What nurses know can help them prepare.
- In 2020, polio and small pox reemerged in the United States.
- No cure exists for polio, but it can be safely and effectively prevented with vaccination.
- The World Health Assembly declared small pox eradicated in 1980 and no naturally occurring cases have been identified since.
- Education and awareness of vaccines can help prevent future outbreaks.
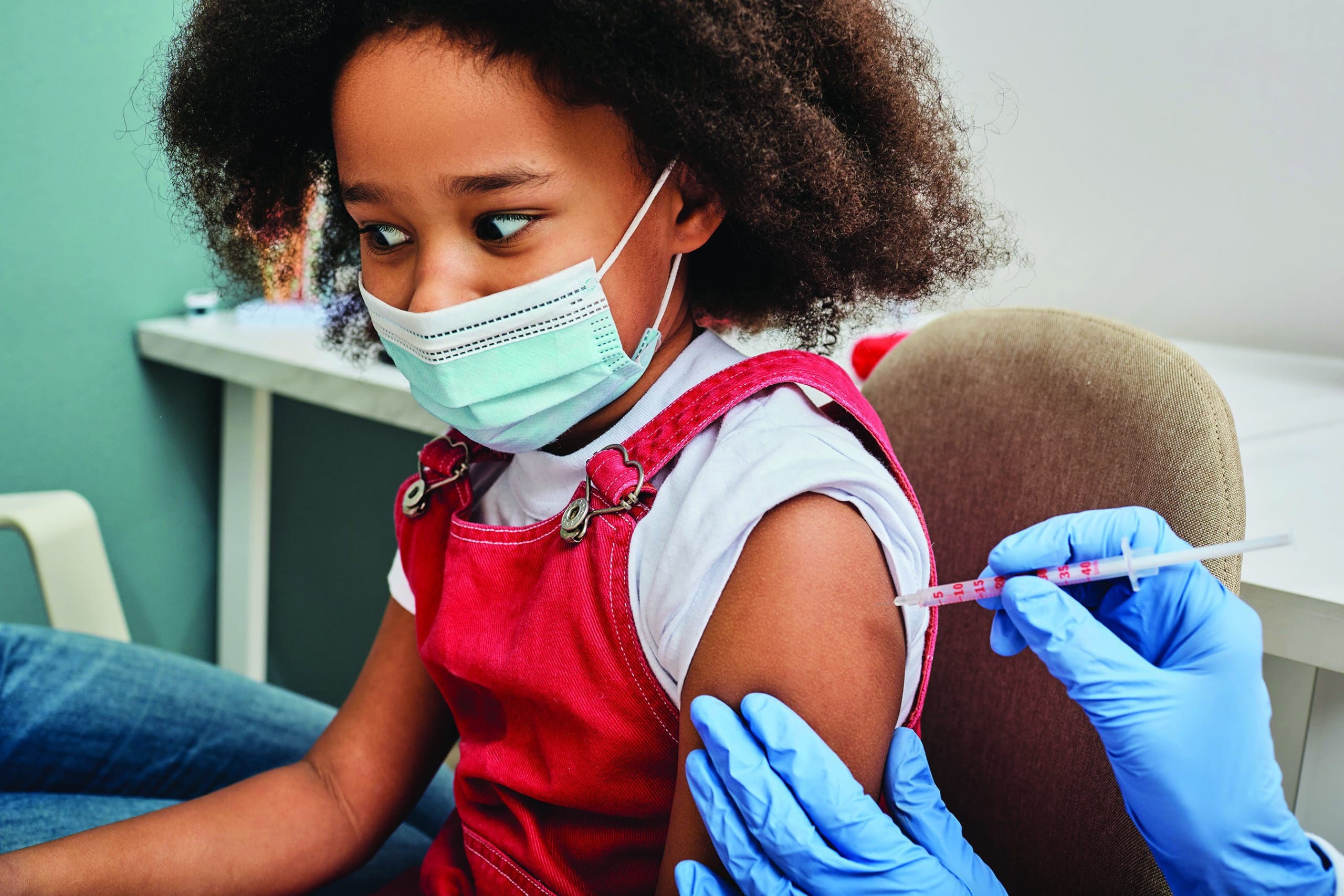
The 2022 reemergence of polio and smallpox in the United States has many healthcare providers wondering if they should prepare for a potential outbreak. Nurses need to know what lies ahead and how best to protect themselves and their patients if they encounter either of these viruses in their practice. (See 2022 outbreak.)
