managers to have received a raise less than 1 year ago (66% vs. 45%).
The most common benefits respondents reported receiving were health insurance (60%), paid time off (58%), and dental insurance (54%).
As expected, those who work 35 hours or more a week receive more benefits. For example, 67% receive health insurance and paid time off. Other higher percentages included 60% for dental insurance, 55% for retirement benefits, and 51% for vision insurance.
About half (48%) of nurse managers received a discretionary bonus in the past 12 months, with another 23% receiving a nondiscretionary bonus; 7% received both. Nearly half (49%) of clinical nurses received additional compensation for shift work. Other areas where clinical nurses received additional compensation included certification (36%), charge nurse role (32%), serving as a preceptor (32%), education level (31%), and clinical ladder (22%).
Nurse manager perspectives
Almost half (48%) of nurse managers who responded to the survey had been in a management role for 5 years or less, and only 21% had 11 or more years of experience. Most (44%) reported that they supervise 10 or fewer employees, with 38% supervising between 11 and 30. In all, 42% had been with their current employer for 5 years or less, with another 28% falling in the 6- to 10-year time frame.


Most managers (68%) reported that their workload had increased in the past year, down from 78% in 2021. However, respondents carved out time to become certified—71% reported holding leadership certification, up from 27% in 2021 and 18% in 2020.
About half of nurse managers who responded to the survey held the position of charge nurse (29%) or nurse executive (chief nursing officer, chief nursing executive, or vice president of nursing, 23%), followed by director or assistant director (19%). One-fourth worked in an academic medical center. The highest levels of education were bachelor’s degree in nursing (27%) and master’s degree in nursing (26%).
Other interesting observations from manager respondents included the following:
- Nurse managers’ opinions are valued when it comes to purchasing decisions. Most (69%) survey participants said they’re members of a value-based purchasing committee or are involved in making purchasing decisions.
- Of the manager respondents, 21% were men, as opposed to 16% of respondents as a whole.
- Managers and clinicians have similar future plans about their current employers, with 38% of managers and 37% of clinicians indicating that they plan to stay in their jobs for another 5 years or more. Nearly a quarter (24% of managers and 23% of clinicians) plan to stay 3 to 5 years.
Clinician perspectives
Among clinician respondents, 44% reported a certification in their chosen specialty, up slightly from 39% last year, and 64% noted that their workload had increased in the past 12 months. Slightly more than half (53%) work 12-hour shifts on a regular basis.
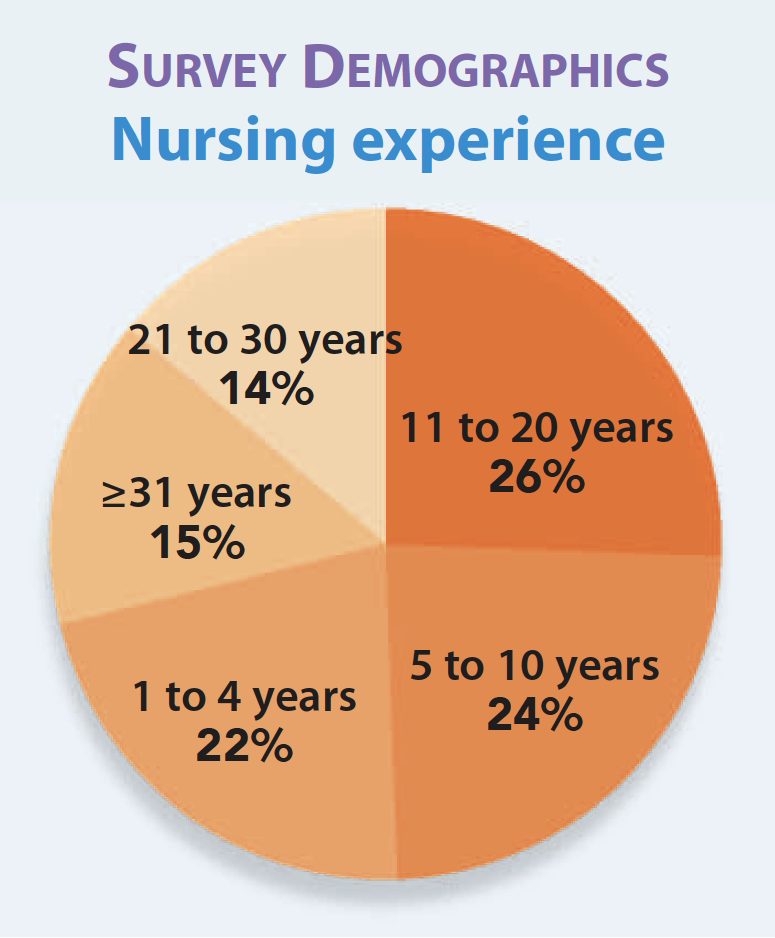

More than half (54%) of clinician respondents had worked for their employers 5 years or less, while 20% had been with their current employer for 6 to 10 years. In all, 23% work in a community hospital, with another 23% in academic medical centers, and 9% in teaching hospitals. More than half (58%) work in acute care, and the most common role was clinical staff nurse (52%). Medical–surgical was the most common specialty (16%), followed by critical or progressive care (11%). Most clinicians (44%) have a bachelor’s in nursing as their highest degree, with 23% having a master’s degree in nursing.
