What nurses need to know to provide the best patient care.
Takeaways:
- Today, practicing nurses must understand the relationship of genetics and genomics to health, prevention, screening and treatment.
- Nurses need the skills to gather family history, identify hereditary risk, and make appropriate referrals for genetic consultation and testing.
- During the genetic assessment process nurses can help patients understand test results, provide support, explore implications for family, and encourage compliance with screening and treatment recommendations.
By Susan Montgomery, BSN, OCN, GCN; Wendy A. Brouwer, MSN, RN-C, WHNP, AGN-BC; Phyllis C. Everett, MSN, RN, AOCN, APNG, NP-C; Elizabeth Hassen, PhD(c), RN, OCN; Tracy Lowe, PhD(c), MS, RN; Sheila B. McGreal, MSN-CV, RN-BC, ACNS-BC, ANP-BC; and Julie Eggert, PhD, RN, FAAN
The central dogma of biology (deoxyribonucleic acid [DNA] to ribonucleic acid [RNA] to protein) was first described in 1957, before the current average-aged 50-year-old nurse was born. And it wasn’t until 2008 that genetics was considered essential to nursing education, when most experienced nurses were already at least 45. In other words, many nurses have minimal genetics education and may not feel comfortable incorporating genetics assessment and implications into a patient care plan.
Patient care in the dawn of the genomic age
Genetics and ethics in health care and nursing


Since 2003, when human genome sequencing was completed, much genetic information and technology has been introduced into healthcare, requiring nurses to understand and translate these concepts to patients. However, without a strong foundation in genetic facts, how do nurses know what’s important? How do we identify the red flags of inherited diseases, use a family assessment to recognize risk factors, develop a plan of care to educate patients, and ensure proper diagnosis?
This article explains basic genetic terminology and processes and describes assessment steps to help clinical nurses care for and manage patients at risk for inherited adult-onset diseases.
Genetics, genomics, and epigenetics
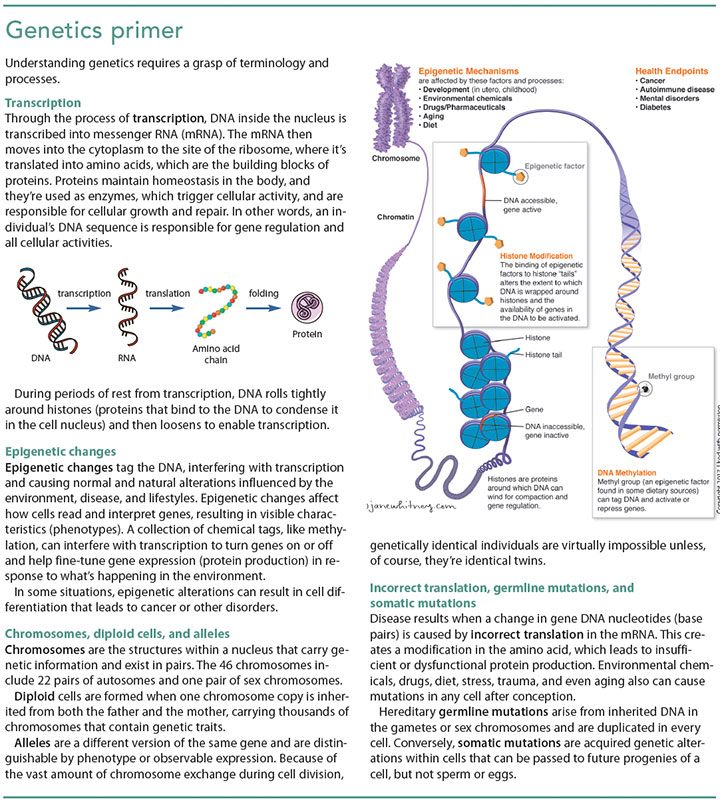
Genes are composed of DNA sequences located in segments along an individual’s chromosomes. A person’s genes are passed from one generation to the next, making genetics the study of heredity. The complete length of a person’s DNA within a cell is called the genome, making genomics the study of the structure of the genome through mapping and sequencing of DNA. Epigenetics studies the environment’s role in activating and deactivating genes. (See Genetics primer.)
