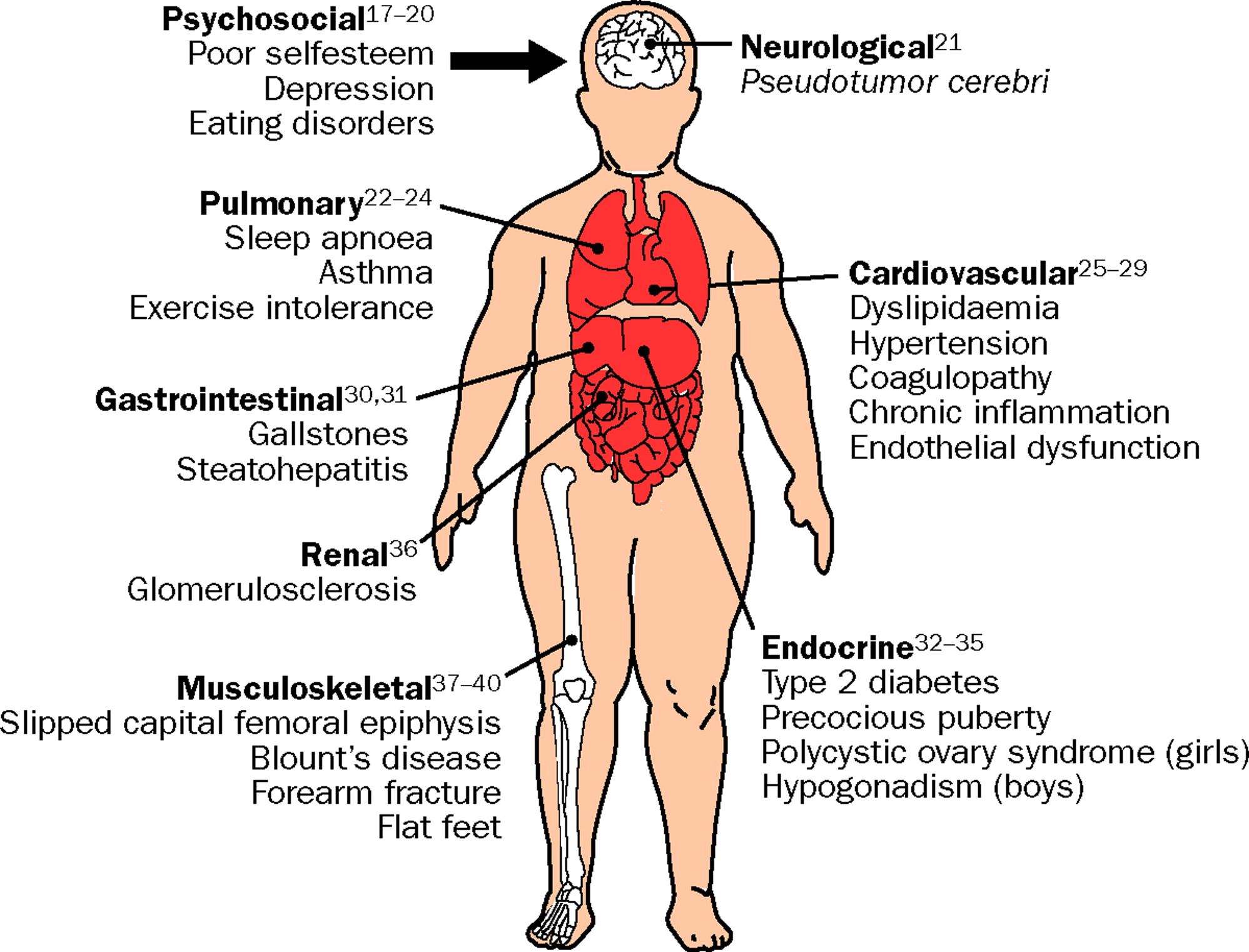
As the prevalence of obesity in the United States continues to rise, no doubt more of your patients are having weight issues that complicate their medical conditions and are receiving “lose weight” prescriptions from their healthcare providers.
Although you may have no trouble explaining to the patient why weight loss will benefit his or her health, you may be less comfortable in talking about the nuts and bolts of weight management.
After all, most people already know that to lose weight they need to eat less and exercise more. They just don’t know how to lose the weight and how to keep it off.
Weight loss therapy is a combination of diet, exercise, and behavioral lifestyle modifications. Tackling weight issues successfully requires specific strategies on how to make changes in all three areas. There is no magic formula but research does highlight strategies that are the most successful. Incorporating these tips into your teaching means better success rates for your patient. First, however, it’s important to understand how to communicate with patients about weight.