2022 outbreak
For decades in the United States, we haven’t worried about polio. However, in July 2022, an unvaccinated New York man who developed poliomyelitis was hospitalized with the virus. According to Backman, the patient came into contact with someone who had a vaccine-derived poliovirus infection. Vaccine-derived poliovirus is a strain related to the weakened live poliovirus contained in oral polio vaccine. The United States stopped using the oral vaccine more than 20 years ago because it contains live virus that can—in rare circumstances—mutate and become virulent.
In August 2022, the New Jersey Department of Health detected poliovirus in sewage water samples in several New York locations, which indicated that the virus had been silently circulating for months. According to the Polio Global Eradication Initiative, the United States reported 20 cases of wild poliovirus type 1 in 2022. Public health officials urged all New Yorkers to get vaccinated. Those same officials believe that the reemergence of the polio virus originated in a country that still uses the oral polio vaccine.
Polio
Polio (caused by the poliovirus), a disabling and potentially deadly disease, was one of the most feared diseases of the 20th century. It resulted in hundreds of thousands of paralysis symptoms in children.
Although no cure exists for polio, it can be prevented with a safe and effective vaccine, which was developed in the 1950s and 1960s. People who have never been vaccinated against polio are at highest risk of contracting and becoming sick from poliovirus; the risk of severe disease and death increases with age.
How polio spreads
Polio, which is very contagious, can be transmitted immediately before but usually 1 to 2 weeks after an infected person develops symptoms. Because the virus lives in the throat and intestines, it can be spread by both the fecal and oral routes. In unsanitary conditions, the virus can contaminate food and water.
Signs and symptoms
Polio frequently goes undetected because many people experience no symptoms or it’s misdiagnosed as the flu due to symptom similarity (GI distress, fever, fatigue, gastroenteritis, body aches). According to Backman, 200 to 1,000 people who become infected with the poliovirus will develop poliomyelitis (paralytic polio or acute flaccid paralysis), which places them at risk for developing delayed post-polio syndrome with a range of outcomes—from mild disability to acute respiratory failure and death.
According to the Centers for Disease Control and Prevention (CDC), one out of four people with polio will present with flulike symptoms, which usually last 2 to 5 days and then resolve on their own. Less than 1% of infected individuals present with weakness or paralysis. The incubation period for nonparalytic symptoms ranges from 3 to 6 days. If the virus reaches the spinal cord or brain, the patient may experience paralysis or meningitis; paralysis typically occurs 7 to 21 days after infection.
Eradication
Polio eradication requires rapid detection and interruption of any new outbreaks; strengthened routine immunization (the best defense against polio); community outreach and education; strategies to reach children from mobile and migrant populations, those in conflict zones, and those in remote regions; sensitive surveillance (testing sewage or other environmental samples for the presence of poliovirus, especially in hard-to-reach areas); financial resources; and political commitment from national governments and multilateral institutions.
Today, poliovirus is no longer endemic in the United States, but all healthcare providers, including nurses, must be familiar with its symptoms and rule out poliovirus infection in cases of unexplained acute flaccid paralysis, especially in patients with anterior myelitis, for quick identification and investigation. Since 1979, according to the CDC, no cases of wild polio (naturally occurring virus circulating in a community) have been acquired in the United States. An imported case occurred in 1993, and poliovirus infections still occur outside of the United States and can easily be brought here.
Exposure risk and vaccination recommendations
All healthcare workers have a high risk for exposure to polio if a patient has polio or has been in close contact with a person who might be infected with poliovirus. Unvaccinated adults are at the highest risk of contracting the virus. The CDC urges everyone who isn’t fully vaccinated against polio to complete the vaccination series as soon as possible to help protect themselves.