Most nurses view staffing committees as a positive way to address issues, but only 14% of clinician respondents serve on such a committee, and nearly half (48%) report that their organization doesn’t have one. That may be one reason why 51% of clinicians responded “no” when asked if staffing assignments were appropriate to meet patient needs at least 80% of the time.
Salary was the most common response when asked to choose the three most important aspects of nursing (71% chose this as one of their three options), but more than half also responded providing patient care (55%) and flexible hours (51%). In addition, 39% selected opportunity for career growth.
Manager and clinician differences
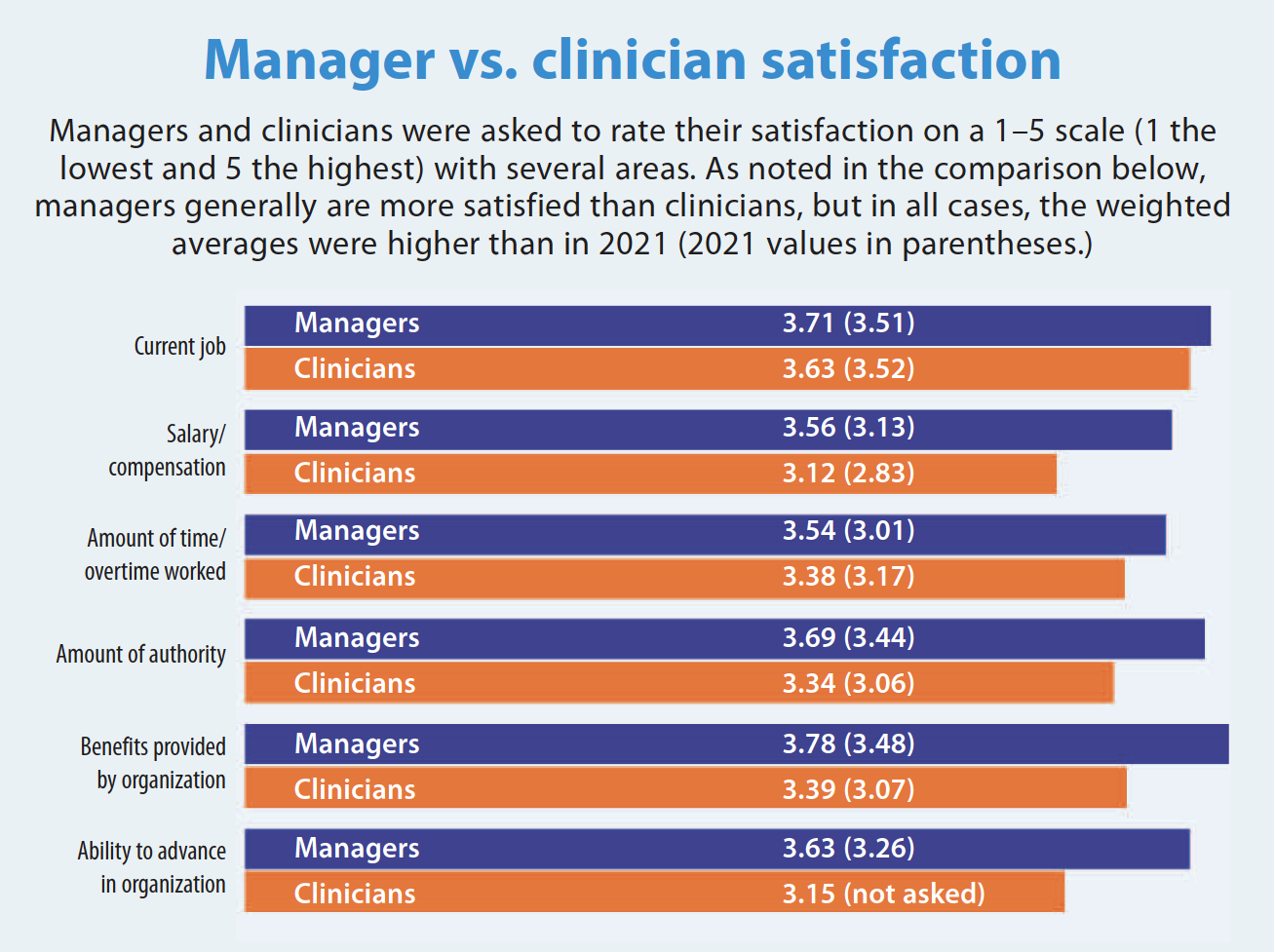