Communicating about weight
Perhaps you feel uncomfortable talking to your patient about his or her weight. The good news is that weight management experiences of patients indicate that they expect to be counseled about weight and want specific advice about diet, exercise, and setting realistic goals. Research indicates that patients who receive guidance about weight loss are more likely to change their diet and exercise habits, especially if the weight is affecting their health.
The bad news is that overweight and obese patients fear that healthcare providers are judging them. Unfortunately, discrimination and prejudicial behavior from nurses and other healthcare providers toward those who are overweight and especially those who are obese does exist.
Implementing these simple interventions will help build trust and respect:
- Reflect on your own attitude toward people with weight issues. Appreciate that obesity is a complex condition with multi-faceted etiologies. People with weight issues are not simply lazy, unmotivated, or lack self-control.
- Cultivate an obesity-friendly environment. Supplies (blood-pressure cuffs, large-size wheelchairs, beds, gowns) geared to care for an obese patient should be readily available and used.
- Use the nonjudgmental term of ‘weight’ when describing the problem. For example, begin the conversation by saying, “Mr. Simpson, I would like to talk to you about how your weight is affecting your diabetes.”
- Be mindful of privacy before you launch into a discussion about weight. The patient may not want the roommate or visitors in the room as bystanders.
- Assess readiness. Gently ask, “How do you feel about working on your weight issue?” Ask the patient what has worked or not worked in the past so that you can best tailor your teaching.
Maintain the right diet
Maintaining the prescribed diet is often a challenge for the patient. His or her medical condition will dictate the type of diet. Be sure the registered dietitian meets with your patient about suitable foods and amounts that are consistent with the prescribed diet.
Assess the patient’s understanding of the dietary guidelines and clarify any misunderstandings. For example, many patients do not realize that fat-free processed foods are not synonymous with low calorie foods. Reinforce that gradual weight loss is best—one-half to 2 pounds a week. Researchers found that health benefits begin to accrue with just a 5% to 10% loss of body weight.
Here are some tips you can give patients to help them succeed.
Simple healthy eating tips that can be incorporated into any diet plan include:
- Eat breakfast daily.
- Eat three meals a day.
- Limit fruit juice.
- Eat a variety of vegetables daily.
- Choose meats that are 90% lean.
- Remove poultry skin before cooking.
- Use low-fat or fat-free dairy products.
- Use salad dressings sparingly.
- Weigh yourself at least once a week.
Tips to for managing overeating include:
- Keep low-fat, low sugar food on hand for snacks such as whole grain cereal.
- Keep favorite foods out of sight.
- Eat meals as a family around the table.
- Eat more meals at home.
- Take half of your entrée home when eating out.
- Do not eat in front of the TV.
- Learn the right-sized portions of food to eat.
- Maintain diet consistency (no binges on weekends).
- Know what triggers eating binges and plan strategies to avoid them.
Encourage your patient to recruit help. According to weight loss experts, a weight management plan that is supported by family and friends is more likely to succeed.
Warn your patient to avoid over-the counter weight loss preparations unless specifically ordered by the physician. The U.S. Food and Drug Administration does not require that manufacturers provide data on safety or efficaciousness of their products before commercial dispersal. Despite the claims that these preparations are “natural” or “drug free”, many contain active ingredients that produce unhealthy biological effects or interact with medications that the patient is taking.
What about commercial weight loss programs such as Jenny Craig, L.A. Weight Loss, or Weight Watchers? Many people find the nutrition counseling, portion-controlled food plans, and the social support helpful. However, research evidence on the effectiveness of these programs is limited and some of the programs require a substantial financial commitment. Caution your patient to research the program and discuss this option with his or her healthcare provider before joining.
Increase physical activity
Your patient’s medical condition determines the kind and intensity of appropriate activity. Consult with the patient’s provider or physical therapist about activity limitations.
Medical and fitness experts recommend at least 30 minutes of accumulated moderate-intensity activity at least 5 days a week. Brainstorm with your patient how to meet this exercise prescription. Physical activity programs designed specifically for older adults at little or no cost are available at some senior centers and YMCA facilities. Even gardening and yard work count as exercise to build strength and endurance.
Tips to help patients boost their physical activity include:
- Take the stairs instead of the elevator.
- Walk to work.
- Get off the bus a stop or two early and walk the rest of the way.
- Choose parking spots further away from the store.
- Plan to walk regularly after dinner.
- Walk at lunch or during a coffee break.
- Walk the dog.
- Go to museums, art galleries, zoos.
- Recruit a walking partner.
Be sure to teach your patient to start slow and build up to the recommended amount and review warning signs of cardiovascular distress.
