Learn how to recognize and intervene for patients with these electrical heart abnormalities.
Ventricular arrhythmias—the mere words may sound scary, even to a nurse. After all, these arrhythmias are a leading cause of sudden cardiac death. This article demystifies ventricular arrhythmias to help you gain confidence when caring for patients who have these electrical abnormalities.
A review of the heart’s electrical conduction system can enhance your understanding of how ventricular arrhythmias arise. All cardiac cells initiate impulses. The sinoatrial (SA) node, the heart’s intrinsic pacemaker, generates impulses faster than other cardiac cells. Impulses originating in the SA node travel through various pathways within the atria to the atrioventricular node, then through the bundle of His, down through the right and left bundle branches and into the Purkinje fibers. Here, the impulses cause the ventricles to contract.
The heart functions best when impulses follow this normal pathway, producing adequate cardiac output and perfusion to the coronary vessels and organs. Problems arise when impulses deviate from this pathway. An impulse generated by the ventricles, for instance, produces less effective and less efficient ventricular contractions. As a result, cardiac output drops, which decreases perfusion to major organs, leading in turn to tissue ischemia and eventually, tissue damage.
Factors contributing to ventricular impulse generation include myocardial ischemia, electrolyte imbalances (especially a low potassium level), hypoxemia, acidosis, drug overdose or toxicity, bradycardia, cardiomyopathy, and cardiac disease. Ventricular arrhythmias also can occur in a healthy heart, brought on by smoking, excessive caffeine consumption, and certain other factors.
Assessment
If your patient has a known or suspected ventricular arrhythmia, evaluate blood pressure and mean arterial pressure (MAP). Systolic pressure above 100 mm Hg and MAP above 60 mm Hg indicate good cardiac output. In this case, the patient may lack adverse effects from the arrhythmia. The skin may be warm, dry, and of normal color; the patient may not complain of chest pain and lack signs and symptoms of heart failure.
In contrast, a patient with compromised cardiac output and poor perfusion appears pale, gray, or dusky and complains of chest pain or shortness of breath. Be aware that confusion, dizziness, mental-status changes, and decreasing urinary output indicate decreased cardiac output.
Premature ventricular contractions
When an irritable cell in the ventricle (frequently called a focus) fires and initiates an impulse, a ventricular contraction occurs. This contraction, which occurs early (prematurely) in the electrical cycle, isn’t part of the normal electrical pattern initiated by the SA node; it’s termed ectopic. A premature ventricular contraction (PVC) is an early contraction initiated by the ventricles. Unlike normal contractions, PVCs appear wide and bizarre on the electrocardiogram (ECG).
PVS may be unifocal or multifocal. Unifocal PVCs arise from the same irritable site in the ventricle. Multifocal PVCs result from irritation in multiple ventricular cells; each contraction looks different on the ECG. (See the waveforms below.)
Unifocal PVCs
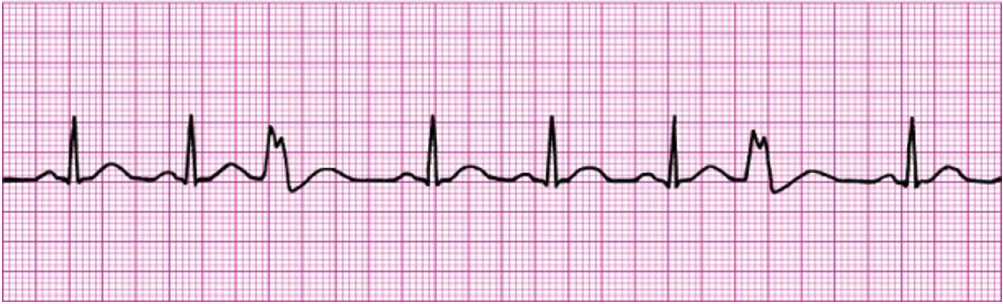

Multifocal PVCs
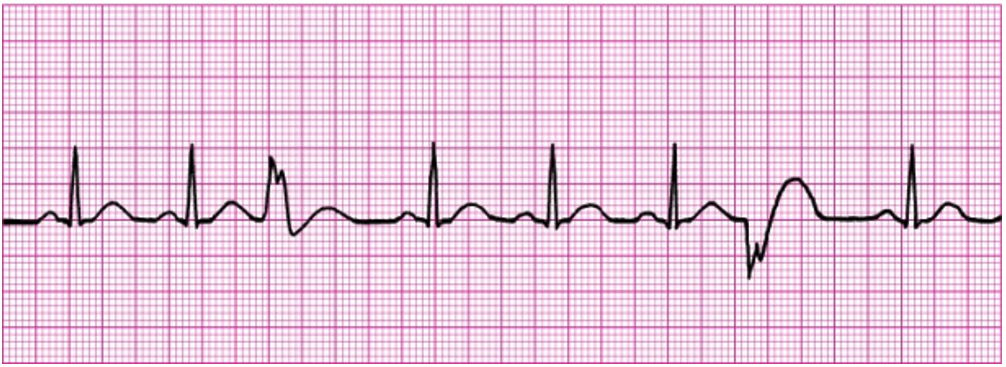

PVCs can occur in both normal and diseased hearts. Differentiating benign PVCs from dangerous ones is an important nursing responsibility. Danger signs include:
- PVCs occurring in groups of two or more
- PVCs of increasing frequency; for example, a jump from three or four PVCs to 10 or 12 PVCs an hour later
- PVCs occurring near the T wave (“R on T” phenomenon).