Pharmacogenomics
Pharmacogenomics, the study of how a person metabolizes medications based on his or her personal genetic makeup, is one of the earliest applications of genetic and genomic research into clinical intervention. (See Genetic markers for drug response and function.) Pharmacogenomics has been most commonly used in psychiatry to determine drug choice and response, and in pain management to assess addiction potential. In addition, genetic testing can be used to tailor medication management to reduce and minimize side effects and promote treatment plan adherence.
While not routinely used in general practice, this type of personalized medicine may become more commonplace as we begin to tie patient outcomes to reimbursement. Adverse drug reactions are the fourth leading cause of death and are responsible for over 1 million emergency department visits each year, with 25%r of these patients requiring hospitalization for further treatment. Issues related to drug metabolism cost $3.5 billion per year in supplementary healthcare expenditures.
Genetic markers for drug response and function
OPRM1—opioid analgesic effectiveness
SLC6A4—antidepressant response
SLCO1B1—statin safety and efficacy
VKORC1—warfarin sensitivity
MTHFR—dietary folate conversion to its active form
BDNF and DRD2—dopamine release enhancement
Hepatic isoenzymes (cytochrome P450, including CYP2D6, CYP2C9, CYP2C19, CYP3A4, CYP3A5, CYP2B6, and CYP1A2)—drug metabolism interference
Nursing care and genetics
The initial Scope and Standards for Clinical Genetics Nursing Practice was first published in 1998 after the American Nurses Association (ANA) recognized genetics as a nursing specialty. Then, shortly after completion of human genome sequencing, ANA published the Essentials of Genetic and Genomic Nursing: Competencies, Curricular Guidelines, and Outcome Indicators, which was endorsed by 47 nursing organizations. These guidelines challenge nurses to:
- recognize how their personal attitudes about genetics might impact their practice
- advocate for clients for genetic services and autonomous genetic decision-making
- incorporate genetic and genomic information into their practices and regularly evaluate their competency
- tailor genetic and genomic information to patients based on their culture, literacy, religion, and preferred language.
To incorporate these competencies into practice, nurses need basic genetic and genomic knowledge. ANA provides a list of current genetics publications and resources that are earmarked for nurses. The competencies divide the professional practice guidelines into four categories—nursing assessment; identification of hereditary risk; referrals; and education, care, and support.
Nursing assessment
To assess a patient’s genetic risk, you must understand the relationship of genetics and genomics to health, prevention, screening, treatment, and monitoring. Essential nursing competencies include basic knowledge of genetic and genomic principles, genetic resources, current research, and professional guidelines and recommendations. Consider genetic, environmental, and genomic influences and risks during physical assessments, when collecting personal and family health histories, and when analyzing this information. In addition, assess the patient’s knowledge and perceptions of genetic and genomic information, as well as his or her responses, and address any issues or concerns. In developing the care plan in conjunction with the patient, integrate clinical judgment, patient preferences, evidence-based research, and family implications to plan genetic- and genomic-focused care.
Identification of hereditary risk
In the clinical setting, identification of hereditary risk begins with the primary care nurse. Obtain a three-generation family history to identify individual and family genetic risk factors. Start with the patient’s history, then gather information on first- (children, siblings, and parents), second- (maternal and paternal grandparents, aunts, uncles, nieces, and nephews), and third-degree (first cousins) relatives. Note any missing information or unknown family history. (See Family history resources.)
Family history resources
Access these online resources to learn more about genetics, genomics, and family histories.
American Academy of Family Physicians Genomics CME
Collection of the best content from the American Family Physician journal on genetics, family history, and individual syndromes.
Centers for Disease Control and Prevention
This site provides links to genetic, genomic, and family health history resources, including case studies, for health professionals.