Modify lifestyle
Making the lifestyle changes to reduce and maintain weight loss is challenging. Most people will regain most of the weight they lose or more if they are unable to make lifestyle changes that sustain healthy eating and an active lifestyle. A number of strategies can increase the likelihood for success, including the support of family and friends. Social support from these sources enhances motivation to stick with a weight loss plan.
Setting reasonable and attainable goals is essential. Help your patient set two or three reasonable goals in the context of his or her medical condition. Examples of putting this into action are, “Mary, let’s figure out ways you can meet your goal of losing five pounds this month. Here is a list of healthy snack food alternatives. Which ones do you think will work for you?” Tell your patient that plateaus and setbacks happen to everyone and not to be discouraged.
Obesity management experts from the National Heart Lung and Blood Institute (NHLBI) suggest a great way to stay on track is through self-monitoring of progress by regularly noting weight, exercise patterns, and food consumption in daily diaries. Taking the diary to follow-up appointments with the healthcare provider makes it less likely that weight management is ignored or forgotten. Stress the importance of making and keeping follow-up appointments with the healthcare provider. Early recognition of factors complicating weight loss success, such as depression or eating disorders, ensures timely treatment.
Is weight management for everyone?
Are there any patients who would not benefit from discussion about reaching a healthy weight? Teaching about healthy eating and exercise habits is recommended for the prevention of further weight gain in normal-weight patients and overweight patients without co-morbidities. However, NHLBI obesity experts recommend that specific weight control advice for those with eating disorders, serious uncontrolled physical or mental illnesses, or pregnant or nursing mothers be avoided. Evidence for support of weight loss for those over 65 years of age is limited, but the benefits of weight loss in this age group decreases the disease burden of excess weight in many chronic conditions. If the weight loss regimen is tailored to maintain muscle and bone mass, it is appropriate for patients until 80 years of age.
Increasing your confidence in weight management
Abundant free sources are available online for health professionals and the public regarding healthy weight attainment. Increase your knowledge and confidence in talking to your patients about reaching a healthy weight by taking advantage of these sources. Seek out and familiarize yourself with what is available on your unit.
Patient information documents are available free from reputable government sources that can be used “as is” or altered to fit the needs of your facility. Patient-friendly websites include:
http://www.cdc.gov/nccdphp/dnpa/ Tips to increase vegetable eating, portion size, and avoiding sugar-filled drinks. Also has BMI calculator
http://win.niddk.nih.gov/ Weight-control Informational Network (WIN) offers research-based information for professionals and non-professionals on weight management strategies
http://www.win.niddk.nih.gov/publications/choosing.htm#responsible Information on choosing the right commercial weight loss program
http://aoaweb.obesity.org/subs/fastfacts/Obesity_Treatment.shtml Information on weight loss, physical activity, determining BMI, and obesity treatments
http://www.mypyramid.gov/ The new food pyramid couples healthy eating with exercise
http://www.cdc.gov/nccdphp/dnpa/physical/index.htm Physical activity resources and other healthy lifestyle information
You can help your patient begin the journey to a healthier weight and ultimately, a healthier life.
Penny S. Boyer, PhD, RN CNE is an Associate Professor of Nursing at Hartwick College, Oneonta, NY.
References
Brown I. Nurses’ attitudes toward adult patients who are obese. Journal of Advanced Nursing. 2006;53(2):221-232.
Federal Drug Administration. Dietary supplements – what you need to know. http://www.fda.gov/Food/ResourcesForYou/Consumers/ucm109760.htm
Katz, D. Competing dietary claims for weight loss: Finding the forest through the trees. Annual Review of Public Health, 2005; 26:61-88.
McTigue K, Harris R, Hemphill B, et al. Screening and interventions for obesity in adults: Summary of the evidence for the U.S. Preventive Services Task Force. Annals of Internal Medicine. 2003;139:933-932.
National Heart Lung and Blood Institute (NHLBI). The practical guide: Identification, evaluation, and treatment of overweight and obesity in adults. http://www.nhlbi.nih.gov/guidelines/obesity/prctgd_c.pdf
National Institutes of Health. Talking with patients about weight loss: Tips for primary care professionals. http://www.win.niddk.nih.gov/publications/talking.htm
Tan D, Zwar N, Dennis S, Vagholkar S. Weight management in general practice: What do patients want? Medical Journal of Australia. 2006;185(2):73-75.
United States Department of Agriculture. MyPyramid. http://www.mypyramid.gov/
Wadden T, Didie E. What’s in a name? Patients’ preferred terms for describing obesity. Obesity Research. 2003;11:1140-1146.
From our readers gives nurses the opportunity to share experiences that would be helpful to their nurse colleagues. Because of this format, the stories have been minimally edited. If you would like to submit an article for From our readers, click here.