Since 2000, only the inactivated polio vaccine has been administered in the United States. The CDC recommends that all children get four doses as part of the routine childhood vaccination schedule. Most adults living in the United States are presumed to be protected against polio because they should have received routine childhood immunization and are considered to have only a small risk of exposure to poliovirus. Adults who aren’t vaccinated or are at high risk for exposure should talk to their provider to understand their risk and the need for polio vaccination. (View CDC polio vaccine recommendations at cdc.gov/vaccines/vpd/polio/public/index.html.)
Nursing implications
The nursing assessment for a patient with polio includes obtaining vaccination and travel histories and any contact with recently returned travelers. Assess the patient for possible signs and symptoms of polio (fatigue, fever, muscle weakness, severe headache, nausea, muscle wasting, sore throat, stomachache, loss of appetite, vomiting, neck pain, aches or stiffness in the arms or legs, deceased reflexes, intense pain, tingling or pricking sensations, muscle spasms or twitching, extreme sensitivity to touch, and paralysis).
Some nursing interventions related to a polio diagnosis include promoting nutritional and fluid intake; monitoring respiratory rate, rhythm, depth, effort, and breath sounds; elevating the head of the bed; and assessing for airway clearance. In infants, thermoregulation is critical, so reduce or eliminate the source of heat loss and monitor their body temperature.
Smallpox
Smallpox has a long history around the world of causing illness and death. According to the CDC, outbreaks continue to occur from time to time. However, due to successful vaccination, the last natural outbreak of smallpox in the United States occurred in 1949. In 1980, the World Health Assembly declared smallpox eradicated, and no cases of naturally occurring smallpox have been identified since.
Early efforts to control the disease included variolation, an inoculation process that involved exposing people to material from smallpox sores via inhalation or scratching it into their arm. Most people who received variolation developed a fever and a rash, typical symptoms associated with smallpox. According to Riedel, variolation was the most successful method for combatting smallpox before the discovery of a vaccine. Results included a milder form of the disease and a 2% to 3% fatality rate compared to natural smallpox infection, which had a fatality rate of 20% to 60%. Variolation risks involved developing disseminated smallpox and then spreading it to others, as well as the potential for transmitting other bloodborne diseases such as syphilis.
How smallpox spreads
Smallpox spreads primarily via direct and prolonged face-to-face contact. The incubation period, during which the individual isn’t contagious, usually ranges from 10 to 12 days but can be 7 to 17 days. The prodromal phase lasts 2 to 4 days and includes symptoms such as fever or macular rash. When the first sores appear in the mouth and throat, people are contagious and can spread the virus when they cough or sneeze. Scabs from the smallpox sores and related fluid contain the variola virus, so patients remain contagious until the last scab separates from the skin. Smallpox also can be transmitted via objects such as clothing or bedding. It’s rarely spread through the air in enclosed settings or buildings. Only humans can spread smallpox; no evidence exists that it’s spread by insects or animals.
Signs and symptoms
The clinical presentation of smallpox includes a fever (101° F to 104° F [38° C to 40° C]), severe headache, backache, pharyngitis, nausea, vomiting (rare), prostration, and enanthema (ulcers or eruptions) on the mucous membranes of the tongue and oropharynx. A macular rash (flat, red area) may occur in fair-skinned individuals. The virus can be found in respiratory secretions, skin lesions, and contaminated objects for a few days. The characteristic smallpox rash (firm, sharply raised, usually round sores that become pustules) begins after the prodromal phase. It first appears on the face of an infected person and is characterized by small red macules that later spread to the extremities and the trunk. As the rash appears, the fever reduces, leaving the patient feeling better. By the third and fourth day of the rash, it appears as raised papules filled with a thick, opaque fluid, which may resemble a bellybutton with a depression in the center (the distinguishing appearance of smallpox). The fever frequently rises at this time and remains elevated until scabs form over the papules. By days 4 to 7, lesions develop into pustules and grow in size until around day 10. About 2 weeks after the rash appears, most of the sores form scabs and begin to separate from the skin.