Genetic Alliance
The Genetic Alliance promotes patient awareness of family health history with links to downloadable booklets in English and Spanish to help patients share their histories with clinicians.
U.S. Surgeon General
This patient-friendly website reviews the importance of family history and includes a web-based tool to organize and print family history information.
For each family member, collect the following information:
- Name, date of birth
- Health status, including medical conditions and age at diagnosis
- If deceased, age and cause of death
- Racial and ethnic ancestry of maternal and paternal grandparents.
After all data are gathered, analyze the information to determine patterns of both monogenic and multifactorial disease risks. (See Understanding monogenic and multifactorial disorders.) A drawn pedigree is a succinct way to visualize this information.
Understanding monogenic and multifactorial disorders
Adult-onset monogenic disorders are single-gene disorders with disease signs and symptoms (phenotypes) that can begin during childhood. These rare heritable conditions may be seen in multiple generations of a family and include:
• hereditary hemochromatosis
• alpha-1 antitrypsin deficiency resulting in obstructive pulmonary disease
• Huntington’s disease
• autosomal dominant polycystic kidney disease
• Gaucher disease
• Fanconi syndrome II
• inherited cancer syndromes, such as hereditary breast/ovarian cancer and Lynch syndrome.
More common are multifactorial disorders that result from a combination of genetic and environmental factors. They occur any time during the lifespan, but tend to be more common in adulthood. Like monogenic disorders, many multifactorial disorders can be identified in multiple family generations. They include:
• hypertension
• hypercholesterolemia
• coronary artery disease
• stroke
• autoimmune disorders (for example, rheumatoid arthritis, systemic lupus erythematous, psoriasis, Graves’
disease, multiple sclerosis, scleroderma)
• Alzheimer’s disease
• Parkinson’s disease
• schizophrenia
• alcoholism
• cancer
• bipolar affective disorder.
Electronic health records (EHRs) typically include a family history section for documenting health information over three generations. Ideally, an alert would prompt you to clarify information related to genetic risk factors. The best EHR would generate a pedigree based on the family history entered. Current EHRs aren’t able to produce pedigrees or prompt practitioners to potential genetic risks, but the need for this software development is recognized.
Several red flags in a patient’s personal and family history may indicate a potential for inherited susceptibility to a disease or genetic condition. Both the Genetic Alliance and the National Coalition for Health Professional Education in Genetics are reliable resources to learn about red flags. Primary care, cardiology, oncology, and other specialties have published data that specify red flags in their specialty. (See Genetic red flags.)
Genetic Red Flags


According to the Genetics in Primary Care Institute, red flags vary based on the assessment. For example, red flags for hereditary cancer will be different from those for a preconception evaluation. Also, an individual’s ethnicity and race have a significant influence on the distribution, incidence, and prevalence of many genetic diseases.
Referral
When red flags are identified during the family history, you or the provider should make a referral to a genetic specialist. To help patients and families make informed decisions and to decrease their anxiety, provide information about the reasons for testing, types of tests, and benefits and risks.
Benefits of genetic testing include providing a definitive diagnosis, offering information related to familial risk, and identifying prevention, management, and treatment options. Risks include the potential for discrimination based on genetic results, anxiety over the uncertainty of incidental findings of unknown significance, and the psychological impact of what the findings mean. (See Uses of genetic testing.)
Uses of genetic testing
You can help patients and families understand the purpose behind genetic testing options.
Diagnostic testing confirms or rules out a diagnosis. This testing is indicated when symptoms already exist.
Carrier testing determines whether an individual is a carrier of a recessive or X-linked Mendelian disorder.
Predictive or presymptomatic testing indicates whether a person is very likely to develop a condition such as Huntington’s disease.
Prenatal or antenatal testing looks for genetic and chromosomal disorders such as Down syndrome.
Susceptibility testing determines an individual’s genetic risk for an etiologically complex disorder that involves multiple risk factors, such as diabetes or heart disease.
Pharmacogenetic testing analyzes genetic variants to predict an individual’s response to a specific medication or class of medications.