The survey revealed a few key differences between managers and clinicians. Overall, managers reported more satisfaction with their job, salary, benefits, amount of authority, and ability to advance in the organization. Managers also were more satisfied with the amount of time worked, compared to amount of overtime worked by clinicians. However, given that the highest weighted average among the responses was 3.78 on a 5-point scale, more work is needed to boost satisfaction in both groups.

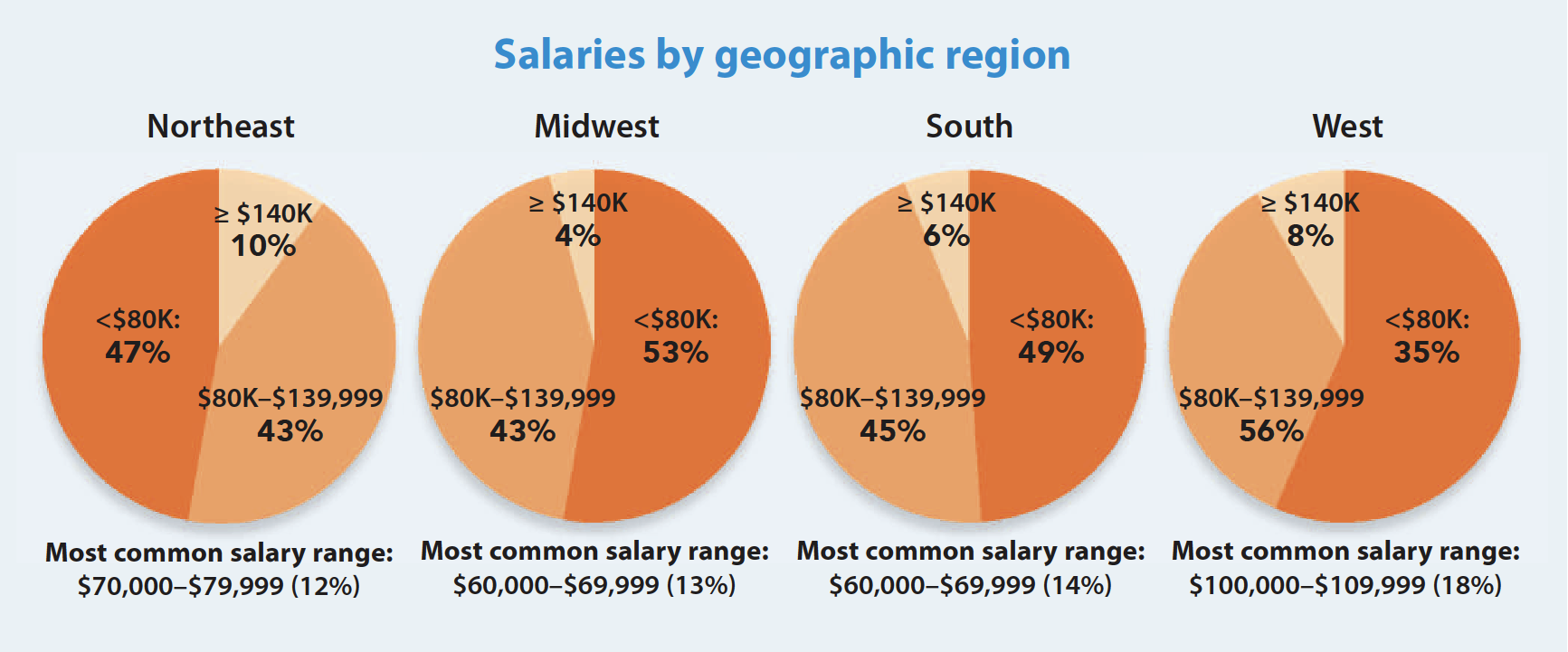
The survey showed increased salaries more often for clinicians than managers. In all, 43% of clinicians earn $80,000 to $139,999 per year, up from 33% in 2021. Nearly half (49%) of managers fall in this range, but that is a drop from 53% last year. Fewer than half (42%) of managers earn less than $80,000, compared to 55% of clinicians.