R on T phenomenon
Every normal QRS complex has a P wave, a QRS complex, and a T wave. The P wave represents atrial contraction; the QRS complex, ventricular contraction; the T wave, repolarization. During repolarization, heart cells prepare for the next impulse. During the contraction and early repolarization phases of the cardiac cycle, cardiac cells can’t respond to a stimulus, no matter how strong. Called the absolute refractory period, this phase protects the heart and allows cells to prepare for the next impulse. The absolute refractory period starts from the end of the P wave and extends to approximately the middle of the T wave.
The remaining portion of the T wave is the relative refractory period. During this period, the heart isn’t quite ready to respond, but a stimulus that’s strong enough can cause a contraction. However, the cardiac cells are irritable and commonly respond by causing a life-threatening rhythm, such as ventricular tachycardia or ventricular fibrillation.
Managing PVCs
PVC management varies with the cause and whether the PVCs pose a danger. Suppressing PVCs without treating the cause is dangerous; the PVCs may return or the rhythm may deteriorate to a more serious one.
Check for likely causes of your patient’s PVCs. Administer oxygen as ordered, check electrolyte levels, and obtain orders for other treatment. Antiarrhythmic drugs occasionally are used to control PVCs; these may include amiodarone, beta blockers, and calcium channel blockers. Be aware that when used to treat PVCs, these drugs must be given in an evenly spaced dosing pattern to maintain a blood level that suppresses the arrhythmia.
Ventricular tachycardia
Ventricular tachycardia is defined as three or more PVCs in a row. (See the waveform below.) When a single cell within the ventricles fires repeatedly at a fast rate (greater than 120 beats/minute), this overrides the SA node’s control of the electrical conduction system. Ventricular tachycardia is a life-threatening arrhythmia.
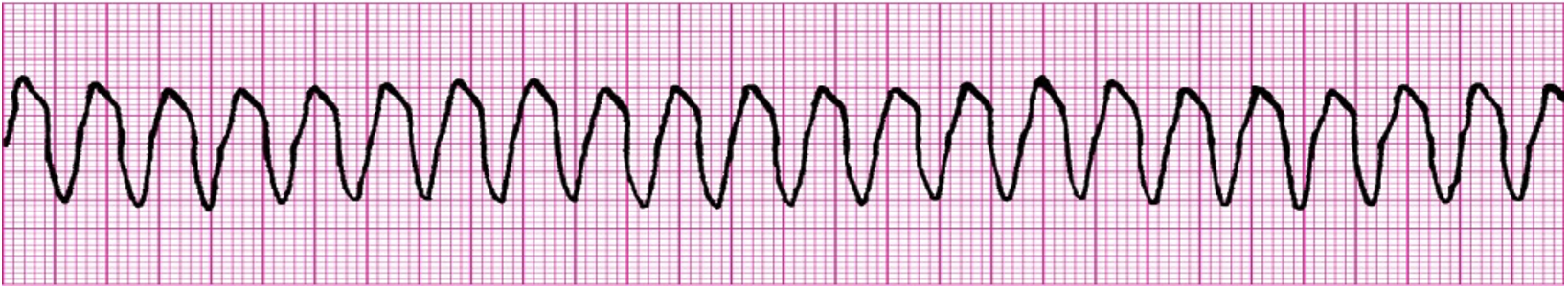

Several types of ventricular tachycardia exist, all of them potentially dangerous. Sustained ventricular tachycardia lasts 30 seconds or longer. Nonsustained tachycardia occurs when the tachycardia terminates itself before 30 seconds.