Be aware of barriers to genetic technology and services, including culture, language, family values, traditions, religion, and health beliefs. In addition, stay up-to-date on current health policy regarding reimbursement for genetic and genomic health services as well as genetic discrimination related to insurance and employment.
Local and national resources can help facilitate referrals. The International Society of Nurses in Genetics and the National Society of Genetic Counselors can help locate genetic professionals. Genetic services are frequently offered by specialty (for example, cardiology or oncology), so keep a list of local resources. Genetests.org is another useful clinical tool to assist in identifying available genetic testing in clinical and research labs.
In addition to genetic and genomic referrals, the personal or family history may require risk-management referrals to appropriate specialists. You can be instrumental in initiating these referrals and providing follow-up.
Education, care, and support
The genetic testing process, from initial counseling through disclosure of test results, can take 4 weeks or more. During this time, you can offer emotional support and discuss potential strategies for action after the results are received. (See Interpreting genetic test results.)
Interpreting genetic test results
Understanding what test results mean can help you explain them to patients and their families, connect them to resources, and provide support.
Positive test results:
• show a change in a particular gene, chromosome, or protein of interest.
• may confirm a diagnosis, but generally can’t be used to predict the course
or severity of a condition.
• may provide options for prevention and management of the disorder.
Negative test results:
• indicate no change in the gene, chromosome, or protein of interest.
• virtually rule out a particular disorder, assuming the test is highly accurate
and the individual’s symptoms can be attributed to other causes.
• don’t rule out the presence of a mutation in another gene that could cause
he same disorder.
Variant of unknown significance results:
• indicate a finding of a variation in the DNA that’s not normal, but hasn’t
yet been associated with a disorder in other people.
• may be difficult to evaluate because everyone has common natural
variations in their DNA (polymorphisms) that don’t affect health.
After learning the test results, help clarify information provided by genetic professionals, explore implications for the patient and family, recommend health promotion and prevention practices based on genetic risk factors, and collaborate with healthcare providers for optimal care delivery. Individuals identified as high risk for genetic diseases should be referred for early detection and screenings based on recommended national guidelines. Encourage patients to discuss risks with family members so each person can make individual decisions for referral, intervention, and testing.
Offer support as patients navigate a new diagnosis associated with a genetic mutation. This can include exploring the effect of genetic information on extended family members, supporting lifestyle changes based on genetic predisposition, explaining pharmacogenomic therapies, and identifying strategies for reimbursement of genetic services.
Nursing and precision medicine
Precision medicine (tailoring medical treatment to each patient’s individual characteristics) has become an important component of nursing practice. Research supports precision medicine as an evolving strategy for disease treatment and prevention that includes attention to an individual’s variability in genes, environment, and lifestyle.
The National Institute of Nursing Research (NINR) supports research across diverse populations and settings to develop more personalized strategies to prevent and manage the adverse symptoms of illness. NINR-supported scientists are actively engaged in implementing clinical applications of genomics to accelerate discoveries that allow healthcare providers and researchers to accurately predict what disease treatment and prevention strategies will work in which groups of people. In contrast to a one-size-fits-all approach, precision medicine challenges nurses to think genetically across specialties and practice settings.
Nursing at the forefront
For 15 years, the Gallup Honesty and Ethics poll has ranked nursing as the most trusted profession in the United States. This public trust places nurses in the unique position to educate individuals and their families on the presence, absence, or future possibility of disease to improve health outcomes and promote delivery of patient-centered care.
Essential competencies related to genetics have been developed for nurses with undergraduate and graduate degrees. You can access these and other online resources for continuing education, professional organizations dedicated to nursing genetics and genomics, and additional information (See Genetic and genomic resources.)
As nurses become more aware of genetics and the need to incorporate genetic assessment into everyday practice, we’re initiating and facilitating referrals to improve patient care and outcomes. However, each state has a nursing scope of practice regarding genetics and genomics, so make sure you know the restrictions within your state.