Most patients infected with smallpox report spinal pain and severe headaches; some may experience hallucinations, delirium, psychosis, depression, and manic depression. These symptoms may result from perivenular demyelination, which has been seen in autopsies of those with smallpox. Patients also may develop ophthalmologic complications known as variola residua. Conjunctivitis, the most common ophthalmologic complication, appears 5 days after rash onset. Osteomyelitis, seen in 2% to 5% of children with smallpox, results from viral invasion into the bone.
Exposure risk
Worldwide smallpox immunization has significantly reduced the risk of contracting the virus; routine vaccination among the general public ceased in 1972. However, the CDC advises vaccination for all healthcare providers who care for patients with suspected or confirmed smallpox and laboratory professionals who work with variola virus or other similar viruses. In the event of a smallpox outbreak or use of the virus as a bioweapon, the U.S. government has stockpiled enough vaccine (ACAM2000 and JYNNEOS) for the entire population. Individuals who require long-term protection can receive booster vaccines every 3 years.
Nursing implications
Emergency department nurses may be the first to notice a smallpox outbreak. Suspect smallpox in patients with a 2-day history of fever, malaise, body aches, and a rash (fewer lesions on the trunk than the distal extremities and face). When caring for these patients, practice strict infection control protocols, including chemically decontaminating (autoclaving or washing in hot water and hypochlorite bleach) all exposed instruments and surfaces.
Educate and raise awareness
Polio and smallpox aren’t an immediate threat to the general population or healthcare providers, but nurses have a responsibility to remain knowledgeable about the diseases, the importance of needed vaccinations, and nursing implications when caring for patients who’ve contracted the viruses. Nurses play an important role in providing individual patient education regarding vaccine efficacy and safety and raising public awareness about the vaccination process.
Lisa Draze is a family nurse practitioner at My Choice Wisconsin in Madison.
American Nurse Journal. 2023; 18(8). Doi: 10.51256/ANJ082312
References
Backman I. Is polio making a comeback? Yale School of Medicine. August 26, 2022. medicine.yale.edu/news-article/is-polio-making-a-comeback/
Belleza M. Polio (poliomyelitis). Nurselabs. February 11, 2021. nurseslabs.com/polio/
Centers for Disease Control and Prevention. History of smallpox. February 20, 2021. cdc.gov/smallpox/history/history.html
Centers for Disease Control and Prevention. Poliomyelitis: For healthcare providers. June 1, 2023. cdc.gov/polio/what-is-polio/hcp.html
Centers for Disease Control and Prevention. Vaccinate staff. December 2, 2019. cdc.gov/smallpox/bioterrorism-response-planning/healthcare-facility/vaccinate-staff.html
Centers for Disease Control and Prevention. Vaccines. August 8, 2022. cdc.gov/smallpox/Clinicians/vaccines.html
Centers for Diseases Control and Prevention. Who should get vaccination. July 12, 2017. cdc.gov/smallpox/vaccine-basics/who-gets-vaccination.html
Housman T. Variolation vs. vaccination: 18th century developments in smallpox inoculation. The Beehive. May 12, 2020. masshist.org/beehiveblog/2020/05/variolation-vs-vaccination-18th-century-developments-in-smallpox-inoculation
Hussain AN. Smallpox clinical presentation. Medscape. July 28, 2020. emedicine.medscape.com/article/237229-clinical
Kimball S. How polio came back to New York for the first time in decades, silently spread and left a patient paralyzed. CNBC. October 4, 2022. cnbc.com/2022/10/04/how-polio-silently-spread-in-new-york-and-left-a-person-paralyzed.html
National Institute of Allergy and Infectious Diseases. Smallpox. December 11, 2014. www.niaid.nih.gov/diseases-conditions/smallpox
New Jersey Department of Health. 2022 polio case in the United States: What you need to know. October 5, 2022. nj.gov/health/cd/documents/topics/Polio/polio_provider_information_document.pdf
Polio Global Eradication Initiative This week. 2023. polioeradication.org/polio-today/polio-now/this-week
Riedel S. Edward Jenner and the history of smallpox and vaccination. Proc (Bayl Univ Med Cent). 2005;18(1):21-5. doi:10.1080/08998280.2005.11928028
Key words: polio, small pox, vaccines