Early identification prevents negative outcomes.
Takeaways:
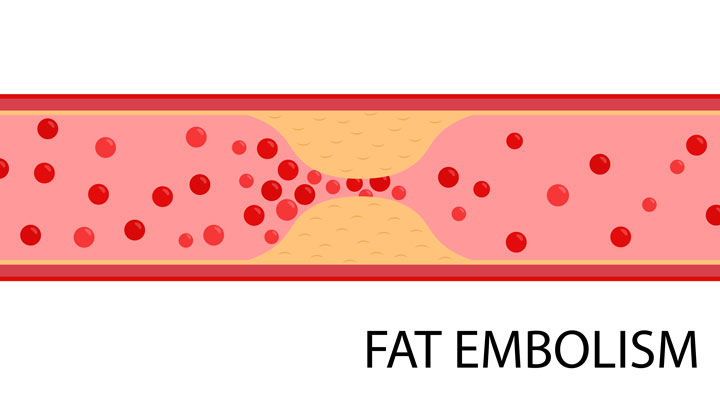
- Fat embolism syndrome is a rare complication that can occur after traumatic orthopedic injuries.
- Early identification of neurologic, respiratory, and dermatologic symptoms is critical.
Scott Hewlett*, age 28, has been transferred from a critical access hospital for surgical reduction and internal fixation (ORIF) of a left femur fracture. Mr. Hewlett was a driver wearing a seat belt when he was involved in a motor vehicle collision about 24 hours earlier. He has no significant medical or surgical history. At shift change, Erica, a nurse on the medical-surgical unit, is told that Mr. Hewlett’s last set of vital signs, 8 hours ago, were unremarkable: temperature 98.3° F (36.8° C), HR 89 bpm, RR 16 breaths per minute, BP 112/64 mmHg, and SpO2 96% on room air.
When Erica enters Mr. Hewlett’s room and notes that he has labored breathing, is confused, and isn’t following commands, she activates the rapid response team (RRT). Erica obtains a complete set of vital signs, which are temperature 101° F (38.3° C), HR 146 bpm, RR 36 breaths per minute, BP 92/50 mmHg, and SpO2 84% on room air. She sees that Mr. Hewlett has a diffuse petechial rash on his arms and torso.
Taking action
When the RRT nurse arrives, he places Mr. Hewlett on a non-rebreather oxygen mask at 15 L/minute while Erica applies the ECG monitor and pages the on-call hospitalist. The monitor shows sinus tachycardia. When the hospitalist arrives, the RRT nurse provides his assessment findings, and Erica shares Mr. Hewlett’s history and that he received 2 mg of morphine sulfate I.V. for pain about 2 hours earlier. The hospitalist orders a STAT ABG, portable chest x-ray, complete blood count, comprehensive metabolic panel, and erythrocyte sedimentation rate (ESR).
The x-ray shows bilateral pulmonary infiltrates, and the ABG shows a PaO2 of 52 mm Hg. Suspecting fat embolism syndrome (FES), a life-threatening condition that can occur after traumatic orthopedic injuries, the hospitalist orders an I.V. fluid bolus of normal saline, a chest computed tomography (CT), and a transfer to the ICU. Because Mr. Hewlett’s neurologic symptoms are thought to be related to hypoxia, the hospitalist doesn’t order a head CT.
Outcome
In the ICU, Mr. Hewlett is placed on continuous pulse oximetry, ECG, and vital sign monitoring with frequent neurologic and respiratory assessments. He requires supplemental oxygen and I.V. fluid support. The chest CT is consistent with FES, demonstrating bilateral ground-glass opacities. Within 24 hours, his neurologic and hemodynamic status return to baseline, and he no longer requires supplemental oxygen. Mr. Hewlett ultimately undergoes the ORIF and is discharged to rehab 4 days later.
Education and follow up
FES is a rare syndrome with prevalence rates between 1% and 30% after traumatic long bone injuries. It occurs when fat emboli occlude the vasculature, resulting in pulmonary (respiratory insufficiency), neurologic (confusion), and dermatologic (petechial rash) symptoms that appear 24 to 72 hours after the initial injury. Minor symptoms include elevated ESR, thrombocytopenia, oliguria, tachycardia, and fever. Signs and symptoms usually start 12 to 72 hours after a trauma. FES mortality rate is approximately 10%, so early recognition is critical. Treatment consists of supportive care with supplemental oxygen and I.V. fluids for hypovolemia, as needed.
Frequently, FES is a diagnosis of exclusion, but it requires astute assessment skills to prevent clinical deterioration. Erica’s critical observation of Mr. Hewlett’s rash, tachycardia, and neurologic status, as well as her prompt activation of the RRT facilitated quick assessment and implementation of an evidence-based treatment plan.
*Names are fictitious.
Aaron M. Sebach is an associate professor and director of graduate nursing programs at Wilmington University in New Castle, Delaware, and a hospitalist nurse practitioner at TidalHealth Peninsula Regional in Salisbury, Maryland.
References
Kosova E, Bergmark B, Piazza G. Fat embolism syndrome. Circulation. 2015;131(3):317-20. doi:10.1161/CIRCULATIONAHA.114.010835
O’Donnell JM. Fat embolism syndrome. In: O’Donnell JM, Nacul F, eds. Surgical Intensive Care Medicine. 3rd ed. New York, NY: Springer; 2016; 349-56.
Rothberg DL, Makarewich CA. Fat embolism and fat embolism syndrome. J Am Acad Orthop Surg. 2019;27(8):e346-55. doi:0.5435/JAAOS-D-17-00571
Weinhouse GL. Fat embolism syndrome. UpToDate. 2019. uptodate.com/contents/fat-embolism-syndrome