As treatment becomes more individualized based on genetic profiles, nurses must acquire genetic and genomic knowledge to provide the best patient care. Primary care nurses knowledgeable in genetics and genomics will be at the forefront of this new era in medicine.
Genetic and genomic resources
American Nurses Assocation—Essentials of Genetic and Genomic Nursing: Competencies, Curricular Guidelines, and Outcome Indicators
American Nurses Association and International Society of Nurses in Genetics—Essential Genetic and Genomic Competencies for Nurses with Graduate Degrees
Centers for Disease Control and Prevention—Training programs and courses
Genetics/Genomics Competency Center—Online repository of peer-reviewed genomics educational materials, with links to courses, websites, and articles
International Society of Nurses in Genetics—Dedicated to fostering scientific and professional growth of nurses in human genetics and genomics worldwide
National Institutes of Health: Genetics Home Reference—Consumer-friendly information about the effects of genetics on health
The Surgeon General’s Family Health History Initiative—Information and template to collect a family history
University of Cincinnati/Cincinnati Children’s Hospital Medical Center—Genetic counseling: graduate program
Susan Montgomery is a genetic nurse navigator in the risk assessment program, department of clinical genetics, at Fox Chase Cancer Center in Philadelphia, Pennsylvania. Wendy A. Brouwer is a women’s healthcare nurse practitioner in the breast medical oncology department at M.D. Anderson Cancer Center in Houston, Texas. Phyllis C. Everett is adult nurse practitioner in the multidisciplinary breast cancer program at the Duke Cancer Institute in Durham, North Carolina. Elizabeth Hassen is a PhD candidate in the healthcare genetics doctoral program and an instructor at Clemson School of Nursing in Clemson, South Carolina. Tracy Lowe is a PhD candidate in the genetics iPhD program and an instructor at Clemson School of Nursing. Sheila B. McGreal is an assistant professor in the College of Nursing and Health Professions at Lewis University in Romeoville, Illinois, and a cardiology nurse practitioner for the University of Chicago in Illinois. Julie Eggert is the Mary Cox Professor and healthcare genetics doctoral coordinator at the Clemson School of Nursing and the College of Behavioral Health and Science at Clemson University.
Selected references
Consensus Panel. Genetics/Genomics Nursing: Scope and Standards of Practice. 2nd ed. Silver Spring, MD: American Nurses Association (ANA), International Society of Nurses in Genetics (ISONG); 2016.
Consensus Panel on Genetic/Genomic Nursing Competencies. Essentials of Genetic and Genomic Nursing: Competencies, Curricula Guidelines, and Outcome Indicators. 2nd ed. Silver Spring, MD: American Nurses Association; 2009.
Dorman JS, Schmella MJ, Wesmiller SW. Primer in genetics and genomics, article 1: DNA, genes, and chromosomes. Biol Res Nurs. 2017;19(1):7-17.
Durmaz AA, Karaca E, Demkow U, Toruner G, Schoumans J, Cogulu O. Evolution of genetic techniques: Past, present, and beyond. Biomed Res Int. 2015; Article ID: 461524.
Loi M, Del Savio L, Stupka E. Social epigenetics and equality of opportunity. Public Health Ethics. 2013;6(2):142-53.
National Institutes of Health. What is precision medicine? September 5, 2017.
Ormondroyd E, Oates S, Parker M, Blair E, Watkins H. Pre-symptomatic genetic testing for inherited cardiac conditions: A qualitative exploration of psychosocial and ethical implications. Eur J Hum Genet. 2014;22(1):88-93.
Schaa KL. Assessing patients with a genetic “eye”: Family history and physical assessment. In: Kasper CE, Schneidereith TA, Lashley FR, eds. Lashley’s Essentials of Clinical Genetics in Nursing Practice. 2nd ed. New York, NY: Springer Publishing Company; 2016; 191-214.



















3 Comments.
Great article!❤️
100% excellent. Thumbs up!
Excellent article