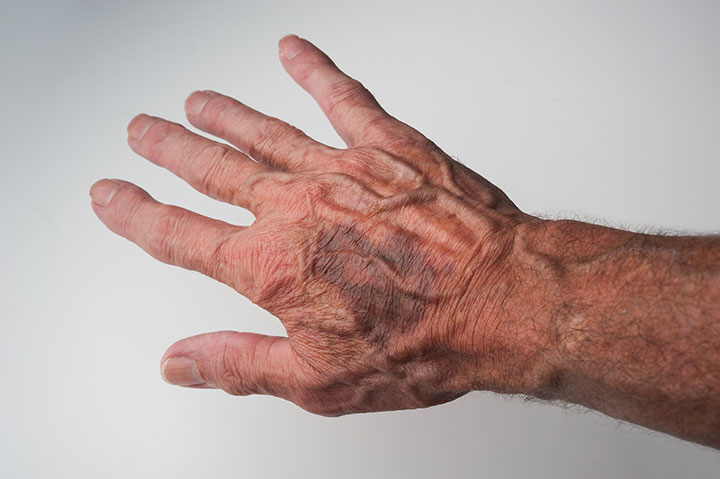
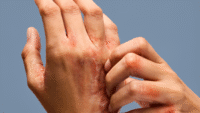
Bruises, grip marks, and lacerations are just some of the indications of elder abuse.
By Armi S. Earlam, DNP, MPA, BSN, RN, CWOCN; Lisa Woods, MSN, RN-BC, CWOCN; and Kari Lind, BSN, RN
Takeaways:
- Physical, psychological, emotional, financial, and sexual abuse are the most common types of elder abuse.
- A nurse’s purposeful interviewing skills and thorough skin assessment are crucial to identifying abuse among the elderly patients, no matter the care setting.
- Competency in skin assessment coupled with excellent interview skills will help a nurse identify abuse and protect the elderly patients.
Every year, approximately 4 million older Americans fall victim to abuse and neglect. And for every reported case of elder abuse and neglect, approximately 23 cases go undetected. About 90% of elder abuse is committed by a family member in the home, with the other 10% committed by hired caretakers, intimate partners, or healthcare workers in long-term care facilities. In some cases, the elderly person is neglecting or abusing him- or herself.
The consequences of elder abuse include increased risk of death, poor health outcomes, decreased quality of life, high costs of care, physical injury, and retaliation from elders on the abusers. In the United States, the annual cost of health conditions related to elder abuse is about $5.3 billion. (See Elder abuse defined)
Risk factors for elder abuse include caregiver stress; fatigue; dissatisfaction; a family history of violence or alcohol or other substance-abuse disorder; psychological impairment; poor impulse control; lack of knowledge of duties and resources; and caregiver dependency (for example, financial or housing dependence). In some cases, the caregiver may be retaliating against the victim, who may have been an abuser in the past.
Several tools can be used to screen patients you suspect are victims of elder abuse. This article focuses on skin assessment.
Elder abuse definedThe most commonly cited definition of elder abuse was developed by the Action on Elder Abuse in the United Kingdom: “Elder abuse is a single or repeated act or lack of appropriate action, occurring within any relationship where there is an expectation of trust, which causes harm or distress to an older person.” Physical, psychological, emotional, financial, and sexual abuse are the most common types of elder abuse. Physical abuse Sexual abuse Neglect |
Screening tools
The various tools used to screen for elder abuse aim to identify multiple forms of abuse. Unfortunately, no gold standard exists. This lack of consensus, combined with lack of training, the need for tool validation, and time constraints have led to inconsistent screening practices among healthcare professionals.
Three tools highlighted in the 2013 Elder Maltreatment Symposium convened by the Centers for Medicare and Medicaid Services are the Elder Abuse Suspicion Index© (EASI), the Hwalek-Sengstock Elder Abuse Screening Test (H-S/East), and the Vulnerability to Abuse Screening Scale (VASS). The first two tools have six items and the last one has 12. They all have completed psychometric validation. The symposium chose these tools based on their benefit potential and to promote increased use. Of the three tools, only the EASI mentions skin, asking if the provider has observed hygiene issues, cuts, or bruises over a 12-month period.
You can find additional information about screening tools at the National Center on Elder Abuse website (eldermistreatment.usc.edu/wp-content/uploads/2016/10/Elder-Abuse-Screening-Tools-for-Healthcare-Professionals.pdf).
What to look for during skin assessment
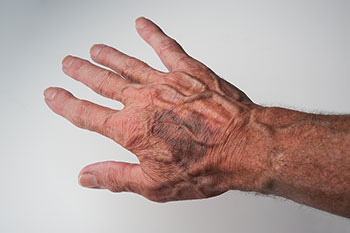

If a patient presents with physical injuries, start with open-ended questions to determine how the injuries occurred. If the patient is with a caregiver, talk to the patient alone so he or she can speak freely. However, if the caregiver wishes to stay with the patient, don’t assume abuse exists; the patient may depend on the caregiver for remembering instructions. Note any inconsistencies between the injuries and the patient’s or caregiver’s explanation about how they occurred. Other clues that may surface during the interview include seeking help from more than one emergency department for repeated injuries or a dismissive attitude about the injuries.