Some patients with ventricular tachycardia have a pulse; others are pulseless. Always assess the patient before deciding what action to take. First determine if the patient has a pulse. Pulseless ventricular tachycardia requires the same treatment as ventricular fibrillation (described below). To determine if the patient is stable or unstable, evaluate blood pressure and MAP to gauge whether perfusion to major organs is adequate. Stable patients with adequate cardiac output generally receive antiarrhythmic drugs. Unstable patients require synchronized cardioversion to immediately terminate ventricular tachycardia; antiarrhythmic drugs aren’t given because they can cause further decompensation with loss of blood pressure and pulse. Remember—all drugs used to treat ventricular tachycardia decrease blood pressure. If the patient had low blood pressure before receiving the drug, pressure will drop even more after the dose, further compromising cardiac output and organ perfusion. In most cases, synchronized cardioversion is used to rapidly convert unstable ventricular tachycardia to a sinus rhythm, thus reestablishing cardiac output and organ perfusion.
Ventricular fibrillation
Ventricular fibrillation is a chaotic rhythm with no discernible waves or complexes. (See the waveform below.) Multiple sites within the ventricles fire simultaneously, but none of this electrical activity produces effective contractions or cardiac output. Lacking both circulation and cardiac output, the victim is in cardiac arrest and requires immediate defibrillation to reestablish a normal heart rhythm. While chest compressions can buy some time in ventricular fibrillation (or pulseless ventricular tachycardia), the most crucial treatment is defibrillation. (Keep this verse in mind: To treat v fib, always defib.) Defibrillation “stuns” the heart, stopping all electrical activity and giving the SA node a chance to reestablish control over the conduction system and restore a normal sinus rhythm.
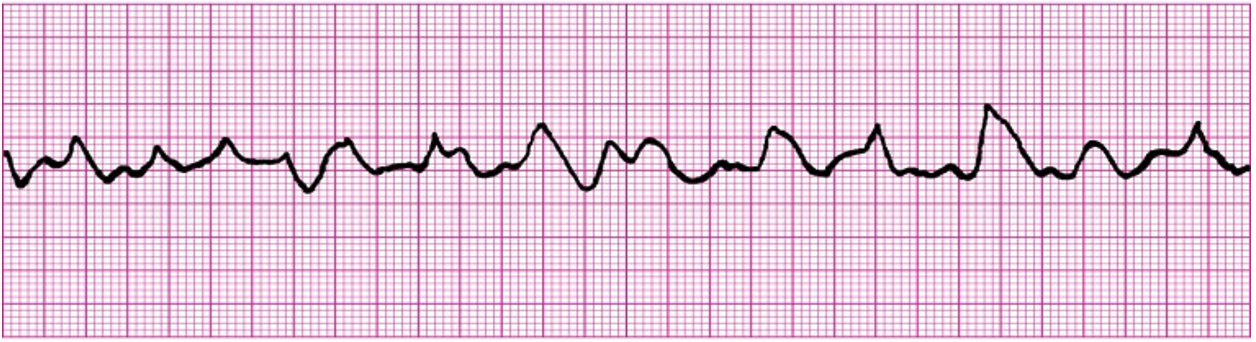

Two types of defibrillators are available—monophasic (the traditional type) and biphasic. Monophasic defibrillators deliver a shock in a single direction; the energy travels from one electrode to another. Biphasic defibrillators deliver energy in two directions. First they send energy from one electrode to the other (like a monophasic defibrillator); then, in a second phase, the energy reverses direction and travels in the opposite direction. This process allows effective stunning of the myocardium at lower energy settings, sparing myocardial tissue from damage caused by higher energy settings.
The 2010 American Heart Association (AHA) Advanced Cardiac Life Support (ACLS) guidelines for ventricular fibrillation recommend a pattern of a single shock followed by 2 minutes of cardiopulmonary resuscitation (CPR). Chest compressions should continue while the defibrillator is charging, with each shock immediately followed by chest compression. Evidence shows that a period of chest compressions after defibrillation produces more effective defibrillation. After defibrillation, the heart usually is unable to produce an effective cardiac output even if the rhythm changes to a normal sinus rhythm. The heart needs the support of chest compressions to perfuse body tissues.