Other interesting differences include the following:
- Managers rated their emotional health slightly higher than clinicians (3.64 vs. 3.34).
- For the first time in the survey’s history, the percentage of certified nurse managers exceeded the percentage of certified clinicians (71% vs. 44%). Both results may reflect the growing importance of certification for career growth.
- More managers than clinicians currently attend school (32% vs. 18%)
- Each group answered “more money” when asked what would make them consider leaving their current employer, but the strength of the appeal differed (48% of managers vs. 65% of clinicians).
Workplace violence—Some improvement but more needed
This year’s responses to questions related to workplace violence indicate that The Joint Commission’s workplace violence–related mandate that went into effect in January 2022 might be having some impact. Compared to 2021’s survey, reporting of assault and bullying incidents was higher in every category except with regard to verbal assaults from patients. In addition, satisfaction with the response to a report increased significantly. For example, the percentage of those who were satisfied with the handling of a report of verbal assault or bullying from a manager increased from 18% in 2021 to 65% this year.
FEATURE SURVEY
Workplace violence: What nurses are saying
An additional sobering indication of continued violence was that two thirds (66%) of respondents reported they had witnessed someone being bullied in the past 2 years, up from 48% in 2021. Of those who witnessed an incident, more than half (53%) intervened, with saying something to the bully in public during the incident the most common response (52%), followed by speaking with the bully in private about the incident (40%) and reporting the incident to the manager (37%). (Respondents could choose more than one option.)
Comments from nurses confirm that violence remains a major concern, with many calling on it to stop and for legislation addressing the issue.
- “There is NEVER a good reason for nurses to experience violence in the workplace. I don’t care what excuse the attacker has, including mental status/health issues, it should never even occur to people that violence against a nurse is an option. However, since that isn’t the case, all nurses should be fully supported by their employer in reporting all violence to the appropriate authorities, and the perpetrator should be prosecuted.”
- “The hospital needs to proactively inform patients and families that verbal and physical abuse of nurses and other personnel will not be tolerated and the consequences to be expected if it occurs.”
- “The verbal abuse is getting worse, and there are days that you worry that it will escalate too physical assault.”
- “Sometimes the staff is unaware of their legal right against assault and battery, even from confused patients. This information needs to be part of orientation.”
- “All registered nurses and employers in all settings, including practice, academia, and research institutions, must work together to create a culture of respect, free from bad manners, bullying, and workplace violence.”
- “We suffer in silence.”
A few comments noted that organizations are addressing this issue:
- “My new place of work is much more supportive and responsive than the previous. We have police officers available on site, and they routinely round on the units and their numbers have been increased recently.”
- “Our manager is very serious about keeping our unit bully free from all aspects.”
- “My organization supports police reports and charges, is in the process of installing weapons detection systems, amnesty boxes at ED entrances, and increased signage regarding zero tolerance for violence.”
Satisfaction with organizational support also increased. When asked to rate the degree of support from their organization to reduce workplace violence on a scale of 1 to 5, with 1 being not supportive and 5 being completely supportive, the weighted average was 3.74, up from 3.3 in 2021. Nearly two-thirds (63%) said their organization was completely or somewhat supportive.
Nurses who experienced a workplace violence incident but didn’t report it were asked to select a reason why. The most common responses were that they did not think the incident was serious enough and they did not think anything would be done about the situation. However, when a manager verbally assaulted or bullied a nurse, the most common reason was fear of reprisal.