Your full-body skin assessment should include the genitals. Look for bruises or grip marks around the arms or neck, rope marks or welts on the upper or lower extremities, lacerations, traumatic alopecia, and repeated unexplained injuries. Bruises, fractures, and other injuries at various healing stages also are warning signs. Burns in a stocking or glove distribution may indicate immersion burns. Other red flags include cigarette burns, foul-smelling pressure injuries, and pressure injuries outside of the sacral and lumbar areas.
Look for defensive injuries on the back of the patient’s dominant hand. Some skin lesions may resemble implements used (such as a shoe, belt buckle, or stick) when the perpetrator hit the victim.
Signs of sexual abuse include new-onset sexually transmitted diseases in elderly patients who are cognitively impaired and can’t give consent, genital injuries, torn or stained underwear, genital bleeding or pain, difficulty ambulating without obvious reasons, anal bleeding, and bruised breasts or buttocks. Note that sexual abuse, which is the least-reported type of abuse among the elderly, also includes inappropriate photographing of the person in suggestive poses, forcing an individual to look at pornography, and coerced nudity. These other forms of abuse may be revealed during the interview.
Other abuse signs to watch for include dehydration, malnutrition, poor dental health, exacerbation of medical conditions due to medication withholding, and failure to follow up with medical providers. Foul odors (such as “body odor” and urine or ammonia smells), soiled or inappropriate clothing (such as thin clothing during cold weather), poor hygiene, and evidence of denuded skin on the perineum or buttocks also are signs of abuse and neglect.
Nursing implications
Your first priority is to ensure that the patient is safe. Follow your institution’s protocol for handling suspected abuse and neglect, which may include contacting law enforcement.
Document patient, witness, and suspected abuser statements verbatim, without offering your opinion. Your documentation may be used in court if charges are brought against the abuser. Depending on the facility, you may be required to photograph wounds. Make sure the photographs are clear and properly labeled.
Reporting to law enforcement varies by state. For example, abuse in a community setting may require referral to adult protective services, while abuse that happens in an institutional setting may be referred to an ombudsman. Follow your organization’s policies and the reporting rules outlined by the state where you work.
Failure to report elder abuse can result in civil or criminal charges. Healthcare professionals who don’t report abuse also may risk professional disciplinary action, including losing professional licenses.
Protect elderly patients
Elder abuse is a complex issue with various causes. The staggering number of undetected cases and subsequent detrimental consequences warrant action by nurses and other healthcare professionals. Competency in skin assessment coupled with excellent interview skills will help you identify abuse and protect your elderly patients. Learn the risk factors for elder abuse and take part in identifying and reporting it according to your organization’s rules and your state’s laws.
Armi S. Earlam is the lead certified wound, ostomy and continence nurse at Lutheran Medical Center in Wheat Ridge, Colorado. Lisa Woods is a certified wound, ostomy and continence nurse at Lutheran Medical Center in Wheat Ridge, Colorado. Kari Lind is an RN working in wound and ostomy care.
Selected references
American Psychological Association. Elder Abuse & Neglect: In Search of Solutions. 2012.
Cannell MB, Jetelina KK, Zavadsky M, Gonzalez JM. Towards the development of a screening tool to enhance the detection of elder abuse and neglect by emergency medical technicians (EMTs): A qualitative study. BMC Emerg Med. 2016;16(1):19.
Centers for Disease Control and Prevention. Understanding Elder Abuse: Fact Sheet. 2016.
Danesh MJ, Chang AL. The role of the dermatologist in detecting elder abuse and neglect. J Am Acad Dermatol. 2015;73(2):285-93.
De Donder L, De Witte N, Brosens D, Dierckx E, Verté D. Learning to detect and prevent elder abuse: The need for a valid risk assessment instrument. Procedia Soc Behav Sci. 2015;191:1483-8.
Department of Health and Human Services. A Profile of Older Americans: 2016.
Hoover RM, Polson M. Detecting elder abuse and neglect: Assessment and intervention. Am Fam Physician. 2014;89(6):453-60.
National Center on Elder Abuse. Elder Abuse Screening Tools for Healthcare Professionals. 2016.
New York State Nurses Association. Position statement: Elder abuse, neglect and maltreatment.
Pickering CE, Phillips LR. Development of a causal model for elder mistreatment. Public Health Nurs. 2014;31(4):363-72.
Sooryanarayana R, Choo WY, Hairi NN. A review on the prevalence and measurement of elder abuse in the community. Trauma Violence Abuse. 2013;14(4):316-25.