After 2 minutes of CPR, check the patient’s heart rhythm on the monitor; if ventricular fibrillation (or pulseless ventricular tachycardia) persists, deliver a second shock. Remember—chest compressions should continue while the defibrillator is charging. Reducing the interval between the last compression and the shock may make the defibrillatory shock more effective.
Asystole
Asystole is absence of a heart rhythm. (See the waveform below.) The heart is silent, with no electrical activity and no contractions. Neither cardiac muscle cells nor the electrical conduction system are functioning. Occasionally, some atrial activity may appear on the monitor as P waves without a QRS complex, called ventricular standstill.
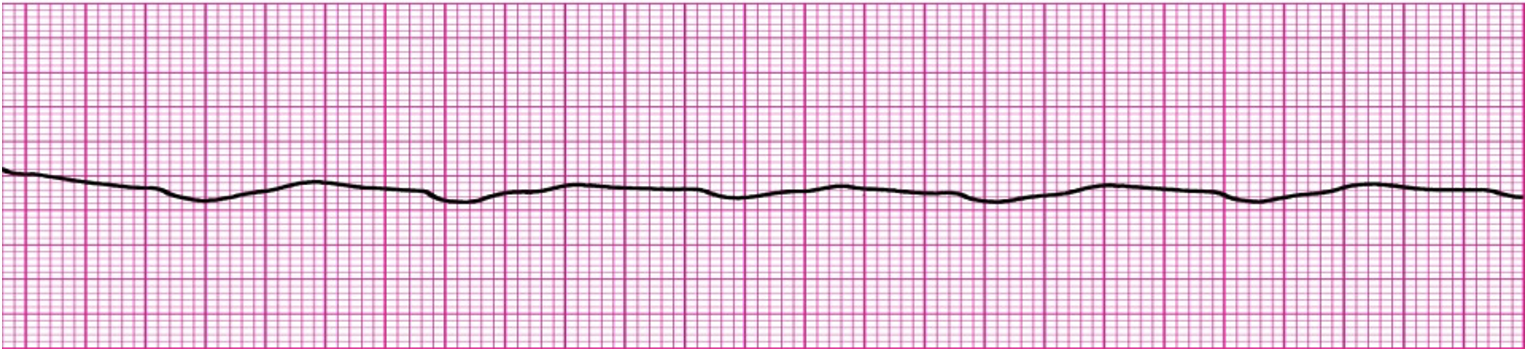

Lack of QRS complexes means no contractions and no cardiac output. So the first and most important intervention for asystole is to perform effective chest compressions. (Defibrillation is contraindicated because a heart that’s silent and not contracting doesn’t need to be stunned.) The objective is to move blood and produce cardiac output so as to perfuse the tissues; that’s why continuous effective CPR is so important. The patient also should receive drugs that stimulate the heart, such as epinephrine or vasopressin.
The cause of asystole must be identified and treated rapidly to avert death. AHA’s ACLS algorithm classifies potential causes of asystole as the “Hs” and “Ts”.
- H stands for hypovolemia, hypoxia, hydrogen ion (acidosis), hypokalemia, hyperkalemia, hypoglycemia, and hypothermia.
- T stands for toxins, tamponade (cardiac), tension pneumothorax, thrombosis (coronary or pulmonary), and trauma.
In some cases, the cause isn’t treatable and the healthcare team must make the final decision as to when to stop resuscitation efforts.
Caring for patients with ventricular arrhythmias is challenging because many are in a life-threatening situation. Early recognition and quick action give them the best chance to survive.
Selected references
2010 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiac Care Science. Circulation. 2010 Nov 2;122(18):S676-705.
Gahart BL, Nazareno AR. 2012 Intravenous Medications: A Handbook for Nurses and Health Professionals. 28th ed. St. Louis, MO: Mosby; 2011.
McCance KL, Huether SE. Pathophysiology: The Biologic Basis for Disease in Adults and Children. 6th ed. St. Louis, MO: Mosby; 2009.
Walraven, G. Basic Arrhythmias. 7th ed. Upper Saddle River, NJ: Prentice Hall; 2010.
Mary Jo Lombardo is clinical education program manager at Howard County General Hospital in Columbia, Maryland.




















3 Comments.
this is EXCELLENT. thanks
very good and thanks
good article, thanks for sharing; i learned alots from this article. please continue to post more.
thanks.