Encouraging nurses to report incidents and acting on those reports are key to addressing violence, but the ultimate goal is to stop violence from occurring in the first place. Survey results may indicate the elusiveness of that goal. Incidents of every type of assault or bullying were higher—sometimes significantly—compared to last year, particularly in the case of patients’ family members or visitors. Reports of verbal assaults or bullying by this group rose from 34% in 2021 to 41% this year and physical assaults rose from 3% to 14%. Other notable trends include the increase in the percentage of those reporting physical assaults by managers (from 1% to 11%) and the increase in the percentage of those reporting physical assault by another employee (from 3% to 12%). However, the increases also may reflect the increased willingness of nurses to speak up about violence and not represent an actual rise in incidents.
Continuing effects of COVID-19

Although COVID-19’s domination of the news cycle has faded, that doesn’t mean it’s not continuing to have a significant impact on individual nurses, staffing, and the profession. Two-thirds of managers reported that the pandemic had resulted in higher than usual staff shortages, and nearly half (48%) continue to tap into more temporary staff.
When asked how COVID-19 had changed their career plans, many responded that they had changed jobs and/or specialty (26%), no longer actively work in bedside nursing (24%), or plan to leave nursing sooner than expected (27%). Hundreds of nurses added comments, with most reflecting on the pandemic’s toll, as indicated by statements such as, “Less fulfilled with being a nurse,” “Emotional and physical burnout,” “I’ve had to assume more responsibility and work with less resources,” “The change in academia has taken the joy out of teaching,” and “Hospital staff are tired: Tired from working understaffed, lack of supplies, angry families that do not like to follow rules or do not like the rules implemented for safety in a pandemic environment.”
COVID-19: What nurses are saying
Although many respondent comments about the pandemic highlighted the negative effects, several noted positive comments, such as the following:
- “I have a greater sense of responsibility and purpose.”
- “It made me more determined to keep doing it.”
- “I have really started to put things in perspective as far as what’s really important in life.”
- “I have no intention of leaving my profession.”
- “I still love nursing.”
When it comes to organizations, participants reported an average satisfaction level of 3.49 (vs. 3.33 in 2021) on a scale of 1 to 5 in terms of their employers’ response to COVID-19, but only 35% felt “satisfied” with the response, compared to 75% in last year’s survey. In addition, only slightly more than half (56%) thought their organization was “well” or “extremely” prepared to handle a surge in patients from a pandemic, natural disaster, or another reason for a sudden influx of patients.
Committed and inspired
Most nurses remain committed to the profession, as indicated by responses to a question asking them to share their most inspiring experience within the profession from the past few years. Replies included the following:
- “Seeing the way our hospital staff and community came together to support each other during the pandemic was amazing!”
- “No matter how bad the pandemic was, [it] brought generations of nurses together. The older and very young nurses worked together in the greatest stress environment. They have now forged a trust with both the older and younger having a new-found respect for one another.”
- “I have so many! Working in a rural hospital with people you know is very personal. People remember that I cared for them, or their parents, or was there with them when their child was born. To be recognized on our unit as the ‘mom’ of the unit. Have worked at my employer for 55 years!”
- “I have seen some younger nurses, few though they are, handle this difficult situation with grace and skill. They impress me. We need more!”
- “Nursing being recognized by the general public as ethical providers and legislation to allow us to work to the fullest extent of our licenses.”
- “It has been gratifying to work with clients from cultures and languages who tell me that they feel heard and understood. I feel encouraged to be a part of removing the stigma from mental illness in minority groups.”
- “The bedside staff’s ability to rally for the patient’s care despite being grossly understaffed, exhausted, and underpaid. There are so many resilient, compassionate nurses, patient care techs, and support staff that have sacrificed their own comfort and needs to better that of our patients. They inspire me every day and are the reason that I LOVE being a nurse.”
We at American Nurse Journal thank you for what you do every day for your patients, students, colleagues, and general public.
Cynthia Saver is president of CLS Development, Inc., and editor of Anatomy of Writing for Publication for Nurses, 4th Ed. Her blog, The Writing Mind, is available at myamericannurse.com/category/the-writing-mind.
American Nurse Journal. 2023; 18(1). Doi: 10.51256/ANJ012313
Key words: nursing trends, nursing salaries, survey, nurse clinicians, nurse managers, job satisfaction, workplace violence